Blog > Treatment Strategies > PTSD Treatment Plan: Examples, Goals & SMART Objectives
PTSD Treatment Plan Examples, Goals, and SMART Objectives for Clinicians
This comprehensive guide to creating a PTSD treatment plan walks clinicians through everything needed to build effective, audit-ready documentation. You’ll find PTSD treatment plan examples, measurable goals and objectives, and SMART goal frameworks that align with payer and accreditation requirements. The article also covers evidence-based interventions, including CBT, CPT, cognitive therapy, and prolonged exposure, along with practical tips for documenting progress and improving patient outcomes. Whether you’re looking for a sample treatment plan for PTSD or guidance on writing trauma-informed goals, this resource provides clear, clinician-focused direction you can apply immediately.

Last Updated: May 1, 2026


What You'll Learn
- What a PTSD treatment plan is and how it supports clinical care, compliance, and reimbursement
- The difference between PTSD and trauma treatment plans — and when each applies
- Common PTSD treatment plan goals and measurable objectives (with real examples)
- How to write SMART goals for PTSD that meet payer and accreditation standards
- A complete sample PTSD treatment plan you can adapt for your own documentation
- Evidence-based approaches, including CBT, CPT, cognitive therapy (CT), and prolonged exposure (PE)
- Best practices for documenting progress, tracking outcomes, and maintaining audit-ready records
Contents
A strong PTSD treatment plan does three things at once: it organizes the clinical work, satisfies payer and accreditation documentation requirements, and gives the patient a clear path forward. This guide walks through how to build one — with sample goals, SMART objectives, an example plan you can adapt, and CBT- and CPT-specific approaches grounded in the APA Clinical Practice Guideline for PTSD.
If you'd rather start from a structured template, you can download our PTSD Treatment Plan Template (PDF) and adapt the examples below to your patient.
What is a PTSD Treatment Plan?
Quick Definition
What is a PTSD treatment plan?
A PTSD treatment plan is a structured clinical document that outlines a client’s trauma-related symptoms, diagnosis, treatment goals, measurable objectives, planned interventions, and review timeline. It helps clinicians organize care, document medical necessity, track progress over time, and align treatment with payer, accreditation, and clinical documentation requirements.
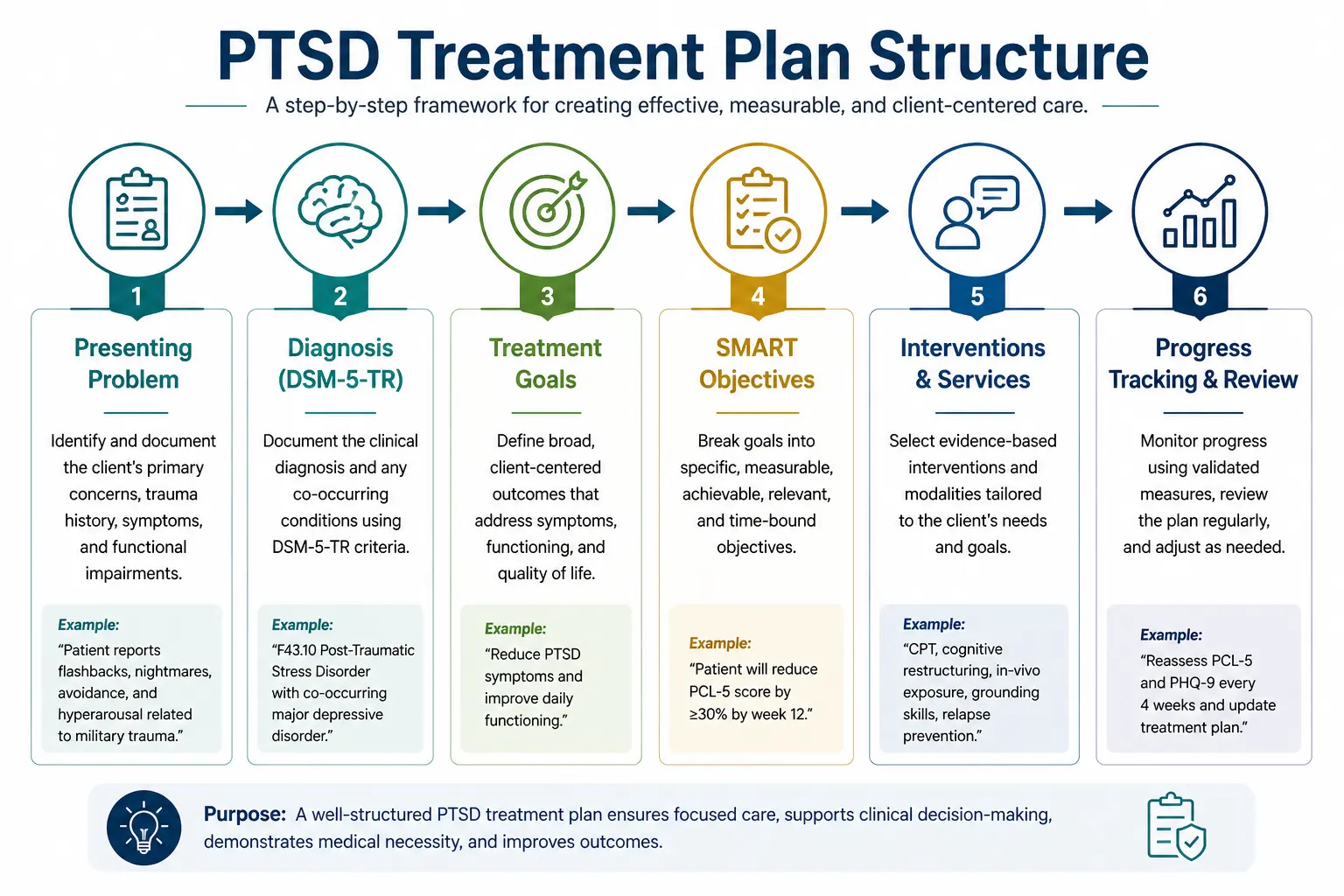
A PTSD treatment plan is a clinical document that captures the patient's presenting trauma-related problems, measurable goals and objectives, the interventions you'll use, and the timeframe for review. It functions as both a clinical roadmap and a record for payers, accreditors, and the next clinician who reviews the chart.
Post-traumatic stress disorder follows exposure to a traumatic event — combat, sexual assault, domestic violence, a serious accident, or repeated exposure to traumatic material — and is characterized by intrusion, avoidance, negative alterations in cognition and mood, and changes in arousal and reactivity. The DSM-5-TR criteria (American Psychiatric Association, 2022) are the diagnostic anchor most clinicians use when documenting the presenting problem. Lifetime PTSD prevalence in U.S. adults is approximately 6%, while a much larger share will experience a qualifying traumatic event at some point (VA National Center for PTSD).
Why a written plan matters
- Guides treatment by tying each session back to a specific goal and objective.
- Supports reimbursement — most payers require documented, measurable objectives tied to medical necessity.
- Meets accreditation standards (CARF, Joint Commission, Medicaid) for individualized treatment planning.
- Smooths transitions of care if the patient changes clinicians or levels of care.
- Helps the patient see progress, which improves engagement and retention in trauma work.
For more information on writing treatment plans, read our related guide: How to Write a Mental Health Treatment Plan: Examples, Goals & Templates

Free Download
PTSD Treatment Plan Template
Download a clinician-ready, fillable framework for documenting PTSD treatment plans with measurable goals, SMART objectives, interventions, baseline measures, review dates, and signature fields.
- Goal, objective, and intervention fields
- SMART goal worksheet for measurable treatment planning
- PCL-5, PHQ-9, GAD-7, and other baseline measure prompts
- Review log, safety planning, and coordination-of-care sections
PTSD vs. Trauma Treatment Plans: What's the Same, What's Different
Clinicians often use "PTSD treatment plan" and "trauma treatment plan" interchangeably, but they aren't identical. A PTSD treatment plan is built around a confirmed DSM-5-TR diagnosis of post-traumatic stress disorder. A trauma treatment plan is broader — it can apply to acute stress disorder, adjustment disorder with trauma features, complex trauma presentations that don't yet meet full PTSD criteria, or subclinical trauma symptoms in the context of another diagnosis.
The structural elements — problem statements, measurable goals, SMART objectives, evidence-based interventions, target dates — are the same. What changes is the diagnostic anchor, the medical-necessity language, and sometimes the recommended modality. CPT and Prolonged Exposure are first-line for PTSD specifically; trauma-focused CBT, EMDR, and stabilization-phase work may be more appropriate earlier in the trajectory.
PTSD Treatment Plan Goals and Objectives (with Examples)
Goals describe the broad clinical outcome the patient is working toward. Objectives are the measurable, time-bound steps that get them there. Most payers expect at least two objectives per active goal, written so progress can be observed and documented.
Below are common PTSD goal areas and example objectives you can adapt to your patient's presentation. These PTSD treatment plan goals and objectives should be individualized based on symptom severity, functional impairment, and treatment setting.
| Goal | Sample Measurable Objectives |
|---|---|
| Reduce intrusion symptoms (flashbacks, nightmares, intrusive memories) |
Patient will identify three trauma-related triggers and a corresponding grounding skill for each within 4 weeks. Patient will report a ≥30% reduction in PCL-5 intrusion subscale score by week 12. Patient will use a written nightmare-rescripting exercise at least twice weekly for 6 weeks. |
| Decrease avoidance behaviors |
Patient will construct a written exposure hierarchy of 8–10 avoided situations within 3 sessions. Patient will complete two in-vivo exposure assignments per week for 8 weeks, logging SUDS pre/post. Patient will resume one previously avoided activity (e.g., driving, social setting) by week 10. |
| Improve negative alterations in cognition and mood |
Patient will identify and challenge three trauma-related cognitive distortions per week using a thought record. Patient will increase positive activity scheduling from baseline 0–1 to 4 events per week within 6 weeks. Patient will report a ≥5-point reduction on the PHQ-9 by week 12. |
| Reduce hyperarousal and reactivity |
Patient will practice diaphragmatic breathing or progressive muscle relaxation daily for 10 minutes for 8 weeks. Patient will report a sleep latency of ≤30 minutes on at least 5 nights per week by week 10. Patient will demonstrate two grounding techniques in-session by week 4. |
| Address co-occurring substance use |
Patient will identify trauma-related substance use triggers and a coping plan for each within 6 weeks. Patient will reduce alcohol use from baseline X drinks/week to ≤Y drinks/week by week 12, verified by self-report. Patient will attend one peer-support meeting per week for the duration of treatment. |
| Strengthen interpersonal functioning |
Patient will initiate one supportive social contact per week for 8 weeks. Patient will use an assertive communication skill in two interpersonal situations per week by week 6. Patient will report improved relationship satisfaction on a 0–10 scale (baseline → +2 points) by week 12. |
| Improve safety (when indicated) |
Patient will complete and sign a written safety plan within the first two sessions. Patient will identify two emergency contacts and one crisis-line number by session 2. Patient will demonstrate use of safety plan in-session if suicidal ideation re-emerges. |
SMART Goal Examples for PTSD
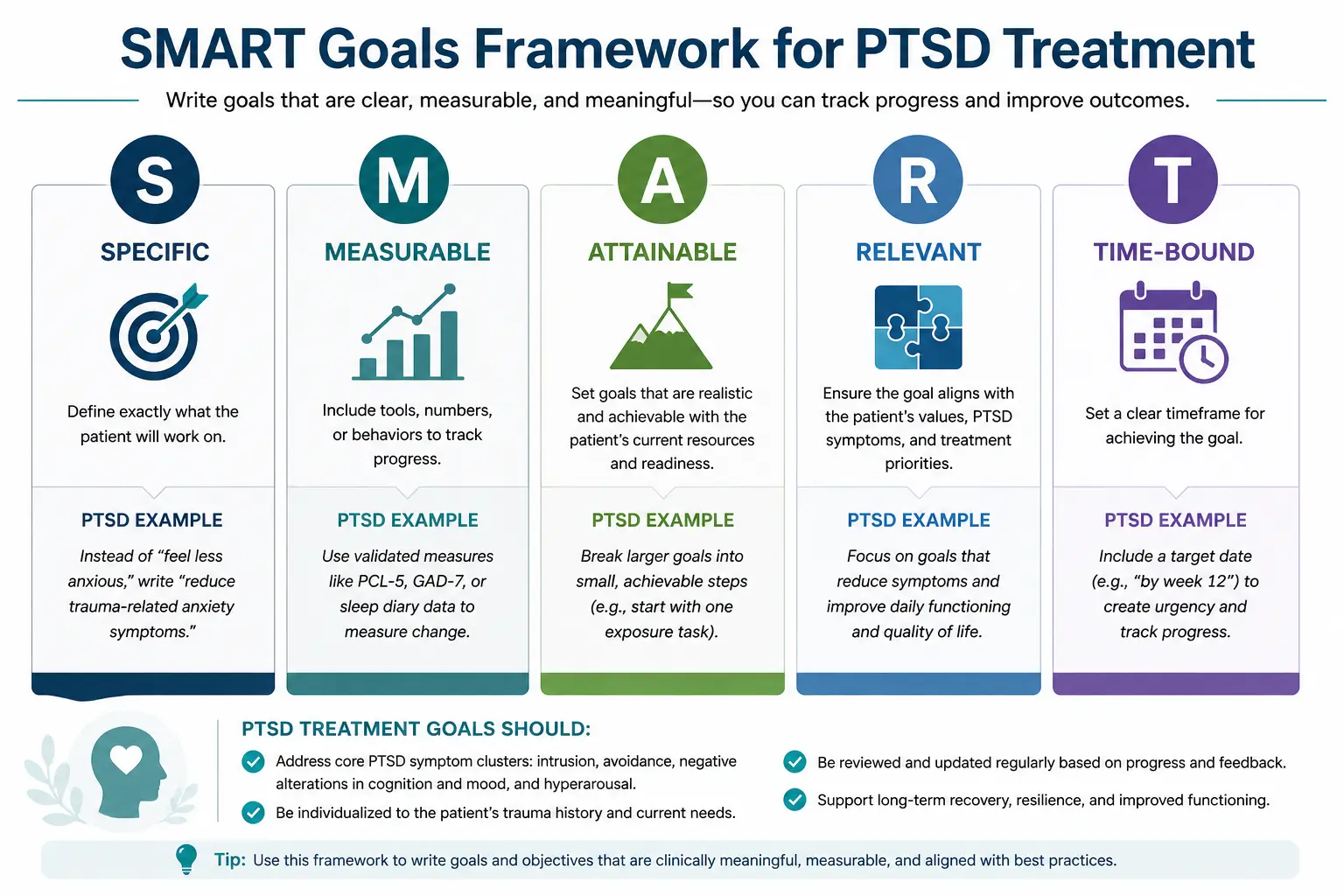
SMART (Specific, Measurable, Attainable, Relevant, Time-bound) is the framework most payers and accreditors expect. The difference between a goal that supports reimbursement and one that gets flagged is usually a missing date or an unmeasurable verb. Writing SMART goals for PTSD ensures your treatment plan meets payer requirements and supports measurable clinical outcomes.
Weak vs. SMART — three quick rewrites
Weak
"Patient will feel less anxious."
SMART
Patient will reduce GAD-7 score from 16 to ≤10 by week 12, evidenced by weekly self-report and twice-monthly clinician administration.
Weak
"Patient will avoid less."
SMART
Patient will complete two graduated in-vivo exposure assignments per week from a written hierarchy for 8 consecutive weeks, with SUDS ratings logged pre- and post-exposure.
Weak
"Patient will sleep better."
SMART
Patient will achieve sleep latency of ≤30 minutes on at least 5 of 7 nights per week by week 10, tracked via daily sleep diary.
PTSD Treatment Plan Example (Sample Plan You Can Use)
The plan below is a fictional, abbreviated example built for illustration. It shows how a real plan strings together: identifying information, presenting problems, diagnosis, three active goals with SMART objectives, evidence-based interventions, and a review date. Adapt the structure — not the specifics — to your patient.
CBT Treatment Plan for PTSD: A Sample Outline
Trauma-focused cognitive behavioral therapy is one of the strongest-supported interventions for PTSD. A CBT treatment plan for PTSD keeps the same overall structure but specifies CBT-aligned interventions: psychoeducation, cognitive restructuring of trauma-related beliefs, exposure work, and behavioral activation.
Sample CBT-Driven Plan Elements
- Phase 1 (sessions 1-3): Psychoeducation on the CBT model and PTSD; collaborative case formulation; introduction of grounding and breathing skills.
- Phase 2 (sessions 4-10): Cognitive restructuring of trauma-related stuck points (self-blame, world-as-dangerous, broken-self beliefs) using thought records; concurrent in-vivo exposure hierarchy.
- Phase 3 (sessions 11-14): Imaginal exposure or trauma narrative work; consolidation of new beliefs; behavioral activation toward valued activities.
- Phase 4 (sessions 15-16): Relapse prevention; review of progress on PCL-5 and behavioral indicators; discharge or step-down planning.
Choosing a Treatment Approach: CBT, CPT, CT, and Prolonged Exposure
The APA's Clinical Practice Guideline for PTSD strongly recommends four trauma-focused therapies. Each has a slightly different center of gravity, and the right choice depends on patient preference, comorbidities, and clinical context.
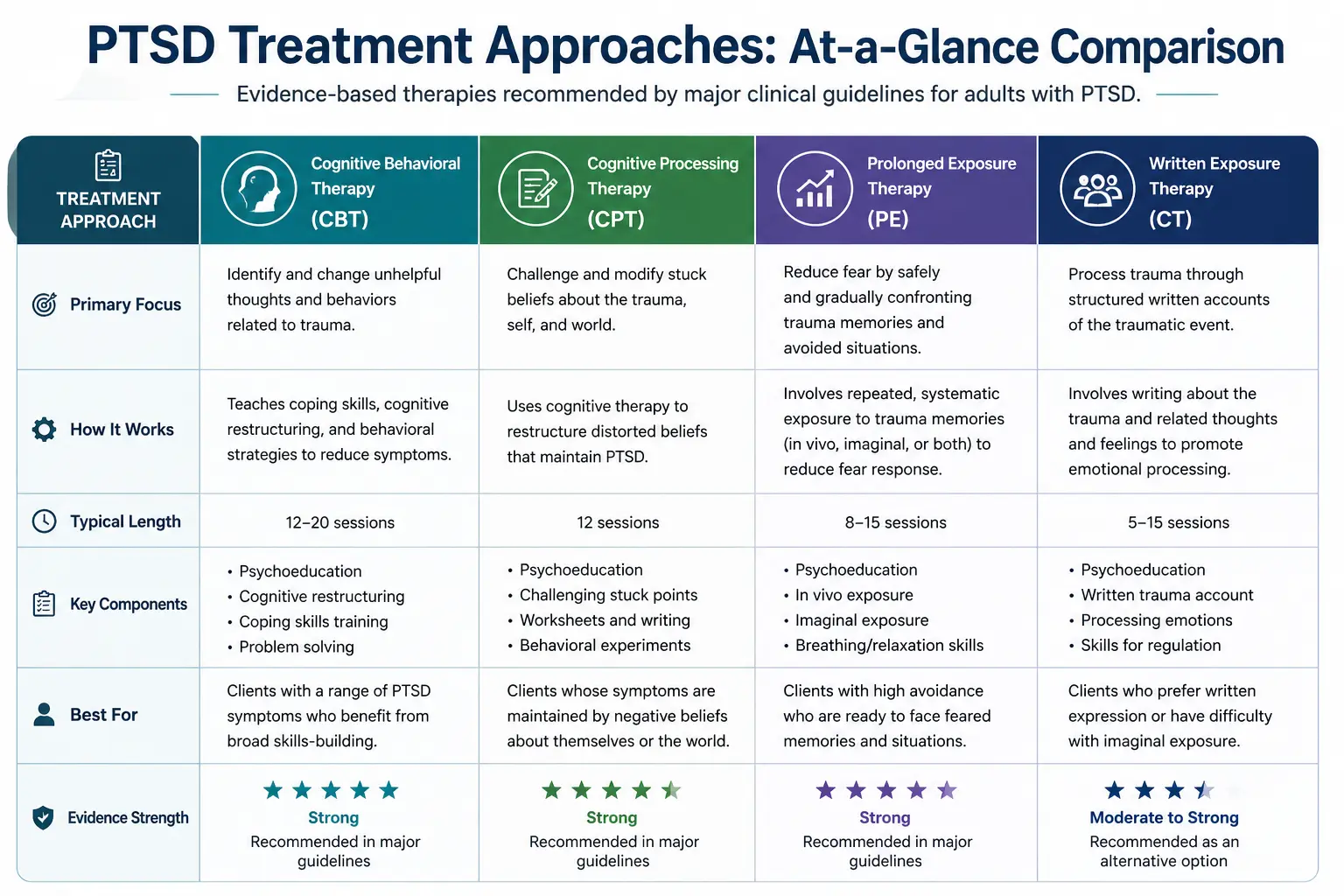
Cognitive Behavioral Therapy (CBT)
Cognitive behavioral therapy (CBT) is a widely used, evidence-based approach that helps patients identify and change the thought–behavior patterns that maintain PTSD symptoms. It focuses on the relationship between thoughts, emotions, and behaviors, helping patients develop more adaptive coping strategies.
How it works: CBT combines cognitive restructuring (challenging unhelpful thoughts) with behavioral techniques such as exposure and activity scheduling to reduce avoidance and improve functioning.
Best fit: CBT is a strong option for patients with a broad range of PTSD symptoms, especially those who benefit from structured skill-building and practical coping strategies.
Example in a treatment plan:
Patient will identify and challenge three trauma-related cognitive distortions per week using a structured thought record, with progress measured by a ≥5-point reduction in PHQ-9 score by week 12.
Cognitive Processing Therapy (CPT)
Cognitive processing therapy (CPT) is a structured, trauma-focused form of CBT that targets “stuck points” — rigid, trauma-related beliefs about safety, trust, power, esteem, and intimacy that develop after a traumatic experience.
How it works: CPT uses guided worksheets and cognitive restructuring to help patients examine and reframe distorted beliefs about the trauma, reducing emotional distress and improving functioning.
Best fit: CPT is particularly effective for patients experiencing guilt, shame, or self-blame related to the trauma, or those whose symptoms are maintained by negative beliefs about themselves or the world.
Example in a treatment plan:
Patient will complete weekly CPT worksheets to identify and challenge trauma-related beliefs, with progress measured by a ≥30% reduction in PCL-5 score over 12 sessions.
Cognitive Therapy (CT)
Cognitive therapy (CT) for PTSD focuses on how patients interpret and assign meaning to the traumatic event and its aftermath. It places greater emphasis on modifying the personal significance of the trauma memory.
How it works: CT involves detailed cognitive restructuring and imagery-based techniques to help patients re-evaluate the trauma and reduce the sense of current threat associated with it.
Best fit: CT is well-suited for patients who experience persistent negative interpretations of the trauma or who benefit from deeper cognitive and imagery-based work.
Example in a treatment plan:
Patient will identify and reframe trauma-related beliefs about safety and self-worth during weekly sessions, with progress evidenced by reduced avoidance behaviors and improved functioning by week 12.
Prolonged Exposure (PE)
Prolonged exposure (PE) is a trauma-focused therapy that reduces PTSD symptoms by helping patients gradually confront trauma-related memories and avoided situations in a safe, structured way.
How it works: PE includes imaginal exposure (revisiting the trauma memory during sessions) and in-vivo exposure (gradually approaching avoided but safe situations) to decrease fear and avoidance over time.
Best fit: PE is especially effective for patients with high levels of avoidance who are ready to directly engage with trauma-related memories and triggers.
Example in a treatment plan:
Patient will complete two in-vivo exposure assignments per week from a structured hierarchy for 8 weeks, with SUDS ratings recorded pre- and post-exposure to track reduction in distress.
Medications in the PTSD Treatment Plan
Pharmacotherapy is most often used alongside trauma-focused psychotherapy. SSRIs are the first-line class. Sertraline (Zoloft) and paroxetine (Paxil) are FDA-approved for PTSD; venlafaxine (Effexor), an SNRI, is supported by APA guidelines as well. Document the prescriber, dose, response, side effects, and review date in the plan.
Avoid benzodiazepines as a primary PTSD treatment — the VA/DoD Clinical Practice Guideline advises against routine use given limited efficacy and risk of dependence, particularly in patients with co-occurring substance use.
Documenting the Plan and Tracking Progress
A treatment plan is a living document. Most payers and accreditors require periodic review (typically every 90 days, or sooner with significant clinical change). Each progress note should reference the active goal and objective being worked on, so the chart tells a coherent story from intake through discharge.
- Review and update the plan after any significant clinical change, level-of-care change, or every 90 days at minimum.
- Tie each progress note to a specific goal/objective from the plan.
- Use validated measures (PCL-5, PHQ-9, GAD-7) at intake, mid-treatment, and discharge to evidence outcomes.
- Have the patient co-sign the plan and any major revisions.
From PTSD Treatment Plans to Audit-Ready Documentation — In Minutes
Creating a PTSD treatment plan with measurable goals, SMART objectives, and evidence-based interventions is essential — but documenting it clearly is what supports reimbursement, compliance, and continuity of care.
ICANotes helps you turn CBT, CPT, cognitive therapy, and prolonged exposure approaches into structured, defensible treatment plans and progress notes — without starting from scratch.
- Pre-built PTSD treatment plan templates with goals and objectives
- SMART goal frameworks that meet payer and accreditation requirements
- Integrated assessment tools like PCL-5, PHQ-9, and GAD-7
- Automatic linking between treatment plans and progress notes
Start your free 30-day trial — no credit card required.
Takes less than 60 seconds to get started
PTSD Treatment Plan FAQs
Related Resources for Trauma Treatment
Explore additional clinical insights and evidence-based approaches to trauma treatment, PTSD, and related conditions.
Recent Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.






