Blog > Treatment Strategies > Eating Disorder Treatment Plan: Templates & Examples for Clinicians
Eating Disorder Treatment Plan and Note Writing Tips
An effective eating disorder treatment plan provides a structured, individualized roadmap for treating complex eating disorders such as anorexia nervosa and binge eating disorder. This guide helps behavioral health clinicians understand what to include in a treatment plan, offers practical eating disorder treatment plan templates, and walks through real-world examples to support goal setting, documentation, and continuity of care. Whether you’re building a new plan or refining an existing one, this resource supports both clinical decision-making and defensible documentation.

Last Updated: January 14, 2026


What You'll Learn
-
What to include in a clinically sound eating disorder treatment plan
-
How to structure treatment goals and objectives for eating disorders
-
A practical eating disorder treatment plan template you can adapt
-
A sample treatment plan for anorexia nervosa
-
A binge eating disorder treatment plan example
-
Tips for documenting treatment plans and progress notes effectively
Contents
- Eating Disorder ICD-10 Codes and Documentation Requirements
- What Should Be Included in an Eating Disorder Treatment Plan?
- Eating Disorder Treatment Plan Goals and Objectives
- Eating Disorder Treatment Plan Template
- Eating Disorder Treatment Plan Examples
- Tips for Writing Eating Disorder Treatment Plans and Progress Notes
Creating an effective eating disorder treatment plan is essential because eating disorders are complex conditions that require careful assessment and ongoing clinical attention. Therapists play a critical role in helping individuals recognize disordered eating patterns and work toward recovery through structured, individualized care. By developing a strong understanding of eating disorder signs and symptoms, clinicians can create clearer treatment plans and more accurate clinical notes that support better outcomes. Well-documented treatment plans also help practices operate more efficiently while maintaining compliance and continuity of care.
In this guide, we’ll walk through how to structure an effective eating disorder treatment plan, including treatment plan templates and real-world examples for common diagnoses such as anorexia nervosa and binge eating disorder.
Identifying and Recognizing Symptoms of Eating Disorders
Eating disorders impact almost a tenth of the population worldwide but are especially prevalent among certain groups, including young girls and athletes. Despite their prevalence, eating disorders are often tricky to spot. Because patients may not fully recognize the severity of an eating disorder or may hesitate to seek care, and because symptoms can present subtly, clinicians must carefully monitor for emerging signs, symptoms, and red flags.
While common in young girls and athletes, anyone can experience disordered eating behaviors, and they appear in many different ways. Eating disorders can significantly affect physical health, so clinicians must know when to pursue more intensive treatment or hospitalization.
Below are some common eating disorders and tips for identifying them.
Anorexia Nervosa
A patient with anorexia nervosa may starve themselves to lose or maintain weight lower than is normal for their height and age. The disorder's subtypes include the restricting type — which involves weight loss activities like dieting, fasting and excessively exercising — and the binge-eating/purging type, characterized by binging and purging behaviors such as vomiting or misusing laxatives and enemas.
This condition is severe and has the second-highest mortality rate of any psychiatric diagnosis, making early detection critical. Effects of anorexia can include suicide, starvation and complications from binging and purging activities. Patients with anorexia nervosa may have a strong fear of gaining weight and self-evaluation that is heavily influenced by body shape or weight.
The following symptoms may emerge as a result of anorexia nervosa:
- Low weight or weight fluctuations
- Amenorrhea, or a lack of menstrual periods
- Dizziness and fainting due to dehydration
- Weakness and fatigue
- Cold intolerance
- Brittle hair and nails
- Constipation, bloating and early satiety
- Stress fractures due to low bone mineral density or osteoporosis
When assessing for anorexia nervosa, clinicians should ask plenty of questions related to the above symptoms and pay special attention to concerns expressed by family members. Clinicians should also inquire about the patient's eating habits, attitude toward body image, menstrual history, weight loss patterns and exercise habits.
Bulimia Nervosa
Bulimia nervosa is characterized by eating high amounts of food in a short period of time, typically with the patient feeling a loss of control over their eating. When not binging, they may restrict themselves heavily to low-calorie foods. Binges are often secretive and come with feelings of shame or embarrassment. The patient usually follows binging with compensatory behaviors, such as vomiting, fasting, using laxatives or compulsively exercising to avoid gaining weight.
People of any weight can have bulimia nervosa, but those who are significantly underweight are more likely to have the binge-eating/purging type of anorexia nervosa. Like anorexia nervosa, the patient's self-evaluation is unjustifiably influenced by their body shape and weight.
Some physical signs of bulimia might include:
- Chronic sore throat.
- Dental problems due to the erosion of tooth enamel from vomiting.
- Heartburn and gastroesophageal reflux.
- Misuse of laxatives, diet pills or diuretics.
- Dizziness and fainting.
Bulimia nervosa can be harder to detect than anorexia nervosa. You may need to ask specific questions about the patient's eating habits. Screening tools can be helpful, as well as interviews with family members.
Other Eating Disorders
Other eating disorders to watch for include:
- Binge-eating disorder: Binge-eating disorder also involves losing control over eating habits and consuming large amounts of food. Unlike bulimia nervosa, it doesn't include purging, fasting or excessive exercise, and patients are often obese or overweight.
- Other specified feeding and eating disorders: This diagnosis refers to disturbances of eating behavior that may not fit neatly under the previous two disorders. For example, a patient who exhibits symptoms of anorexia nervosa but does not meet the weight criteria might have this diagnosis.
- Avoidant restrictive food intake disorder (ARFID): In ARFID, patients restrict the amount or type of food eaten but do not have concerns over weight or body image. They may avoid foods to an extreme level based on sensory characteristics, such as texture or smell. They may also feel anxiety over the consequences of eating. For example, they may avoid foods due to fear of choking, vomiting or experiencing an allergic reaction. Patients with ARFID may lose weight, become nutrient deficient or become dependent on nutritional supplements.
Download this Checklist for Identifying Eating Disorders
Eating Disorder ICD-10 Codes and Documentation Requirements
Accurate ICD-10 coding and thorough documentation are essential components of an effective eating disorder treatment plan. Because eating disorders often involve medical risk, insurance scrutiny, and comorbid mental health conditions, clinicians must ensure that diagnoses are clearly supported by clinical findings and consistently reflected across treatment plans and progress notes.
Common ICD-10 Codes for Eating Disorders
The following ICD-10 codes are frequently used when documenting eating disorders in outpatient behavioral health settings:
-
F50.0 – Anorexia nervosa
-
F50.01 – Anorexia nervosa, restricting type
-
F50.02 – Anorexia nervosa, binge-eating/purging type
-
F50.2 – Bulimia nervosa
-
F50.81 – Binge-eating disorder
-
F50.89 – Other specified eating disorder
-
F50.9 – Eating disorder, unspecified
Clinicians should select the most specific code that accurately reflects the client’s current presentation and update diagnoses as symptoms change over time.
Documentation Requirements to Support Medical Necessity
To support medical necessity and continuity of care, eating disorder documentation should clearly demonstrate the severity, frequency, and impact of symptoms. Treatment plans and progress notes should include:
-
A clear link between the diagnosis and presenting symptoms
-
Description of disordered eating behaviors and associated psychological distress
-
Functional impairment affecting daily life, relationships, or work
-
Measurable treatment goals and objectives tied to the diagnosis
-
Ongoing assessment of risk factors, including medical instability or compensatory behaviors
When treatment plans and progress notes consistently align with the diagnosed eating disorder, documentation is easier to defend during audits, utilization reviews, or insurance inquiries.
Maintaining Consistency Across Treatment Plans and Notes
Consistency is critical when documenting eating disorder treatment. The diagnosis, treatment goals, and interventions outlined in the treatment plan should be reflected in each progress note. Any changes in symptom severity, risk level, or clinical focus should prompt a timely update to both the diagnosis and the treatment plan.
Using structured documentation tools and templates can help clinicians maintain clarity, reduce administrative burden, and ensure compliance while focusing more time on patient care.
What Should Be Included in an Eating Disorder Treatment Plan?
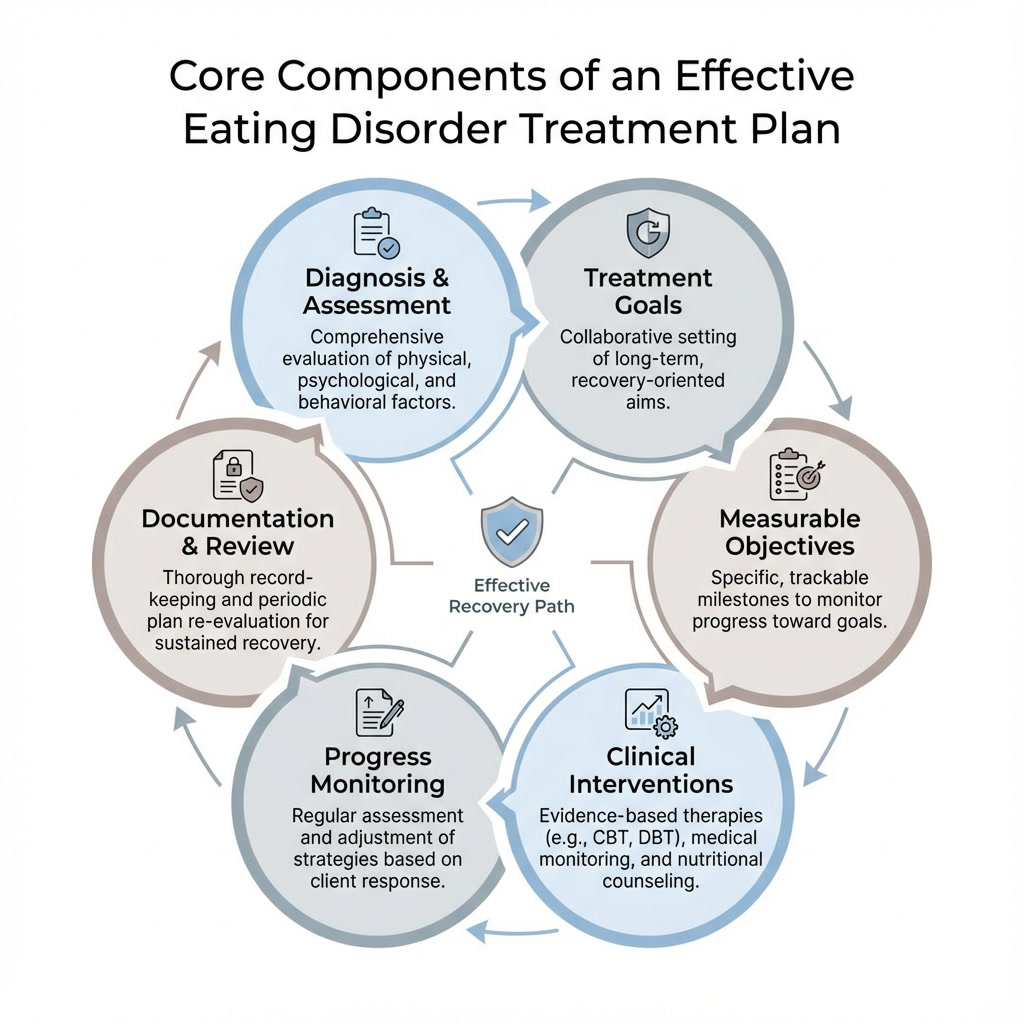
An effective eating disorder treatment plan should clearly outline the client’s diagnosis, clinical needs, and the specific goals and interventions that will guide care. Because eating disorders often involve both psychological and medical risk factors, treatment plans should be detailed, individualized, and regularly updated.
At a minimum, an eating disorder treatment plan should include:
-
Diagnosis and presenting concerns, such as anorexia nervosa, bulimia nervosa, or binge eating disorder
-
Measurable treatment goals related to eating behaviors, emotional regulation, and physical health
-
Short- and long-term objectives that define how progress will be evaluated
-
Clinical interventions, including psychotherapy modalities, nutritional counseling, and coordination with medical providers
-
Risk and safety considerations, especially when there is weight instability, purging behavior, or medical compromise
-
Plan for monitoring progress, including symptom tracking and reassessment timelines
Clearly documenting these elements supports continuity of care, medical necessity, and defensible clinical documentation.
Download an Eating Disorder Treatment Plan Example

Eating Disorder Treatment Plan Goals and Objectives
Treatment goals and objectives form the clinical foundation of an effective eating disorder treatment plan. While templates provide structure, clearly defined goals ensure that care remains individualized, measurable, and responsive to each client’s presentation. Well-written goals also help demonstrate medical necessity and guide day-to-day clinical decision-making.
Defining Treatment Goals
Treatment goals describe the broader clinical outcomes the client is working toward over time. In eating disorder treatment, goals often address both behavioral and psychological components of the disorder.
Common treatment goals may include:
-
Stabilizing eating patterns and reducing disordered behaviors
-
Improving emotional regulation and distress tolerance
-
Addressing distorted beliefs related to food, weight, and body image
-
Supporting physical and psychological safety
-
Building skills to reduce relapse risk
Goals should be client-centered, clinically appropriate for the diagnosis, and aligned with the client’s stage of change.
Writing Measurable Objectives
Objectives translate broader goals into specific, observable steps that allow clinicians to track progress over time. In an eating disorder treatment plan, objectives should clearly describe what will change, how progress will be measured, and within what timeframe.
Effective objectives are typically:
-
Specific – focused on clearly defined behaviors or skills
-
Measurable – observable or trackable through session data
-
Time-bound – associated with a realistic review period
Examples of well-written objectives may include:
-
Client will reduce frequency of binge eating episodes over a defined period
-
Client will demonstrate increased use of coping strategies during urges to restrict or binge
-
Client will challenge and reframe eating-disorder-related cognitive distortions in session
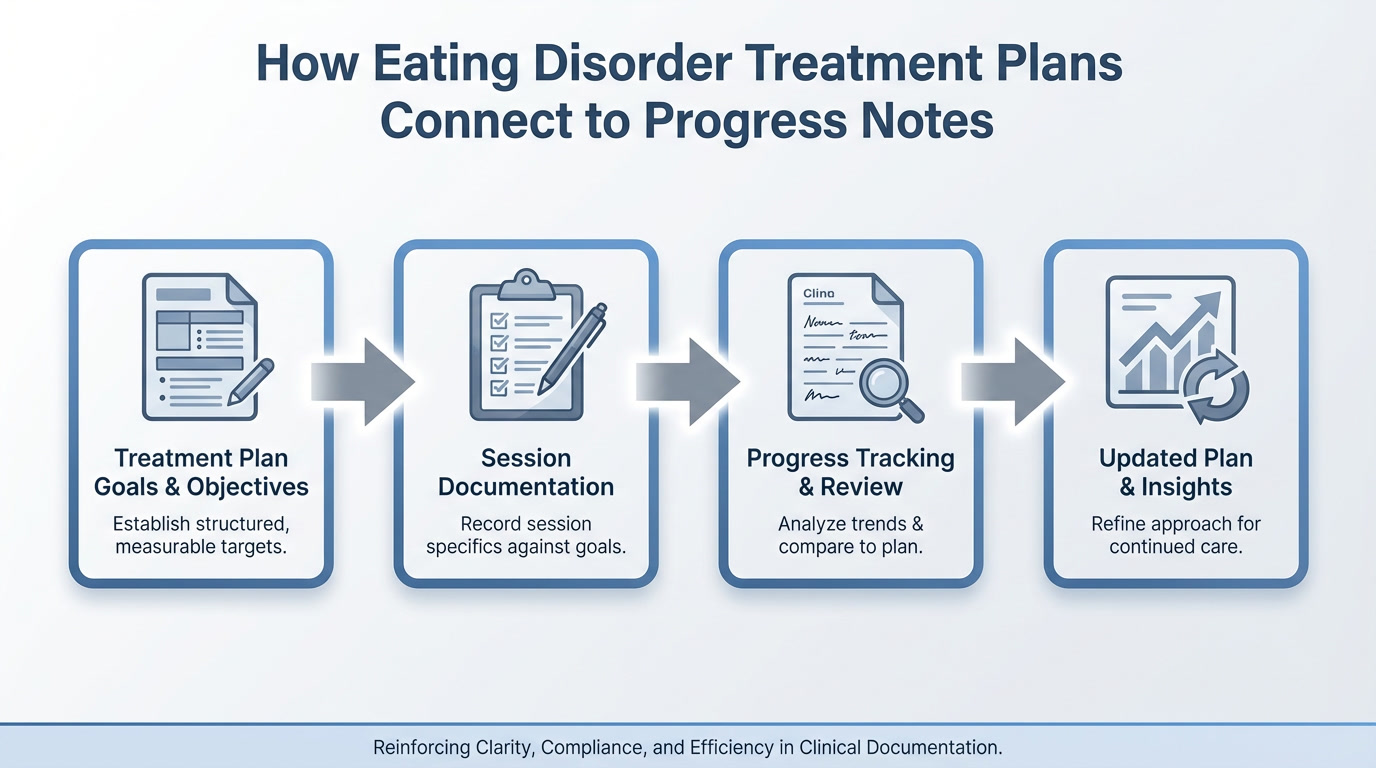
Aligning Goals and Objectives With Documentation
For documentation to remain clear and defensible, treatment goals and objectives should be consistently reflected in progress notes. Each session note should reference relevant objectives and describe observable progress, barriers, or clinical adjustments.
When goals, objectives, and progress notes are aligned, clinicians can more easily:
-
Monitor treatment effectiveness
-
Update treatment plans as symptoms change
-
Support continuity of care and compliance requirements
The following sections provide a structured treatment plan template and diagnosis-specific examples that show how these goals and objectives come together in practice.
Eating Disorder Treatment Plan Template
Below is a sample eating disorder treatment plan template that clinicians can adapt based on diagnosis, level of care, and client needs.
Diagnosis:
-
Primary diagnosis (e.g., Anorexia Nervosa, Binge Eating Disorder)
-
Co-occurring conditions (e.g., anxiety, depression)
Problem Statements:
-
Disordered eating behaviors impacting physical and psychological functioning
-
Distorted body image and maladaptive beliefs related to food and weight
Treatment Goals:
-
Restore and maintain healthier eating behaviors
-
Reduce eating-disorder-related thoughts and behaviors
-
Improve emotional regulation and body image
-
Support medical stability and relapse prevention
Objectives:
-
Client will demonstrate consistent meal patterns as defined by treatment team
-
Client will reduce frequency of bingeing, restricting, or purging behaviors
-
Client will identify and challenge distorted thoughts related to food and body image
Interventions:
-
Cognitive Behavioral Therapy (CBT or CBT-E)
-
Psychoeducation related to nutrition and eating behaviors
-
Skills training for emotion regulation and distress tolerance
-
Coordination with dietitian and medical providers as needed
Progress Monitoring:
-
Ongoing symptom tracking
-
Regular review of goals and objectives
-
Updates documented in progress notes
This format allows clinicians to maintain clarity while tailoring care to each individual client.
Eating Disorder Treatment Plan Examples
The following examples illustrate how treatment goals and interventions may vary based on diagnosis and symptom presentation. These examples are for educational purposes and should always be individualized.
Sample Treatment Plan for Anorexia Nervosa
Primary Goal: Stabilize eating behaviors and support medical and psychological recovery.
Objectives:
- Client will follow a structured eating plan as recommended by the treatment team.
- Client will demonstrate reduced fear-based avoidance of food.
- Client will engage in therapy to challenge distorted beliefs related to weight and control.
Interventions:
- Cognitive Behavioral Therapy focused on eating disorder cognitions.
- Collaboration with medical providers to monitor physical health.
- Psychoeducation regarding the effects of restriction on mental and physical functioning.
Progress Indicators:
- Increased consistency in eating patterns.
- Improved insight into eating-disorder-driven thoughts.
- Reduction in restrictive behaviors over time.
Binge Eating Disorder Treatment Plan Example
Primary Goal: Reduce binge eating episodes and improve regulation of eating behaviors.
Objectives:
- Client will identify emotional and situational triggers for binge eating.
- Client will practice alternative coping strategies during urges to binge.
- Client will develop a more balanced relationship with food.
Interventions:
- Cognitive Behavioral Therapy targeting binge-restrict cycles.
- Skills training for emotional regulation and impulse control.
- Mindfulness-based strategies related to hunger and fullness cues.
Progress Indicators:
- Decreased frequency of binge episodes.
- Improved awareness of triggers.
- Increased use of adaptive coping strategies.
Tips for Writing Eating Disorder Treatment Plans and Progress Notes
Once a treatment plan is in place, clinicians should incorporate these tips into their ongoing documentation process. Doing so helps ensure that progress notes clearly reflect treatment focus, support medical necessity, and demonstrate measurable progress over time.
1. Involve the Family System
Like many behavioral health problems, cognitive-behavioral therapy (CBT) and individual sessions are often beneficial therapy techniques for eating disorders. Still, many eating disorders stem from or are exacerbated by family environments that may reinforce unhealthy eating behaviors or invoke emotional responses. For example, a child with anorexia nervosa may have a parent constantly dieting or commenting on how their child shouldn't gain weight. A client with ARFID could have a spouse that wants them to "get over it."
In such situations, family therapy can help you and the client discuss their disorder with their family members. You might stress the severity of the disorder and discuss ways that the family can be more supportive of their loved one. They could start to remove harmful phrases from their vocabulary, help create healthy meals or check in with the client more often to provide accountability.
Even if family therapy isn't possible, ensure the client understands their home environment's impact. Provide tools for helping them stay resilient in less-supportive spaces or talk to their family members themselves about being supportive. Activities like these can help the client and their family build stronger connections. Many families are happy to help, but they need your guidance to get there.
2. Provide Specific Guidance Through Psychoeducation
Eating disorders often come from a place of externalization. Clients might build their perceptions of "healthy" and "normal" based on those around them, like parents or even media portrayals. They may seek acceptance and validation from others rather than themselves. With this externalized approach, clients might not have a good idea of what overcoming their disorder would look like.
Try to take an active role during eating disorder treatment by providing clear guidance — often called psychoeducation — and helping the client broaden their views. Focus on shifting ideas of external approval into internalized ideas that stand independently, regardless of what others do. This approach may be particularly useful for adolescents, who tend to be heavily influenced by others' experiences.
Activity-based therapy sessions can be beneficial in helping the client build stronger internal views of the world with the therapist's gentle influence.
3. Be Explicit About Unhealthy Behaviors
Similarly, many clients with eating disorders struggle to see what constitutes unhealthy behavior. Work with the client to make unhealthy behaviors explicit. You might create a list with the client of these behaviors, such as purging or limiting calories due to a fear of gaining weight. Provide examples of healthier alternatives and thinking patterns the client can work toward.
For example, instead of thinking, "This must look like a lot of food to anyone watching," you might ask your client to focus on how good the food looks or how much fun they're having with friends. Another approach might be to provide examples of healthy, well-rounded meals the client can incorporate into their diet.
4. Include Information from Other Professionals and Treatments
If your client's treatment involves input from other adults, such as dietitians or athletic coaches, include these comments and updates in your notes. Even if you do not have direct access to other providers' information, you can ask your client about their progress with them and update your notes accordingly. You'll also want to check in on progress with other treatment approaches, like group therapy or medication.
5. Use Eating Disorder Assessments
Include the results of eating disorder assessments in your notes. Some are designed for diagnosis, while others can help you keep tabs on the disorder during treatment and monitor progress. Some popular assessments include:
- The SCOFF Questionnaire: This screening questionnaire includes five questions about self-control, body image, weight loss and the role food plays in someone's life. It has a simple scoring system of one point for "yes" and zero points for "no," and two points or more suggest an eating disorder.
- Eating Disorder Examination Questionnaire - Short (EDE-QS): Another screener, this short questionnaire has 12 scaled questions, with higher scores corresponding to more severe symptoms.
- Eating Disorder Examination Questionnaire (EDE-Q): As the longer version of EDE-QS, this assessment includes 24 items to assess behaviors associated with eating disorders. It includes four subscales regarding restraint, eating concern, shape concern and weight concern.
- Eating Attitudes Test (EAT-26): EAT-26 has 26 questions about attitudes, feelings, beliefs and behaviors toward eating. It can be a useful assessment for ongoing treatment. It's a widely used assessment that can also serve as a screening tool.
6. Simplify Your Eating Disorder Documentation System
As with most behavioral health services, efficient and accurate documentation is essential when treating eating disorders. Writing clear, timely notes allows clinicians to spend more time focused on patient care while supporting continuity, compliance, and appropriate reimbursement. When documentation becomes overly time-consuming, it can interfere with both clinical effectiveness and practice sustainability.
Using documentation tools designed specifically for behavioral health can help streamline this process. ICANotes supports clinicians working with eating disorders through structured, diagnosis-driven templates and a primarily click-based note system that reduces reliance on free-text typing. Because notes are integrated directly within the ICANotes electronic health record (EHR), clinicians can easily reference prior assessments, treatment plans, and clinical history while documenting current sessions — helping ensure notes remain consistent, thorough, and clinically relevant.
Frequently Asked Questions: Eating Disorder Treatment Plans
How ICANotes Supports Eating Disorder Treatment Planning
ICANotes helps clinicians document eating disorder treatment plans and progress notes with structured, diagnosis-specific templates that support clinical clarity and consistency. By aligning treatment goals with session documentation, clinicians can more easily track progress, update plans, and support medical necessity across episodes of care.
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







