Blog > Treatment Strategies > Interventions for Anxiety: How to Choose the Right Technique for Each Client
Interventions for Anxiety: Evidence-Based Techniques for Anxiety Disorders
This clinician-focused guide breaks down the most effective interventions for anxiety disorders, including CBT, exposure therapy, mindfulness, and ACT. Learn how to choose the right intervention for each client using a practical framework for applying evidence-based anxiety treatment techniques in real-world sessions.

Last Updated: April 3, 2026


What You'll Learn
- The five core categories of interventions for anxiety disorders — cognitive, behavioral, somatic, psychoeducational, and lifestyle — and how to apply each in clinical practice
- How to choose and match the right intervention to each client using a practical, in-session decision framework
- Evidence-based techniques including CBT, exposure therapy, ACT, and mindfulness interventions for anxiety
- Real-world tools to improve client engagement, including symptom tracking, coping strategies, and structured prompts
- How to document anxiety interventions, treatment plans, and progress efficiently and compliantly using ICANotes
Contents
- How to Choose the Right Intervention for Anxiety
- How to Match Interventions for Anxiety to Each Client
- Understanding Anxiety Disorders and Clinical Presentation
- Core Therapeutic Interventions for Anxiety Disorders
- Using Anxiety Assessment Tools to Measure Treatment Outcomes
- FAQ: Interventions for Anxiety
- How ICANotes Supports Anxiety Intervention Documentation
Anxiety is one of the most common mental health conditions in the United States, affecting nearly 20% of adults each year. For clinicians, the challenge isn’t just understanding anxiety — it’s knowing which interventions for anxiety will be most effective for each individual client.
With so many evidence-based options available — from cognitive behavioral therapy (CBT) and exposure therapy to mindfulness and acceptance-based approaches — selecting the right technique can feel overwhelming. The most effective treatment plans don’t rely on a single method, but instead match therapeutic interventions for anxiety disorders to a client’s specific presentation, symptoms, and level of functioning.
This guide breaks down the most effective clinical interventions for anxiety into five core categories: cognitive, behavioral, somatic, psychoeducational, and lifestyle-based strategies. More importantly, it shows you how to apply them in real-world settings — so you can move confidently from assessment to intervention.
If you’re looking for a structured way to decide which intervention to use, you can also download our anxiety intervention cheat sheet for clinicians — a quick-reference tool designed to help you match the right technique to each client’s needs. The key is matching the right intervention to the client’s presentation. Here’s a simple framework you can use.
How to Choose the Right Intervention for Anxiety
Not every client with anxiety needs the same treatment approach. The most effective interventions for anxiety depend on what is driving the client’s distress, how symptoms show up in daily life, and whether there are complicating factors such as trauma, depression, substance use, or limited insight.
A client whose anxiety is fueled by catastrophic thinking may respond well to cognitive restructuring and other CBT interventions for anxiety, while a client whose life has narrowed because of avoidance may benefit more from graded exposure. For clients whose symptoms are primarily physical — such as panic, muscle tension, shortness of breath, or hyperarousal — somatic strategies like breathing exercises, grounding, and relaxation training may be a better entry point. And when a client is early in treatment or struggles to understand their anxiety cycle, psychoeducation and symptom tracking can build the foundation for more advanced work.
The goal is not to choose one intervention category forever. In practice, clinicians often begin with the pathway that best matches the client’s primary presentation, then adjust over time based on outcomes, engagement, and comorbid needs. Using this kind of structured decision-making can make your therapeutic interventions for anxiety disorders more targeted, measurable, and effective.
Use this framework to match the client’s primary presentation with the most effective intervention pathway. Most clients benefit from a blended approach, but starting with the dominant pattern improves engagement and outcomes.
Racing thoughts, catastrophizing, rumination, “what if” loops, overthinking.
CBT, cognitive restructuring, journaling, behavioral experiments
Avoiding situations, people, or triggers; reliance on safety behaviors.
Graded exposure, in vivo/imaginal exposure, skills training
Panic, tension, shortness of breath, hyperarousal, sleep disruption.
Breathing, grounding, relaxation, mindfulness techniques
Limited understanding of anxiety cycle, new to therapy, low coping awareness.
Psychoeducation, symptom tracking, structured homework
Poor sleep, high caffeine, inactivity, inconsistent routines, overstimulation.
Sleep hygiene, movement, routine stabilization, nutrition changes
Consider comorbid depression, trauma history, substance use, developmental factors, or treatment resistance. Modify pacing, integrate modalities, and reassess regularly.
How to Match Interventions for Anxiety to Each Client
Choosing an intervention category is only the first step. In practice, effective treatment requires clinicians to adapt and combine interventions for anxiety based on each client’s presentation, comorbidities, and response to treatment over time.
Match the primary driver of anxiety (cognitive, behavioral, somatic) before layering additional techniques.
Combine CBT, exposure, mindfulness, or ACT techniques to address multiple symptom pathways.
Integrate behavioral activation, trauma-informed pacing, or substance use considerations as needed.
Use tools like the GAD-7 to track progress and adjust interventions when improvement plateaus.
In real-world practice, clinicians rarely rely on a single technique. For example, a client with social anxiety may begin with graded exposure, while also using cognitive restructuring to challenge distorted beliefs and mindfulness strategies to regulate physiological symptoms during exposure exercises. Similarly, clients with comorbid depression may need behavioral activation integrated alongside anxiety-focused interventions to improve motivation and engagement.
Treatment planning should remain flexible. If a client is not responding to a chosen intervention after several sessions, clinicians should reassess the underlying drivers of anxiety and consider shifting approaches or integrating additional modalities. Measurement tools like the GAD-7 can help guide these decisions by providing objective markers of progress.
Ultimately, the most effective therapeutic interventions for anxiety disorders are those that evolve alongside the client’s progress and needs.
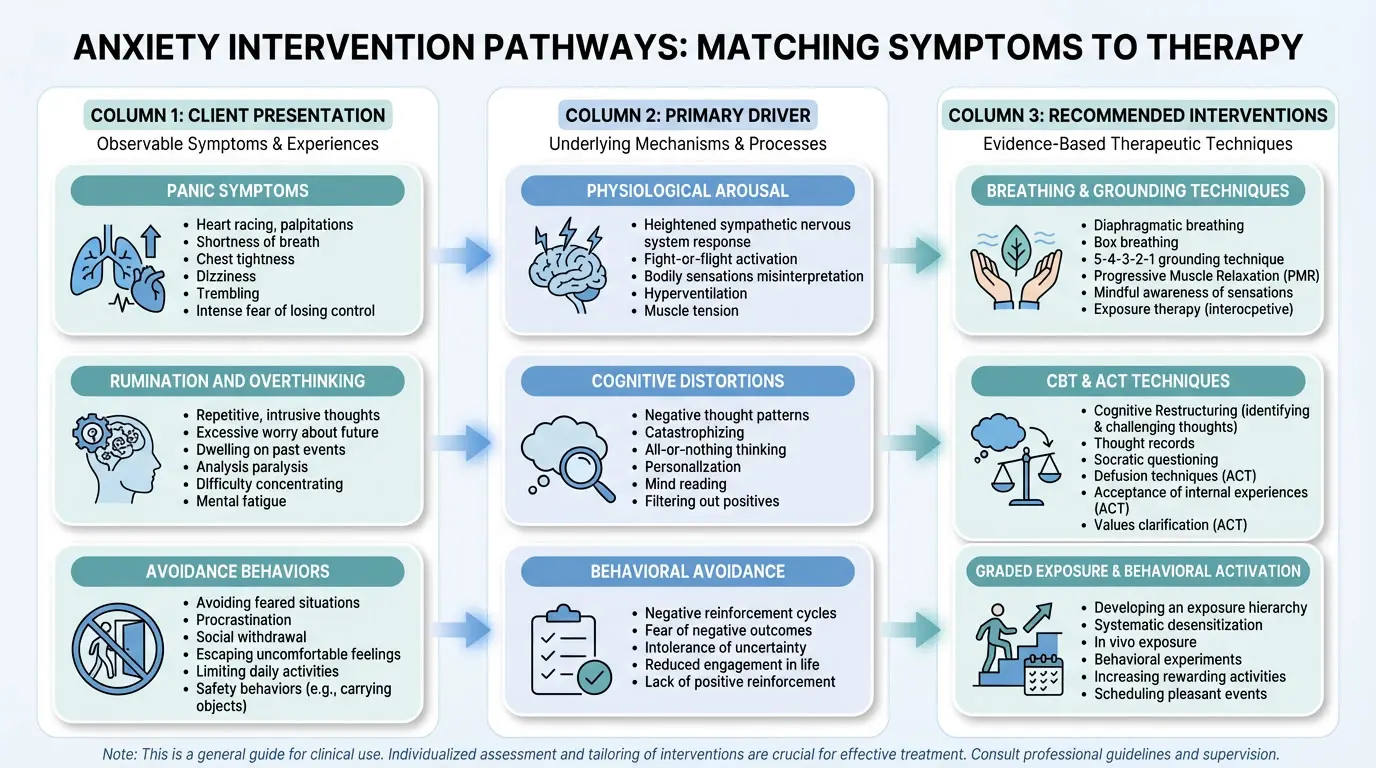
Understanding Anxiety Disorders and Clinical Presentation
Anxiety can have diverse presentations, but it generally involves fear, persistent worry, and anticipatory dread. While mild anxiety is necessary to keep us alert and prepared for danger, too much can impair our daily ability to function. Patients may present with cognitive symptoms (racing thoughts, rumination), emotional symptoms (irritability, dread), and physical symptoms (muscle tension, rapid heartbeat, insomnia).
Common anxiety disorders include Generalized Anxiety Disorder (GAD), Social Anxiety Disorder, Panic Disorder, Specific Phobias, Obsessive-Compulsive Disorder (OCD), and Post-Traumatic Stress Disorder (PTSD). Anxiety frequently co-occurs with depression, bipolar disorder, ADHD, trauma histories, substance use, and broader environmental stressors. Clinicians must consider these related diagnoses when selecting therapeutic interventions for anxiety disorders. You can explore these dynamics further in our guides to anxiety and substance use, the relationship between anxiety and trauma, and climate anxiety.
Using standardized tools can help track symptom progression over time and inform treatment decisions — especially when paired with structured approaches like those covered in our anxiety assessment tools guide.
Core Therapeutic Interventions for Anxiety Disorders
Interventions for anxiety disorders can be divided into five categories: cognitive, behavioral, somatic, psychoeducational, and lifestyle-based techniques. The following sections detail how these categories function and which evidence-based strategies fall into each one. For many clients, an integrated approach — blending cognitive, behavioral, somatic, and lifestyle interventions — yields the best outcomes, particularly when progress is measured regularly and interventions are adjusted as needed.
CBT Interventions for Anxiety: Techniques Clinicians Can Use in Session
Cognitive-behavioral therapy (CBT) is one of the most widely researched and effective therapeutic interventions for anxiety disorders. CBT interventions for anxiety focus on identifying, understanding, and reframing distorted thought patterns to achieve desired behavioral outcomes. Because anxiety often stems from cognitive distortions — catastrophizing, black-and-white thinking, emotional reasoning — CBT gives clients structured tools to interrupt these cycles.
How CBT Works in Anxiety Treatment
CBT interventions for anxiety typically follow a structured format. The clinician helps the client identify automatic anxious thoughts, evaluate the evidence for and against those thoughts, and develop a more balanced perspective. This process is supported by tools like thought logs, behavioral experiments, and exposure exercises. CBT can be delivered individually, in group formats, or through structured digital programs.
CBT Thought Log Example
A client records the triggering situation, the automatic thought (“I’m going to fail”), the evidence for and against that thought, and a replacement thought (“I’ve prepared thoroughly and have passed before”). Over time, this practice helps clients recognize patterns in their thinking and develop greater cognitive flexibility.
CBT Techniques Commonly Used for Anxiety
Cognitive restructuring: Clients learn to identify and challenge cognitive distortions using Socratic questioning (“What evidence supports this fear?”) and reappraisal techniques.
Behavioral experiments: Clients test anxious predictions against real-world outcomes. For example, a client who believes “everyone will judge me” might agree to initiate a conversation and compare the predicted outcome to the actual result.
Exposure with cognitive processing: CBT frequently integrates exposure techniques with thought challenging, helping clients confront feared situations while simultaneously restructuring the beliefs that maintain avoidance.
Homework assignments: Between-session activities such as thought records, relaxation practice logs, and behavioral activation tasks reinforce progress and build self-efficacy.
For clinicians who want to implement CBT systematically as part of a broader treatment strategy, our guide to building an anxiety treatment plan covers how to align CBT interventions with SMART goals and measurable outcomes.
Stop Guessing Which Anxiety Intervention to Use
When a client presents with anxiety, choosing the right intervention can feel unclear — especially when symptoms overlap.
This clinician-designed cheat sheet gives you a fast, structured way to match interventions to presentation—so you can move confidently from assessment to action.
- Decision flowchart for selecting interventions
- CBT, exposure, ACT, and mindfulness prompts
- Ready-to-use scripts for real sessions
- Built for busy clinicians—not theory-heavy
Download it free and use it in your very next session.

Cognitive Interventions for Anxiety: Thought Restructuring and ACT Techniques
Beyond structured CBT programs, several cognitive techniques can be used as standalone interventions or integrated into a broader treatment plan. These approaches help clients identify, challenge, and reframe the unhelpful thought patterns that drive anxiety.
Identify and reframe distorted thinking patterns such as catastrophizing and black-and-white thinking.
Help clients change their relationship to anxious thoughts rather than trying to eliminate them.
Build insight into anxiety triggers, emotional responses, and recurring thought patterns.
Thought Challenging and Cognitive Restructuring
This technique helps clients take a step back from automatic anxious thoughts and evaluate them more rationally. Clinicians may use Socratic questioning ("What evidence supports this fear?") or work with clients to identify cognitive distortions such as black-and-white thinking or emotional reasoning. For instance, a client afraid of being bitten by a spider might explore the actual rarity of dangerous spiders in their region and develop a more balanced belief.
Acceptance and Cognitive Flexibility
Acceptance and Commitment Therapy (ACT) and Mindfulness-Based Cognitive Therapy (MBCT) teach clients to accept difficult thoughts and emotions without judgment. Instead of fighting anxious thoughts, clients learn to observe them with curiosity and refocus on actions that align with their values. This approach promotes psychological flexibility, especially for clients with chronic or treatment-resistant anxiety. For clinicians looking to implement ACT more systematically, our ACT for anxiety disorders guide provides practical techniques and examples.
Journaling and Emotional Processing
Structured journaling allows clients to identify anxiety triggers, log their emotional reactions, and track recurring thought patterns. Prompts such as "What was I afraid of today and how did I cope?" help clients build insight and connect thoughts to behaviors.
Behavioral Interventions for Anxiety: Exposure Therapy and Anxiety Treatment Techniques
Behavioral interventions reduce anxiety by helping clients confront feared situations, interrupt avoidance cycles, and build practical coping skills. These action-oriented anxiety treatment techniques are especially effective for phobias, social anxiety, panic-related avoidance, OCD, and other conditions in which avoidance reinforces distress.
Systematically helps clients confront anxiety-provoking stimuli instead of avoiding them.
Best for: Phobias, social anxiety, PTSD, OCD, and panic-related avoidance
Uses a fear hierarchy to move from lower-intensity exposures to more difficult situations over time.
Best for: Building confidence gradually while reducing overwhelm
In vivo exposure targets real-life feared situations, while imaginal exposure helps clients process feared scenarios mentally.
Best for: Situations that can be faced directly or safely revisited through visualization
Combines exposure with relaxation training so anxiety triggers become paired with calming responses instead of fear.
Best for: Clients who benefit from structured pacing and body-based regulation during exposure work
Group-based interventions normalize symptoms, reduce isolation, and let clients practice skills in a social context.
Best for: Social anxiety, generalized anxiety, and clients who benefit from peer modeling and validation
Helps clients build practical supports such as coping cards, sensory tools, worksheets, and emotion regulation skills.
Best for: Strengthening self-efficacy and improving follow-through between sessions
Exposure Therapy
Exposure therapy involves systematically helping clients confront anxiety-provoking stimuli. It is especially effective for phobias, social anxiety, PTSD, and OCD. A client might begin with minor exposures — like viewing a photo of a feared object — and work toward more intense experiences, such as direct interaction. Combining exposure with relaxation training, often called systematic desensitization, can help pair anxiety triggers with calming responses.
Graded Exposure Plan Example
A client with social anxiety might rank a fear hierarchy from lower-intensity tasks, such as greeting a neighbor, to higher-intensity situations, such as giving a presentation. Weekly exposure assignments can then be tracked and debriefed in session, with each step building confidence for the next.
In Vivo and Imaginal Exposure Techniques
In vivo exposure refers to confronting real-life feared situations, while imaginal exposure involves mentally visualizing distressing scenarios. For example, a client with PTSD might repeatedly recount a traumatic event in a safe setting, allowing desensitization over time. These methods require appropriate training, pacing, and clinical support.
Group Therapy and Peer Support
Group-based interventions can normalize clients’ experiences and reduce isolation. Group CBT programs or support groups help clients learn coping strategies from peers, practice exposure in social contexts, and receive validation. These formats are particularly effective for clients with social anxiety or generalized anxiety.
Skills Training and Coping Toolkits
Helping clients build a personalized set of coping tools can enhance self-efficacy. These may include cue cards with positive affirmations, sensory tools like fidget objects, and structured worksheets for reframing anxious thoughts. Clinicians might also teach practical skills such as assertiveness, time management, or distress tolerance.
Somatic Interventions for Anxiety: Mindfulness and Relaxation Techniques
Somatic techniques target the body’s stress response through mindfulness, relaxation, and movement-based practices. By calming the nervous system, these therapeutic interventions for anxiety help clients gain control over the physiological symptoms of anxiety disorders.
Help clients stay grounded in the present moment and respond to anxious thoughts with less reactivity.
Slow physiological arousal by activating the parasympathetic nervous system during moments of stress.
Reduce physical tension by helping clients notice and release muscle tightness systematically.
Use calming mental imagery to shift attention away from distress and support relaxation.
Provide nonverbal pathways for processing anxiety through art, music, movement, or sensory expression.
Mindfulness and Acceptance Strategies
Mindfulness practices help clients anchor their awareness in the present moment rather than becoming consumed by feared future outcomes. Techniques such as guided meditation, body scans, grounding exercises, and present-moment observation can reduce reactivity and improve emotional regulation. These approaches are especially useful for clients who feel overwhelmed by rumination, panic symptoms, or chronic hypervigilance. ACT often incorporates mindfulness strategies to help clients stay grounded during distress without struggling against internal experiences.
“Breathe in for four counts… hold… and breathe out slowly. Notice the ground beneath your feet. Let your thoughts pass like clouds across the sky.”
Relaxation Training
Relaxation training targets the physiological symptoms of anxiety by helping clients regulate breathing, muscle tension, and autonomic arousal. Diaphragmatic breathing can activate the parasympathetic nervous system, while progressive muscle relaxation helps clients identify and release chronic tension patterns. Guided imagery and visualization can also provide a structured way to shift attention toward calming sensations and environments. These practices are often most effective when rehearsed in session and assigned for regular use between sessions.
Creative and Expressive Therapies
Creative and expressive approaches can offer clients a nonverbal way to process anxiety, especially when emotional experiences feel difficult to articulate directly. Art therapy, music therapy, and movement-based activities may support emotional expression, regulation, and insight. While clinicians may refer clients to credentialed creative arts therapists for more formal treatment, general interventions such as drawing an image of anxiety, externalizing worry through metaphor, or using movement to release physical tension can still be useful adjunctive tools.
Psychoeducational Interventions for Anxiety: Education and Symptom Tracking
Psychoeducational interventions help clients understand how anxiety works and give them concrete tools for recognizing symptoms, tracking patterns, and applying coping strategies between sessions. These techniques can improve engagement, reduce shame, and lay the groundwork for more targeted therapeutic work.
Help clients understand how thoughts, emotions, body sensations, and behaviors interact to maintain anxiety.
Use journals, logs, or apps to identify triggers, symptom intensity, and patterns over time.
Reinforce skills between sessions with worksheets, reflection prompts, and structured practice.
Teach caregivers how to support coping skills without reinforcing avoidance or over-reassurance.
Encourage structured use of apps, worksheets, or guided tools that support skill practice and self-monitoring.
Psychoeducation and Symptom Tracking
Educating clients about the physiological and psychological roots of anxiety can reduce shame and help them understand why symptoms persist. Clinicians might explain the fight-or-flight response, walk clients through the anxiety cycle, or use a simple body map or stress diagram to illustrate how anxiety shows up physically and cognitively. Encouraging clients to track symptoms in a journal, worksheet, or app can also help identify triggers, measure intensity, and monitor change over time.
Homework and Digital Tools for Anxiety Management
Assigning between-session activities helps reinforce learning and supports skill generalization outside the therapy room. These activities may include thought records, relaxation practice logs, exposure worksheets, or guided reflection prompts. Some clients may also benefit from mood-tracking apps, coping reminders, or other digital tools that encourage consistent practice and self-awareness between sessions.
Parental Involvement in Pediatric Cases
For children and adolescents with anxiety, caregiver involvement can be an important part of treatment. Parents and caregivers can support progress by reinforcing coping skills, modeling calm behavior, and avoiding patterns that unintentionally strengthen avoidance. Psychoeducation can help families understand how reassurance, accommodation, or rescuing behaviors may maintain anxiety over time, while collaborative coaching can promote independence and skill use.
Reinforce independence by encouraging the child to try the anxiety-provoking task before offering reassurance.
Lifestyle Interventions for Anxiety: Sleep, Exercise, and Daily Habits
Lifestyle-focused interventions address the foundational habits that influence emotional well-being. Encouraging healthy sleep, nutrition, and physical activity can significantly enhance anxiety management and overall treatment outcomes.
Exercise, Diet, and Sleep Hygiene
Lifestyle factors strongly influence anxiety symptoms. Regular exercise (even short walks) releases endorphins and reduces cortisol. A balanced diet with stable blood sugar supports mood regulation, while consistent sleep patterns improve cognitive functioning. Clinicians can help clients identify barriers (e.g., time constraints, poor routines) and build realistic habits.
Use this quick-reference table to identify the most appropriate intervention category based on your client’s presentation.
Summary of Therapeutic Interventions for Anxiety by Category
Using Anxiety Assessment Tools to Measure Treatment Outcomes
Standardized anxiety assessment tools can help clinicians measure anxiety severity, track treatment outcomes, and support documentation. Common assessments include the Generalized Anxiety Disorder-7 (GAD-7), Depression Anxiety Stress Scales (DASS-21), Zung Self-Rating Anxiety Scale, and Hamilton Anxiety Rating Scale (HAM-A). These tools can be administered during intake, periodically during treatment, and at discharge.
Related Resources for Clinicians
Continue building your anxiety treatment toolkit with these in-depth clinical guides on assessment, treatment planning, and specialized interventions:
- → Anxiety Assessment Tools for Clinicians: GAD-7, BAI, & More
- → Anxiety Treatment Plan: Goals, SMART Objectives & Interventions
- → ACT for Anxiety Disorders: A Practical Guide for Clinicians
- → Anxiety and Substance Use: Breaking the Cycle
- → Understanding the Relationship Between Anxiety and Trauma
- → Treating Clients with Climate Anxiety: Integrating Eco-Therapy into Practice
Frequently Asked Questions About Interventions for Anxiety
What are the most effective interventions for anxiety disorders? +
How do you choose the right intervention for anxiety? +
What are the best CBT interventions for anxiety? +
Which anxiety therapy techniques work quickly in session? +
What should clinicians do when anxiety does not respond to treatment? +
What assessment tools help track anxiety treatment progress? +
How ICANotes Supports Anxiety Intervention Documentation
High-quality documentation is essential when delivering structured interventions for anxiety disorders. ICANotes, an EHR designed specifically for behavioral health providers, offers:
- Built-in anxiety assessments like the GAD-7
- Templates for CBT, ACT, exposure therapy, and psychoeducation
- Progress note and treatment plan templates tailored to behavioral interventions
Effective anxiety treatment requires a thoughtful combination of clinical skill and supportive tools. Whether you're using cognitive restructuring, exposure therapy, or mindfulness practices, your interventions are more powerful when backed by strong documentation and organization.
Get started with a free trial of ICANotes today — no credit card required — and see how a behavioral health EHR built for your needs can elevate your work with anxious clients.
Turn Anxiety Interventions Into Clean, Defensible Notes
Choosing the right intervention is only half the work. Documenting it clearly and efficiently is what supports reimbursement, compliance, and continuity of care.
ICANotes helps you translate CBT, exposure, mindfulness, and other interventions for anxiety into structured, audit-ready documentation in minutes.
- Pre-built templates for anxiety interventions
- Faster progress notes with clinical language built in
- Integrated rating scales like GAD-7
- Supports medical necessity and compliance
Start your free 30-day trial — no credit card required.
Takes less than 60 seconds to get started
Related Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.





