Outcome Measurement Tools for
Behavioral & Mental Health Clinicians
What is Outcomes Measurement?
In behavioral and mental healthcare settings, outcome measures are tools that help determine the impact of a service or intervention on a patient's health status. According to the Donabedian model, outcome measures are the third of three types of healthcare quality measures — accompanying structural measures and process measures.
Implementing outcome measures can help increase treatment effectiveness and create meaningful change for your patients. Outcome measures also help put quantitative data behind mental and behavioral health transformation that can be challenging to evaluate otherwise. The time and effort you invest in outcomes measurement can give you the knowledge to better serve your patients and grow as a facility.
Start Free Trial
Why Measuring Outcomes is Important
in Behavioral and Mental Healthcare
According to the Joint Commission on Accreditation of Healthcare Organizations (JCAHO), measurement-based care provides several valuable insights within behavioral and mental healthcare, including:
- The knowledge of whether the treatments an organization or individual practitioners provide are having a positive and significant impact on the patients served.
- Help prevent the failure of care, treatment, or services.
- Help patients evaluate their progress in a quantifiable manner throughout care, treatment, or service.
- Increased knowledge of developments for both patient and practitioner that can help providers adjust or maintain current treatment.
- Better patient outcomes and higher quality care.
Though measuring outcomes is favorable for the patient and facility growth, it also generates valuable data for other parties. Measuring outcomes also helps respond to the movement of assessing care on a population level and helps illuminate the value of specific treatments amid increasing healthcare costs. Regardless, outcome measures help answer the question patients, insurers, and more ask: Does this treatment work?
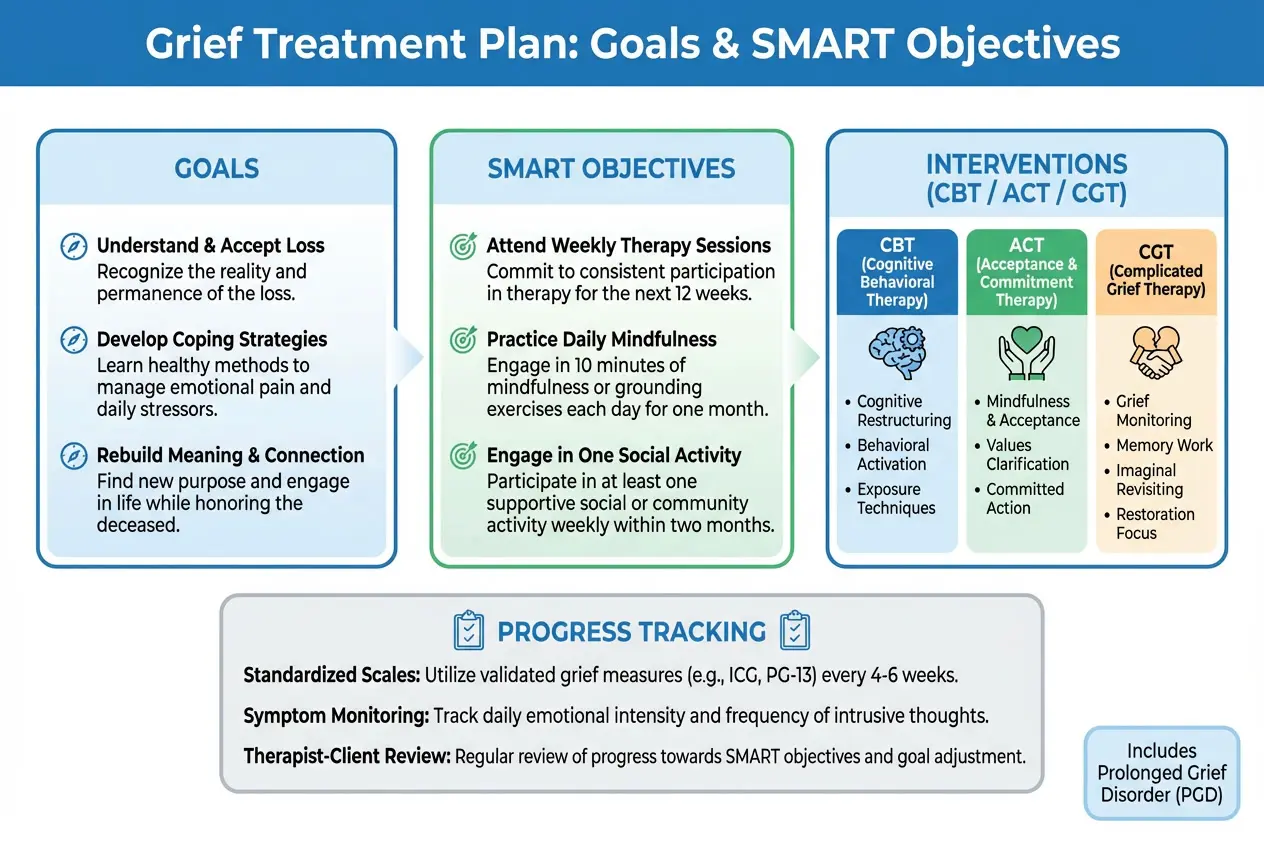
4 Types of Healthcare Outcome Measures
What are outcome measures in healthcare? They look different for each type of healthcare facility. There are no "standardized" measures to begin with — but your patients and courses of treatment can help determine what types of outcome measures might be relevant in your facility. Though these measurements vary, a study of outcome measures conducted by BMC Psychiatry found four general domains.
There are many assessments for a variety of topics within these four domains. The Kennedy Forum recommends the following measure and topic combinations as examples of outcome measures in healthcare for adult patients.
- Depression: PHQ-9
- Panic Attacks: PDSS_SR
- Mania: Altman Scale
- Alcohol: Audit-C
- Anxiety: GAD-7
- Drug Abuse: DAST-10
- PTSD: PCL
- Somatization: PHQ-15
You can and should adapt outcome measures to the symptoms and illnesses treated in your patients. Tracking outcomes across the four common domains can provide quantitative evidence to support progress or the need for treatment adjustments. A key to executing outcome measurements is creating an approach tailored to your organization.
Measuring Outcomes in Mental & Behavioral Healthcare
Measuring behavioral and mental health outcomes requires a mix of patient input — typically through patient-reported outcome measures — facility analysis and outcome measurement tools. The Journal of the World Psychiatry Association offers the following recommendations for implementing outcome measures.

Compile a portfolio of measures: Identify valid measures for assessing outcomes across a spectrum of common conditions, patient populations, and levels of healthcare access.

Develop common data elements: Standardize these for diagnoses and clinical outcome measures, and add them to an electronic health record (EHR) system.
Assess potential gaps: Examine measures to ensure no subpopulations or groups are not getting assessed effectively. If you discover gaps, adapt measures accordingly.

Commit to investment: Facility leaders need to invest in and act on their commitment to outcome measures to communicate to staff — who will likely collect and measure data — the importance of the system.

Use measures routinely: Incorporate implemented measures into the facility culture, EHR, and treatment plans. Regular outcome measure use contributes to quality improvements, whereas infrequent use does not provide the same results.
This process is detailed, but the results allow you to provide better care, garner patient and payer trust and comply with organizational standards.
Frequently Asked Questions About Outcome Measurement
Common questions about outcome measurement include the following.
JCAHO and CARF Compliance in EHRs
When measuring outcomes in an EHR, compliance is essential. There is little standardization for EHR systems, but several regulations — such as HIPAA — pose significant fines for EHR compliance violations. Because there are no HIPAA "certifications" for EHRs, you must trust your EHR vendor to implement a system that complies with relevant regulations.
In addition to HIPAA compliance, it's vital to use a CARF- and JCAHO-compliant EHR. These accreditation organizations endorse businesses they trust for quality care, which helps patients decide who they'll trust for their treatments. CARF and JCAHO require their endorsed facilities to supply accurate data, like outcome measures, to demonstrate their effectiveness and service satisfaction among their patients.
Compliance in your EHR and outcome measurement does not eliminate the potential for violation. Clinicians and staff need to remain vigilant when handling patient data and maintaining accreditation. However, tracking your outcome measures with EHR software such as ICANotes can help you remain compliant and accredited. ICANotes stays ahead of regulation updates and is ONC-certified to be compliant and comprehensive.
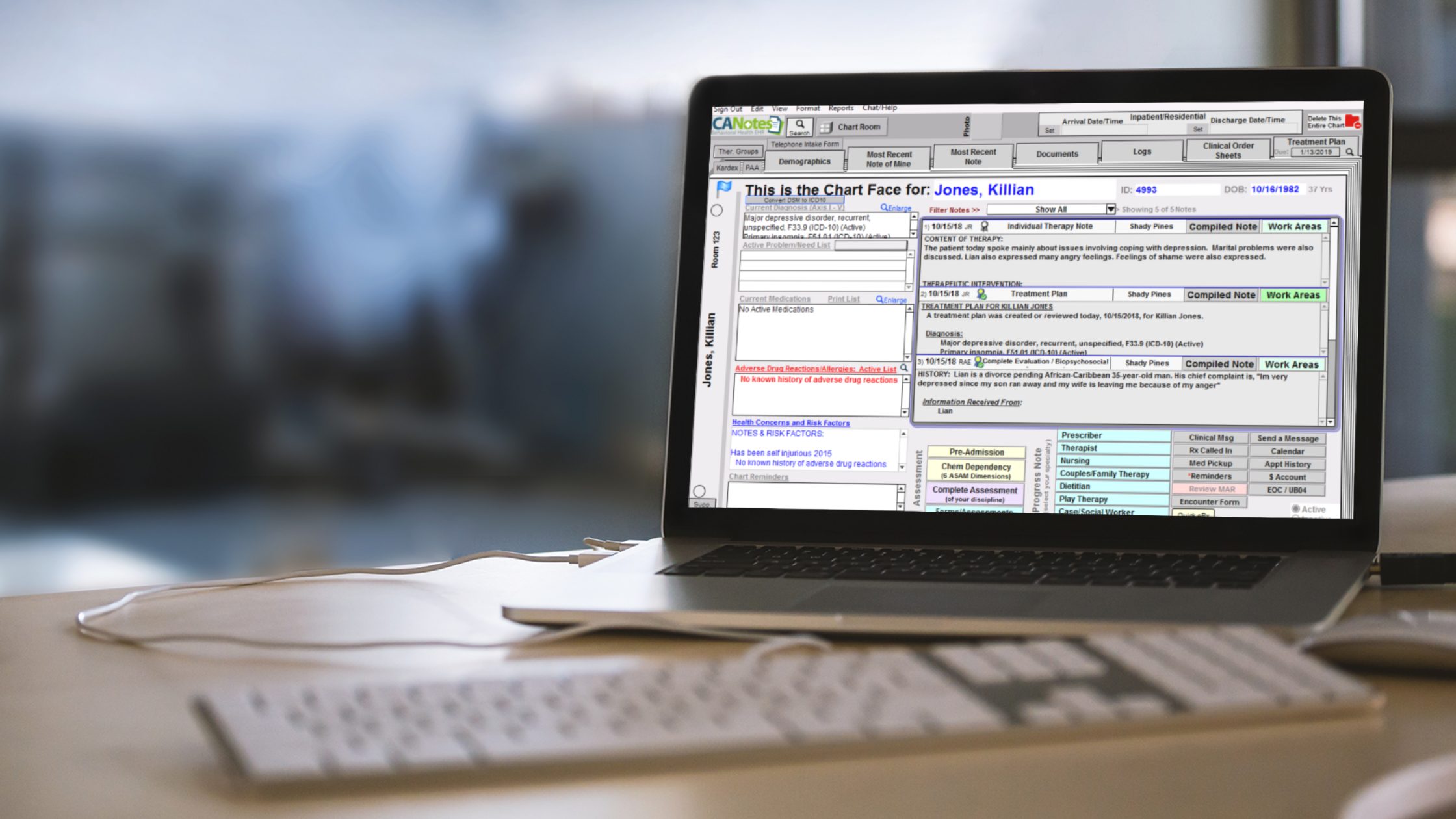
Behavioral Health EHR You Can Trust
ICANotes is an intuitive, accessible, and time-saving behavioral health EHR system. Our product is CARF- and JCAHO-compliant and features a variety of security precautions that comply with HIPAA regulations.
Posts Related to Outcome Measurement
Intuitive, Accessible, Time-Saving
ICANotes - the only EHR software that actually thinks like a clinician.