Blog > Documentation > How to Write a Mental Health Treatment Plan: Examples, Goals & Templates
How to Write a Mental Health or Behavioral Health Treatment Plan: Examples, Goals & Templates
A mental health treatment plan is a structured, individualized roadmap that guides clinical care, defines measurable goals, and supports both patient outcomes and documentation requirements. In this comprehensive guide, we break down how to create an effective behavioral health treatment plan, including essential components, SMART goals and objectives, condition-specific examples, and best practices for compliance and reimbursement. Whether you're a therapist, psychiatrist, or social worker, this resource provides the tools and templates needed to build clear, actionable treatment plans that improve care quality and streamline documentation.

Last Updated: April 15, 2026


What You'll Learn
- What a mental health treatment plan is—and why it matters for outcomes and compliance
- The essential components every behavioral health treatment plan should include
- How to write SMART goals and measurable objectives that support progress and documentation
- Condition-specific treatment plan goals and objectives for anxiety, depression, trauma, and substance use
- How treatment planning differs for counselors, psychiatrists, and social workers
- Practical tips for collaboration, compliance, and insurance-ready documentation
- How ICANotes simplifies and speeds up behavioral health treatment planning
Contents
- What Is a Mental Health Treatment Plan?
- What Is the Purpose of a Treatment Plan?
- Key Components of a Mental Health Treatment Plan
- Mental Health Treatment Plan Goals and Objectives
- How to Write a Treatment Plan for Mental Health
- Treatment Plan Templates by Discipline
- Key Considerations for Creating Personalized Mental Health Treatment Plans
- Mental Health Treatment Plan Tips
- Mental Health Treatment Plan Checklist
- Insurance Documentation and Medical Necessity
- How a Mental Health Treatment Plan Complements Other Clinical Notes
- How ICANotes Streamlines Mental Health Treatment Plans
- FAQ: Mental Health Treatment Plans
A well-crafted behavioral health treatment plan is one of the most important documents a clinician creates. It establishes a clear, shared roadmap for care — setting the direction for therapy, anchoring every session to measurable goals, and providing the documentation trail that supports clinical decisions, insurance reimbursement, and regulatory compliance.
Whether you're a therapist in private practice, a psychiatrist in an agency setting, or a social worker managing complex caseloads, this guide covers everything you need to know about writing effective mental health treatment plans — from core components and goal-setting frameworks to condition-specific examples, profession-specific templates, and best practices for documentation.
What is a Mental Health Treatment Plan?
A mental health treatment plan is a written roadmap that outlines a client’s goals, tracks progress, and guides the clinician’s interventions.
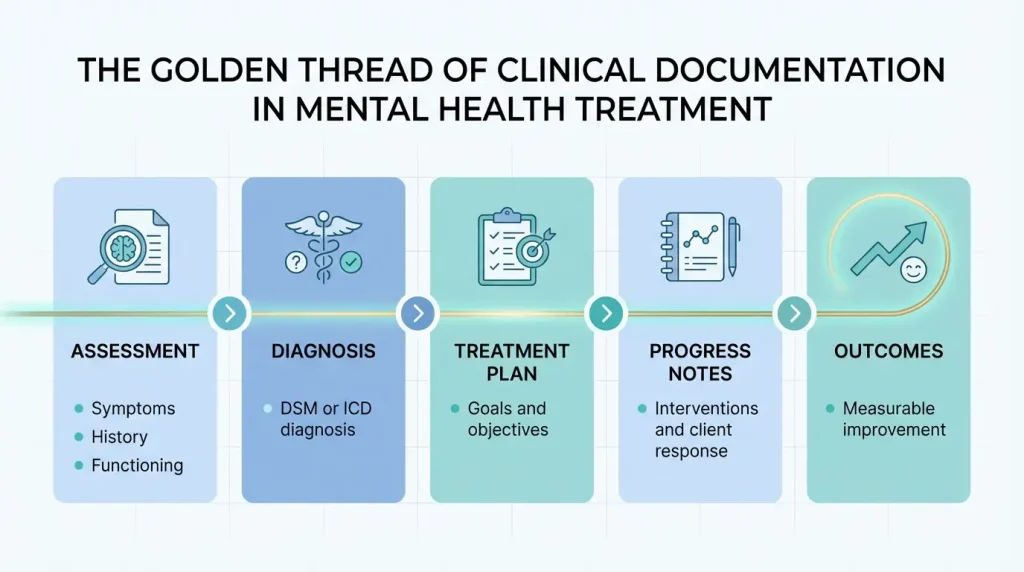
What a Mental Health Treatment Plan Includes
Presenting Problems
Identify what the client is struggling with and how symptoms affect daily functioning.
Goals
Define the broad outcomes the client wants to achieve through treatment.
Objectives
Break each goal into specific, measurable steps the client can work toward.
Interventions
Document the clinical methods the clinician will use to support progress.
Progress
Track results over time and update the plan as treatment needs change.
In simple terms, a mental health treatment plan is a written roadmap that shows what the client is working on, how progress will be measured, and how the clinician will help.
A behavioral health treatment plan is a structured, individualized document that outlines a client's clinical needs, therapeutic goals, and the specific interventions a clinician will use to help them make progress. It serves as both a clinical roadmap and a formal record of the care being provided.
Treatment plans are used across all behavioral health disciplines — from outpatient therapy and psychiatric care to community mental health centers and substance use treatment programs. While the format and level of detail may vary by setting and payer, every effective treatment plan answers four core questions:
- What is the client struggling with? (presenting problems and diagnosis)
- What does the client want to achieve? (goals)
- What specific steps will get them there? (objectives)
- How will the clinician help? (interventions and modalities)
Mental health treatment plans are sometimes called therapy treatment plans, psychotherapy treatment plans, or simply tx plans. Regardless of the terminology, the purpose is the same: to organize and document individualized care in a way that supports both the client's progress and the clinician's practice.
What is the Purpose of a Mental Health Treatment Plan?
Treatment plans serve multiple purposes — for the client, the clinician, the care team, and the payer.
For Clients
A treatment plan makes the path forward visible. It breaks an often overwhelming experience — seeking help for mental health challenges — into specific, manageable goals. Research shows that structured goal-setting improves engagement and outcomes, helping clients stay motivated and follow through.
For Clinicians
Treatment plans provide a structured documentation framework that organizes clinical thinking, supports continuity of care, and creates a defensible record of medical necessity. They make it easier to write meaningful progress notes and track client development over time.
For Billing & Compliance
Treatment plans are often required for insurance reimbursement. They demonstrate that services are clinically indicated, tied to a diagnosis, and structured around measurable goals — key elements payers look for when reviewing claims.
Key Components of a Mental Health Treatment Plan
Understanding what goes into a treatment plan is essential before you start writing one. While plans vary by discipline, setting, and payer, most behavioral health treatment plans share the same core components. Knowing these treatment plan components helps clinicians avoid gaps in documentation and ensures that every plan supports both clinical care and reimbursement.
Client Information
Basic demographic and administrative details: name, date of birth, insurance information, emergency contacts, and the name of the treating clinician.
Presenting Problem(s)
A clear, behavioral description of the issues that brought the client to treatment. These should be written in objective, non-judgmental language that reflects the client's current functioning.
Diagnosis
The client's current DSM or ICD diagnosis, including any co-occurring or comorbid conditions. This is the clinical anchor for everything else in the plan.
Strengths and Support Systems
An often-overlooked but important component. Documenting the client's personal strengths, coping skills, and social supports helps ground goals in realistic expectations and informs intervention planning.
Treatment Goals
Broad outcomes that the client hopes to achieve through the therapeutic process. Goals are written in plain language and reflect the client's own priorities and aspirations.
Objectives
Specific, measurable steps that move the client toward each goal. Good objectives are time-bound and observable — they describe what the client will do, how often, and how progress will be measured.
Interventions
The clinical techniques and therapeutic modalities the clinician will use to help the client achieve their objectives. These should be evidence-based and matched to the presenting diagnosis.
Target Dates and Progress Indicators
Each goal and objective should have a target timeframe and a way to measure progress. This is essential for ongoing treatment review and insurance documentation.
Clinician and Client Signatures
Both parties sign the treatment plan, confirming that the client has participated in the planning process and agrees with the goals as written. This is a standard requirement for most payers and accreditation bodies.
Get the Ultimate Guide to Creating Mental Health Treatment Plans
Want a practical resource you can reference while writing treatment plans? Download this free guide for a clearer, faster way to build individualized, client-centered plans that support outcomes, documentation quality, and compliance.
Inside, you’ll get guidance on core treatment plan components, SMART goals and objectives, evidence-based interventions, sample treatment plans, common documentation pitfalls, and how to connect treatment plans to progress notes and audits.
Why download it: This guide is built for behavioral health clinicians who want treatment plans that are individualized, measurable, easier to update, and better aligned with reimbursement and audit requirements.
Download the Free Guide
Get practical examples, treatment planning tips, and documentation guidance you can use right away.
Quick access. No fluff. Just practical treatment planning guidance.
Mental Health Treatment Plan Goals and Objectives
Goals and objectives are the heart of any treatment plan. Understanding the difference between the two — and how to write them effectively — is one of the most important skills in treatment planning.
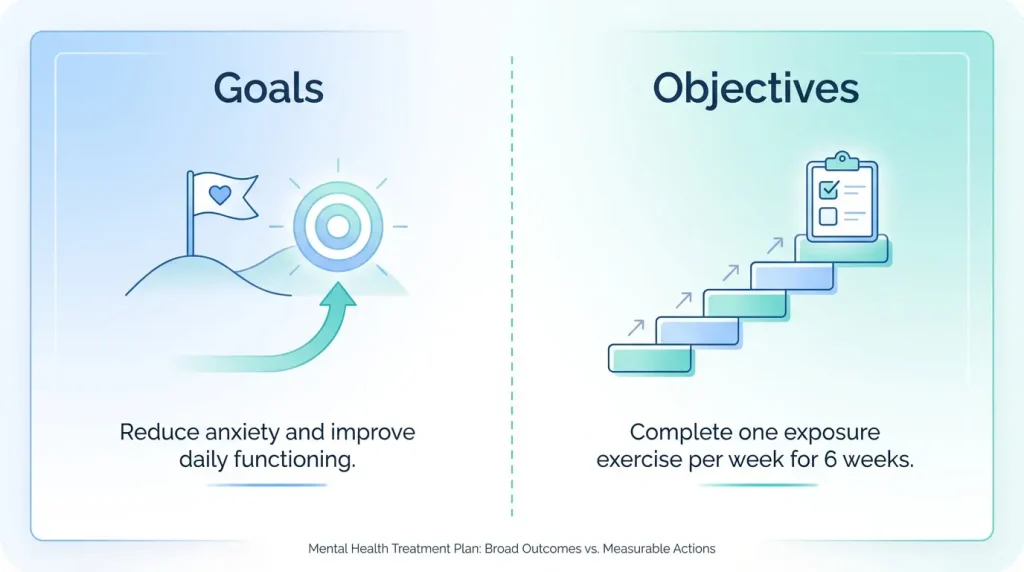
Goals are broad, overarching outcomes that reflect what the client wants to achieve by the end of the therapeutic process. They describe the destination.
Objectives are the specific, measurable steps that move the client toward each goal. They describe the path. Think of each objective as a rung on a ladder — a concrete task or milestone the client can accomplish on the way to their larger goal.
Examples of Treatment Plan Goals
- Reduce the frequency and severity of anxiety symptoms
- Develop healthy coping strategies for managing stress
- Improve interpersonal communication skills
- Achieve and maintain sobriety from substances
- Process and integrate traumatic experiences
- Manage symptoms of depression and improve daily functioning
- Reduce self-harming behaviors
- Improve self-esteem and self-worth
- Establish a stable daily routine and self-care habits
- Build a supportive social network
Examples of Treatment Plan Objectives
- Attend individual therapy sessions weekly for 90 days
- Complete a daily mood log and bring it to each session
- Practice one grounding technique per day during periods of high anxiety
- Attend a substance use support group at least twice per week
- Identify and document three coping strategies within 30 days
- Use the PHQ-9 or GAD-7 at each session to track symptom severity
- Initiate one social interaction per week to reduce isolation
- Read one psychoeducation resource on communication skills within two weeks
The Relationship Between Goals and Objectives: An Example
If a client's goal is to "manage anxiety symptoms and reduce their impact on daily functioning," the objectives might include:
- Identify anxiety triggers using a weekly thought journal (ongoing)
- Practice a relaxation technique (diaphragmatic breathing or progressive muscle relaxation) daily for 30 days
- Reduce PHQ score by 30% within 60 days
- Complete three exposures to an avoided social situation within 45 days
Each objective gives both the client and the clinician a clear, trackable way to measure progress toward the broader goal.
Condition-Specific Treatment Plan Goals and Objectives
Because every client presents with unique circumstances, treatment plan goals should be tailored to their diagnosis and individual situation. Below are example goals and objectives for four of the most common presenting concerns in behavioral health.
Treatment Plan Goals and Objectives for Anxiety
Sample Goals
- Reduce the frequency and intensity of anxiety attacks
- Develop reliable coping strategies for managing anxiety in daily life
- Resume avoided activities and social situations
Sample Objectives
- Complete a CBT thought record daily, tracking anxiety-provoking thoughts and cognitive distortions
- Practice diaphragmatic breathing for 10 minutes each morning for 30 days
- Reduce GAD-7 score by at least 5 points within 60 days
- Identify three specific situations currently avoided due to anxiety and create an exposure hierarchy within the next two weeks
- Complete one step on the exposure hierarchy per week for 8 weeks
Treatment Plan Goals and Objectives for Depression
Sample Goals
- Reduce depressive symptoms and improve overall mood
- Re-engage with activities that previously brought meaning and pleasure
- Improve daily functioning, including sleep, routine, and self-care
Sample Objectives
- Complete the PHQ-9 at the beginning of each session to track symptom severity
- Engage in one pleasurable activity per day as assigned through behavioral activation exercises
- Establish a consistent sleep schedule (target 7–8 hours per night) within 30 days
- Reduce PHQ-9 score by 5 or more points within 90 days
- Identify and challenge three automatic negative thoughts per week using a CBT thought record
Treatment Plan Goals and Objectives for Trauma (PTSD)
Sample Goals
- Process traumatic memories and reduce their interference with daily functioning
- Decrease trauma-related hypervigilance and avoidance behaviors
- Develop a stable sense of safety and self-regulation
Sample Objectives
- Engage in trauma-focused CBT or EMDR therapy weekly for 12 weeks
- Practice one grounding technique (e.g., 5-4-3-2-1) daily and as needed during periods of distress
- Identify three personal safety cues or grounding anchors within the next two sessions
- Track avoidance behaviors weekly using a self-monitoring log
- Report a 30% reduction in PCL-5 score within 90 days of beginning trauma-focused work
Treatment Plan Goals and Objectives for Substance Use
Sample Goals
- Achieve and maintain sobriety or a clinician-defined reduction in substance use
- Identify and address triggers contributing to substance use
- Build a recovery support network
Sample Objectives
- Attend a peer support or 12-step meeting at least twice per week
- Complete a functional analysis of substance use triggers within the first three sessions
- Develop a written relapse prevention plan within 30 days
- Maintain self-reported sobriety for 30 consecutive days within the first 60 days of treatment
- Identify two sober supports to contact during high-risk situations within the next two weeks
How to Write a Treatment Plan for Behavioral Health
Effective treatment planning begins before you ever open a template. Here's a step-by-step overview of the process.
How to Write a Mental Health Treatment Plan
Follow this structured process to build treatment plans that are clinically meaningful, measurable, and aligned with documentation requirements.
Assess
Begin with screening and a biopsychosocial assessment to understand symptoms, functioning, and contributing factors.
Diagnose
Identify the current DSM or ICD diagnosis and any co-occurring conditions that support medical necessity.
Prioritize Problems
Define the key clinical problems in behavioral, objective terms and rank them by urgency and impact.
Set Goals
Collaborate with the client to define broad treatment goals that reflect their needs, priorities, and readiness for change.
Write Objectives
Break each goal into specific, measurable, attainable, relevant, and time-bound objectives.
Choose Interventions
Document the therapeutic approaches, modalities, and techniques that will support each objective.
Review & Sign
Finalize the plan with review dates, signatures, and a process for updating goals as treatment progresses.
In simple terms: assess the client, identify the diagnosis, define the problems, set goals, write measurable objectives, choose interventions, and review the plan regularly.
Step 1: Conduct a Screening and Biopsychosocial Assessment
The first step is gathering a thorough clinical picture through an initial screening and a comprehensive biopsychosocial assessment. During the screening, the client shares a general overview of what brought them to treatment. The assessment goes deeper — exploring the nature, severity, and duration of symptoms, as well as the medical, psychological, social, and environmental factors contributing to the client's presentation.
This assessment forms the foundation for everything else in the treatment plan. Every goal and intervention should be traceable back to what you learn here.
Step 2: Establish a Diagnosis
Based on your assessment findings, identify the client's current diagnosis (DSM or ICD, per your setting's requirements) and any co-occurring conditions. This diagnosis is what you'll use to justify medical necessity and connect goals to clinical need.
Step 3: Identify Problems and Prioritize
With the assessment complete, identify the specific problems to address in treatment. These should be written in behavioral, objective language — not clinical jargon. Prioritize them so the most pressing concerns are addressed first.
Step 4: Collaborate with the Client on Goals
This step is critical, and it's where many treatment plans fall short. Goals should not be written by the clinician alone and handed to the client to sign. Invite the client into the conversation — ask about what they most want to change, what a better version of their daily life looks like, and what they're ready to work toward.
Client-generated goals increase engagement, improve motivation, and strengthen the therapeutic alliance. A client who helped write their own goals is far more likely to pursue them.
Step 5: Write SMART Objectives
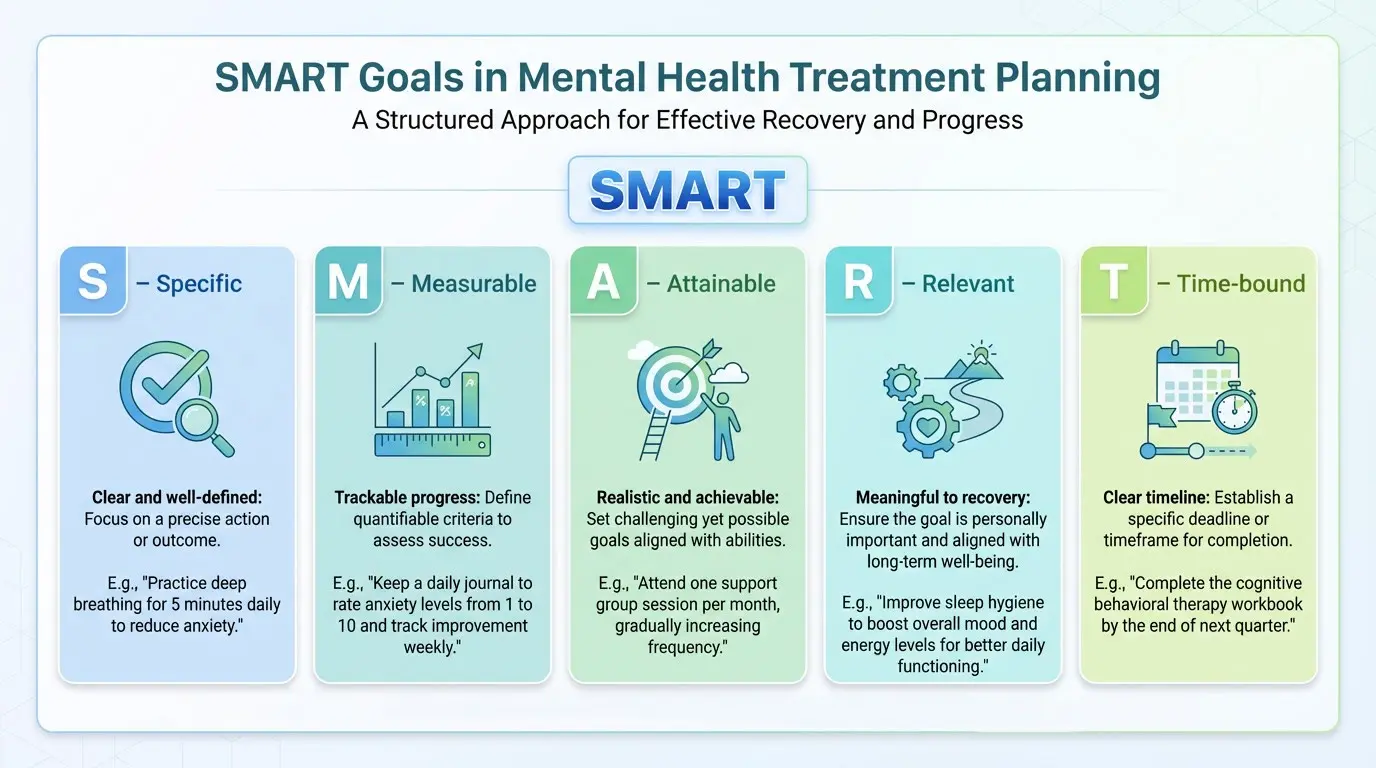
For each goal, develop one or more objectives using the SMART framework:
- Specific — Clear and explicit, with strong action verbs
- Measurable — Tied to specific amounts, timeframes, or assessment scores so progress can be tracked
- Attainable — Realistic given the client's current level of functioning and readiness for change
- Relevant — Directly connected to the stated goal and the client's diagnosis
- Time-bound — Includes a target date or timeframe for completion
Step 6: Identify Interventions
For each objective, document the specific clinical techniques and modalities you'll use. These might include cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), EMDR, motivational interviewing, psychoeducation, family therapy, medication management, or others appropriate to the presenting diagnosis.
Step 7: Get Signatures and Set a Review Date
Both the clinician and the client sign the completed treatment plan. Schedule a date to review and update it — typically every 30, 60, or 90 days, or as required by your payer or accreditation body.
Treatment Plan Templates by Discipline
While the core structure of a behavioral health treatment plan is consistent across settings, clinicians in different disciplines often need to tailor the format to their specific context.
Counseling Treatment Plan
Counseling treatment plans emphasize therapeutic goals related to behavioral change, emotional regulation, relationship skills, and coping strategies. They are collaborative and client-centered, typically including the presenting problem, diagnosis, goals, measurable objectives, therapeutic modalities, and session frequency.
Psychiatric Treatment Plan
Psychiatric treatment plans place greater emphasis on diagnostic detail, medication management, and symptom monitoring. They often include medications, target symptoms, review timelines, and coordination with providers, along with crisis planning for complex or co-occurring conditions.
Social Work Treatment Plan
Social work treatment plans address a broader range of life domains, including housing, employment, legal status, family systems, and community supports. They often incorporate the six problem domains and include goals for both service needs and mental health outcomes.
General Treatment Plan Template for Behavioral Health
Regardless of discipline, a well-structured treatment plan template should contain:
| Section | What to Include |
|---|---|
| Client Information | Name, DOB, insurance, emergency contacts |
| Diagnosis | Current DSM/ICD diagnosis, co-occurring conditions |
| Presenting Problems | Behavioral descriptions of the client's challenges |
| Strengths | Personal assets, support systems, coping resources |
| Goals | Broad therapeutic outcomes (minimum 3–4) |
| Objectives | Specific, measurable steps toward each goal |
| Interventions | Clinical techniques and modalities |
| Target Dates | Timeframe for each objective |
| Review Date | Scheduled date for plan review and update |
| Signatures | Clinician and client signatures with date |
Key Considerations for Creating Personalized Mental Health Treatment Plans
Every patient brings a unique set of experiences, symptoms, and strengths to the therapeutic relationship, regardless of their diagnosis. A well-structured treatment plan helps clinicians stay organized, focused, and aligned with each patient’s specific goals and care needs.
To develop effective, individualized goals and objectives, consider these key factors that influence treatment planning:
-
Current Mental Health Status:
Assess the nature, duration, and severity of the patient’s symptoms or presenting concerns. Their current mental and emotional state should directly inform the pace and intensity of treatment. -
Strengths and Support Systems:
Identify personal strengths such as resilience, insight, or coping strategies as well as external resources like family support, community engagement, or stable housing. These assets can serve as building blocks toward recovery. -
Readiness for Change:
A patient’s motivation level can influence the success of any intervention. Tools like the Transtheoretical Model of Change can help determine where a client falls along the continuum, from precontemplation to maintenance, and guide realistic goal-setting. -
Cultural and Social Context:
Treatment plans should reflect the patient’s cultural identity, values, language preferences, and community experiences. This ensures goals are both respectful and relevant, increasing engagement and therapeutic alliance. -
Holistic Care Needs:
Mental health doesn’t exist in a vacuum. Consider incorporating goals related to physical health, social relationships, emotional regulation, and even spiritual well-being to support the patient’s overall functioning.
By thoughtfully addressing these factors, you can avoid generic plans and instead create treatment strategies that are meaningful, measurable, and truly patient-centered.
Mental Health Treatment Plan Tips
There are no rigid rules for developing a treatment plan — every plan is unique to the patient in front of you. Typically, you'll start with a mental health treatment plan template and modify it as needed. Here are six best practices to guide you through the process.
1. Monitor Progress Consistently
To evaluate whether a treatment plan is working, you need a systematic way to track how the patient is doing between sessions and over time. Ask patients to record their thoughts, feelings, and behaviors in a journal or mood log. Self-reports give you a clearer picture of their state of mind between sessions. You should also note clinical observations during sessions — shifts in body language, improved affect, increased engagement — as signs of progress or decline. Validated rating scales like the PHQ-9, GAD-7, or PCL-5 are especially useful for creating objective benchmarks to reference at treatment plan reviews.
2. Write SMART Goals
Your patients may become overwhelmed if you set goals that are too challenging or vague. For treatment to be both effective and motivating, use the SMART framework to create clear, realistic goals that guide patients toward their intended outcomes:
- Specific — Goals should be clear and explicit, written with strong action verbs so the patient knows exactly what to do
- Measurable — Tied to specific dates, amounts, or assessment scores so progress can be tracked
- Attainable — Realistic given the patient's current functioning and circumstances
- Relevant — Directly connected to the patient's individual needs and diagnosis
- Time-bound — Includes a specific end date or timeframe so patients stay motivated and goals can be measured
3. Set Goals That Motivate
Patients are far more likely to follow through on goals that matter to them personally. Help your patients identify goals they have a genuine stake in — goals that connect to their values, relationships, or daily life. Make sure goals are prioritized in order of importance so patients can focus on what matters most. If a goal doesn't add value or meaning to their life, they won't be motivated to work toward it, no matter how clinically appropriate it may seem.
4. Use Language Carefully
Adequately describing your patients' conditions and progress is essential to creating an effective treatment plan. Therapists often use a range of clinical terms to describe their patients, but word choice matters more than clinicians sometimes realize. For example, "obsessive" and "all-consuming" can be used synonymously in some contexts, but they carry very different emotional connotations. Describing someone or their behavior as "obsessive" sounds more negative and pathologizing than "all-consuming" — even when the clinical meaning is similar. When writing treatment plans and progress notes, aim for language that is objective and non-judgmental, and consider where a synonym might better serve the patient's dignity and self-perception.
5. Collaborate With Patients
A client-centered approach — one that actively involves patients in the treatment planning process — is important for making them feel like participants in their own care rather than subjects of it. Let your patient know you're on the same team and that the treatment plan is a shared roadmap, not something done to them. Start by gathering information about their hopes, concerns, and expectations. Ask what they most want to change and what a better version of their daily life looks like.
When you invite patients to co-create their treatment plan, you signal that you value their perspective. This builds trust, increases engagement, and often leads to more meaningful goals. Give patients time to open up and contribute as the process unfolds, and always consider their comfort level when discussing interventions and assignments.
6. Leverage Templates
Proper documentation, organization, and maintenance of behavioral health records are essential for accuracy, compliance, and reimbursement. But writing treatment plans from scratch for every patient is time-consuming — and with a full caseload, capturing the same necessary details repeatedly can feel demanding and repetitive.
Intuitive, prebuilt templates allow you to document efficiently without sacrificing quality. Templates designed for behavioral health documentation enable you to customize a treatment plan to each patient's individual needs while ensuring that nothing required is missed. In addition to treatment plans, good templates can support initial assessments, progress notes, and discharge summaries — giving you a complete, consistent clinical record.
Mental Health Treatment Plan Checklist
Your treatment plans should be thorough while including only clinically relevant details. Use this checklist before finalizing any plan to make sure nothing critical has been missed.
Presenting Problems
- Do the problems reflect the key clinical domains (medical status, employment, substance abuse, legal status, family/social status, psychiatric status where applicable)?
- Are problems written in behavioral, observable, and non-judgmental terms?
- Are they prioritized by clinical urgency?
Goals
- Does each goal address at least one identified problem?
- Are goals attainable within the expected course of treatment?
- Does the patient understand the goals as written?
- Has the patient participated in selecting their goals and does the plan reflect their readiness to change?
Objectives
- Is each objective specific and measurable?
- Does each objective have a target date?
- Are objectives realistic for the patient's current level of functioning?
- Does the patient understand what is expected of them for each objective?
Interventions
- Is each intervention linked to a specific goal?
- Are interventions evidence-based and appropriate for the diagnosis?
- Is session frequency documented?
- Is the patient willing and able to engage in the planned interventions?
General
- Is the plan individualized to this specific patient — reflecting their strengths, culture, values, and circumstances?
- Has the patient participated in developing the plan?
- Have both the clinician and the patient signed and dated the plan?
- Is a treatment review date documented?
Insurance Documentation and Medical Necessity
If you bill insurance for behavioral health services, your treatment plan is more than a clinical document — it's a core piece of your reimbursement record. Payers use treatment plans to evaluate medical necessity and determine whether the services being provided are clinically justified. A plan with missing or inaccurate information can result in undercoding, claim denials, or audit findings.
While specific requirements vary by payer, most insurance companies want to see documentation of:
- A current diagnosis and any co-occurring conditions
- Medications and dosages (where applicable)
- Severity and duration of symptoms
- How symptoms are affecting the patient's daily functioning
- Specific, measurable objectives tied to symptom reduction
- Session frequency and anticipated duration of treatment
- Therapeutic interventions and modalities
- A timeline for progress measurement and plan review
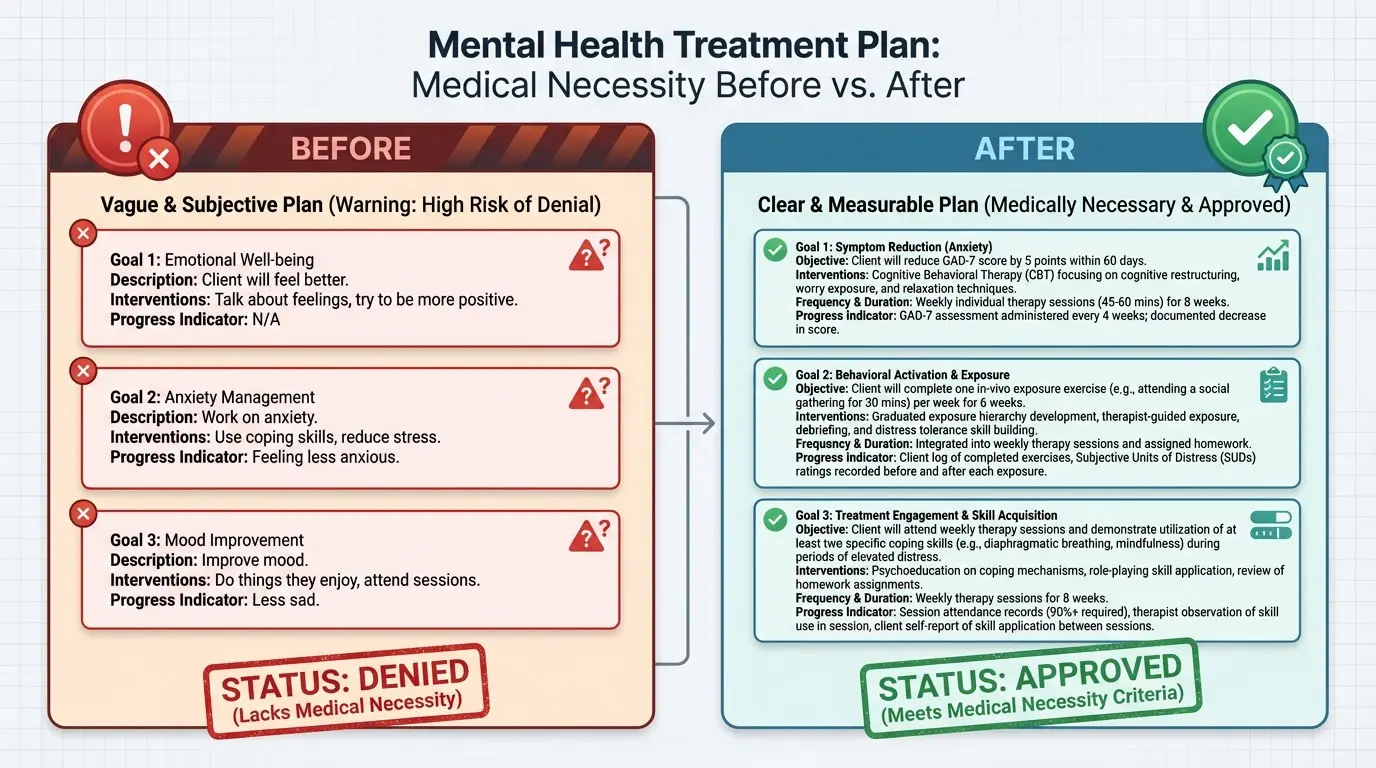
One important tip: when framing goals for insurance documentation, write them in clinical terms that reflect medical necessity — not just personal improvement. Rather than stating that a client's goal is "to improve their agoraphobia," write that the goal is "to decrease physiological anxiety symptoms — including dizziness, elevated heart rate, and chest tightness — in unfamiliar environments." The first sounds like a preference; the second sounds like treatment.
Insurance companies look for evidence that treatment is a medical necessity. When you document each goal in terms of the specific symptoms being addressed and how interventions will reduce them, you significantly strengthen your claims — and your ability to defend them if audited.
How a Mental Health Treatment Plan Complements Other Clinical Notes
A mental health treatment plan not only supports patient progress but also strengthens collaboration across the behavioral health care team. It promotes consistent communication among clinicians, ensures alignment of care goals, and provides essential documentation for reimbursement and regulatory compliance. As a core component of the patient's record, the treatment plan plays a vital role in meeting federal and state documentation standards. Here's how it connects to the other key documents in the clinical record.
Psychiatric Evaluation or Biopsychosocial Assessment
The initial psychiatric evaluation — or a comprehensive biopsychosocial assessment — serves as the foundation for understanding a patient's mental health status. It involves gathering detailed information about the patient's presenting concerns, history, behavior, thought processes, and functioning. This process typically leads to a formal diagnosis, which informs the direction of care.
The treatment plan builds directly on the findings from the evaluation. It translates diagnostic insights into a structured, goal-oriented roadmap for care. Every treatment goal and objective should clearly correspond to a specific concern identified during the assessment, ensuring that interventions are both relevant and measurable. A standardized treatment plan template further supports this process by promoting consistency, clarity, and compliance in documentation.
Progress Notes
Progress notes and treatment plans work in tandem to document and guide the course of care. While the treatment plan outlines the patient's goals and objectives, progress notes capture session-by-session movement toward those targets — providing a clinical narrative of what is working, what has changed, and what needs adjustment.
Because progress notes often reference one or more specific treatment objectives, a well-structured treatment plan ensures that each note is purposeful and aligned with the broader care goals. This alignment also helps meet insurance documentation standards and supports timely, accurate reimbursement.
A typical progress note includes:
- The treatment goals or objectives addressed in the session
- The patient's response to interventions
- Any changes in the patient's condition or presentation
- Clinical observations and insights
- The outcome of the session and next steps
A clearly defined treatment plan streamlines this process, making it easier to write defensible notes that reflect the patient's progress and the clinician's reasoning.
Discharge Summary
A discharge summary is completed when a patient concludes treatment. It provides a comprehensive overview of the care delivered, the patient's progress, and recommendations for ongoing support or follow-up services. A well-structured treatment plan serves as the primary reference point during this process — helping clinicians accurately summarize the course of treatment, document the rationale for discharge, and demonstrate clinical improvement.
By reviewing the goals and objectives in the treatment plan, clinicians can efficiently document the interventions provided, assess how the patient responded to care, and identify what changed over time. Since many patients engage in treatment over extended periods, the treatment plan also serves as a visual timeline — making it easier to track symptom reduction, behavior change, and functional gains.
A discharge summary typically includes:
- A summary of the patient's presenting problem(s) and diagnosis
- Treatments and interventions provided
- The patient's progress toward each treatment goal
- Clinical observations at the time of discharge
- The reason for discharge (goals met, patient decision, referral, etc.)
- Recommendations for aftercare or continued services
Example discharge summary statements:
- The patient reports no longer experiencing suicidal ideation.
- The patient demonstrates improved coping strategies for managing depressive symptoms.
- Mood is stable, with no current signs of depression, anxiety, or psychosis.
- The patient expresses confidence in communicating effectively with others.
- Behavior is appropriate, with no signs of delusions or hallucinations.
Using the treatment plan as the foundation for discharge documentation helps ensure accuracy, compliance, and a smooth transition to the next phase of care.
How ICANotes Streamlines Behavioral Health Treatment Planning
Clinicians evaluating behavioral health EHRs often have specific questions about treatment planning: Does the software actually connect diagnosis to goals and progress notes? Does it generate generic templates, or does it support clinically meaningful documentation? How much time does it realistically save?
ICANotes was purpose-built by behavioral health clinicians — not adapted from a general medical EHR — which means treatment planning is built into the core clinical workflow rather than added on as a secondary feature. Here's what that means in practice:
- Diagnosis-linked goals and objective libraries. When you enter a diagnosis, ICANotes surfaces clinically relevant goals and objectives for that condition. Rather than writing from scratch, you select and customize from a vetted library — then link them directly to billing codes and session documentation.
- Integrated documentation workflow. Treatment plans in ICANotes connect directly to progress notes. When you document a session, you reference the specific treatment plan objectives addressed — creating the structured alignment that payers look for and auditors require.
- Profession-specific templates. Whether you're practicing as a therapist, psychiatrist, or social worker in an agency setting, ICANotes includes configurable templates tailored to your discipline and documentation requirements.
- Compliance-ready documentation. Guided prompts help you cover diagnostic requirements, demonstrate medical necessity, and monitor progress — so you're less likely to overlook something that could trigger a claim denial.
Our customers consistently highlight how ICANotes helps them document more efficiently, improve reimbursement accuracy, and navigate audits with confidence. They also appreciate our responsive technical support and an interface designed specifically for mental health workflows — not retrofitted from a system built for primary care.
Whether you're treating a new client or updating a long-term care plan, ICANotes gives you the structure and flexibility to document clearly and efficiently — so you spend less time writing and more time delivering care.
Create Better Treatment Plans in Less Time
Writing a strong mental health treatment plan takes time—and every goal, objective, and intervention needs to support both quality care and clean documentation. ICANotes helps behavioral health clinicians build structured, individualized treatment plans faster without starting from scratch.
With diagnosis-linked content, guided workflows, and documentation tools built specifically for behavioral health, ICANotes makes it easier to create plans that support medical necessity, track progress, and connect directly to your progress notes.
Why clinicians use ICANotes: Build clear, measurable treatment plans more efficiently, reduce repetitive data entry, and keep documentation aligned with payer and audit requirements.
Start Your Free Trial
See how ICANotes helps you create structured treatment plans faster while supporting clinical quality, compliance, and continuity of care.
No credit card required.
Explore Treatment Plans by Diagnosis and Use Case
Looking for more specific examples? Browse these guides to see how treatment plans are structured across different conditions and clinical scenarios.
Anxiety Treatment Plan
Goals, objectives, and interventions for anxiety disorders.
Treatment Planning in Counseling
How software improves treatment planning workflows.
Grief Treatment Plans
Structured approaches for grief and loss therapy.
Self-Harm Treatment Plan
Interventions and goals for reducing self-harm behaviors.
Depression Treatment Goals
SMART goals and measurable objectives for depression.
Couples Therapy Goals
Examples of goals for relationship and couples work.
Eating Disorder Treatment Plan
Planning and documentation tips for eating disorders.
Substance Abuse Treatment Plan
Goals, objectives, and interventions for substance use.
Frequently Asked Questions About Mental Health Treatment Plans
Recent Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.