Blog > Treatment Strategies > Creating a Depression Treatment Plan: Examples & Best Practices
Creating a Depression Treatment Plan: A Practical, Clinically Sound Guide for Mental Health Clinicians
A well-constructed depression treatment plan provides more than clinical direction — it creates clarity, continuity, and accountability for both clinicians and clients. In outpatient mental health settings, treatment planning plays a critical role in guiding care, supporting medical necessity, and documenting progress over time. This guide walks through how to create an effective treatment plan for depression, including key components, clinical examples, and documentation best practices. Whether you’re developing an initial plan or refining an existing one, this framework is designed to support ethical, evidence-based, and audit-ready care.

Last Updated: April 8, 2026


What You'll Learn
-
What a comprehensive depression treatment plan should include and how it differs from progress notes
-
How to translate assessment findings into clear, individualized problem statements for depression care
-
How treatment goals, interventions, and measurement tools work together within treatment planning for depression
-
Examples of evidence-based interventions commonly used in depression treatment plans, and how to document them effectively
-
Why ongoing risk assessment and safety planning are essential components of depression treatment planning
-
How to structure measurable, time-bound elements within a depression treatment plan to support progress monitoring
-
Common documentation pitfalls in depression treatment plans and how to avoid issues that can weaken clinical or payer review
-
How behavioral-health-specific EHRs like ICANotes support efficient, compliant depression treatment planning workflows
Contents
What is a Depression Treatment Plan?
Why Treatment Planning Matters in Depression Care
Core Components of a Depression Treatment Plan
The Importance of Risk Assessment in Depression Treatment Planning
Measuring Progress and Adjusting the Plan
Common Documentation Pitfalls in Depression Treatment Planning
A depression treatment plan is a structured clinical document that outlines a client’s diagnosis, treatment goals, selected interventions, and measurable outcomes. It serves as a roadmap for therapy, helping clinicians align evidence-based interventions with clearly defined goals while supporting medical necessity, continuity of care, and treatment effectiveness.
What is a Depression Treatment Plan?
A treatment plan for depression is a structured clinical document that outlines how depressive symptoms will be assessed, addressed, monitored, and reviewed over time. It typically includes:
-
Diagnostic and assessment findings
-
Problem statements describing functional impairment
-
Treatment goals and supporting objectives
-
Risk assessment considerations
-
Methods for measuring progress
-
Timeframes for review and revision
Unlike progress notes, which document what occurred during a single session, depression treatment plans describe the broader clinical roadmap guiding care.
What a Depression Treatment Plan Should Include
A strong depression treatment plan connects assessment findings to clear goals, measurable objectives, selected interventions, and ongoing progress tracking.
Why Treatment Planning Matters in Depression Care
Effective treatment planning for depression supports both clinical outcomes and professional accountability. A strong plan helps:
-
Maintain clinical focus across sessions
-
Align interventions with symptom severity
-
Support client engagement and transparency
-
Demonstrate medical necessity for reimbursement
-
Provide continuity across providers or levels of care
-
Reduce clinical drift or unfocused treatment
For clients with depression — where motivation, concentration, and hope may be impaired — a clear plan can also serve as a stabilizing reference point throughout treatment.
Core Components of a Depression Treatment Plan
While treatment plans may look different across settings, effective depression treatment planning consistently includes a set of foundational components. These elements help clinicians translate assessment findings into targeted interventions and measurable outcomes over time.
1. Comprehensive Assessment and Diagnosis
Treatment planning begins with a thorough assessment that captures both symptom presentation and functional impact. This may include:
-
Clinical interview
-
DSM-5-TR diagnostic criteria
-
Standardized screening tools (e.g., PHQ-9)
-
Psychosocial history
-
Medical and medication review
-
Trauma history and protective factors
Example (Assessment Summary):
Client reports persistent low mood, anhedonia, fatigue, impaired concentration, and sleep disturbance for approximately four months, resulting in decreased work performance and social withdrawal.
A clear diagnostic foundation ensures interventions are appropriately matched to severity and duration.
2. Problem Statements and Clinical Formulation
Problem statements translate assessment findings into concise descriptions of how depression affects the client’s life. Strong problem statements are:
-
Behaviorally specific
-
Linked to functional impairment
-
Free of judgment or vague language
Example Problem Statements::
Client experiences persistent depressed mood and low energy resulting in difficulty maintaining employment responsibilities.
Client reports social withdrawal and loss of interest in previously enjoyable activities, contributing to increased isolation.
These statements guide goal development and intervention selection.
3. Treatment Goals and Objectives (Contextual Overview)
Treatment goals describe the desired outcomes of care, such as symptom reduction, improved functioning, or relapse prevention. Objectives support those goals through measurable benchmarks.
This article focuses on how goals fit into the overall treatment plan, rather than how to write them in detail. Read our related step-by-step guide for more guidance on how to write treatment goals for depression.
How Goals, Objectives, and Interventions Connect
4. Interventions and Therapeutic Approaches
Interventions outline how treatment goals will be addressed. These should be evidence-based and clearly linked to identified problems.
Common interventions for depression include:
-
Cognitive Behavioral Therapy (CBT): Addressing negative thought patterns and behavioral avoidance
-
Behavioral Activation: Increasing engagement in meaningful activities
-
Interpersonal Therapy (IPT): Improving relationship functioning and role transitions
-
Psychoeducation: Increasing insight into depressive symptoms and treatment rationale
-
Medication management: When appropriate and coordinated with prescribers
Example Intervention Language:
Clinician will utilize CBT techniques to identify cognitive distortions contributing to feelings of worthlessness and replace them with balanced thought patterns.
Related: Interventions for Depression: Evidence-Based Techniques for Clinicians
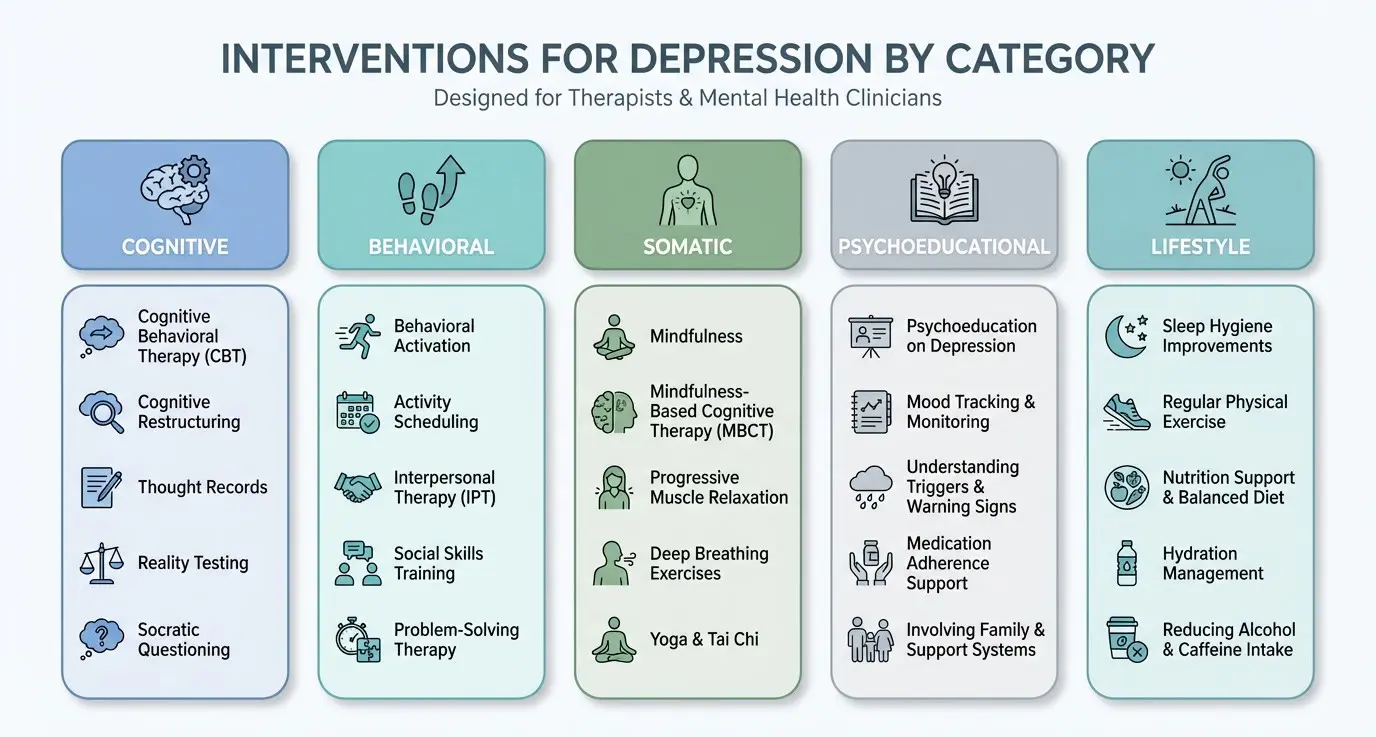
Download the Depression Intervention Cheat Sheet
Need a faster way to match symptoms to treatment? This practical cheat sheet gives clinicians a structured, quick-reference guide to evidence-based interventions for depression.

Examples of Intervention Language
Cognitive & Behavioral Interventions
-
Clinician will utilize cognitive restructuring techniques to help client identify and challenge automatic negative thoughts contributing to hopelessness and self-criticism.
-
Clinician will implement behavioral activation strategies to increase engagement in pleasurable and mastery-based activities at least three times per week.
-
Clinician will support client in developing a structured daily routine to address inactivity, fatigue, and disrupted sleep patterns.
Emotional Regulation & Coping Skills
-
Clinician will teach grounding and emotion regulation techniques to support client in managing periods of acute emotional distress.
-
Clinician will introduce mindfulness-based strategies to increase present-moment awareness and reduce rumination.
-
Clinician will guide client in developing a personalized coping plan for managing depressive symptoms outside of sessions.
Interpersonal & Relational Interventions
-
Clinician will explore interpersonal stressors contributing to depressive symptoms and support client in developing healthier communication patterns.
-
Clinician will assist client in identifying social supports and increasing meaningful interpersonal contact to reduce isolation.
-
Clinician will use interpersonal therapy techniques to address role transitions and unresolved grief impacting mood.
Psychoeducation & Insight
-
Clinician will provide psychoeducation regarding depressive symptoms, treatment expectations, and the role of thoughts, behaviors, and emotions in maintaining depression.
-
Clinician will review the relationship between sleep, activity level, and mood to support improved symptom management.
-
Clinician will normalize fluctuations in mood while reinforcing strategies for sustained improvement.
Risk Monitoring & Safety-Oriented Interventions
-
Clinician will assess suicide risk at each session and document changes in ideation, intent, or protective factors.
-
Clinician will collaborate with client to develop and review a safety plan, including coping strategies and crisis resources.
-
Clinician will coordinate with additional providers as needed to support client safety and continuity of care.
Access Our Sample Treatment Plan Library
Get instant access to our full library of sample treatment plans.

The Importance of Risk Assessment in Depression Treatment Planning
Risk assessment is a critical component of treatment planning for depressed clients. Depression is associated with increased risk for suicidal ideation, self-harm, and functional deterioration, making ongoing evaluation essential.
Why Risk Assessment Matters
Incorporating risk assessment into the treatment plan helps clinicians:
-
Identify safety concerns early
-
Determine appropriate level of care
-
Document clinical decision-making
-
Adjust interventions responsively
-
Protect client welfare and clinician liability
Risk assessment should be ongoing, not limited to intake.
Key Risk Factors to Assess
Risk evaluation may include assessment of:
-
Suicidal ideation (passive or active)
-
History of suicide attempts or self-harm
-
Substance use
-
Recent losses or major stressors
-
Feelings of hopelessness or burdensomeness
-
Limited social supports
Protective factors — such as supportive relationships, religious beliefs, or future orientation — should also be documented.
Safety Planning Within the Treatment Plan
When risk is identified, the treatment plan should reflect appropriate safeguards.
Example Risk-Related Plan Language:
Client denies current suicidal intent but reports passive thoughts of “not wanting to wake up.” Clinician will monitor risk each session, develop a safety plan, and provide crisis resources.
Including safety planning demonstrates proactive, ethical care and strengthens clinical documentation.
Related: Mental Health Safety Planning: Why It's No Longer Optional for Clinicians
Measuring Progress and Adjusting the Plan
Treatment plans should specify how progress will be evaluated, such as:
-
Standardized tools (e.g., PHQ-9)
-
Client self-report
-
Functional improvements (sleep, work attendance, relationships)
Example:
Progress will be monitored using PHQ-9 scores administered bi-weekly and client-reported changes in daily functioning.
Plans should be reviewed every 30–90 days and updated as symptoms evolve.
Measurement-Based Care Example
Tracking PHQ-9 scores over time helps clinicians monitor treatment response and update the plan when progress stalls.
18
14
10
6

Sample Depression Treatment Plan
Client Overview
Client is a 35-year-old adult presenting with symptoms consistent with Major Depressive Disorder, moderate severity. Symptoms include persistent low mood, fatigue, impaired concentration, sleep disturbance, and withdrawal from social and occupational activities. Symptoms have been present for approximately four months and are negatively impacting daily functioning and quality of life.
Assessment Summary
Assessment findings indicate moderate depressive symptoms as measured by a baseline PHQ-9 score of 16. Client reports decreased motivation, difficulty completing work tasks, and reduced engagement in previously enjoyable activities. Client denies active suicidal intent but endorses passive thoughts of “wanting everything to stop” during periods of heightened distress. Protective factors include a supportive partner and willingness to engage in treatment.
Problem Statements
-
Persistent depressed mood and low energy are interfering with occupational performance and daily functioning.
-
Cognitive distortions and negative self-talk are contributing to feelings of worthlessness and hopelessness.
-
Social withdrawal and reduced activity level are maintaining depressive symptoms.
-
Passive suicidal ideation is present during periods of increased emotional distress.
Treatment Goal 1: Reduce Depressive Symptom Severity
Time Frame: 12 weeks
Measurable Objectives:
-
Client will demonstrate a reduction in PHQ-9 score from 16 (moderate) to 10 or below within 12 weeks.
-
Client will report a decrease in frequency and intensity of depressive symptoms as evidenced by weekly self-report.
Interventions:
-
Clinician will utilize CBT techniques to identify and challenge cognitive distortions contributing to depressed mood.
-
Clinician will provide psychoeducation regarding the cognitive-behavioral model of depression.
-
Clinician will monitor symptom severity using the PHQ-9 at bi-weekly intervals.
Treatment Goal 2: Increase Daily Functioning and Activity Level
Time Frame: 8–10 weeks
Measurable Objectives:
-
Client will engage in at least three scheduled activities per week that promote routine, pleasure, or mastery within 6 weeks.
-
Client will report improved ability to complete basic daily tasks (e.g., work responsibilities, household tasks) on at least 4 out of 7 days per week within 8 weeks.
Interventions:
-
Clinician will implement behavioral activation strategies to support increased engagement in daily activities.
-
Clinician will assist client in developing a realistic weekly activity schedule.
-
Clinician will review barriers to activity and problem-solve challenges during sessions.
Treatment Goal 3: Improve Coping Skills and Emotional Regulation
Time Frame: 6–8 weeks
Measurable Objectives:
-
Client will identify and demonstrate use of at least three coping strategies for managing depressive symptoms within 6 weeks.
-
Client will report decreased rumination and improved emotional regulation during periods of distress.
Interventions:
-
Clinician will teach grounding, relaxation, and emotion regulation techniques.
-
Clinician will support client in developing a personalized coping toolkit for use outside of sessions.
-
Clinician will reinforce skill use through review and reflection during therapy sessions.
Treatment Goal 4: Address Risk and Enhance Safety
Time Frame: Ongoing
Measurable Objectives:
-
Client will verbalize understanding of their safety plan and identify support resources.
-
Client will report reduced frequency of passive suicidal ideation over the course of treatment.
Interventions:
-
Clinician will assess suicide risk at each session and document findings.
-
Clinician will collaboratively develop and review a safety plan with the client.
-
Clinician will provide crisis resources and reinforce use as needed.
Progress Monitoring and Review
Progress will be monitored using standardized measures (PHQ-9), client self-report, and functional indicators. Treatment plan will be formally reviewed every 60 days and updated based on clinical progress, symptom changes, or emerging needs.
Discharge Planning (Preliminary)
Discharge planning will focus on sustained symptom reduction, independent use of coping strategies, and relapse prevention. Client will demonstrate stable mood, improved functioning, and ability to manage symptoms with minimal clinical support prior to discharge.
Common Documentation Pitfalls in Depression Treatment Planning
Even experienced clinicians can unintentionally weaken their documentation when treatment plans are rushed, templated, or not revisited regularly. Below are common pitfalls seen in depression treatment planning, along with examples of what to avoid and how to strengthen documentation.
What Makes a Treatment Plan Stronger?
No measurable objective
Generic intervention language
No outcome tracking
No clear connection between symptoms and interventions
SMART objective with timeframe
Specific interventions like CBT or behavioral activation
Progress tracking with PHQ-9
Direct alignment between assessment, goals, and treatment
1. Vague or Non-Actionable Goals
Problem: Goals that lack specificity or measurable outcomes do not clearly demonstrate progress or medical necessity.
Weak Example: “Client will feel better.”
Why this is an issue: This goal does not indicate what will change, how improvement will be measured, or when progress is expected.
Stronger Alternative: “Client will report a reduction in depressive symptoms as evidenced by a decrease in PHQ-9 score from 16 to 10 or below within 12 weeks.”
2. Interventions That Don’t Align With the Assessment
Problem: Interventions are listed that do not clearly address the problems identified in the assessment.
Weak Example:
-
Problem: Social withdrawal and isolation
-
Intervention: “Provide supportive therapy.”
Why this is an issue: The intervention is vague and does not show how it targets the identified problem.
Stronger Alternative: "Clinician will utilize behavioral activation strategies to increase client’s engagement in social and routine activities at least three times per week.”
3. Missing or Inadequate Risk Documentation
Problem: Depression treatment plans fail to address suicide risk, even when indicators are present.
Weak Example: No mention of risk assessment despite client endorsing passive suicidal thoughts.
Why this is an issue: Omitting risk considerations can raise serious clinical, ethical, and liability concerns.
Stronger Alternative: “Client endorses passive suicidal ideation without intent or plan. Clinician will assess risk at each session, maintain an active safety plan, and provide crisis resources.”
4. Copy-and-Paste or Over-Generic Treatment Plans
Problem: Treatment plans rely heavily on templated language that does not reflect the client’s unique presentation.
Weak Example: Identical goals and interventions across multiple clients with different symptom profiles.
Why this is an issue: Payers and auditors often flag repetitive plans as evidence of insufficient individualization.
Stronger Alternative: Tailor goals and interventions to the client’s specific symptoms, functional impairments, and life context (e.g., work stress, caregiving responsibilities, recent loss)
5. Lack of Measurable Progress Indicators
Problem: Plans do not specify how improvement will be tracked.
Weak Example: “Monitor progress as treatment continues.”
Why this is an issue: Without defined metrics, it is difficult to justify continued care or adjust treatment appropriately.
Stronger Alternative: “Progress will be monitored using PHQ-9 scores administered bi-weekly and client self-report of daily functioning.”
Frequently Asked Questions: Depression Treatment Plans
Build Stronger, More Effective Depression Treatment Plans
Explore these additional guides to strengthen your clinical decision-making, improve documentation, and align interventions with measurable outcomes in depression care.
- Treatment Goals for Depression: SMART Goals and Objectives That Work
- Depression Assessment Tools: How to Measure Symptoms and Track Progress
- Interventions for Depression: Evidence-Based Techniques for Clinical Practice
- ACT for Depression: Practical Acceptance and Commitment Therapy Interventions
- Depression in Older Adults: Clinical Considerations and Treatment Approaches
How ICANotes Supports Depression Treatment Planning
Effective treatment planning requires more than clinical insight — it also depends on documentation tools that support clarity, consistency, and efficiency. ICANotes is designed specifically for behavioral health clinicians, making it well-suited to support depression treatment planning workflows.
Structured, Clinician-Friendly Treatment Plans
ICANotes provides structured treatment plan templates that guide clinicians through key components, including:
-
Assessment and diagnosis
-
Problem statements
-
Treatment goals and objectives
-
Interventions
-
Progress tracking
This customizable structure helps ensure that depression treatment plans are complete, organized, and aligned with best practices — without forcing clinicians into rigid or generic formats.
Seamless Connection Between Treatment Plans and Notes
One of the challenges in depression care is keeping treatment plans and session documentation aligned. ICANotes helps address this by:
-
Allowing clinicians to reference treatment plan goals directly within progress notes
-
Supporting continuity between what is planned and what is addressed in sessions
-
Making it easier to demonstrate how interventions relate back to established goals
This linkage strengthens documentation for both clinical clarity and utilization review.
Support for Measurement-Based Care
ICANotes supports the use of standardized screening tools commonly used in depression treatment, such as the PHQ-9. This makes it easier to:
-
Document baseline symptom severity
-
Track progress over time
-
Update treatment plans based on objective data
Measurement-based documentation helps clinicians justify treatment decisions and demonstrate progress (or need for continued care).
Efficient Updates and Ongoing Review
Depression treatment plans should evolve as symptoms change. ICANotes makes it easier to:
-
Review and update treatment plans at required intervals
-
Modify goals or interventions as clinical needs shift
-
Maintain clear versioning and historical documentation
This reduces administrative burden while supporting ethical, responsive care.
Designed Specifically for Behavioral Health Workflows
Unlike generic EHR systems, ICANotes is built for behavioral health settings, which means:
-
Language and workflows reflect how clinicians actually practice
-
Treatment planning supports psychotherapy, psychiatry, and integrated care models
-
Documentation emphasizes clinical reasoning, not just billing requirements
For clinicians treating depression, this translates into treatment plans that are both clinically meaningful and administratively sound.
Build Better Depression Treatment Plans—Faster
Creating a strong treatment plan takes more than listing goals—it requires aligning interventions, objectives, and outcomes in a way that supports medical necessity and clinical progress.
ICANotes helps you turn depression treatment planning into a structured, efficient workflow—so your documentation is clear, compliant, and easy to maintain.
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







