Blog > Documentation > Best Behavioral Health EHR (2026): Buyer’s Guide + 20 Questions
Best Behavioral Health EHR (2026): Buyer’s Guide + 20 Questions to Ask
The Complete Behavioral Health EHR Buyer’s Guide for Mental Health Practices
Choosing the best behavioral health EHR can directly impact your documentation efficiency, billing accuracy, and long-term practice growth. In this comprehensive buyer’s guide, we break down what to look for in behavioral health EHR software, how it differs from general EMR systems, and the key questions to ask before making a decision. Whether you’re evaluating EMR software for behavioral health, comparing platforms, or upgrading your current system, this guide will help you confidently select the right solution for your practice.

Last Updated: April 6, 2026


What You'll Learn
- How to evaluate and compare the best behavioral health EHR systems for your practice
- The key differences between behavioral health EHR vs. general EMR software
- What features matter most in behavioral health EMR software (documentation, billing, telehealth, compliance)
- 20 essential questions to ask vendors before choosing an EHR for behavioral health
- Common pitfalls to avoid when selecting EMR software for behavioral health practices
- How to choose a system that supports both clinical workflows and revenue cycle performance
Contents
- Why Behavioral Health Practices Need a Specialized EHR
- How to Choose the Best Behavioral Health EHR
- Clinical Documentation and Note Efficiency
- Compliance and Security
- Telehealth and Client Engagement
- Billing and Revenue Cycle Management
- Group Practice Functionality
- Psychological Testing and Assessments
- Pricing, Support, and Long-Term Fit
- How to Use These Questions Effectively
- Choosing the Best Behavioral Health EHR for Your Practice
- Frequently Asked Questions
What Is the Best Behavioral Health EHR?
The best behavioral health EHR is one that is purpose-built for mental health workflows, allowing clinicians to complete documentation quickly, generate claims directly from notes, support telehealth, and maintain compliance with payer and regulatory requirements. Top systems include structured templates, integrated billing, outcome tracking tools, and customizable workflows designed specifically for behavioral health practices.
Best Behavioral Health EHR Software (2026)
Choosing a behavioral health EHR is one of the highest-stakes decisions a mental health practice will make. The right system reduces administrative burden, protects revenue, and supports clinical care. The wrong one creates workarounds, billing gaps, and documentation headaches that compound over time.
Strong clinical documentation is one of the biggest differentiators between behavioral health EHR systems. If you're unsure what high-quality documentation should look like, review our guide on behavioral health documentation best practices.
The challenge? Most behavioral health EHR software is marketed with the same promises — streamlined workflows, easy billing, compliance built in. Every vendor's demo looks polished. The differences only surface once you're locked into a contract and running real sessions.
This buyer's guide gives you 20 targeted questions to ask during demos, free trials, and contract reviews — so you can separate the systems that actually support behavioral health workflows from the ones that just claim to.
Here’s how to think about the best behavioral health EHR based on your practice type and priorities:
Quick Picks: Best Behavioral Health EHR by Practice Type
There’s no single best behavioral health EHR for every practice. The right choice depends on your workflows, documentation style, and growth plans. Here’s how different types of platforms tend to perform across common use cases:
Best for Solo Practices
Look for systems that prioritize speed and simplicity. Platforms with structured documentation workflows—like ICANotes—can significantly reduce note-writing time for independent clinicians.
Best for Therapy Practices
Therapy-focused practices benefit from systems that support SOAP, DAP , and BIRP formats, along with long-term treatment planning. Structured, narrative-friendly platforms tend to perform best.
Best for Group Practices
Multi-provider practices need strong scheduling, role-based permissions, and integrated billing. Systems designed specifically for behavioral health scale more effectively as teams grow.
Best for Psychiatry
Psychiatry workflows require ePrescribing, E/M coding support, and medication tracking. Platforms with integrated prescribing and coding tools are typically the best fit.
Why Behavioral Health Practices Need a Specialized EHR
General-purpose EMR software wasn't built for therapy, psychiatry, or substance use treatment. Behavioral health documentation is fundamentally different from medical charting: session notes are narrative-driven, treatment plans evolve across months or years, and compliance requirements vary by payer, state, and accreditation body.
A purpose-built behavioral health EMR software handles these realities natively — with pre-configured templates, behavioral health–specific coding logic, and workflows that reflect how clinicians actually document care. A general EHR forces you to build those workflows yourself, which means more time configuring and less time with clients.
Many general systems fall short when it comes to documenting medical necessity, which is critical for reimbursement. Learn how to properly document medical necessity in mental health.
Before you start comparing platforms, get clear on what "built for behavioral health" should actually mean in practice.

Behavioral Health EHR vs. General EMR Software
A behavioral health EHR is designed around the workflows mental health practices actually use, while general EMR software often requires extra customization to fit therapy, psychiatry, and substance use treatment.
That difference matters because the wrong system may look capable in a demo but create daily friction once your clinicians start documenting real sessions, managing claims, and coordinating care. This distinction becomes especially important when considering how data is used across care settings and documentation workflows. For example, understanding how to write effective progress notes can highlight the difference between structured and generic systems.
Once you understand how behavioral health EHRs differ from general systems, the next step is evaluating how different platforms actually perform in practice.
How to Choose the Best Behavioral Health EHR
Choosing the best behavioral health EHR starts with evaluating how well a system supports your real-world workflows — not just how it performs in a demo. The right platform should reduce documentation time, connect clinical care to billing, and scale with your practice without adding administrative complexity.
A well-designed behavioral health EHR should support the full clinical and operational workflow — from scheduling through outcomes tracking.
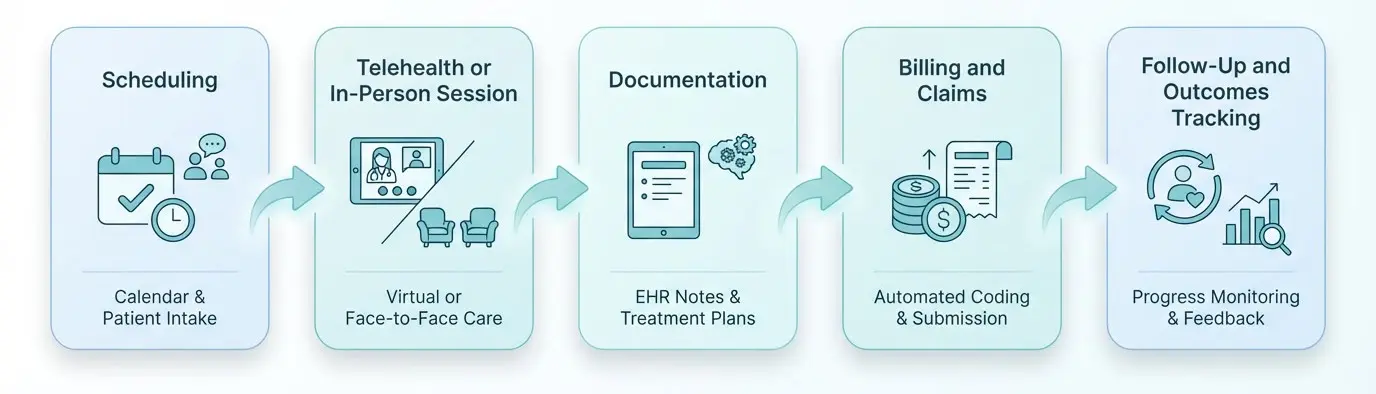
1. Evaluate Documentation Speed and Usability
Start with the most critical workflow: writing notes. If documentation is slow or cumbersome, everything else suffers.
During a trial, time how long it takes to complete a realistic progress note. The best behavioral health EHR software allows clinicians to create detailed, individualized notes quickly using structured content tools — not excessive typing or rigid templates. Look for systems that support behavioral health–specific formats like SOAP, DAP, and BIRP while still allowing clinical flexibility.
2. Confirm Billing and Claims Integration
Your EHR should connect documentation directly to billing without requiring manual steps.
Ask whether completing a note automatically generates a billable encounter with the correct CPT codes. Systems that require separate billing workflows introduce delays, errors, and lost revenue. Also evaluate clearinghouse integration, ERA posting, and how the system handles rejected claims.
For more information about billing, read our Complete Guide to Mental Health Billing.
3. Test Telehealth and Client Workflow Integration
Telehealth should be fully integrated — not a workaround.
Run a complete workflow: schedule a session, launch telehealth, complete documentation, and generate a claim. If any step requires switching tools or manual entry, it will create friction at scale. Also assess client-facing features like intake forms, reminders, and portal access, since these directly impact engagement and no-show rates.
4. Assess Compliance and Audit Support
Compliance isn’t optional — it’s built into every note and claim.
Look for systems that guide clinicians toward audit-ready documentation, flag incomplete notes, and maintain detailed audit trails. Behavioral health practices also need to consider requirements related to payer documentation standards and regulations like HIPAA and 42 CFR Part 2.
5. Evaluate Scalability and Practice Fit
The best behavioral health EHR should support your practice not just today, but as you grow.
Consider whether the platform can handle multiple providers, locations, and service types without requiring a system change. Evaluate role-based permissions, scheduling flexibility, and whether pricing scales reasonably as you add clinicians or expand services.
Once you’ve identified your priorities across documentation, billing, telehealth, compliance, and scalability, the next step is to pressure-test each system. Use the questions in this guide to evaluate how each platform performs in these core areas during demos and free trials.
How Behavioral Health EHR Platforms Compare
While many behavioral health EHR systems offer similar core features, the way those features are implemented can significantly impact day-to-day efficiency.
Platforms designed specifically for behavioral health — such as ICANotes — tend to align more closely with these best practices than general-purpose systems.
If you want to evaluate how a specific platform performs across these areas, use the checklist below during your next demo or trial.
Smart Questions to Ask Before Choosing a Mental Health EHR
Download this free printable checklist to bring to every vendor demo. It helps you compare behavioral health EHR software more confidently by focusing on the questions that matter most for documentation, billing, telehealth, compliance, and long-term fit.
- Evaluate behavioral health EHRs more objectively
- Bring smarter questions into every demo or trial
- Avoid hidden workflow, billing, and compliance gaps
- Print it, save it, or share it with your team
Get the Free Checklist
Fill out the form below and we’ll send it straight to your inbox.
Clinical Documentation and Note Efficiency
Documentation speed and quality are the foundation of any behavioral health EHR. If your system slows you down at the note-writing stage, everything downstream — billing, compliance, treatment planning — suffers.
1. How quickly can I complete a progress note?
Ask vendors to be specific. "Fast" is relative. The best behavioral health EHR systems let clinicians complete a detailed, clinically individualized progress note in two to three minutes using structured content tools — not free-text typing. During a trial, time yourself completing a note for a realistic session. If it takes longer than five minutes with content you'd actually submit, that's a red flag.
2. Does your system offer pre-built mental health templates (SOAP, BIRP, DAP, etc.)?
Templates should go beyond blank section headers. Look for systems where templates are pre-loaded with behavioral health–specific language, diagnoses, and clinical phrasing you can select and customize — not just empty fields labeled "Subjective" and "Objective." The best EMR software for behavioral health includes content libraries that reflect real clinical language across therapy, psychiatry, and substance use treatment.
3. Can notes auto-populate from prior sessions or carry forward clinically relevant information?
Carry-forward functionality saves significant time, but it also introduces compliance risk if it's not implemented carefully. Ask whether carried-forward content is clearly distinguished from new documentation, and whether clinicians can selectively carry forward specific elements rather than entire notes. A good behavioral health EHR makes carry-forward a clinical tool, not a copy-paste shortcut.
4. How does your system help ensure documentation meets payer and audit requirements?
This question reveals whether the platform actively supports compliance or just provides a blank canvas. Look for systems that flag incomplete documentation before it reaches billing, support auto-coding based on note content, and align note structures with common payer expectations. Behavioral health–specific coding logic — not generic medical coding — should be built in.
Compliance and Security
Compliance isn't a feature you check once during a demo. It's an operational reality that affects every note, every claim, and every client interaction. The questions below help you assess whether a behavioral health EHR treats compliance as a core design principle or an afterthought.
5. Is your EHR fully HIPAA-compliant, and what encryption standards are used?
Every vendor will say yes to HIPAA compliance. Push deeper. Ask about encryption at rest and in transit, how PHI is stored and segmented, and whether the platform has undergone independent security audits. For behavioral health specifically, ask how the system handles the heightened sensitivity of mental health and substance use records, which carry additional protections under federal regulations like 42 CFR Part 2.
6. Are audit trails, access logs, and PHI permissions built into the system?
Audit trails should show who accessed or changed records, when, and what was modified. This matters not just for regulatory compliance but for documentation defensibility — if a note is ever questioned during an audit, you need a clear chain of custody. Also ask whether the system distinguishes between note edits and formal amendments, since payers and accreditation bodies treat these differently.
7. Does your platform support compliance with CMS, CARF, and Joint Commission requirements?
If your practice participates in Medicare, Medicaid, or accredited programs, your documentation needs to meet specific standards. Ask how the system's note structures, treatment plan formats, and reporting capabilities align with these requirements. The best behavioral health EHR software doesn't just store your documentation — it guides clinicians toward compliant output. For guidance on compliance with Joint Commission and CMS standards, read our related guides on Mastering CMS Compliance in Mental Health and our Joint Commission Compliance Roadmap.
Telehealth and Client Engagement
Telehealth is no longer optional for most behavioral health practices. But "we have telehealth" can mean anything from a fully integrated video platform to a Zoom link pasted into a scheduling note. The distinction matters for workflow efficiency and billing accuracy.
8. Is telehealth built in, or do I need a third-party integration?
Built-in telehealth should mean the video session connects to the scheduled appointment, feeds into documentation, and flows into billing without manual steps. If telehealth requires a separate login, a separate platform, or manual linking to notes and claims, you're introducing friction and error points into every virtual session. During a trial, run a complete telehealth workflow — schedule, connect, document, bill — and see where the seams are.
9. Can clients schedule, complete intake forms, and pay through a secure portal?
A client portal should do more than display appointment times. Evaluate whether digital intake supports real behavioral health workflows — consent forms, screening tools, insurance information — and whether completed forms flow directly into the client chart without manual data entry. Also check whether staff can easily help clients who struggle with portal access, since onboarding friction directly affects no-show rates.
10. Are appointment reminders automated, and can I customize them?
Automated reminders reduce no-shows, but customization matters. Can you control the timing, channel (email vs. text), and content of reminders? Can you set different reminder sequences for different appointment types? And critically, does the reminder system integrate with the scheduling module so cancellations and reschedules update automatically?
Billing and Revenue Cycle Management
Billing gaps are where behavioral health practices lose the most money — and where EHR shortcomings cause the most frustration. The right behavioral health EMR software should make clean claim submission the default outcome of completing a clinical note, not a separate process that requires manual reconciliation.
11. Can claims be generated directly from completed notes?
This is the single most important billing question. If completing a clinical note doesn't automatically create a billable encounter with the correct codes attached, you're relying on manual processes that introduce errors, delays, and lost revenue. Ask to see this workflow live during a demo — complete a note and watch what happens on the billing side.
12. Does the system integrate with clearinghouses for claim submission and ERA posting?
Clearinghouse integration should be seamless, not bolted on. Ask whether claims can be submitted electronically from within the platform, whether electronic remittance advice (ERA) posts automatically, and whether rejected claims are flagged with actionable information. Also ask about filing deadline visibility — can you see which claims are approaching payer deadlines before they expire?
13. Are eligibility checks, copays, and superbills built into the workflow?
Front-end eligibility verification prevents claim denials before they happen. Check whether the system can verify insurance eligibility at scheduling or check-in, calculate expected copays, and generate superbills for out-of-network clients — all within the same workflow. If eligibility checks require a separate tool or manual lookup, that's a workflow gap that costs time and revenue.
Mental Health Practice Management Software Evaluation Checklist
Compare behavioral health EHR software side-by-side with this vendor-neutral scorecard. Evaluate scheduling, billing, telehealth, compliance, customization, and total cost of ownership — so you can make a confident decision before signing a contract.
- Score vendors across critical feature categories
- Identify hidden gaps in billing, compliance, and workflows
- Standardize your evaluation process across your team
- Make a more confident, data-driven EHR decision
Get the Free Checklist
Enter your details for instant access.
Group Practice Functionality
Solo clinicians can sometimes work around EHR limitations. Group practices cannot. If you're running or growing a multi-provider practice, these questions reveal whether a platform can scale with you or will become a bottleneck.
14. How does your EHR support multi-provider scheduling and documentation?
Multi-provider scheduling should handle the realities of group practice: varying session lengths, provider substitutions, coverage changes, and location-based scheduling. Ask whether the system can display and manage schedules across providers in a single view, and whether provider changes don't require duplicate scheduling entries. On the documentation side, ask whether each clinician can maintain their own documentation workflow within the same system.
15. Can multiple clinicians collaborate on shared treatment plans or group sessions?
Collaboration features matter for practices that co-treat clients, run group therapy, or coordinate across disciplines. Ask how the system handles shared treatment plans, whether group session documentation can be individualized per client, and whether role-based permissions allow appropriate access without overexposing sensitive records.
16. Are role-based permissions customizable?
Permissions should be granular — not all-or-nothing. Can you restrict access by note type, document type, or client? Can administrative staff access scheduling and billing without seeing clinical notes? Can supervisors review supervisee documentation without editing it? The best behavioral health EHR systems let you configure permissions that reflect your actual organizational structure.
Psychological Testing and Assessments
Standardized assessments are increasingly expected by payers and essential for outcome measurement. Your EHR should make administering, scoring, and integrating assessments a natural part of the clinical workflow — not a side process.
17. Are validated rating scales like PHQ-9, GAD-7, and MMSE available in the system?
Check whether commonly used behavioral health assessments are built in and whether they auto-score. Then ask the harder question: can you add additional assessments beyond the pre-loaded options? Practices that serve specialized populations or participate in outcome-based programs need flexibility to incorporate the specific tools their workflows require.
18. Does the system link assessment results to progress notes and treatment plans?
Assessment data is most valuable when it's connected to the clinical record — not trapped in a separate module. Ask whether scores appear within progress notes and treatment plans, whether trends are trackable over time, and whether outcome data can be reported on for program evaluation or payer reporting.
Pricing, Support, and Long-Term Fit
The final questions address the factors that determine whether your EHR relationship works over the long term. Hidden costs, inadequate support, and scalability limitations are the most common reasons practices switch systems — and switching is expensive.
19. What's included in the base price and what costs extra?
Ask specifically about telehealth, e-prescribing, text reminders, client portal access, and reporting. Are these included or gated behind higher subscription tiers? Also ask about training costs — is onboarding included for current staff, and is training available at no additional cost for future hires? Hidden fees for implementation, data migration, and support tiers are where "affordable" platforms become expensive.
20. Can I scale from a solo to a group practice without switching platforms?
Growth shouldn't require a technology overhaul. Ask whether adding providers or locations triggers pricing jumps, whether the platform's architecture supports multi-site management, and whether data migration from your current system is included or supported. If you're evaluating behavioral health EHR software as a solo clinician, think two to three years ahead — the cheapest option now may be the most expensive decision later.
How to Use These Questions Effectively
Asking the right questions is only half the process. How you evaluate the answers matters just as much.
During demos, watch for vague or deferred responses. Phrases like "we're working on that" or "that's on our roadmap" mean the feature doesn't exist today. If a vendor can't demonstrate a workflow live, it's not ready for your practice.
During free trials, test real workflows — not idealized scenarios. Schedule an actual appointment, write a note for a realistic session, submit a claim, and see where the process breaks down. A system that looks smooth in a guided demo may reveal friction when you're working independently.
During contract reviews, read the fine print on data ownership, export options, and cancellation terms. Ask about breach notification timelines and whether full data export is available if you leave. Your client records shouldn't be held hostage by a vendor relationship.
The goal isn't to find a system that checks every box. It's to identify the systems that can't support your core workflows — and eliminate them before you commit.
Choosing the Best Behavioral Health EHR for Your Practice
The best EHR for behavioral health is the one that fits the way your practice actually operates — not the one with the longest feature list or the most polished demo. Prioritize systems that are purpose-built for behavioral health, that connect clinical documentation to billing without manual steps, and that treat compliance as a design principle rather than a marketing claim.
If you're evaluating behavioral health EHRs, start by defining your non-negotiables: documentation speed, billing integration, telehealth, compliance support, and scalability. Then use the questions in this guide to pressure-test every platform against those requirements.
See What a Behavioral Health EHR Should Actually Feel Like
After evaluating your options, the real test is how a system performs in your day-to-day workflow. ICANotes is designed specifically for behavioral health, helping clinicians complete notes faster, reduce billing friction, and stay audit-ready—without adding complexity.
- Complete progress notes in minutes with structured templates
- Generate clean claims directly from documentation
- Built-in tools for compliance, telehealth, and assessments
- Designed exclusively for behavioral health workflows
Start Your Free Trial
No credit card required. Try ICANotes with your real workflows.
Related Resources for Choosing a Behavioral Health EHR
Explore these in-depth guides to better understand behavioral health EHR software, costs, and what to look for when evaluating vendors.
- Mental Health Practice Management Software: What Vendors Won’t Tell You
- Best EHR for Mental Health Private Practice
- Best Therapy Notes Software and EMR for Therapists
- Mental Health EHR Costs: What to Expect
- EHR for Small Behavioral Health Practices: What to Look for in 2025
- Step-by-Step EHR Data Migration Guide
Frequently Asked Questions
Below are answers to common questions about choosing a behavioral health EHR.
Related Posts

Sandy Crowley
Chief Marketing Officer
About the Author
Sandy Crowley is the Chief Marketing Officer at ICANotes, a leading EHR platform purpose-built for behavioral health. Sandy has over two decades of experience bridging healthcare, marketing, and software innovation. Formerly the company’s CEO, she guided ICANotes through a period of rapid growth and product expansion. With a background in communications from Stanford University and a passion for helping clinicians streamline documentation and improve outcomes, Sandy continues to drive ICANotes’ mission to make behavioral health software smarter, more efficient, and clinician-focused.





