Blog > Documentation > Anxiety SOAP Note Example + 5 Copy-Ready Templates
Anxiety SOAP Note Example + 5 Copy-Ready Templates for Clinicians
Writing an effective anxiety SOAP note requires more than documenting symptoms — it demands clear clinical reasoning, measurable progress, and a defensible treatment plan. In this guide, you’ll learn how to write compliant, audit-ready SOAP notes for anxiety and access five copy-ready examples covering GAD, panic disorder, social anxiety, and more. Whether you're a therapist or prescriber, these templates will help you document faster while supporting medical necessity and better patient outcomes.

Last Updated: April 13, 2026


What You'll Learn
- How to structure an anxiety SOAP note using Subjective, Objective, Assessment, and Plan
- What to document to support medical necessity and payer requirements
- How to capture anxiety severity, functional impairment, and risk level
- The difference between documenting GAD, panic disorder, and social anxiety
- How to write stronger Assessment and Plan sections that justify treatment
- Common SOAP note mistakes that can lead to denials or audit risk
- 5 copy-ready anxiety SOAP note examples you can adapt for your practice
Writing a thorough anxiety SOAP note requires more than documenting “anxious mood.” To meet clinical, legal, and payer expectations, your note must capture the nature of the patient’s anxiety symptoms, the severity and functional impact, diagnostic impressions, risk factors, and a clear treatment plan.
Whether you’re documenting generalized anxiety disorder (GAD), panic disorder, social anxiety, or anxiety co-occurring with insomnia, a well-structured SOAP note protects your practice, supports medical necessity, and tracks patient progress over time.
This guide walks you through each section of an anxiety SOAP note step by step and provides five copy-ready anxiety SOAP note examples you can adapt for your own clinical documentation.
What Is an Anxiety SOAP Note?
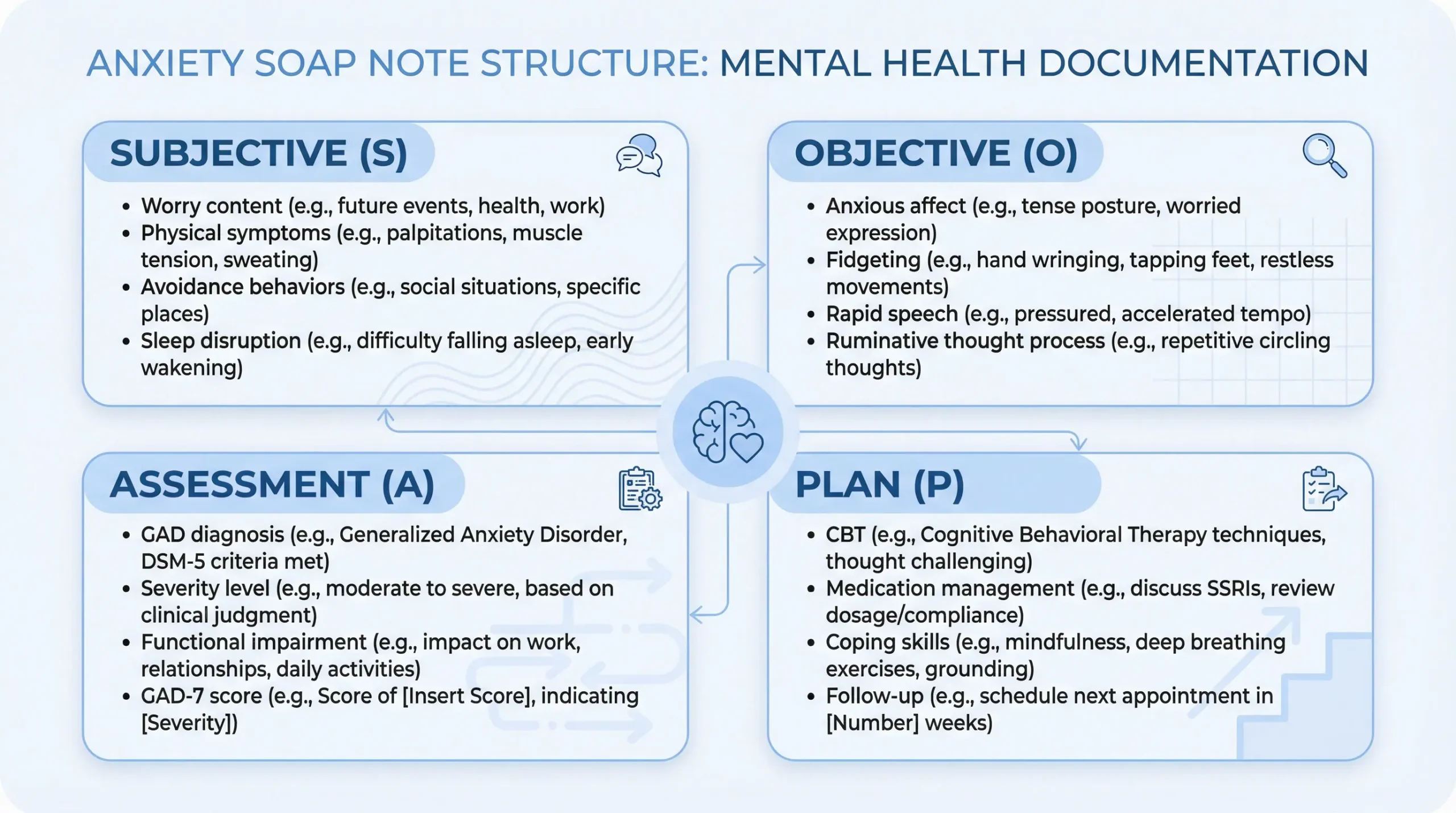
A SOAP note is a standardized documentation format used by mental health clinicians to organize session information into four sections: Subjective, Objective, Assessment, and Plan. When applied to anxiety-related sessions, the SOAP framework helps clinicians capture the full clinical picture — from the patient’s self-reported worry and physical symptoms to the clinician’s diagnostic formulation and next steps.
Subjective (S)
What the patient reports—worry content, physical symptoms, avoidance, panic episodes, sleep disruption, medication adherence, and safety concerns.
Objective (O)
What the clinician directly observes during the session, including mental status exam (MSE) findings such as appearance, speech, affect, thought process, and insight/judgment.
Assessment (A)
The clinician’s diagnostic impression, severity rating, functional impact, risk level, and treatment response.
Plan (P)
Medication adjustments, therapeutic interventions, coping strategies, referrals, and follow-up scheduling.
It’s worth noting that the focus of each section can vary depending on the provider’s role. A psychiatrist’s SOAP note for anxiety may lean more heavily on medication management and biological markers, while a therapist’s note will emphasize therapeutic interventions, session themes, and psychosocial factors. The SOAP structure accommodates both approaches.

Write Better Anxiety SOAP Notes With More Clarity and Less Stress
Download our free Mental Health SOAP Notes Guide to improve your anxiety documentation with practical examples, stronger clinical language, and tips that support medical necessity, compliance, and faster note-writing.
- How to document worry content, panic symptoms, avoidance, and functional impairment
- SOAP note examples and formatting tips for behavioral health clinicians
- Practical guidance to make anxiety SOAP notes more complete and audit-ready
- Tips for writing faster without sacrificing clinical quality
Get the guide instantly and start writing stronger anxiety SOAP notes today.
How to Write a SOAP Note for Anxiety (Step by Step)
The following step-by-step breakdown covers what to include in each section of an anxiety SOAP note, with specific language and clinical detail that supports both treatment planning and payer documentation requirements.
Step 1: Subjective — What the Patient Reports
The Subjective section captures the patient’s own report of their anxiety symptoms, concerns, and functioning since the last session. For anxiety presentations, this section should clearly reflect what the patient is experiencing in their own words.
- Nature of worries, including whether the worries are generalized or tied to specific situations
- Duration and frequency of symptoms, such as daily anxiety, episodic spikes, or trigger-based distress
- Physical symptoms like restlessness, muscle tension, heart pounding, shortness of breath, dizziness, or GI distress
- Panic episodes, including frequency, duration, trigger context, and peak intensity when present
- Avoidance behaviors involving work, school, driving, public places, or social situations
- Functional impairment affecting relationships, work performance, self-care, sleep, or daily routines
- Medication adherence, missed doses, side effects, or concerns about current treatment
- Safety screening, including suicidal ideation, self-harm urges, or other immediate concerns (even when negative)
Strong Anxiety Subjective Sections Often Include
Tip: Use the patient’s own language when possible. A quote like “I can’t turn my brain off” often communicates severity more clearly than a generic statement such as “patient reports anxiety.”
Step 2: Objective — What the Clinician Observes
The Objective section documents what you directly observe during the session, typically through mental status exam findings. This section should stay separate from patient self-report and focus on clinical observation.
- Appearance, such as tense posture, fidgeting, poor eye contact, restlessness, or nail biting
- Speech characteristics including rate, volume, rhythm, hesitation, or pressured speech
- Affect, especially whether it appears anxious, fearful, tense, or congruent with stated mood
- Thought process, including rumination, circumstantiality, tangentiality, or perseverative worry
- Thought content such as catastrophic thinking, excessive worry, or intrusive thoughts
- Insight into the anxiety symptoms and whether the patient recognizes them as excessive or disproportionate
- Judgment and decision-making related to treatment participation and symptom management
Focus Areas for Anxiety-Related Objective Findings
Tip: Avoid simply repeating the patient’s self-report here. The Objective section should reflect what you observed, not what the patient told you.
Step 3: Assessment — Clinical Impression and Severity
The Assessment section synthesizes the Subjective and Objective findings into a clinical formulation. This is where you document your diagnostic impression, severity, functional impact, and overall interpretation of the case.
- Diagnosis with the appropriate ICD-10 code, such as GAD (F41.1), panic disorder (F41.0), social anxiety disorder (F40.10), or unspecified anxiety disorder (F41.9).
- Severity rating, such as mild, moderate, or severe
- Standardized measure results when available, including GAD-7, PHQ-9, BAI, or other symptom scales
- Functional impact across occupational, social, academic, or daily living domains
- Risk level and the rationale supporting that determination
- Treatment response, including whether symptoms are improving, stable, worsening, or unchanged from baseline
A Strong Assessment Should Answer
Tip: Use measurable symptom change when possible. Referencing score changes over time helps demonstrate treatment response and supports continued care.
Step 4: Plan — Next Steps in Treatment
The Plan section documents what happens next. A clear, specific plan shows clinical reasoning, supports continued authorization, and tells the next provider exactly how treatment is moving forward.
- Medication management, including current medications, dosage changes, new prescriptions, or discontinuation rationale
- Therapeutic interventions such as CBT, exposure therapy, ACT, relaxation training, psychoeducation, or mindfulness-based strategies
- Coping skills practiced in session or assigned for between-session use, such as grounding techniques, diaphragmatic breathing, or cognitive restructuring
- Referrals to psychiatry, primary care, group therapy, lab work, or other services when needed
- Follow-up timing, homework, and any specific next-session priorities
Strong Anxiety Plans Often Include
Tip: Avoid vague language like “continue therapy.” Instead, specify the intervention, skill focus, medication plan, and follow-up timeframe.
Anxiety SOAP Note Examples & Templates
Below are five anxiety SOAP note examples covering common clinical presentations. Each is formatted in standard SOAP structure and written with copy-ready language you can adapt for your documentation.
1. Generalized Anxiety Disorder (GAD) SOAP Note Example
Patient is a 34-year-old female presenting for a follow-up session. She reports persistent, excessive worry about work performance, finances, and her children’s health over the past two weeks. She describes difficulty controlling the worry, stating, “I can’t turn my brain off.” She endorses restlessness, muscle tension in her neck and shoulders, difficulty concentrating, and disrupted sleep (averaging 4–5 hours per night). She denies panic attacks. She reports avoiding team meetings at work due to fear of being judged. She is adherent to sertraline 100 mg daily and reports no side effects. She denies suicidal ideation, self-harm urges, or homicidal ideation.
Patient is casually dressed and groomed. She appears tense, with intermittent fidgeting and restless leg movement throughout the session. Speech is normal in rate and volume but becomes rapid when discussing work stressors. Mood is “anxious.” Affect is anxious and congruent with stated mood. Thought process is linear but ruminative, with perseverative worry about worst-case scenarios. Thought content is negative, focused on catastrophic outcomes. No perceptual disturbances. Insight is fair—she recognizes her worry is excessive but struggles to interrupt it. Judgment is intact. GAD-7 score: 14 (moderate).
Generalized Anxiety Disorder (F41.1), moderate severity. GAD-7 decreased from 17 to 14 since last session, indicating modest improvement. Anxiety continues to impair occupational functioning (avoidance of meetings) and sleep quality. No acute safety concerns. Risk level: low.
Continue sertraline 100 mg daily. Continue cognitive behavioral therapy with focus on cognitive restructuring around catastrophic thinking patterns. Introduced worry time technique—patient will practice scheduling a 15-minute daily worry window. Assigned progressive muscle relaxation exercises for sleep onset. Follow-up in two weeks. Patient is agreeable to the plan.
2. Panic Disorder SOAP Note Example
Patient is a 28-year-old male presenting for an initial psychiatric evaluation. He reports recurrent, unexpected panic attacks over the past three months, occurring approximately 3–4 times per week. He describes episodes of sudden intense fear accompanied by heart pounding, chest tightness, shortness of breath, dizziness, and tingling in his hands. Episodes last approximately 10–15 minutes and peak within minutes of onset. He reports persistent worry about having another attack and has begun avoiding driving on the highway and crowded stores. He missed three days of work in the past month due to panic symptoms. He denies substance use. He denies suicidal ideation, self-harm, or homicidal ideation.
Patient is well-groomed and alert. He is visibly anxious, with perspiration on his forehead and rapid speech when describing episodes. Mood is “on edge.” Affect is anxious and mildly restricted. Thought process is logical but preoccupied with somatic symptoms. Thought content includes fear of cardiac event during episodes; denies psychotic symptoms. Insight is good—he recognizes the episodes as panic attacks. Judgment is intact. PHQ-9 score: 8 (mild depressive symptoms). GAD-7 score: 16 (severe).
Panic Disorder (F41.0), moderate-to-severe, with agoraphobic avoidance features. Panic attacks are frequent, causing significant occupational and social impairment. Mild comorbid depressive symptoms likely secondary to anxiety. No acute safety concerns. Risk level: low.
Initiate escitalopram 5 mg daily, increasing to 10 mg after one week if tolerated. Psychoeducation provided on the panic cycle and the role of avoidance in maintaining symptoms. Refer to therapist for CBT with interoceptive exposure. Provided patient with psychoeducation handout on panic disorder. Follow-up in two weeks to assess medication tolerance and symptom response. Patient was receptive to the plan.
3. Social Anxiety Disorder SOAP Note Example
Patient is a 22-year-old female college student presenting for a follow-up therapy session. She reports ongoing fear of being negatively evaluated in social and performance situations. She describes intense anxiety before and during class presentations, stating, “I feel like everyone is watching me and thinking I’m stupid.” She reports blushing, trembling, and a “blank mind” during her most recent presentation. She has begun skipping classes where participation is graded. She denies panic attacks but reports anticipatory anxiety that builds for days before events. She reports adequate sleep and appetite. She denies suicidal ideation, self-harm, or homicidal ideation.
Patient is neatly dressed. She avoids sustained eye contact and speaks softly, particularly when discussing social fears. Mood is “nervous.” Affect is anxious and somewhat constricted. Thought process is linear with themes of self-doubt and anticipated rejection. Thought content includes negative self-appraisal (“I always say the wrong thing”). No perceptual disturbances. Insight is good—she identifies her fears as disproportionate. Judgment is fair, impaired by avoidance. SPIN score: 38 (moderate social anxiety).
Social Anxiety Disorder (F40.10), moderate severity. Social anxiety is significantly impairing academic performance and peer relationships. Avoidance pattern is entrenched and expanding, now including skipping graded participation. No acute safety concerns. Risk level: low.
Continue weekly CBT. Introduced graded exposure hierarchy targeting classroom participation. This session focused on cognitive restructuring of core belief “Others are judging me negatively.” Assigned behavioral experiment to initiate one brief comment in a small class and log the outcome. Discussed potential medication consultation if avoidance continues to impair academic functioning. Follow-up next week.
4. Anxiety Medication Follow-Up SOAP Note Example
Patient is a 45-year-old male returning for a four-week medication follow-up. He was started on venlafaxine 75 mg daily for generalized anxiety disorder at his last visit. He reports a noticeable reduction in baseline worry and states, “The constant knot in my stomach has let up some.” He continues to experience mild restlessness in the evenings and occasional difficulty falling asleep but reports improved concentration at work. He denies nausea, dizziness, or sexual side effects. He is adherent to his medication regimen. He denies suicidal ideation, self-harm urges, or homicidal ideation.
Patient is well-groomed and cooperative. He appears more relaxed than at his previous visit. Speech is normal in rate and volume. Mood is “better, not perfect.” Affect is mildly anxious but brighter than baseline. Thought process is linear and goal-directed. Thought content includes ongoing worry about job security but at reduced intensity. No perceptual disturbances. Insight and judgment are intact. Vitals: BP 128/82, HR 76. GAD-7 score: 10 (moderate), down from 18 at baseline.
Generalized Anxiety Disorder (F41.1), moderate severity, improving. Patient is showing a clinically meaningful response to venlafaxine 75 mg, with GAD-7 reduced from 18 to 10 over four weeks. Residual evening restlessness and mild sleep-onset difficulty persist. No adverse effects reported. No acute safety concerns. Risk level: low.
Increase venlafaxine to 150 mg daily to target residual symptoms. Continue sleep hygiene recommendations. Reassess in four weeks for treatment response and tolerability. Consider adding short-term hydroxyzine 25 mg PRN if evening restlessness does not improve with dosage increase. Patient agrees with the plan.
5. Anxiety With Insomnia SOAP Note Example
Patient is a 38-year-old female presenting for a therapy session. She reports worsening anxiety and insomnia over the past three weeks following a job loss. She describes lying awake for 2–3 hours at night with racing thoughts about financial concerns, worst-case scenarios, and self-blame. She reports averaging 3–4 hours of sleep per night, daytime fatigue, irritability, and difficulty managing daily tasks. She endorses restlessness and muscle tension. She denies using alcohol or sleep aids. She reports reduced appetite but denies weight loss. She denies suicidal ideation, self-harm, or homicidal ideation.
Patient appears fatigued, with dark circles under her eyes. She is dressed casually and appropriately. She yawns several times during the session. Speech is normal but slowed. Mood is “anxious and exhausted.” Affect is anxious and flat. Thought process is ruminative with repetitive worry loops. Thought content focuses on financial ruin and self-criticism. No perceptual disturbances. Insight is fair. Judgment is intact. GAD-7 score: 15 (moderate). ISI score: 21 (moderate-to-severe insomnia).
Generalized Anxiety Disorder (F41.1), moderate severity, exacerbated by acute psychosocial stressor (job loss). Comorbid insomnia disorder, moderate to severe, likely maintained by anxiety-driven cognitive hyperarousal. Anxiety and insomnia are mutually reinforcing and collectively impairing daily functioning. No acute safety concerns. Risk level: low.
Initiate CBT-I alongside ongoing anxiety-focused CBT. Introduced stimulus control strategies, including using the bed only for sleep, leaving the bedroom if awake for more than 20 minutes, and maintaining a consistent wake time. Practiced sleep-focused cognitive restructuring targeting catastrophic beliefs about sleep loss. Assigned a sleep diary for the next two weeks. Will discuss medication options if behavioral strategies do not sufficiently improve sleep. Follow-up in one week.
Risk Assessment Language for Anxiety Notes
Documenting risk and safety is essential in every anxiety SOAP note, even when the patient presents as low risk. Using clear, consistent language demonstrates clinical diligence and protects your practice in the event of an audit or legal review. Below are copy-ready phrases you can incorporate into the Subjective and Assessment sections of your anxiety notes:
- Patient denies suicidal ideation, intent, or plan. Denies self-harm urges. Denies homicidal ideation.
- Patient denies panic-related emergency room visits since last session.
- No evidence of psychotic features, manic symptoms, or substance-related impairment.
- No imminent safety concerns identified at this time. Risk level assessed as low.
- Safety plan reviewed and remains in place. Patient identifies [support person] as primary emergency contact.
- Patient reports passive suicidal ideation without intent or plan. Safety plan reviewed and updated. Emergency contacts confirmed. Follow-up shortened to [timeframe].
Always document the specific screening performed (e.g., PHQ-9 item 9, Columbia Suicide Severity Rating Scale) and the patient’s response, even when the response is negative. Payers and auditors expect to see that safety was addressed, not assumed.
Common Mistakes in Anxiety SOAP Notes
Even experienced clinicians can fall into documentation habits that weaken the clinical and legal value of their notes. Here are the most common mistakes to avoid when writing anxiety SOAP notes:
- Documenting only “anxious mood” without detail. A one-word descriptor doesn’t capture the nature, severity, or functional impact of anxiety. Specify what the patient is anxious about, how it manifests, and how it affects daily life.
- Missing functional impairment. Payers use functional impairment to determine medical necessity. If your note doesn’t explain how anxiety is affecting work, relationships, sleep, or daily activities, it may not support continued authorization.
- Failing to document panic frequency and characteristics. If the patient reports panic attacks, document how often they occur, how long they last, what triggers them, and the specific symptoms experienced.
- No measurable symptom change between sessions. Use standardized measures like the GAD-7 or BAI and reference score changes over time to demonstrate treatment progress or justify adjustments.
- Weak or vague Plan section. “Continue therapy” is not a sufficient plan. Specify the intervention modality, skills being targeted, medication changes, homework assignments, and follow-up timing.
- Blurring Subjective and Objective sections. The Subjective section reflects what the patient reports. The Objective section captures what the clinician observes. Restating self-reported symptoms as objective findings undermines the clinical structure of the note.
How ICANotes Helps You Write Better Anxiety SOAP Notes
Writing high-quality anxiety SOAP notes takes time — especially when you’re trying to balance clinical detail, compliance, and a full caseload. ICANotes is designed specifically for behavioral health clinicians to make that process faster, easier, and more consistent.
With ICANotes, you can generate structured, compliant SOAP notes using intuitive point-and-click templates tailored to anxiety disorders like GAD, panic disorder, and social anxiety. Instead of starting from scratch, the system guides you through clinically relevant prompts, helping you capture key details like worry content, functional impairment, and treatment response.
ICANotes also helps ensure your documentation supports medical necessity by organizing your notes into clear, defensible Subjective, Objective, Assessment, and Plan sections. Built-in phrasing and customizable options allow you to create detailed notes in minutes — without sacrificing quality.
The result? More complete anxiety documentation, reduced risk during audits, and more time to focus on your clients instead of your notes.

Write Better Anxiety SOAP Notes in Less Time
ICANotes helps behavioral health clinicians create faster, more complete, and more defensible anxiety SOAP notes with point-and-click documentation designed specifically for mental health.
- Built-in templates for anxiety, panic, and related disorders
- Clinical language that supports medical necessity
- Faster documentation with structured workflows
- No credit card required
Start Your Free Trial
Complete the form below to try ICANotes free for 30 days.
Related Resources for Better SOAP Notes and Anxiety Documentation
Continue improving your clinical documentation with these related guides on anxiety assessment, treatment planning, and SOAP note best practices.
Frequently Asked Questions About SOAP Notes for Anxiety
How do you write a SOAP note for anxiety?
Start by documenting what the patient reports in the Subjective section, including the nature of their worry, physical symptoms, avoidance behaviors, functional impairment, and safety screening. In the Objective section, record your mental status exam observations. The Assessment should include the diagnosis with ICD-10 code, severity, functional impact, and risk level. The Plan should specify interventions, medication management, coping strategies, and the follow-up timeline.
What should be included in an anxiety SOAP note?
An effective anxiety SOAP note includes the type and severity of anxiety symptoms, physical manifestations, avoidance patterns, functional impairment, mental status exam findings, a diagnosis with supporting rationale, a risk assessment, and a specific treatment plan. Including standardized measure scores such as the GAD-7 strengthens the note’s clinical value.
How do you document panic attacks in a SOAP note?
Document the frequency of panic attacks, duration, trigger context if identifiable, peak intensity, and the specific physical symptoms experienced during episodes. In the Objective section, note any signs of autonomic arousal observed during the session. The Assessment should reflect the panic disorder diagnosis, and the Plan should address both acute management strategies and longer-term treatment such as CBT with interoceptive exposure.
How long should an anxiety SOAP note be?
There is no fixed length requirement, but a thorough anxiety SOAP note typically ranges from one to two pages. The note should be long enough to establish medical necessity, document clinical decision-making, and capture meaningful symptom detail, but concise enough to be practical for regular use. Structured EHR templates can help clinicians produce comprehensive notes efficiently without adding time to each session.
What is the difference between GAD and panic disorder documentation?
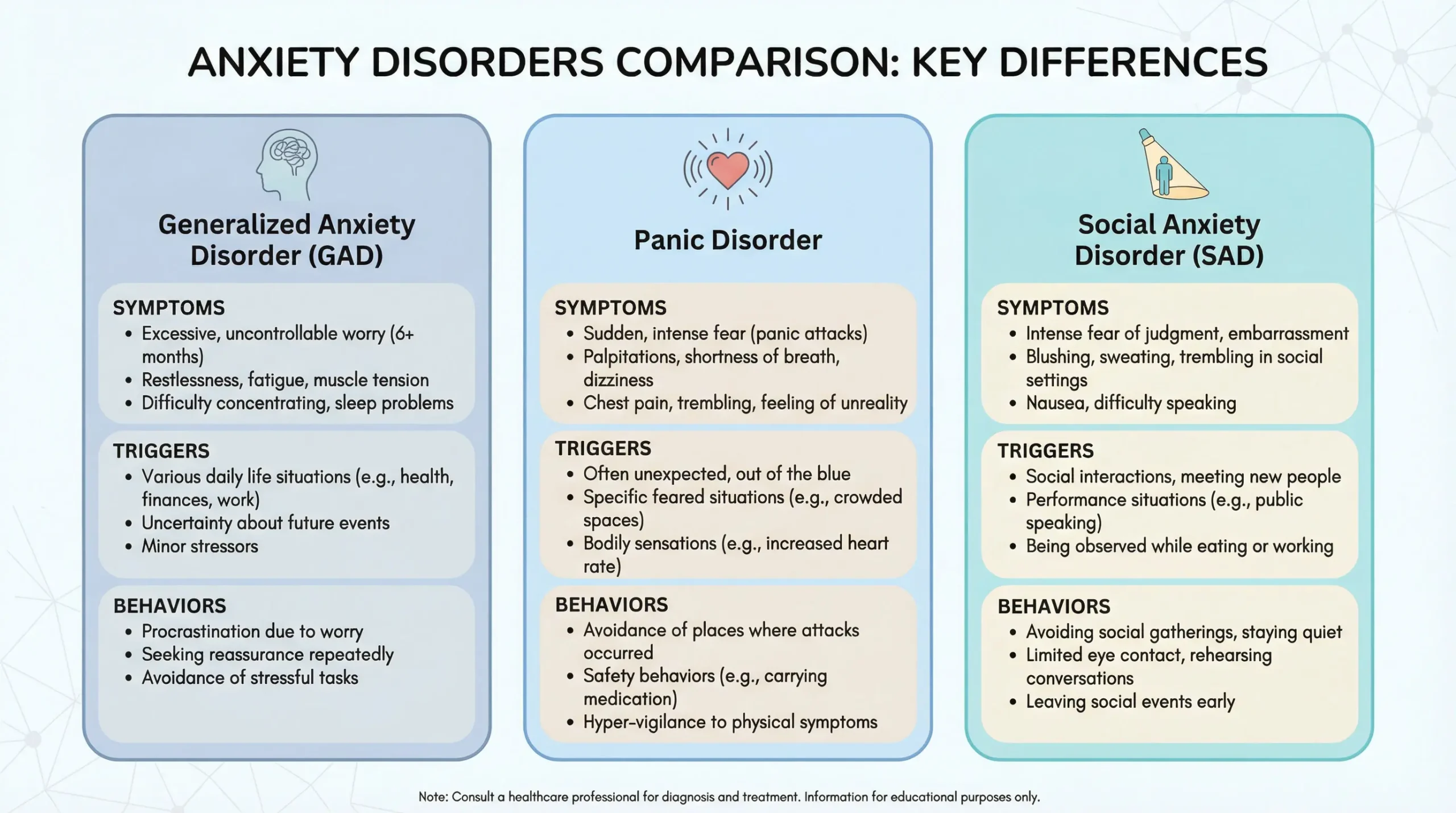
GAD documentation focuses on persistent, excessive worry across multiple domains, difficulty controlling the worry, and associated physical symptoms like restlessness and muscle tension. Panic disorder documentation centers on recurrent, unexpected panic attacks, the specific physical symptoms during episodes, avoidance behaviors that develop in response to the attacks, and persistent concern about future episodes. Both require a clear diagnosis, severity assessment, and specific treatment plan, but the clinical language and focus differ.
Recent Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.





