Blog > Documentation > Mental Health Documentation Best Practices: Guidelines & Cheat Sheet
Mental Health Documentation Best Practices (Guidelines and Cheat Sheet)
Mental health documentation is more than record-keeping — it’s the foundation of consistent, compliant, and defensible behavioral health care. Clinicians rely on accurate documentation to track progress, coordinate treatment, meet billing requirements, and reduce legal risk. In this guide, you’ll learn essential mental health documentation guidelines, see real charting examples, and access a printable cheat sheet and psychiatric documentation checklist to improve your clinical notes.

Last Updated: April 10, 2026


What You'll Learn
- Why mental health documentation matters for clinical care, compliance, billing, and risk management
- Mental health documentation guidelines for every stage of care, from intake to discharge
- What to include in clinical notes, with real mental health charting examples
- Best practices for writing defensible documentation that supports medical necessity
- A printable mental health documentation cheat sheet for daily reference
- A psychiatric documentation checklist covering intake, progress notes, and discharge
- Tips to streamline behavioral health documentation using EHR tools and templates
Contents
Why Quality Mental Health Documentation Matters
Mental Health Documentation Guidelines - Intake to Discharge
Mental Health Charting Examples (Good vs Bad Notes)
Mental Health Documentation Best Practices: Do's and Don'ts
How to Document Medical Necessity in Mental Health
Behavioral Health Documentation Requirements for Insurance
Psychiatric Documentation Checklist: Intake to Discharge
Tips to Improve Mental Health Documentation
FAQs: Mental Health Documentation
Simplify Mental Health Documentation with ICANotes
Why Quality Mental Health Documentation Matters
Quality mental health documentation does more than record sessions — it supports clinical care, compliance, and professional accountability. Here are four key reasons why writing good notes matters.
1. Continuity of Care and Clinical Insight
Well-written notes help any clinician (or future you) quickly understand a client’s history, treatment trajectory, and clinical decisions. When a client transfers between providers or returns after a gap in treatment, thorough behavioral health documentation ensures nothing falls through the cracks.
2. Legal, Ethical, and Risk Management Defense
Documentation serves as your best defense if questions arise about treatment decisions or care continuity. Experts recommend completing notes within 48 hours, when details are still fresh. In a malpractice case or licensing board review, your notes are the primary evidence of what happened — and what didn’t.
3. Justification for Billing and Medical Necessity
Strong documentation demonstrates that the sessions and therapeutic interventions were necessary and appropriate, which is required by payers and auditors. Without clear documentation of medical necessity, even clinically sound treatment can result in denied claims or audit recoupments.
4. Professional Accountability and Quality Control
Following mental health documentation guidelines helps standardize care, reduces ambiguity, and makes audits or peer reviews smooth. Consistent documentation practices also help supervisors identify training needs and ensure staff are meeting organizational and regulatory standards.
Mental Health Documentation Guidelines: Intake to Discharge
Mental health documentation guidelines are standardized practices that ensure clinical notes are accurate, compliant, and support medical necessity for billing and care continuity. Effective behavioral health documentation follows a structured process that mirrors the client’s journey in treatment. By applying consistent mental health documentation guidelines from the first intake form to the final discharge summary, clinicians create records that are defensible, compliant, and clinically useful.
The Mental Health Documentation Process
From intake to discharge, each stage of documentation supports continuity of care, compliance, and clinical decision-making.
Intake
Collect baseline information, presenting concerns, consent, history, and referral details.
Assessment
Record symptoms, clinical impressions, diagnoses, and screening or MSE findings.
Treatment Plan
Establish SMART goals, planned interventions, review timelines, and expected outcomes.
Progress Notes
Track interventions, client response, measurable progress, and ongoing medical necessity.
Discharge
Summarize care provided, outcomes, remaining needs, and aftercare recommendations.
1. Intake Documentation
At the intake stage, clinicians gather a wide range of baseline information: presenting concerns, personal and family psychiatric history, medical history, risk factors, and consent forms. This documentation establishes the foundation for treatment and ensures care begins with a clear, informed baseline.
Best Practice Tip: Always document informed consent and confidentiality agreements, as these are key legal protections.
For a complete guide to conducting a successful client intake, please read our related post: A Guide to Successful Mental Health and Psychiatry Intake .
2. Initial Assessment Notes
Assessment documentation captures your clinical impressions and diagnostic reasoning. This may include results from standardized screening tools, observations from a mental status exam, and diagnostic impressions. Strong assessment notes justify the need for care and support medical necessity requirements for billing and insurance.
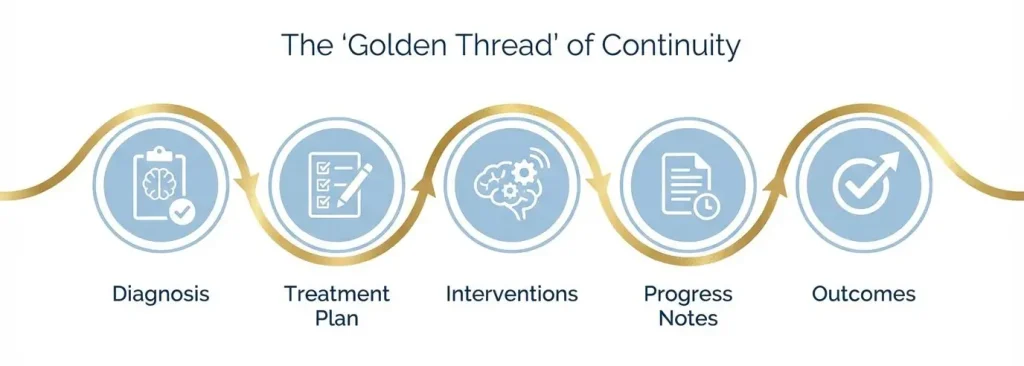
Best Practice Tip: Link assessments directly to treatment goals to create a clear “golden thread” in your documentation. The visual below illustrates how each stage of documentation connects to form the “golden thread.”
For more guidance, read our related articles on writing a biopsychosocial assessment and conducting an initial psychiatric evaluation .
3. Treatment Planning
A treatment plan is the roadmap for care. It should include individualized measurable goals, planned interventions, and expected outcomes. Documenting treatment plans in line with mental health documentation guidelines ensures alignment with payer expectations and provides a framework to measure progress.
Best Practice Tip: Write goals that are SMART (Specific, Measurable, Achievable, Relevant, Time-bound).
For more detailed information, read our related Guide to Creating Mental Health Treatment Plans .
4. Ongoing Progress Notes
Progress notes document what occurs in each session, including session details, interventions used, and the client’s response. Using structured formats like SOAP, DAP, or BIRP notes helps maintain consistency and defensibility. Thorough progress notes support continuity of care, demonstrate ongoing medical necessity, and protect clinicians in the event of an audit.
Best Practice Tip: Use objective language — focus on observable behaviors and direct client quotes rather than vague impressions.
For more information on writing the best progress notes, review our related articles:
How Strong Are Your Progress Notes?
Take our free 5-minute Progress Note Self-Assessment Tool to see how your documentation stacks up. Identify gaps, reduce compliance risk, and get practical insight into whether your notes are audit-ready.
It’s a quick way to spot documentation weaknesses before they become billing or compliance problems.
Take the 5-Minute Self-Assessment
5. Discharge Summaries
At the end of treatment, discharge documentation provides a summary of care, client progress, remaining challenges, and aftercare recommendations. Discharge summaries are critical for both legal protection and continuity of care if the client transitions to another provider.
Best Practice Tip: Document reasons for discharge (e.g., treatment goals met, referral, non-compliance) and include specific aftercare recommendations.
For detailed guidance, read our related article on writing a mental health discharge summary .
What Should Be Included in Every Mental Health Note?
A high-quality mental health note should include the following elements, adapted from standard templates like SOAP, DAP, and BIRP.
| Section | What to Document | Why It Matters |
|---|---|---|
| Session Details | Date, time (start/stop), location, provider name/credentials, client identifiers | Ensures clarity and audit compliance |
| Subjective / Data / Behavior | What the client says or reports; include direct quotes when relevant | Shows authenticity and the client’s voice |
| Objective / Observations | Observable behavior and MSE indicators (appearance, speech, affect, thought process) | Grounds clinical impressions in facts |
| Assessment / Interpretation | Clinician’s interpretation of status, progress, barriers; diagnostic reasoning | Connects data to clinical decision-making |
| Interventions / Treatment | Techniques or approaches used (e.g., CBT, DBT, MI) and rationale | Demonstrates active therapeutic work |
| Response / Client Reaction | Client’s response to interventions (e.g., engaged, resistant, emotional) | Shows progress or lack thereof |
| Plan / Next Steps | Goals, homework, referrals, safety plan, next appointment | Keeps treatment moving forward |
| Diagnosis & Codes | DSM/ICD diagnosis and applicable billing codes | Supports clarity, coordination, and billing |
| Safety / Risk Assessment | Any suicidal ideation, self-harm risk, or risk to others; mitigation steps | Essential for client safety and liability reduction |
Access Our Sample Notes Library
Get instant access to our full library of sample behavioral health notes, including Initial Evaluations, Progress Notes, Treatment Plans, and Discharge Summaries. We have note samples for psychiatry, therapy, case management, PRP, substance abuse, group therapy, couples therapy, and more!

Mental Health Charting Examples (Good vs. Bad Notes)
One of the most effective ways to improve mental health clinical documentation is to see what strong charting looks like compared to weak charting. The table below shows common documentation mistakes alongside improved versions that meet behavioral health documentation requirements.
| Element | ❌ Weak Documentation | ✅ Strong Documentation |
|---|---|---|
| Subjective | "Client seemed upset." | "Client reported feeling overwhelmed by work stress, stating, 'I can’t stop thinking about it even at night.'" |
| Objective | "Client looked nervous." | "Client appeared tearful with slow, halting speech. Avoided eye contact. Fidgeted with hands throughout session." |
| Assessment | "Client is doing better." | "Client demonstrates improvement in mood regulation, reporting a decrease in depressive episodes from daily to 2–3 times per week since initiating CBT interventions." |
| Intervention | "Discussed coping skills." | "Utilized cognitive restructuring (CBT) to challenge client’s automatic thought pattern: 'I’m a failure.' Client identified two alternative thoughts and rated belief in the original thought at 40% (down from 80%)." |
| Plan | "Continue therapy." | "Continue weekly individual therapy focused on CBT for depression. Client to complete thought record worksheet between sessions. Reassess PHQ-9 at next visit. Follow up on PCP referral for sleep concerns." |
| Risk | "No SI." | "Client denied current suicidal ideation, intent, and plan. No history of prior attempts. Identified spouse and faith community as protective factors. Safety plan reviewed and remains current." |
These mental health charting examples illustrate the difference between notes that would survive an audit and notes that would raise red flags. The key: be specific, be objective, and connect everything back to the treatment plan.
Mental Health Documentation Best Practices: Do's and Don'ts
Following clear mental health documentation guidelines helps ensure your notes are professional, defensible, and clinically valuable. Use these do’s and don’ts as a quick reference when writing progress notes, treatment plans, and discharge summaries.
✅ Do’s of Mental Health Documentation
- Do document promptly. Complete your notes within 24–48 hours to maintain accuracy and compliance with best practice standards.
- Do use objective, descriptive language. Record observable behaviors (e.g., “client appeared tearful, with slow speech”) rather than vague impressions ("seemed upset").
- Do link notes to the treatment plan. Maintain the “golden thread” by tying progress notes and interventions directly to client goals.
- Do include client strengths and progress. Highlight resilience and improvement alongside challenges to present a balanced clinical picture.
- Do quote clients when appropriate. Direct quotes add authenticity and show that notes reflect the client's own words.
- Do ensure confidentiality. Protect client privacy by following HIPAA standards and limiting details to those clinically relevant.
- Do use structured formats. SOAP, DAP, or BIRP templates promote consistency adn align with common mental health documentation guidelines.
❌ Don’ts of Mental Health Documentation
- Don’t use vague terms or jargon. Avoid words like "doing better" or shorthand that could be unclear to others reviewing the record.
- Don’t include unnecessary personal details. Stick to clinically relevant information and avoid speculation.
- Don’t alter or backdate notes. Make corrections transparently with dates and initials.
- Don’t copy and paste previous notes. Each entry should reflect the unique session and client's current status.
- Don’t overlook risk factors. Always document suicidal ideation, self-harm, or harm-to-others risk and safety concerns thoroughly.
- Don’t let notes pile up. Writing retroactively increases the risk of incomplete or inaccurate documentation.
- Don’t forget signatures. Every entry should be dated and signed (or electronically authenticated in your EHR).
Applying these do’s and don’ts makes clinical notes clear, defensible, and aligned with mental health documentation best practices. By avoiding common pitfalls and sticking to proven strategies, clinicians can reduce liability, support billing requirements, and deliver better client care.

Free Download
Mental Health Documentation Cheat Sheet
Download the Mental Health Documentation Cheat Sheet to improve note quality, ensure compliance, and support stronger reimbursement with audit-ready documentation.
- Improve documentation quality and consistency
- Support medical necessity and reimbursement
- Use clear examples to strengthen progress notes
Get the free cheat sheet
How to Document Medical Necessity in Mental Health
Medical necessity in mental health documentation means clearly showing that treatment is clinically appropriate and required to address a diagnosed condition and functional impairment. Documenting medical necessity is one of the most critical — and most frequently failed — aspects of behavioral health documentation. Payers require clear evidence that services are reasonable and necessary to treat a diagnosed condition. Without it, claims get denied, payments get delayed, and audits get triggered.
For a deeper dive, including step-by-step examples and common audit pitfalls, read our full guide on how to document medical necessity in mental health.
What Medical Necessity Documentation Should Include
To meet behavioral health documentation requirements for medical necessity, every session note should address these elements:
Presenting Symptoms and Functional Impairment
Describe how the client’s condition affects daily functioning, relationships, work, or self-care.
Example: “Client reports inability to concentrate at work due to intrusive thoughts, resulting in two written warnings from employer this month.”
Clinical Rationale for the Intervention
Explain why the specific intervention was used in this session.
Example: “Cognitive restructuring was selected to address distorted thinking patterns contributing to depressive symptoms, consistent with treatment plan goal #2.”
Progress Toward Treatment Goals
Use measurable language to show progress — or lack thereof — toward treatment goals.
Example: “Client’s PHQ-9 score decreased from 18 to 14 over the past three sessions, indicating moderate improvement in depressive symptoms.”
Justification for Continued Treatment
Explain why ongoing sessions are still needed.
Example: “Despite improvement, client continues to meet criteria for Major Depressive Disorder, Moderate, and reports ongoing sleep disturbance and social withdrawal. Continued weekly CBT is recommended to consolidate gains.”
Common Medical Necessity Documentation Mistakes
Using Vague Progress Language
“Client is improving” does not demonstrate medical necessity. Use measurable indicators instead.
Failing to Link Sessions to Diagnosis
Every session should clearly connect to the documented DSM/ICD diagnosis.
Omitting Functional Impairment
Insurance reviewers look for evidence that the condition impairs daily living — not just that the client has a diagnosis.
Copy-Pasting Across Sessions
Identical notes across visits signal to auditors that documentation may not reflect actual care.
Behavioral Health Documentation Requirements for Insurance
When it comes to billing, mental health documentation isn’t just about clinical accuracy — it’s also the proof payers require to authorize and reimburse services. Insurers look for specific elements in your notes to confirm that treatment is medically necessary, delivered as described, and compliant with regulatory standards. Failing to meet these behavioral health documentation requirements can lead to denied claims, delayed payments, or audits.
What Do Insurance Companies Look for in Clinical Notes?
Insurance companies look for clear documentation of medical necessity, treatment plan alignment, and session details that justify the services billed. To support reimbursement, every clinical note should include:
- Date and session details: Start and end time, type of service (e.g., psychotherapy, medication management), and whether the session was in person or telehealth.
- Diagnosis codes: Document DSM-5/ICD-10 diagnoses clearly, as payers require coding that matches billed services.
- Treatment plan linkage: Progress notes must connect back to goals and interventions in the treatment plan, showing the “golden thread” of care.
- Medical necessity: Include clinical observations, client reports, and your interpretation that justify why the session was needed at that time.
- Interventions provided: List techniques used (e.g., CBT, trauma-focused interventions) and client response.
- Risk assessment: Note suicidal ideation, self-harm, or safety concerns when relevant, along with interventions taken.
- Provider credentials and signature: Ensure each entry is signed (or electronically authenticated) with the correct professional designation.

Common Pitfalls That Lead to Denials
Insurance reviewers are trained to flag notes that don’t meet minimum requirements. Avoid these errors:
- Vague documentation (e.g., “Client doing better” instead of measurable change)
- Copy-pasted notes across sessions that fail to reflect actual progress
- Missing treatment plan references, making it unclear how today’s session ties into the care plan
- Omissions of session times, dates, or signatures
- Lack of justification for medical necessity, especially for longer or higher-frequency sessions
Best Practices to Stay Compliant
-
Write notes promptly — within 24–48 hours — while details are fresh.
-
Use structured templates (SOAP, DAP, or BIRP) that align with mental health documentation guidelines.
-
Review payer-specific requirements; Medicare, Medicaid, and commercial insurers may have unique criteria.
-
Audit your documentation monthly to ensure billing alignment.
-
Leverage your EHR’s built-in tools to automate time-stamps, signatures, and treatment plan linkages.
Thorough documentation doesn’t just improve care — it ensures you get paid for the services you provide. By following these beahvioral health documentation requirements, clinicians reduce claim denials, protect revenue, and stay audit-ready. For a quick reference, keep our mental health documentation cheat sheet handy to double-check that each note includes all required elements.
Psychiatric Documentation Checklist: Intake to Discharge
Use this psychiatric documentation checklist as a quick-reference tool to ensure your notes are complete, compliant, and defensible at every stage of treatment. This checklist aligns with standard mental health documentation guidelines and can be used alongside our free downloadable cheat sheet.
Intake Documentation Checklist
- ✔️ Presenting concerns and reason for referral documented
- ✔️ Personal and family psychiatric history recorded
- ✔️ Medical history and current medications noted
- ✔️ Risk factors and safety assessment completed
- ✔️ Informed consent and confidentiality agreements signed
- ✔️ Insurance information and authorization obtained
Assessment & Treatment Planning Checklist
- ✔️ Mental status exam (MSE) completed and documented
- ✔️ Standardized screening tools administered and scored
- ✔️ DSM-5/ICD-10 diagnosis documented with clinical justification
- ✔️ SMART treatment goals established
- ✔️ Planned interventions documented with rationale
- ✔️ Expected outcomes and review timeline noted
Progress Note Checklist
- ✔️ Date, start/stop time, and session type recorded
- ✔️ Client’s subjective report captured (with direct quotes when appropriate)
- ✔️ Objective observations noted (appearance, behavior, affect, speech)
- ✔️ Clinical assessment and diagnostic reasoning included
- ✔️ Specific interventions used and client’s response documented
- ✔️ Progress toward treatment plan goals addressed
- ✔️ Risk assessment updated (SI/HI/SH when applicable)
- ✔️ Plan and next steps documented
- ✔️ Provider signature and credentials included
Discharge Summary Checklist
- ✔️ Reason for discharge documented (goals met, referral, non-compliance, etc.)
- ✔️ Summary of treatment provided and client progress included
- ✔️ Remaining challenges and unresolved symptoms noted
- ✔️ Aftercare recommendations and referrals documented
- ✔️ Final diagnoses and billing codes confirmed
Tips to Improve Mental Health Documentation
Strengthening mental health documentation is about more than checking boxes — it’s about creating records that are efficient, accurate, and defensible. These practical tips can help clinicians and organizations elevate their documentation practices.
1. Educate and Train New Staff
Provide training for new team members on mental health documentation guidelines and your organization’s preferred note formats. A structured onboarding process reduces errors, promotes consistency, and ensures compliance from day one.
2. Review and Audit Documentation Regularly
Schedule periodic peer reviews or supervisor audits of notes. This not only helps catch missing elements but also reinforces best practices and provides opportunities for staff feedback and growth.
3. Use Plain, Professional Language
Write notes in clear, jargon-free language that another clinician, auditor, or payer can understand. Avoid slang or vague wording — clarity builds trust and reduces misinterpretation.
4. Capture Client Strengths and Context
Don’t just record symptoms or challenges. Document client strengths, resilience, and contextual factors (e.g., support systems, coping strategies) to give a more complete picture of their progress.
5. Leverage Technology Thoughtfully

Take advantage of your EHR’s features such as phrase banks, drop-down menus, and AI-powered tools. These can reduce documentation time while still supporting accurate and compliant notes. The right behavioral health EHR should make documentation faster without sacrificing quality.
Why These Tips Work
By focusing on staff education, quality review, clear language, and the thoughtful use of technology, clinicians can improve behavioral health documentation in ways that enhance compliance and efficiency — without adding unnecessary burden. These principles, paired with consistent training, ensure documentation supports both excellent care and reliable reimbursement.
Frequently Asked Questions About Mental Health Documentation
Related Resources
Explore more ICANotes resources on chart audits, the golden thread, clinical summaries, insurance reviews, progress notes, and utilization review.
- The Importance of Regular Chart Audits in Behavioral Health
- The Golden Thread in Mental Health Documentation
- How to Write a Clinical Summary in Mental Health
- How to Prepare for an Insurance Treatment Review
- What Every Therapist Needs to Know About Insurance and Progress Notes
- Tips for Passing a Behavioral Health Utilization Review
Simplify Mental Health Documentation with ICANotes
Strong mental health documentation is the foundation of effective, compliant, and defensible care. Yet for many clinicians, keeping up with detailed requirements, while still focusing on clients, can feel overwhelming. That’s where ICANotes makes the difference.
ICANotes is designed specifically for behavioral health professionals, with features that support every step of the documentation process. From intake to discharge, ICANotes provides structured menu-driven templates, built-in rating scales, and smart tools that help you maintain the “golden thread” and demonstrate medical necessity with ease. Our intuitive, menu-driven note builder saves time while ensuring your records meet mental health documentation guidelines and payer requirements — so you can focus less on paperwork and more on your clients.
Whether you’re a solo practitioner or part of a larger practice, ICANotes helps you streamline documentation, reduce errors, and stay audit-ready. Start your free trial today and see how ICANotes can transform the way you document, bill, and deliver care.
Follow Mental Health Documentation Best Practices with ICANotes
ICANotes helps clinicians create faster, clearer, and more defensible notes with structured workflows built specifically for behavioral health.
- Stay aligned with mental health documentation guidelines
- Support medical necessity with stronger clinical detail
- Use structured templates to save time and improve consistency
- Maintain the “golden thread” from intake through discharge
Start your 30-day free trial — no credit card required.
Get full access and see how easy compliant documentation can be.
Recent Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.