Blog > Documentation > DAP Notes: Format, Examples & Free Template
DAP Notes: How to Write Them, With Examples, Template & Best Practices
A DAP note is a clinical progress note format that organizes documentation into Data, Assessment, and Plan sections. It is widely used in mental health settings to record therapy sessions clearly, support clinical reasoning, and meet insurance and compliance requirements. This guide explains how to write DAP notes, breaks down the DAP format, and shows what to include in each section. You will find clear DAP note examples, templates, and best-practice tips to help you write concise, defensible notes more efficiently.

Last Updated: May 11, 2026


What You'll Learn
-
What belongs in the Data, Assessment, and Plan sections — including real-world DAP note examples and sample phrasing for each.
-
How to turn therapy session content into concise, defensible behavioral health progress notes that demonstrate clinical reasoning and support payer/compliance requirements.
-
A repeatable DAP note template and documentation checklist to improve consistency, reduce charting time, and streamline clinical documentation workflows.
-
How DAP notes compare to SOAP, BIRP, and DARP notes — and when clinicians may choose one format over another.
- Best practices for writing compliant, audit-ready DAP notes that support medical necessity, risk documentation, and continuity of care.
Contents
- What is a DAP Note?
- Why Clinicians Use DAP Notes
- DAP Note Workflow
- How to Write DAP Notes: Step-by-Step
- DAP Note Template
- Common DAP Note Phrases
- DAP Note Examples
- How Long Should a DAP Note Be?
- Best Practices for Writing DAP Notes
- DAP Notes vs Other Progress Note Formats
- DAP Notes for CPST Documentation
- Write Your DAP Notes Faster with ICANotes
- FAQ: DAP Notes
DAP notes are structured mental health progress notes that organize documentation into Data, Assessment, and Plan sections. Therapists, counselors, social workers, psychiatrists, and behavioral health clinicians use DAP notes to document sessions, support medical necessity, and maintain compliant clinical records. DAP notes are commonly used within a behavioral health EHR to support compliant therapy documentation, treatment planning, and continuity of care.
This guide covers everything clinicians need to write effective DAP notes: a full breakdown of the DAP format and each section, a copyable template, step-by-step guidance, and multiple real-world examples — including examples for anxiety, depression, substance use, counseling, group therapy, and social work.
What is a DAP Note?
A DAP note is a three-part clinical progress note format used primarily in mental and behavioral health settings. DAP stands for Data, Assessment, and Plan. It is designed to document therapy sessions clearly, efficiently, and in a way that supports clinical reasoning and compliance.
D — Data
Documents what occurred during the session: observable behaviors, client-reported symptoms, interventions used, and the client's response.
A — Assessment
The clinician's professional interpretation of the session data, including progress evaluation, clinical impressions, diagnosis considerations, and risk assessment.
P — Plan
Outlines next steps in treatment: planned interventions, homework assignments, referrals, treatment plan updates, and scheduling for future sessions.
DAP notes are commonly used in psychotherapy, counseling, psychiatry, and social work because they streamline documentation while producing clear, defensible records that support insurance requirements and continuity of care. DAP notes are one of the most widely used formats for writing therapy progress notes in behavioral health settings.
The infographic below explains the anatomy of a DAP note, including what clinicians should document in the Data, Assessment, and Plan sections to create clear, compliant behavioral health progress notes.

Why Clinicians Use DAP Notes
DAP notes are widely used because they balance efficient documentation with clear clinical reasoning, making them especially well-suited to mental and behavioral health settings.
Streamlined Documentation
DAP notes combine subjective client reports and objective clinical observations into a single data section. This reduces unnecessary separation, speeds up writing, and supports a more natural, narrative workflow compared to more rigid formats like SOAP notes.
Clear tracking of progress and treatment direction
By separating session data, clinical interpretation, and planning, DAP notes make it easier to document symptom changes, evaluate progress toward treatment goals, and maintain continuity of care across sessions or providers.
This clarity also supports effective practice management by keeping records organized, consistent, and easy to review.
Built-in support for risk assessment
The assessment section provides a clear place to evaluate risk, document safety concerns, and explain clinical decision-making, particularly important when addressing suicidality, self-harm, or changes in client stability.
Flexible structure for routine care
DAP notes are less prescriptive than some other formats, allowing clinicians to adapt documentation to different session types without sacrificing clarity or consistency.
Strong fit for insurance and compliance requirements
When written well, DAP notes clearly link session data to clinical assessment and treatment planning, helping justify medical necessity during audits, reimbursement reviews, and compliance checks. Detailed behavioral health documentation can also support cleaner claims submission and fewer payer disputes related to behavioral health billing.
DAP Note Workflow
Session
Start with the clinical encounter, including the client’s presentation, concerns, symptoms, and session focus.
Data
Document what happened: observable behaviors, client-reported symptoms, interventions used, and client response.
Assessment
Apply clinical judgment to interpret progress, symptoms, risk, functioning, and medical necessity.
Plan
Outline next steps, including interventions, homework, referrals, treatment plan updates, and follow-up.
How to Write DAP Notes: Step-by-Step
DAP notes use only three sections, which makes them efficient but also means each section needs to be used intentionally. Knowing what belongs in each part of the note helps you document sessions clearly, support clinical reasoning, and meet insurance and compliance expectations without overwriting.
What information goes in the Data section of DAP notes?
The Data section documents what occurred during the session. It should capture observable facts and client-reported information without interpretation, setting the foundation for the assessment and plan.
This section may include:
- Client-reported symptoms, concerns, stressors, or significant events since the last session
- Observable details such as appearance, behavior, mood, affect, thought process, and engagement
- Therapeutic interventions used during the session and the client’s response to those interventions
- Results of screenings, rating scales, or other measurable observations
- Relevant direct quotes that reflect the client’s experience.
- Review of any homework assigned at the previous session.
Clear, specific data helps demonstrate that the session was clinically distinct and necessary, which is especially important for insurance review and audit readiness.
Example: Client arrived on time and appeared visibly tense, with restless movements and constricted affect noted throughout the session. Client reported increased work-related stress over the past week, stating, “I feel constantly on edge and can’t shut my brain off after work.” Client described difficulty sleeping, increased irritability, and persistent worry related to workplace conflict and workload demands. Session focused on identifying anxiety triggers and practicing grounding and diaphragmatic breathing techniques. Client actively participated in interventions and demonstrated improved ability to regulate breathing and reduce visible tension by the end of the session.
How do you document the Assessment portion of a DAP note?
The Assessment section explains what the session data means clinically. This is where you apply professional judgment to evaluate progress, risk, and diagnostic relevance.
This section may include:
- Progress toward treatment goals, including improvement, stability, or regression
- Changes in symptom severity, functioning, or presentation
- Clinical impressions and diagnostic considerations supported by session data
- Risk and safety evaluation, including suicidality, self-harm, and homicidal ideation explicitly
- The client's response to the treatment plan overall
A well-written assessment connects session observations to clinical conclusions and clearly supports medical necessity and ongoing treatment decisions.
Example: Client continues to experience moderate anxiety symptoms related to occupational stressors, including excessive worry, sleep disturbance, and difficulty disengaging from work-related thoughts. Clinical presentation remains consistent with generalized anxiety, though client demonstrates emerging insight into anxiety triggers and increased willingness to use coping strategies outside of sessions. Client showed mild improvement in emotional regulation and reported partial success using grounding techniques during stressful situations this week. Anxiety symptoms continue to impact daily functioning and support the ongoing medical necessity for treatment. No suicidal ideation, self-harm behaviors, or homicidal ideation reported. Current risk level assessed as low.
What should be included in the Plan section of DAP Notes?
The Plan section outlines how treatment will continue after the session. It should be forward-looking, specific, and focused on actionable next steps.
This section may include:
- Planned interventions or therapeutic focus for upcoming sessions
- Homework assignments, skills practice, or behavioral tasks agreed upon with the client
- Referrals, consultations, or coordination with other providers
- Updates to the treatment plan based on current progress or risk
- Timing, format, and frequency of future sessions.
The Plan section should align closely with the client’s behavioral health treatment plan and include actionable next steps. Clear plans help maintain continuity of care and show purposeful treatment progression from one session to the next.
Example: Client will continue practicing grounding and diaphragmatic breathing exercises daily, particularly during periods of elevated work-related stress. Client was encouraged to track anxiety triggers and document automatic negative thoughts between sessions using a thought-record worksheet. Next session will focus on cognitive restructuring techniques to address maladaptive thought patterns contributing to anxiety symptoms. Continue weekly psychotherapy sessions to support anxiety management, emotional regulation, and improved occupational functioning. Follow-up session scheduled for one week from today.
DAP Note Template
Use the template below as a starting point for any session. Replace the bracketed prompts with specific clinical content from your session. A version of this template — with a full example, risk documentation reminders, and a quality checklist — is available as a free downloadable cheat sheet.
DAP Note Template
Use this structured template to document behavioral health sessions clearly and consistently.
Many clinicians use mental health charting software to streamline DAP documentation, improve consistency, and reduce time spent charting after sessions.
Common DAP Note Phrases for Clinicians
The following sample phrases can help behavioral health clinicians write clearer, more consistent therapy progress notes while supporting medical necessity and clinical documentation requirements.
Data Phrases
- Client reported increased anxiety related to work stress.
- Client appeared tearful and fatigued throughout session.
- PHQ-9 score increased from 12 to 16 since prior visit.
- Session focused on CBT-based cognitive restructuring.
- Client engaged actively in grounding exercise.
Assessment Phrases
- Client demonstrates improved insight into cognitive distortions.
- Symptoms continue to impair occupational functioning.
- Risk currently assessed as low.
- Progress toward treatment goals remains gradual but consistent.
- Clinical presentation remains consistent with generalized anxiety disorder.
Plan Phrases
- Continue weekly psychotherapy sessions.
- Client will complete daily thought journal before next visit.
- Introduce behavioral activation strategies next session.
- Referral placed for psychiatric medication evaluation.
- Next session scheduled for [date/time].

DAP Note Examples
The following examples show how the DAP format works across a range of clinical scenarios. Each demonstrates how to document session data, apply clinical interpretation, and outline clear next steps.
DAP Note Example for Anxiety
Client arrived on time, appeared tense, and was well-groomed. GAD-7 score was 12, down from 15 at the prior session. Client reported feeling overwhelmed by work demands and described difficulty managing a new project deadline. Session focused on identifying occupational stressors and practicing grounding techniques. Client engaged actively in discussion about potential workplace accommodations. Client stated: 'I know it's irrational, but I can't stop thinking something will go wrong.'
Client's presentation is consistent with ongoing generalized anxiety related to occupational stressors, with mild symptom improvement noted on the GAD-7. Client demonstrates growing awareness of cognitive patterns maintaining anxiety and showed appropriate use of grounding techniques. Engagement was collaborative. No safety concerns identified; suicidal ideation denied.
Client will practice grounding techniques during periods of work-related stress, at least once daily. Client will consider discussing workload concerns with supervisor before the next session. Continue CBT-informed work in next session, focusing on cognitive restructuring. Next session scheduled for June 12 at 2:00 p.m.
Learn more about documenting anxiety symptoms, interventions, and treatment strategies in our guide to interventions for anxiety.
DAP Note Example for Substance Use
Client appeared less groomed than baseline presentation. Client reported recent bereavement following the death of a close family member and disclosed alcohol binge use after the loss. Client expressed guilt related to breaking sobriety and stated: 'I know I shouldn't have, but I didn't know what else to do.' Session focused on grief processing and identifying alternative coping strategies. Client participated in discussion about support systems, including peer support and family engagement.
Client is experiencing acute grief and increased emotional distress, contributing to elevated relapse risk. Client expresses anxiety regarding ability to maintain sobriety and demonstrates difficulty prioritizing coping strategies under high-stress conditions. Insight into relapse triggers is present, though consistent coping skill use remains a treatment target. No immediate safety concerns; suicidal ideation and intent denied.
Client will attend weekly grief support group beginning next Tuesday at 6:00 p.m. Client will complete at least two identified coping activities per week and track them in a journal. Follow-up session scheduled for [date] at [time], focused on grief processing and relapse prevention. Discuss increasing session frequency if relapse risk remains elevated.
DAP Note Example for Depression
Client arrived on time, appeared fatigued, wore loose clothing consistent with prior sessions. Client reported sleeping approximately 10-11 hours per night but feeling 'exhausted all the time.' PHQ-9 score was 16, up from 13 at the last session two weeks ago. Client disclosed ongoing social withdrawal, having declined invitations from close friends twice in the past week. Session focused on behavioral activation principles. Client identified one low-effort activity willing to attempt before the next session. Engagement was minimal but responsive to structured, direct questions.
Client presents with moderate-to-severe depressive symptoms that have worsened since the previous session, evidenced by an elevated PHQ-9 score, hypersomnia, social withdrawal, and reduced motivation. Client demonstrates limited insight into behavioral patterns contributing to isolation but was willing to engage with the behavioral activation framework. Suicidal ideation explicitly assessed; client denied ideation, intent, and plan. Risk assessed as low based on no active ideation and intact social support network.
Client will attempt one brief social or physical activity (client chose a 10-minute walk near home) before the next session and track mood before and after. Continue behavioral activation work in next session; introduce thought monitoring if client demonstrates readiness. Administer PHQ-9 at next session. Consider consulting with prescribing provider if PHQ-9 score remains elevated or worsens. Next session scheduled for May 18 at 3:00 pm.
Accurate documentation of mood symptoms and functioning is especially important when treating depression. See additional guidance on depression intervention.
DAP Note Example for Counseling
Client arrived 5 minutes late, appeared well-groomed and engaged. Client reported increased conflict with a family member over the past week and described feeling 'dismissed and unheard.' Session focused on identifying communication patterns using an emotionally focused therapy framework. Clinician introduced the demand-withdraw cycle and explored the client's role in the dynamic. Client participated actively and practiced a brief assertive communication exchange during session.
Client demonstrates growing insight into relational patterns and their origins. Willingness to explore both their own behavior and the interpersonal dynamic indicates good treatment engagement and readiness for skill application. Emotional regulation appeared stable throughout the session. No safety concerns identified. Progress is consistent with treatment goals focused on improving communication and reducing relational conflict.
Client will practice one assertive communication exchange with the family member before the next session and journal the outcome. Continue EFT-informed work in upcoming sessions. Introduce conflict de-escalation strategies if current communication practice is successful. Next session scheduled for April 17 at 11:00 am.
DAP Note Example for Group Therapy
Client attended a 75-minute CBT-focused anxiety management group with six participants present. Group topic focused on identifying cognitive distortions and practicing cognitive reframing techniques. Client appeared attentive and engaged throughout the session, maintained appropriate eye contact, and participated voluntarily in group discussion. Client shared difficulty managing anticipatory anxiety before work meetings and stated: “I always assume I’m going to embarrass myself.” Client completed an in-session cognitive restructuring exercise and was receptive to peer feedback. No behavioral concerns observed.
Client demonstrates growing insight into anxiety-related cognitive distortions and is increasingly willing to engage in group processing. Participation level and responsiveness to feedback indicate improved treatment engagement compared to prior sessions. Anxiety symptoms continue to impair occupational functioning and social confidence, supporting ongoing treatment necessity. No suicidal ideation, self-harm urges, or homicidal ideation reported. Current risk assessed as low.
Client will complete a thought-record worksheet before the next group session and practice identifying automatic negative thoughts in workplace situations. Continue CBT-focused group therapy targeting anxiety management and cognitive restructuring. Next group session scheduled for July 15 at 3:00 pm.
Clinicians facilitating groups may also benefit from reviewing best practices for group therapy documentation and participant-specific progress notes.
DAP Note Example for Social Work
Client met via telehealth for a 50-minute session. Client is a single parent of two children (ages 4 and 7) currently receiving case management services. Client's primary presenting concern was an eviction notice received three days ago. Client appeared anxious and tearful and stated: 'I don't know what we're going to do if we lose the apartment.' Clinician and client reviewed available emergency housing assistance resources. Client expressed openness to contacting the housing authority but identified transportation and phone access as barriers. Safety check completed; client denied suicidal ideation.
Client is experiencing an acute situational crisis related to housing instability, with elevated anxiety and significant psychosocial stressors. Coping capacity is currently strained. Client demonstrates adequate problem-solving ability when supported but is limited by access barriers. Protective factors include strong parental motivation and an established case management relationship. No immediate safety concerns; risk currently assessed as low.
Clinician will coordinate with case manager to expedite housing assistance referral before end of week. Client will contact the county housing authority by [date]; clinician will follow up by phone within 48 hours. Next session scheduled for [date] at [time], focused on crisis stabilization and resource navigation. If housing situation deteriorates, consider increasing session frequency.
How Long Should a DAP Note Be?
There is no fixed length requirement for a DAP note, but most are brief and focused. In practice, a DAP note is typically one to three short paragraphs, or roughly 100 to 300 words, covering the Data, Assessment, and Plan sections.
For routine therapy sessions, DAP notes can often be completed in 5 to 10 minutes while still capturing all clinically relevant information. The goal is to capture what matters most, not to record every detail of the session.
More complex situations may require longer documentation. Notes may be expanded when:
- Symptoms change significantly or a new diagnosis is being considered
- Risk or safety concerns are present and require detailed documentation
- Treatment plans are updated based on session content
- A crisis intervention occurs during or following the session
In these cases, additional detail helps support clinical decision-making and medical necessity.
Best Practices for Writing DAP Notes
Writing effective DAP notes takes more than following the right structure. These best practices can help you document sessions clearly and avoid common charting problems.
1. Be objective and clinically focused
Effective DAP notes rely on observable facts and client-reported information rather than personal opinions or assumptions. Keep interpretation in the Assessment section and ensure clinical conclusions are supported by what was documented in the Data section. This separation improves clarity and makes notes easier to defend during reviews or audits.
2. Document medical necessity explicitly
Every DAP note should clearly connect the client's presenting symptoms, the interventions provided, and the treatment goals. Insurers and auditors look for documentation that demonstrates why ongoing treatment is clinically necessary. Vague notes ('Client discussed feelings about work') do not meet this standard. Specific notes ('Client reported increased anxiety with GAD-7 of 14; CBT-based cognitive restructuring introduced to address catastrophizing') do.
3. Be concise without under-documenting
DAP notes should be thorough but not excessive. Other clinicians, insurers, or auditors may review your notes, so they need enough detail to explain clinical decisions without becoming overly long.
4. Use client quotes intentionally
Direct quotes can be valuable when they clarify symptoms, emotional responses, or treatment readiness. Use them selectively to support clinical understanding rather than documenting conversation verbatim.
5. Document interventions and client responses
Clearly noting which techniques were used during the session and how the client responded demonstrates active treatment. This supports continuity of care and helps justify ongoing services, particularly for insurance and compliance purposes.
6. Address risk in every note
The Assessment section should always include a risk evaluation, even when risk is low. Documenting that suicidal ideation, self-harm, and homicidal ideation were assessed and denied — with current risk rated as low — is far more defensible than omitting risk documentation entirely.
7. Write professionally and defensibly
DAP notes may be used in medical decisions, audits, legal proceedings, or client-requested records. Use professional language, avoid personal judgments, and rely on industry-recognized terminology. The American Psychological Association emphasizes clear, accurate, and timely clinical documentation as a core ethical responsibility for mental health providers.
8. Complete notes promptly
Writing notes as soon as possible after the session improves accuracy and reduces the risk of missing important details. Timely documentation is especially important in busy practices or when managing complex or high-risk cases.
9. Store notes securely in compliance with HIPAA
DAP notes and other progress notes are protected health information under HIPAA and must be stored and accessed in ways that protect patient privacy. Using a secure, HIPAA-compliant EHR system safeguards sensitive information while supporting audit readiness and continuity of care.
DAP Notes vs Other Progress Note Formats
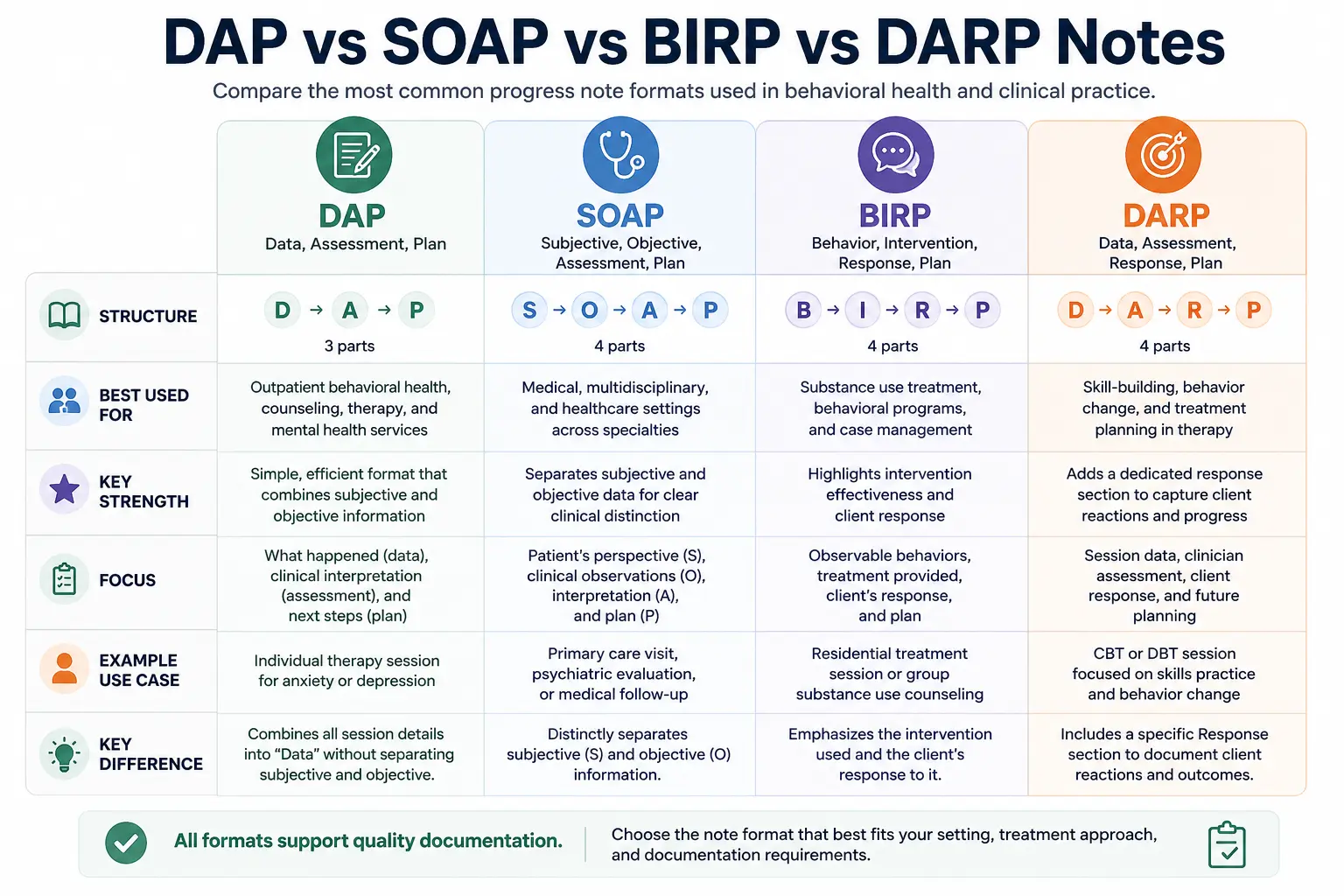
DAP vs. SOAP vs. BIRP vs. DARP Notes
| Format | Stands For | Best Used For | Key Difference |
|---|---|---|---|
| DAP | Data, Assessment, Plan | Behavioral health and psychotherapy documentation | Combines subjective and objective data into one section |
| SOAP | Subjective, Objective, Assessment, Plan | Medical and multidisciplinary settings | Separates subjective and objective observations |
| BIRP | Behavior, Intervention, Response, Plan | Substance use and behavioral treatment programs | Tracks intervention effectiveness and client response closely |
| DARP | Data, Assessment, Response, Plan | Skill-building and behavior-change focused treatment | Adds a dedicated Response section to document client reactions |
DAP Notes vs SOAP Notes
DAP notes and SOAP notes are closely related but differ in how session information is organized. In a SOAP note (Subjective, Objective, Assessment, Plan), client-reported information and clinician observations are documented separately. The Subjective section reflects the client's perspective; the Objective section captures measurable clinical data. Clinicians comparing DAP documentation with SOAP notes often find that DAP notes provide a more streamlined and narrative-friendly structure.
In a DAP note, both types of information are combined into a single Data section. This creates a more streamlined, narrative-style approach before moving into clinical interpretation and planning. SOAP notes are often preferred in medical, nursing, and multidisciplinary settings where structured separation of subjective and objective data is required.
DAP Notes vs BIRP Notes
In a DAP note, session observations and client reports are combined in the Data section, with interpretation in the Assessment and next steps in the Plan. In a BIRP note (Behavior, Intervention, Response, Plan), the session is broken down more explicitly: client behavior is documented first, followed by the clinician's intervention and the client's immediate response.
BIRP notes are useful when close tracking of specific behaviors and interventions is required — commonly used in substance use treatment, behavioral health programs, and crisis-focused sessions where documenting treatment effectiveness is critical.
DAP Notes vs DARP Notes
DAP and DARP notes are closely related, with one key addition. In a DARP note (Data, Assessment, Response, Plan), a separate Response section documents how the client reacted to specific interventions or clinical discussions — content that in a standard DAP note is typically incorporated into the Data or Assessment sections.
DARP notes are helpful when client reactions to interventions are clinically significant and need to be tracked closely, such as in acute care, skill-based treatment, or sessions focused on behavior change and engagement.
Client arrived on time, appeared slightly disheveled compared to baseline. Client reported feeling on edge and disclosed a relapse to alcohol use two nights ago following a confrontation with a coworker. BAC upon arrival was 0.00. Client reported feelings of guilt and shame related to the relapse.
Client is experiencing elevated relapse risk related to occupational stressors and limited distress tolerance skills. Shame response is present and may increase social isolation risk. Consistent coping skill use during high-stress situations remains a treatment target. Suicidal ideation denied; safety contract reviewed and upheld.
Client engaged openly with relapse discussion and appeared willing to analyze the trigger chain without defensiveness. Demonstrated insight into the coworker confrontation as a precipitating relapse event. Responded positively to motivational interviewing; affirmed commitment to sobriety goals. Affect improved noticeably by end of session.
Client will complete a written relapse trigger analysis before the next session. Continue motivational interviewing and distress tolerance skill-building. Increase session frequency to twice weekly for the next two weeks. Referral to peer support group discussed; client will consider attending one meeting before the next session. Next session scheduled for [date] at [time].
DAP Notes for CPST Documentation
Community Support Professional and Specialist (CPST) workers in community mental health settings also commonly use the DAP format for service documentation. When applying the DAP structure to CPST notes, the content of each section reflects the nature of the service contact rather than a therapy session.
The Data section typically documents the specific community support activity — such as transportation assistance, housing navigation, benefits enrollment, or skill-building — along with the client's presentation, engagement, and notable events during the service contact. The Assessment section reflects the clinician's evaluation of the client's functioning and progress toward individualized service goals, including barriers and the client's current capacity for independent skill use. The Plan section outlines the next CPST service contact, specific skill-building targets, referrals, and coordination with other treatment team members.
Note: CPST documentation requirements vary by state and payer. Always confirm local Medicaid and billing standards with your agency's compliance team before finalizing your DAP note format for CPST services.
Write your DAP Notes Faster with ICANotes
Progress notes are essential, but they shouldn't consume your clinical day. ICANotes is built specifically for behavioral health clinicians and helps you create structured, compliant DAP notes quickly using guided, menu-driven documentation — without staring at a blank text box after every session.
With ICANotes, you can:
- Maintain a consistent DAP format across every session
- Reduce documentation time without sacrificing clinical detail
- Generate audit-ready records that align with payer and compliance expectations
- Store notes securely in a fully HIPAA-compliant system.
- Support automatic CPT coding alongside your documentation
By streamlining how DAP notes are created and stored, ICANotes helps you spend less time charting and more time focused on client care. Start your 30-day free trial to see the difference.
Frequently Asked Questions: DAP Notes
Recent Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) from Aspen University and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.






