Blog > Documentation > Mental Health SOAP Notes: Examples, Tips & Templates
Mental Health SOAP Notes: Examples, Templates, and How to Write Them
Mental health SOAP notes are a structured documentation method used by therapists, psychiatrists, counselors, and other behavioral health clinicians to record client sessions. The SOAP format organizes documentation into four sections: Subjective, Objective, Assessment, and Plan, making it easier to track symptoms, document clinical observations, evaluate progress, and outline treatment next steps. This guide explains how to write effective mental health SOAP notes with practical tips, a copyable template, and detailed examples for therapy, psychiatry, and group counseling sessions.

Last Updated: March 13, 2026


What You'll Learn
- What mental health SOAP notes are and why they matter for compliance and billing
- How to write each section (S, O, A, P) with behavioral health-specific guidance
- A copyable SOAP note template you can use right away
- Real SOAP note examples for individual therapy, psychiatry, and group sessions
- How SOAP compares to DAP and BIRP note formats
- The most common SOAP note documentation mistakes — and how to avoid them
Mental health SOAP notes are one of the most important tools in a behavioral health clinician's documentation practice. Done well, they communicate clinical reasoning clearly, support continuity of care, satisfy payer requirements, and protect you during audits. Done poorly, they can jeopardize reimbursement and expose your practice to risk.
This guide breaks down everything you need to write better mental health SOAP notes — whether you're just starting out or looking to sharpen documentation you've been writing for years.
What Are Mental Health SOAP Notes?
Mental health SOAP notes are a structured clinical documentation format used by therapists, psychiatrists, counselors, and other behavioral health clinicians to record client sessions.
The SOAP framework organizes notes into four sections: Subjective (client-reported symptoms), Objective (clinician observations), Assessment (clinical impressions and diagnosis), and Plan (treatment steps and next actions).
This structured format helps clinicians document medical necessity, track treatment progress, and maintain compliant behavioral health records.
Mental Health SOAP Notes at a Glance
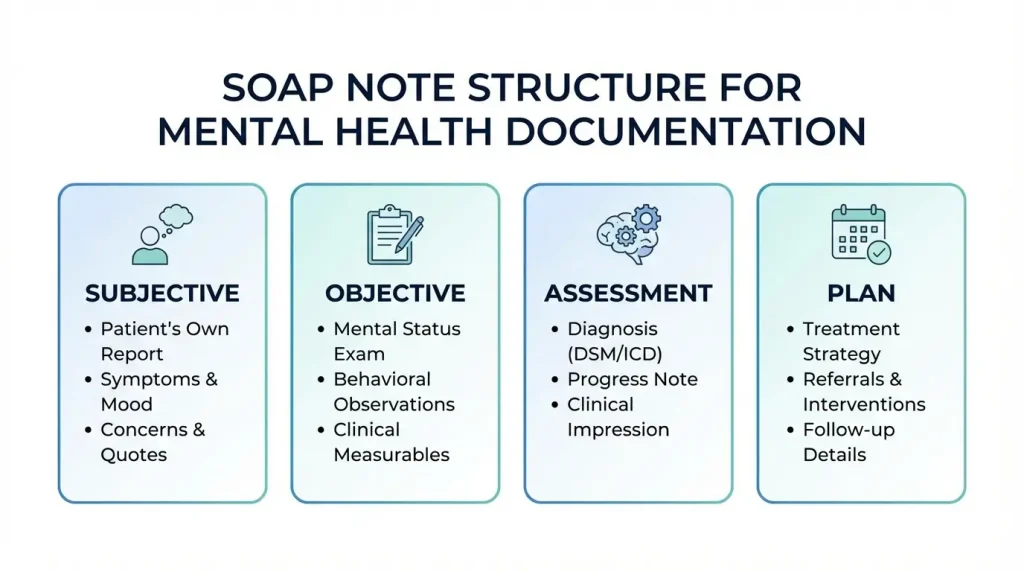
Mental health SOAP notes use a four-part structure that helps behavioral health clinicians document client sessions clearly, demonstrate medical necessity, and track treatment progress.
Client-reported symptoms, mood, stressors, and experiences described in their own words.
Clinician observations, mental status exam findings, and measurable assessment results.
Diagnostic impressions, interpretation of symptoms, and evaluation of treatment progress.
Treatment interventions, next steps, referrals, homework, and follow-up scheduling.
Using this structured framework helps clinicians maintain organized behavioral health documentation while clearly demonstrating clinical reasoning and medical necessity.
What are Mental Health SOAP Notes?
Mental health SOAP notes are a structured documentation framework used by behavioral health clinicians to record client sessions. The acronym stands for Subjective, Objective, Assessment, and Plan — the four sections that make up every complete note.
The format was originally developed in the 1960s as part of the problem-oriented medical record (POMR) system pioneered by physician Lawrence Weed. What began as a medical documentation tool has since become the most widely used note format across all healthcare disciplines — including psychiatry, psychotherapy, counseling, social work, and substance use treatment.
The enduring appeal of SOAP notes is their clarity. Every clinician who reads a SOAP note knows exactly where to find the client's reported experience, the clinician's observations, the working diagnosis, and the treatment direction — even if they've never met the client before.
Mental Health SOAP Note Template
Before diving into each section in depth, here's a template you can use or adapt for your own practice. The fields below reflect mental health-specific documentation needs rather than a generic medical template.
Mental Health SOAP Note Template
Use this behavioral health SOAP note template as a quick reference when documenting therapy, psychiatry, or counseling sessions.
Client's reported symptoms, mood, stressors, and experiences in their own words. Include relevant quotes, changes since last session, medication adherence, sleep and appetite patterns, and safety concerns.
Clinician observations including appearance, behavior, speech, affect, thought process, cognition, orientation, and mental status exam findings. Include relevant assessment scores (e.g., PHQ-9, GAD-7, Columbia) when applicable.
Clinical impression and diagnostic considerations. Document progress toward treatment goals, symptom severity, functional impact, response to interventions, and risk level. Synthesize S and O findings into your professional judgment.
Treatment administered today and rationale. Client's response. Homework or between-session tasks. Next appointment date. Referrals, medication changes, or coordination of care. Specific goal for each active diagnosis.
Download our Mental Health
SOAP Notes Guide
Enhance your clinical documentation skills with a comprehensive guide to writing clear, effective, and compliant SOAP notes for therapy, psychiatry, and group sessions.
How to Write Mental Health SOAP Notes: Step by Step
Each section of a mental health SOAP note has a distinct purpose. Understanding what belongs in each — and what doesn't — is the foundation of efficient, accurate documentation.
Subjective — The Client’s Experience
This section captures what the client tells you: their symptoms, concerns, mood, and perspective on their own condition. It should reflect the client’s voice, not your interpretation.
- Presenting concerns and reason for today’s visit
- Client-reported symptoms, severity, and changes since last session
- Mood in the client’s own words, including direct quotes when clinically meaningful
- Sleep, appetite, energy levels, and daily functioning
- Medication adherence and reported side effects
- Substance use since the last session
- Significant life events, stressors, or relationship changes
- Any statements suggesting suicidal ideation, self-harm, or other safety concerns
Use OLD CHARTS to Systematically Cover Symptoms
Tip: If a client says something clinically significant, quote it directly. For example, “I feel like I’m watching my life from the outside” communicates a dissociative experience more clearly than "client reported feeling detached."
Objective — Your Clinical Observations
This section contains only what you can directly observe or measure during the session — not interpretations, not client self-report. In behavioral health documentation, objective findings typically come from the clinician’s observations and mental status examination.
- Appearance: grooming, hygiene, dress, eye contact
- Behavior: psychomotor activity, cooperation, engagement level
- Speech: rate, tone, volume, clarity, fluency
- Mood and affect: observed emotional presentation (flat, labile, congruent, expansive)
- Thought process: logical, tangential, circumstantial, disorganized
- Thought content: delusions, obsessions, SI/HI
- Cognition and orientation: alertness and orientation to person/place/time/situation
- Assessment scores: PHQ-9, GAD-7, Columbia Suicide Scale, etc.
Remember: Symptoms belong in the Subjective section because they are reported by the client. Signs belong in the Objective section because they are observed by the clinician. If a client reports panic attacks, that goes in S. If you observe visible trembling and accelerated breathing, that goes in O.
Assessment — Your Clinical Impression
The Assessment section synthesizes the information gathered in the Subjective and Objective sections. It reflects the clinician’s professional judgment about diagnosis, treatment progress, and current clinical status. For initial visits, this may include a working or confirmed diagnosis. For follow-up visits, it documents progress toward treatment goals.
- DSM-5 diagnosis or working diagnosis
- Progress toward treatment goals (improving, stable, declining, or remission)
- Functional status and impact on daily living
- Response to current treatment modality
- Risk level assessment (low, moderate, high)
- Changes in the clinical picture since the last session
Billing Tip: The Assessment section is where medical necessity lives. Payers want to see that symptoms cause functional impairment and that continued treatment is clinically indicated. Vague statements like "client is stable" are common audit flags. Be specific.
Plan — The Roadmap Forward
The Plan translates your Assessment into action. Every diagnosis or problem identified in the Assessment should have a corresponding plan item. This section creates continuity between sessions and documents clinical decision-making.
- Therapeutic interventions used in the session and your clinical rationale
- Client’s response to those interventions
- Homework or between-session tasks
- Next appointment date and session frequency
- Medication changes or recommendations (if applicable)
- Referrals to other providers or services
- Goals and measurable outcomes for active diagnoses
- Safety plan status (if risk was identified)
Tip: If your client has multiple diagnoses — for example, PTSD and a co-occurring substance use disorder — include a separate plan item for each. This demonstrates individualized, diagnosis-specific treatment.
Mental Health SOAP Note Examples for Therapy, Psychiatry & Groups
The following examples illustrate how SOAP notes look in real clinical scenarios. These reflect realistic documentation practice — detailed enough to be useful, concise enough for efficient charting.
Example 1: Individual Therapy — Anxiety & Depression
Example 2: Psychiatry Medication Management — Alzheimer's & Depression
Example 3: Group Therapy — Substance Use Recovery
Group therapy notes follow the same SOAP structure, but each group member should have their own individualized note. The note below is for a single client within a group session.
SOAP vs. DAP vs. BIRP Notes: How to Choose
SOAP is the most common format in behavioral health, but it's not the only option. Understanding how it compares to DAP and BIRP notes can help you choose the right framework for your setting and workflow.
| Format | Structure | Best For | Trade-Off |
|---|---|---|---|
| SOAP | Subjective, Objective, Assessment, Plan | All behavioral health settings; insurance-heavy practices; integrated care teams | More sections to complete; can feel repetitive for experienced clinicians |
| DAP | Data, Assessment, Plan | Private practice; settings with lower audit risk; experienced therapists | Combines Subjective and Objective into one Data section, which can blur the distinction between client report and clinical observation |
| BIRP | Behavior, Intervention, Response, Plan | Settings where documenting specific interventions is the priority, such as CBT, DBT, and structured behavioral health programs | Less emphasis on client self-report and diagnosis; may not satisfy all payer requirements |
When in doubt, SOAP is the safest choice. Its explicit separation of Subjective and Objective content is particularly valued during insurance audits and third-party reviews.
Related: Therapist Notes: Complete Guide to Documentation Types & Best Practices
SOAP Notes, Billing & Medical Necessity: What Payers Look For
Mental health SOAP notes are not just a clinical tool — they are a billing document. Every section of your note should be written with the understanding that a payer or auditor may review it to determine whether the service was medically necessary and appropriately coded.
What "Medical Necessity" Means in Practice
To establish medical necessity, your documentation should show that:
- The client has a diagnosable condition (Assessment)
- That condition causes functional impairment (Subjective + Objective)
- The treatment provided is appropriate for the diagnosis (Plan)
- Continued treatment is required — the client has not yet reached maximum benefit (Assessment)
| SOAP Section | Documentation Focus | What Payers Look For | Why It Matters |
|---|---|---|---|
| Subjective | Client-reported symptoms, concerns, and functional challenges | Evidence that symptoms are active, ongoing, and functionally impairing. Vague entries like "client is doing well" without symptom specifics are audit red flags. | Supports medical necessity for treatment services |
| Objective | Clinician observations and measurable findings | Clinical observations that corroborate or contextualize the client's report. MSE findings and assessment scores strengthen the record. | Demonstrates clinical evaluation and diagnostic reasoning |
| Assessment | Clinical interpretation and diagnosis | A specific DSM-5 diagnosis, an evaluation of the client's current clinical status, and a clear statement of why continued treatment is needed. | Shows why continued treatment is appropriate |
| Plan | Treatment interventions and next steps | Specific, measurable interventions tied to the diagnosis — not just "continue therapy." Each active diagnosis should have a corresponding plan item. | Connects documentation to reimbursement and treatment outcomes |
When SOAP notes clearly document symptoms, clinical observations, diagnostic impressions, and treatment decisions, they provide the documentation trail payers expect during utilization review or claim audits.
Payers often audit behavioral health documentation when clinical notes fail to clearly demonstrate medical necessity. Common triggers include vague descriptions of symptoms, treatment plans that do not connect to the client’s diagnosis, missing documentation of clinical interventions, and notes that appear identical from session to session. Using a structured format like SOAP helps clinicians consistently document symptoms, observations, clinical reasoning, and treatment decisions in a way that aligns with payer expectations.
7 Common SOAP Note Mistakes — and How to Fix Them
These documentation errors frequently appear during utilization reviews and insurance audits. The examples below show how small changes can dramatically improve clarity and compliance.
Client statements belong in the Subjective section, while clinician observations belong in Objective. Mixing them creates confusion and can complicate billing.
Documentation should describe symptoms and severity clearly. Entries like "client is doing well" or "session went as planned" provide no clinical information and invite auditor scrutiny.
The assessment should explain why continued treatment is clinically justified — not just describe the current state..
Duplicating prior notes without updating them can make sessions look interchangeable — a major red flag in audits and utilization reviews. Each note should reflect what actually happened in that specific session.
Treatment notes should clearly show what the clinician did in session.
Progress notes should connect to the treatment plan objectives.
If a client expresses hopelessness, discusses self-harm, or is in a high-risk category, the absence of a documented risk assessment creates both a clinical and legal liability.
Notes should be comprehensive, not exhaustive. Anecdotes and tangents that don't serve a clinical purpose dilute the utility of your documentation and add charting time with no benefit.
Many of these documentation mistakes happen because clinicians are working with blank notes or generic EHR templates.
How ICANotes Helps Prevent SOAP Note Documentation Errors
Many documentation mistakes happen when clinicians are working from blank note templates or trying to write detailed session notes under time pressure. Without structured guidance, it becomes easy to miss key clinical details, mix subjective and objective observations, or forget to document interventions and treatment progress.
ICANotes was designed specifically for behavioral health documentation. Instead of starting with an empty note, clinicians select clinically relevant phrases and findings from structured menus, allowing them to quickly generate clear, compliant SOAP notes while maintaining individualized documentation.
- Guided documentation that separates Subjective and Objective information
- Built-in clinical terminology that supports medical necessity
- Structured note sections aligned with SOAP documentation standards
- Tools that help clinicians document interventions and treatment progress clearly
By combining structured templates with flexible narrative generation, ICANotes helps clinicians complete accurate SOAP notes faster while reducing documentation risks during audits or utilization reviews.
Write Faster, More Defensible SOAP Notes
ICANotes helps behavioral health clinicians document sessions quickly using structured templates designed for therapy, psychiatry, and counseling workflows. Our menu-driven documentation system helps reduce vague notes, ensure medical necessity language, and improve compliance.
- Structured SOAP note templates
- Built-in clinical terminology
- Documentation that supports medical necessity
- Integrated behavioral health workflows
Try ICANotes free for 30 days, no credit card required.
Why Mental Health SOAP Notes Matter for Compliance and Billing
Mental health SOAP notes serve three critical functions beyond simply recording what happened in a session.
1. Connectivity Across Providers
With electronic health record (EHR) adoption now widespread across both medical and behavioral health settings, integrated care means multiple providers may access your notes. SOAP format is universally understood — a primary care physician, a prescribing nurse practitioner, and a peer specialist can all extract relevant information from a well-written SOAP note without needing a translation.
2. Accuracy and Continuity
The structured format of SOAP notes reduces the cognitive load of documentation. Rather than free-writing a summary after each session, the four-section framework prompts you to gather specific information at specific times — which results in more complete, accurate records. It also means another clinician can step in and provide continuity of care based on your notes alone.
3. Legal and Regulatory Protection
Mental health SOAP notes create an auditable record of clinical decision-making. In the event of a malpractice claim, an insurance audit, or a licensing board inquiry, your notes are your primary defense. A note that clearly documents your assessment and rationale is far more defensible than one that doesn't.
Frequently Asked Questions About Mental Health SOAP Notes
How do I write the Subjective section of a mental health SOAP note?
The Subjective section captures the client's own report of symptoms, experiences, and concerns. Include presenting concerns, client-reported symptoms and their severity, mood descriptions in the client's own words, sleep and appetite changes, medication adherence, substance use since the last session, significant life stressors, and any statements of risk such as suicidal ideation or self-harm urges.
Use direct quotes when they capture mood or thought patterns precisely. Save clinical interpretations for the Assessment section. For example, “client reports feeling numb all the time” belongs in Subjective, while “flat affect observed throughout session” belongs in Objective.
How detailed should the Objective section be in mental health SOAP notes?
Detail should be proportional to clinical relevance. A session where the client presents as well-groomed, euthymic, and engaged may warrant a brief Objective entry, while a session with notable changes in appearance, affect, or cognition warrants more detail.
At minimum, document appearance, behavior, speech, observed mood and affect, thought process, orientation, and any assessment scores administered. Avoid copying the same Objective section verbatim from session to session, since even subtle changes should be captured.
What are the most common SOAP note mistakes in mental health settings?
Common SOAP note mistakes include blending Subjective and Objective content, using vague language without clinical specifics, failing to demonstrate medical necessity in the Assessment, copying and pasting prior notes without updating them, writing a Plan that only says “continue therapy” without actionable specifics, omitting a documented risk assessment, and including irrelevant personal details that add length without value.
What is the difference between SOAP, DAP, and BIRP notes?
SOAP notes organize documentation into Subjective, Objective, Assessment, and Plan sections and provide a clear separation between client self-report and clinician observation. DAP notes use Data, Assessment, and Plan, combining Subjective and Objective into a single section, which can be faster but less precise. BIRP notes use Behavior, Intervention, Response, and Plan, centering documentation more directly on the intervention itself.
For many insurance-billing contexts, SOAP offers the clearest audit trail and is often the safest default choice.
How do SOAP notes support insurance billing and medical necessity?
Payers use SOAP notes to verify that services were medically necessary and clinically appropriate. The Subjective and Objective sections establish the client's presenting condition and functional impairment. The Assessment connects those findings to a specific DSM-5 diagnosis, and the Plan shows the ongoing clinical rationale for continued treatment.
Weak or vague documentation in any section can lead to claim denials, audit failures, or reimbursement issues. Common triggers include Assessment entries that do not clearly explain why treatment is still needed and Plan sections that are not tied to specific diagnoses.
Recent Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) from Aspen University and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







