Blog > Documentation > Therapy Notes: Types, Formats, Examples & How to Write Them
Therapy Notes: A Complete Guide to Types, Formats, and Best Practices
Therapy notes are essential for documenting client care, supporting medical necessity, and protecting clinicians from audits and liability. This complete guide explains the different types of therapy notes, including progress notes, psychotherapy notes, intake assessments, treatment plans, and discharge summaries. You’ll learn how to choose the right therapy notes format (SOAP, DAP, or BIRP), see real-world therapy notes examples, and use a practical therapy notes template to streamline your workflow. The guide also covers clinical language for therapy notes, objective documentation strategies, HIPAA compliance, and proven methods to write therapy notes faster without sacrificing quality.

Donald Morrison, MSW, LCSW
Last Updated: March 31, 2026

What You'll Learn
- What therapy notes are and why they matter for clinical care, legal protection, and reimbursement
- The different types of therapy notes — progress notes, psychotherapy notes, intake notes, treatment plans, and discharge summaries
- How to choose the right therapy notes format (SOAP, DAP, BIRP) for your practice
- Real-world therapy notes examples showing effective documentation across different formats and clinical scenarios
- How to use clinical language for therapy notes that is objective, specific, and defensible
- A therapy notes template you can adapt to your workflow
- HIPAA compliance essentials for storing and sharing therapy notes
- Practical strategies to write therapy notes faster without sacrificing quality
Contents
- Types of Therapy Notes
- Therapy Notes Formats: SOAP, DAP, and BIRP
- Clinical Language for Therapy Notes
- Therapy Notes Examples
- Therapy Notes Template
- HIPAA Compliance for Therapy Notes
- Common Therapy Notes Mistakes
- How To Write Therapy Notes Faster
- Legal and Ethical Considerations
- Frequently Asked Questions About Therapy Notes
- ICANotes Makes Writing Therapy Notes Faster and Easier
What Are Therapy Notes?
Therapy notes are the clinical records that therapists, counselors, psychologists, and other mental health professionals create to document client care. Every session you conduct should result in some form of documentation — whether it's a progress note, an intake assessment, a treatment plan update, or a discharge summary.
Therapy notes serve several essential purposes. They track your client's progress over time, giving you a clear record to reference between sessions. They support continuity of care when multiple providers are involved. They establish medical necessity for insurance reimbursement. They create a legal record that protects you in the event of audits, complaints, or litigation. And they fulfill the ethical documentation standards set by professional organizations and state licensing boards.
Despite their importance, documentation is one of the biggest pain points in clinical practice. Research shows that clinicians spend an average of 13.5 hours per week on documentation — time that many would rather spend with clients. The key is learning how to write therapy notes that are thorough enough to be clinically useful and legally defensible, but efficient enough that they don't consume your day.
This guide covers everything you need to know about therapy notes: the types, the formats, real-world examples, clinical language guidance, templates, HIPAA compliance, and strategies to document faster.

Clinical Note Writing for Mental Health
Learn how to create meaningful, compliant, and defensible documentation with practical guidance on progress notes, treatment plans, risk assessment, medical necessity, and more.
Download the Free Guide
Complete the form below for instant access.
Types of Therapy Notes
Understanding the different types of therapy notes and when to use each one is foundational to effective clinical documentation. Each type serves a distinct purpose in the treatment process.
For a broader overview of all documentation types used in behavioral health — including assessments, treatment plans, and discharge summaries — see our beginner's guide to mental health notes.
Progress Notes
Progress notes are the most common type of therapy notes. You write one after each session to document what happened, what interventions you used, how the client responded, and what you plan to do next. Progress notes are part of the official medical record and may be reviewed by other providers, insurance companies, and auditors.
Well-written progress notes connect session content to treatment plan goals, document the medical necessity of your services, and create a defensible clinical record. They typically follow a structured format like SOAP, DAP, or BIRP (covered in detail below).
For a comprehensive deep-dive into writing progress notes — including detailed templates, sample notes, and billing guidance — see our full guide: How to Write Mental Health Progress Notes + Examples and Templates →
Psychotherapy Notes (Process Notes)
Psychotherapy notes — sometimes called process notes — are a therapist's private notes containing impressions, hypotheses, and personal reflections about a session. They are fundamentally different from progress notes in both purpose and legal status.
Psychotherapy notes are not part of the medical record. They are stored separately, are not required for billing, and receive special protection under HIPAA. Clients do not have an automatic right to access them, and insurance companies cannot require them as a condition of reimbursement.
Progress Notes vs. Psychotherapy Notes
| Category | Progress Notes | Psychotherapy Notes |
|---|---|---|
| Purpose | Document services provided, client progress, and link to treatment plan | Capture therapist's personal reflections, impressions, and analysis |
| Legal status | Part of the official medical record | Kept separate from the medical record |
| Access | May be requested by clients, insurers, or legal entities | Protected under HIPAA; not typically shared |
| Required for billing? | Yes | No |
| Content | Symptoms, interventions, assessment, progress toward goals | Hypotheses, impressions, details the therapist is processing privately |
For a complete breakdown of these distinctions, see our dedicated guide: Psychotherapy Notes vs. Progress Notes — What Are the Key Differences? →
Intake and Assessment Notes
Intake notes document the initial evaluation when a client first enters treatment. They capture the client's presenting problem, symptom history, medical and mental health background, social history, substance use, risk factors, and your initial clinical impressions. This documentation establishes the baseline for treatment and is typically required to demonstrate medical necessity.
Treatment Plans
Treatment plans outline the goals, objectives, interventions, and timeline guiding a client's care. They're created after the initial assessment and updated periodically — many insurers require reviews every 90 days. Treatment plans connect your ongoing session work to specific, measurable outcomes.
Discharge Summaries
Discharge summaries close out a course of treatment. They document why the client sought care, what services were provided, what progress was made, the client's condition at discharge, and any aftercare or follow-up recommendations. They're important for clinical handoffs and may be required for final reimbursement depending on the payer.
Therapy Notes Formats: SOAP, DAP, and BIRP
There are several standardized formats for structuring therapy notes. The three most widely used are SOAP, DAP, and BIRP. Each organizes clinical information differently, but they all aim to capture the same core elements: what the client reported, what you observed, what you did, how the client responded, and what happens next.
The right format depends on your clinical setting, payer requirements, and personal documentation style. What matters most is that you choose one and use it consistently.
SOAP Notes
SOAP stands for Subjective, Objective, Assessment, Plan. This format is common across healthcare settings and works well for therapists

who want a clear separation between client-reported information and clinical observations.
- Subjective: What the client reports — symptoms, concerns, stressors, goals. Use direct quotes when possible.
- Objective: What you observe — appearance, behavior, affect, speech, mental status indicators, assessment scores.
- Assessment: Your clinical interpretation — diagnostic impressions, progress toward goals, risk evaluation.
- Plan: Next steps — interventions to continue, homework, referrals, session frequency, follow-up topics.
DAP Notes
DAP stands for Data, Assessment, Plan. This format combines subjective and objective information into a single "Data" section, making it more streamlined than SOAP. Many therapists prefer DAP for its efficiency while still maintaining a clear clinical structure.
- Data: What the client reported and what you observed — combined into one narrative section.
- Assessment: Your clinical reasoning, interpretation, and evaluation of progress.
- Plan: Interventions, homework, referrals, and focus for future sessions.
BIRP Notes
BIRP stands for Behavior, Intervention, Response, Plan. This format emphasizes what happened during the session — specifically, how the client behaved, what the therapist did, and how the client responded. It's particularly useful when you want to track the effectiveness of specific interventions over time.
- Behavior: What the client said and did — verbal statements, emotional expressions, observable actions.
- Intervention: The therapeutic techniques and strategies you used during the session.
- Response: How the client reacted to your interventions — engagement, insight, resistance, behavioral changes.
- Plan: Next steps for treatment, homework assignments, and any adjustments to the approach.
Which Format Should You Use?
There's no single correct answer. SOAP is the most widely recognized and may be preferred if you work in a medical or multidisciplinary setting. DAP is efficient for solo practitioners who want less structure. BIRP is strong for tracking intervention effectiveness session over session. Some clinicians switch formats depending on the session type — using SOAP for intake sessions and DAP for regular follow-ups, for example.
The most important thing is consistency within your practice. Pick a format, learn it well, and make sure your notes meet payer and compliance requirements regardless of which structure you choose.
Whichever format you select, ICANotes can help you implement it consistently and compliantly. ICANotes structures progress notes using a menu-driven interface that walks you through each required section — from client presentation and clinical observations to interventions, treatment plan linkage, risk assessment, and the session plan. Because the content options are built from clinically validated language and mapped to documentation standards, the resulting notes meet payer, audit, and legal requirements by design. You're not relying on memory to hit every compliance element — the template guides you through it. ICANotes supports SOAP, DAP, BIRP, and narrative formats, so you can use the structure that fits your practice while maintaining the documentation rigor that protects your license and your revenue.
Clinical Language for Therapy Notes
One of the most common challenges therapists face is choosing the right language for their documentation. Therapy notes need to be objective, specific, and clinically defensible — which means avoiding vague or subjective phrasing that could be questioned in an audit or legal review.
Objective vs. Subjective Language
A frequent question therapists ask is whether they can use words like "appeared" or "seemed" in their notes. The answer depends on how you use them. "Client seemed upset" is vague — it tells the reader nothing concrete. "Client appeared tearful, with reddened eyes and a trembling voice, and stated, 'I don't know how much more I can take'" is objective, because you're describing observable behaviors and quoting the client directly.
The key principle: describe what you saw, heard, and what the client said — not what you interpreted or assumed.

What to Write Instead
Here's a reference table of common vague phrases and their objective alternatives:
| Instead of this... | Write this... |
|---|---|
| Client seemed anxious | Client displayed rapid speech, fidgeting, and avoided eye contact |
| Client was in a good mood | Client smiled frequently, reported feeling "better than last week," and maintained an upbeat tone |
| Good session | Client engaged actively in role-play exercise and identified two alternative coping strategies |
| Client seemed resistant | Client crossed arms, gave brief responses, and stated, "I don't see how this will help" |
| Client appeared better | Client reported sleeping 7 hours per night (up from 4), and PHQ-9 score decreased from 14 to 8 |
| Client was angry | Client spoke in a raised voice, made fists, and stated, "I'm tired of being ignored" |
| Client was uncooperative | Client declined to complete the thought record, stating, "I didn't have time this week" |
| Therapy is going well | Client has achieved 2 of 3 treatment plan objectives and reports decreased frequency of panic attacks from daily to twice weekly |
Objective Content in Therapy Notes
The objective content in your therapy notes — what you directly observed during the session — is one of the most important elements of defensible documentation. It anchors your clinical assessment in facts rather than opinions. Strong objective content includes:
- Appearance and behavior: Grooming, posture, eye contact, psychomotor activity, level of cooperation
- Speech: Rate, volume, tone, coherence
- Mood and affect: Mood is what the client reports ("I feel anxious"); affect is what you observe (tearful, flat, congruent with stated mood)
- Thought process and content: Logical, tangential, circumstantial; presence or absence of suicidal/homicidal ideation, delusions, obsessions
- Cognition and insight: Orientation, judgment, awareness of their own patterns
- Assessment scores: Include instrument name, score, date, and delta from last administration (e.g., "PHQ-9 = 8, down from 12 on 8/01")
Aim to include at least three mental status observations in every progress note. This strengthens the clinical foundation of your documentation and helps justify your assessment and treatment decisions.
How Strong Are Your Progress Notes?
Take our free 5-minute Progress Note Self-Assessment Tool to see how your documentation stacks up. Identify gaps, reduce compliance risk, and get practical insight into whether your notes are audit-ready.
It’s a quick way to spot documentation weaknesses before they become billing or compliance problems.
Take the 5-Minute Self-Assessment
Therapy Notes Examples
Seeing real-world therapy notes examples makes it easier to understand how different formats work in practice. Below are sample notes across several formats and clinical scenarios. Each demonstrates how to be concise, objective, and clinically relevant.
Therapy Notes Template
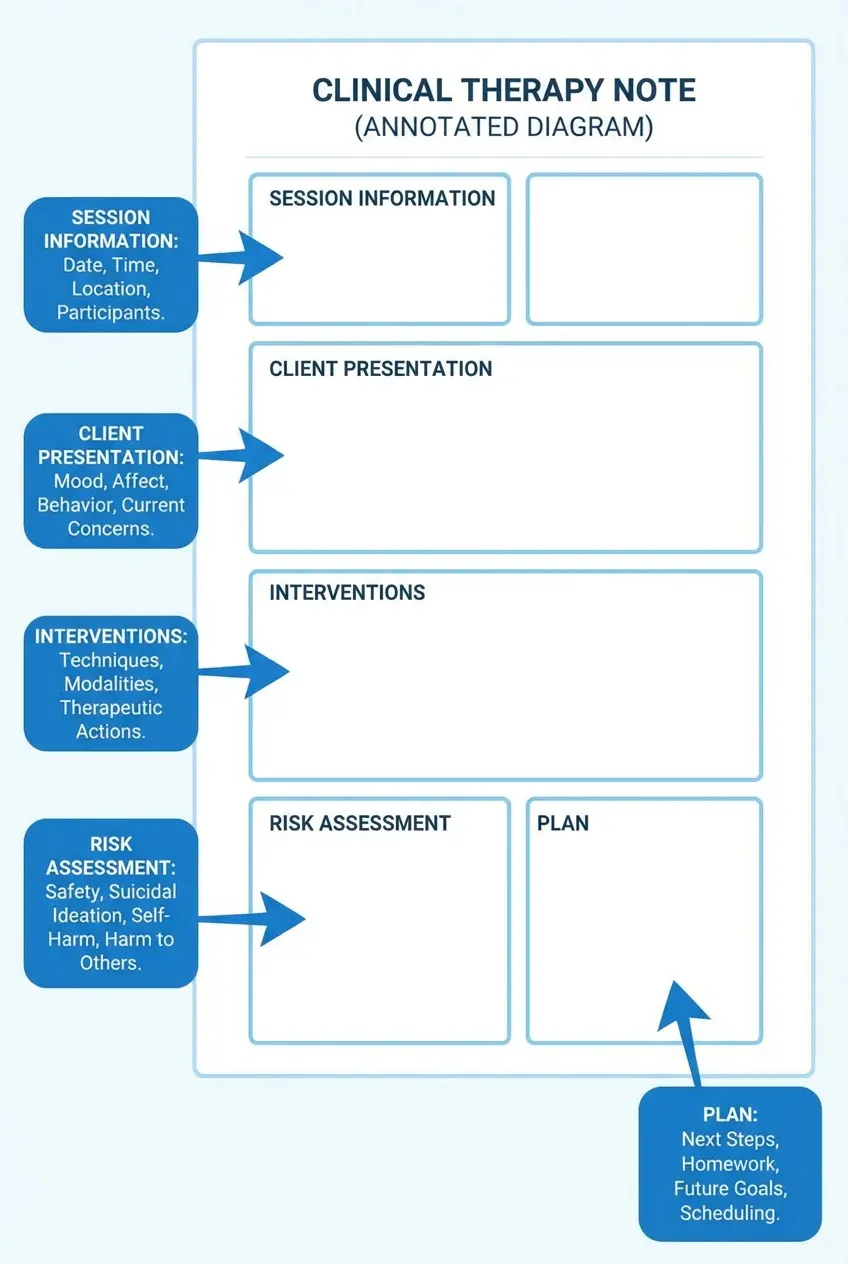
While the specific format of your therapy notes will vary depending on whether you use SOAP, DAP, BIRP, or another structure, every therapy note should cover a core set of elements. Use this as a universal checklist to make sure your documentation is complete regardless of format.
This template can be adapted to fit SOAP, DAP, BIRP, or any other format your practice uses. The key is making sure every element is addressed in every note, regardless of where it falls in the structure.
Session Information
- Date of service
- Start and end time
- Session type (individual, couples, group, family)
- Session format (in-person or telehealth; if telehealth, client's location)
- Client name and unique identifier (date of birth or client ID)
- Provider name and credentials
Client Presentation
- Client's self-reported concerns, symptoms, or focus for the session (use direct quotes)
- Observable presentation: appearance, behavior, mood, affect, speech
- At least three mental status observations
- Any changes from the previous session
Clinical Content
- Interventions used (name the modality — CBT, DBT, EMDR, MI, etc.)
- Client's response to interventions (engagement, insight, resistance, behavioral change)
- Progress toward treatment plan goals (reference specific objectives)
- Any homework assigned or reviewed
Risk Assessment
- Suicidal ideation: present or denied
- Homicidal ideation: present or denied
- Self-harm: present or denied
- Safety plan: reviewed, updated, or not indicated
Plan
- Focus for next session
- Changes to treatment approach or frequency
- Referrals made (medication, psychiatry, testing, community resources)
- Next appointment date
Clinician Signature and Credentials
- Clinician name, signature, and credentials
This diagram shows how therapy notes are typically structured, helping clinicians organize documentation in a clear, consistent, and defensible format.
Related: For format-specific templates with fill-in examples, see our guides to SOAP notes, DAP notes, and BIRP notes.
What Do Therapists Write in Their Notes?
If you're a client wondering what your therapist writes during or after your session — or a new clinician trying to understand what's expected — here's what therapy notes typically contain and what they don't.
Not everything discussed in a session belongs in your progress notes. Here’s what to include—and what to leave out.
- What you reported feeling, experiencing, or struggling with (often including your exact words)
- Observable details about how you presented — your mood, energy level, body language, speech patterns
- The topics discussed and therapeutic techniques used
- Your response to interventions — whether something seemed to click, whether you pushed back, whether you tried a new skill
- Progress toward the goals you set together in your treatment plan
- Any safety concerns or risk factors
- The plan for your next session
- Personal opinions or value judgments about you
- Detailed accounts of every story or anecdote you shared (only what's clinically relevant)
- The therapist's private hypotheses or emotional reactions — those go in psychotherapy notes, which are stored separately and are not part of your medical record
Under HIPAA, you generally have the right to request copies of your progress notes. Psychotherapy notes, however, receive additional protections and are not automatically accessible to clients. Your therapist can explain their specific documentation practices during the informed consent process.
HIPAA Compliance for Therapy Notes
Protecting client information is a core responsibility when creating and storing therapy notes. HIPAA sets the floor for how therapy documentation must be handled, but state laws and professional licensing boards may impose additional requirements.
Protected Health Information in Therapy Notes
Therapy notes contain Protected Health Information (PHI) by definition — client names, diagnoses, session dates, treatment details, and any information that could identify the individual. HIPAA requires that your notes contain only the minimum necessary information required for treatment, payment, and healthcare operations. Avoid including extraneous details that aren't clinically relevant.
Storing Therapy Notes Securely
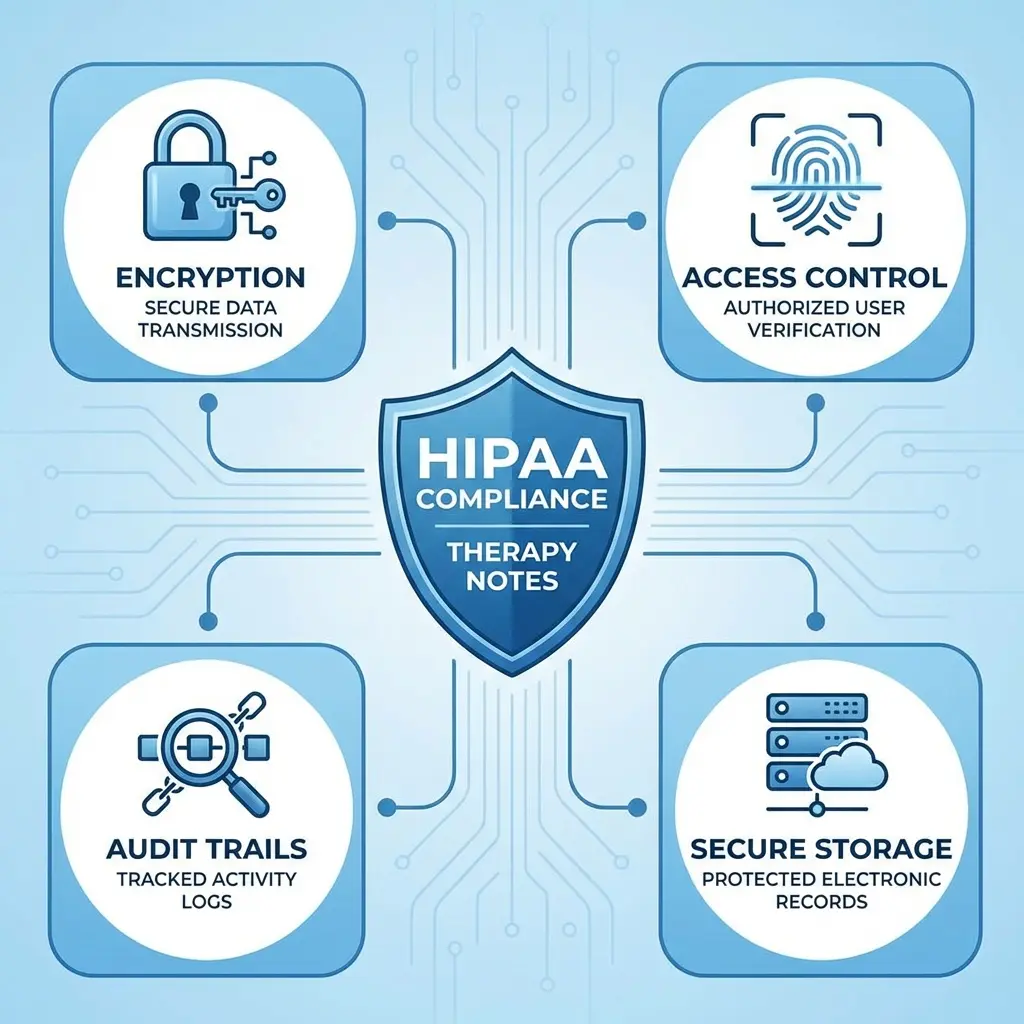
If you're using an electronic system (which you should be), it must meet HIPAA's technical safeguards:
- Encryption for data at rest and in transit
- Access controls with user authentication and role-based permissions
- Audit trails logging who accessed records and when
- Automatic backups to prevent data loss
- Business Associate Agreements (BAAs) with any third-party service that handles PHI
A behavioral health–specific EHR like ICANotes is built to meet these requirements out of the box, so you don't have to piece together compliance across multiple tools.
Documentation Retention
Therapy notes must be retained according to your state's laws and professional licensing board guidelines. Retention periods typically range from 7 to 10 years for adult clients, with longer periods required for minors (often until a set number of years after the client reaches the age of majority). Develop clear policies for retention timelines, secure destruction methods, and documentation of the destruction process.
Common Therapy Notes Mistakes
Even experienced therapists fall into documentation habits that create risk. Here are the most common mistakes and how to fix them.
| Mistake | What it looks like | What to do instead |
|---|---|---|
| Vague language | "Good session." "Client seemed better." "Therapy going well." | Document observable behaviors, specific client statements, and measurable changes. |
| No connection to treatment plan | Session content doesn't reference goals or objectives. | Explicitly tie each session to specific treatment plan goals. Note which objective was addressed and whether progress was made. |
| Inconsistent documentation | Detail level, format, and terminology vary from note to note. | Choose a format and use it consistently. Use templates to standardize structure. |
| Delayed documentation | Notes written days or weeks after the session. | Complete notes the same day. If you can't, use voice memos or brief bullet points to capture key details for expansion later. |
| Copy-pasting previous notes | Multiple sessions read identically, suggesting no progress. | Write each note fresh. Even when addressing recurring issues, describe new observations, different client responses, or updated interventions. |
| Inappropriate content | Personal opinions, judgments, or speculative statements. | Stick to clinical observations and professional assessment. If including interpretations, label them clearly and connect them to clinical reasoning. |
| Missing risk assessment | No mention of safety screening in the note. | Address risk in every note, even if only to document that the client denied SI/HI and no safety concerns were observed. |
How to Write Therapy Notes Faster
How to Write Therapy Notes: A 5-Step Process
Strong therapy notes usually follow the same basic sequence: document what the client reported, what you observed, what interventions you used, how you assessed the session, and what happens next.
Client Report
Document the client’s self-reported symptoms, concerns, stressors, and session focus. Use direct quotes when they add clinical value.
Observe
Record objective details such as appearance, affect, speech, behavior, mental status findings, and any assessment scores.
Intervene
Name the therapeutic interventions you used, such as CBT, DBT, MI, EMDR, psychoeducation, or skills coaching.
Assess
Summarize your clinical impression, the client’s response to treatment, progress toward goals, and any safety considerations.
Plan
Note next steps, homework, follow-up priorities, referrals, changes in treatment approach, and the next appointment date.
Therapy documentation doesn't have to consume hours of your day. These strategies help you write therapy notes efficiently without sacrificing quality or compliance.
Use templates built for behavioral health. A general-purpose EHR forces you to build your own documentation workflows from scratch. A behavioral health–specific system like ICANotes provides pre-configured, menu-driven templates for every session type — intake, individual therapy, group, couples, medication management, and more. Instead of typing full paragraphs, you select clinically validated phrases that generate polished narrative notes in a fraction of the time.
Try concurrent documentation. When clinically appropriate, complete portions of your notes during the session. This works especially well for recording assessment scores, reviewing homework, and documenting agreed-upon goals. Be transparent with your client about why you're taking notes — most clients are comfortable with it once they understand the purpose.
Focus on clinical relevance. Not everything discussed in a session needs to be documented. Concentrate on information that relates to the client's diagnosis, treatment plan goals, risk factors, and significant life events affecting treatment. If a detail doesn't serve a clinical or legal purpose, leave it out.
Block documentation time into your schedule. Adding a 5-10 minute buffer between sessions gives you dedicated time to complete notes while the session is still fresh. This prevents documentation from piling up at the end of the day — or worse, the end of the week.
Include brief assessment score deltas. Instead of lengthy narrative descriptions of progress, use measurement shorthand: "PHQ-9 = 8, down from 12 on 8/01." This is concise, objective, and immediately communicates progress to anyone reviewing the note.
Use your EHR's auto-population features. Session details like date, time, client name, and provider credentials can be auto-filled. Built-in risk assessment checkboxes and intervention menus reduce the number of elements you need to write from scratch. The less manual entry, the faster you finish.
Legal and Ethical Considerations
Beyond HIPAA compliance, therapy notes must meet legal and ethical standards that vary by state and licensing board. Here are the key areas to be aware of.
Subpoenas and Court Orders
Therapy records can be subpoenaed in legal proceedings, but a subpoena is not the same as a court order. A subpoena is a request; a court order is a directive from a judge. If you receive a subpoena, verify its validity, determine exactly which records are being requested, consider consulting an attorney, obtain client consent when possible, and provide only the minimum necessary information. Never release records without understanding your legal obligations.
State-Specific Requirements
Therapy documentation requirements vary by state and professional licensing board. Stay informed about content requirements for therapy notes in your state, signature and date requirements, electronic record regulations, and supervision documentation standards for pre-licensed professionals.
Informed Consent for Documentation
Clients should understand your documentation practices as part of the informed consent process. Cover what types of information you record, how records are stored and for how long, who may have access to their records, circumstances under which records may be disclosed, and their rights regarding accessing their own documentation.
Related: Mental Health Malpractice: Common Lawsuit Triggers and How to Protect Your Practice →
Frequently Asked Questions About Therapy Notes
ICANotes Makes Writing Therapy Notes Faster and Easier
No matter which type of therapy note you write — SOAP, DAP, BIRP, or narrative progress notes — ICANotes is built to make documentation faster, easier, and more compliant.
Menu-driven charting, not blank text boxes. Instead of staring at a blank screen, you select from clinically validated phrases and content blocks that generate polished, narrative-style notes. Most clinicians complete a full progress note in about 5 minutes.
Templates for every session type. ICANotes includes pre-configured templates for individual therapy, group sessions, couples therapy, psychiatric evaluations, medication management, and more. Every template is fully customizable to match your workflow and documentation preferences.
Built-in compliance and coding. Notes are automatically structured in audit-ready formats, and ICANotes maps your documentation to accurate CPT and ICD billing codes — reducing claim denials and coding errors.
Integrated clinical tools. Risk assessments, outcome measures, treatment plan tracking, e-prescribing, telehealth, and billing are all built into one system. No switching between platforms. No gaps in your documentation.
Designed exclusively for behavioral health. ICANotes isn't a general medical EHR with a behavioral health add-on. It was built from the ground up for therapists, counselors, psychiatrists, and other behavioral health providers.
Ready to spend less time on therapy notes and more time with your clients? Start your free trial → or schedule a live demo → to see how ICANotes works.
Start Your 30-Day Free Trial
Experience the most intuitive, clinically robust EHR designed for behavioral health professionals, built to streamline documentation, improve compliance, and enhance patient care.
- Complete Notes in Minutes - Purpose-built for behavioral health charting
- Always Audit-Ready – Structured documentation that meets payer requirements
- Keep Your Schedule Full – Automated reminders reduce costly no-shows
- Engage Clients Seamlessly – Secure portal for forms, messages, and payments
- HIPAA-Compliant Telehealth built into your workflow

Related Posts
About the Author
Donald Morrison graduated from UNC Charlotte in 2004. He has since worked as a school-based therapist, inpatient social work supervisor and outpatient clinician. Donald currently works in private practice, and he is also an adjunct faculty member at the UNC Charlotte School of Social Work. In addition, Donald serves as a clinical supervisor to LCSW associates, and he regularly presents at area mental health conferences and seminars.







