Blog > Documentation > Mental Health Notes: Types, Formats & What to Include
Beginner's Guide to Mental Health Notes
Mental health notes are the foundation of effective clinical care, compliant documentation, and successful reimbursement. In this guide, you’ll learn the key types of mental health notes — assessments, psychotherapy notes, progress notes, treatment plans, and discharge summaries — along with what to include in each and how to write them efficiently. Whether you're new to mental health or refining your workflow, this resource will help you create clear, audit-ready notes that support better outcomes and protect your practice.

Last Updated: March 30, 2026


What You'll Learn
- What mental health notes are and why they matter for care, compliance, and reimbursement
- The key types of mental health notes and when to use each one
- What to include in assessments, progress notes, treatment plans, and discharge summaries
- Common note-taking mistakes clinicians make — and how to avoid them
- Time-saving tips and tools for writing clear, compliant notes faster
Behavioral health clinicians rely on mental health notes to document care, track client progress, and support reimbursement. Whether you’re conducting an initial assessment or documenting an ongoing session, these notes provide a structured way to connect symptoms, diagnoses, and treatment decisions over time. Without clear documentation, it becomes difficult to ensure continuity of care, demonstrate medical necessity, or recall important clinical details across sessions.
What Are Mental Health Notes?
Mental health notes are the clinical records a mental health professional creates during or after an appointment with a client. They capture the client's diagnosis, current status, what was discussed during the session, the clinician's assessment, the treatment plan, and any other relevant health information.
If you're new to the behavioral health field or about to open a private practice, understanding the different types of mental health notes is one of the first things you need to get right. Each type of note serves a different purpose — from documenting a client's initial evaluation to tracking their progress over time to summarizing their care at discharge.
As the American Psychological Association (APA) states, mental health professionals have an ethical and professional responsibility to maintain accurate records. Mental health notes are a necessity because they help clinicians:
- Provide high-quality care. Notes for mental health allow you to monitor a client's progress without relying only on your memory. They help you connect a client's behaviors, symptoms, and statements to form a more accurate diagnosis. If something isn't working in treatment, you can use your notes to guide adjustments to the treatment plan.
- Remember clients between sessions. Some mental health professionals see over 20 clients per week. Trying to remember each individual's mood, thoughts, and feelings without writing these details down is nearly impossible — especially when days or weeks pass between visits. A mental health note from the last session gives you what you need to pick up where you left off.
- Get reimbursed. Insurance companies may need to see your notes to determine whether they will accept or deny a claim. The Centers for Medicare and Medicaid Services, for example, require documentation that reflects medical necessity. Accurate, thorough notes for mental health help you share specific details error-free and get paid for your services.
- Coordinate care across providers. By storing your notes in an electronic health record (EHR) system, you can securely share your client's information with their primary care physician or other providers. This supports informed decision-making across the care team, prevents duplicate testing, and saves clients time and frustration.
- Protect yourself legally. Detailed mental health notes create evidence of a client's diagnosis and how you treated them. If a client files a complaint with the licensing board or initiates legal proceedings, your notes can support your case.
Download Our Guide to Writing Better, Faster Clinical Notes
Streamline your notes, avoid documentation pitfalls, and stay compliant with practical templates, note formats (SOAP, DAP, BIRP), and time-saving tips to write high-quality, defensible notes faster.
Mental health professionals write different types of mental health notes depending on where a client is in the treatment process and what the documentation requirements are. Here are the most important types to understand.
1. Assessments
Clinicians use assessments to learn about new clients, form diagnoses, and develop treatment plans. Behavioral health professionals typically assess clients during their initial sessions, though they should re-evaluate periodically and adjust treatment plans as needed.
The clinical interview is one common assessment method. During a clinical interview, you ask the client questions about their medical history, current symptoms, family history, childhood, and relationships to form a clearer diagnostic picture.
Clinicians may also use biopsychosocial assessments, which evaluate clients holistically by considering biological, psychological, and social factors. A biopsychosocial assessment typically covers current symptoms, medical and mental health history, current and past relationships, employment and educational background, legal issues, and substance use history.
Initial assessments are typically required to establish medical necessity and get approved for reimbursement by insurers and government programs.
Related:
How to Write a Biopsychosocial Assessment
Essential Components of an Initial Psychiatric Evaluation
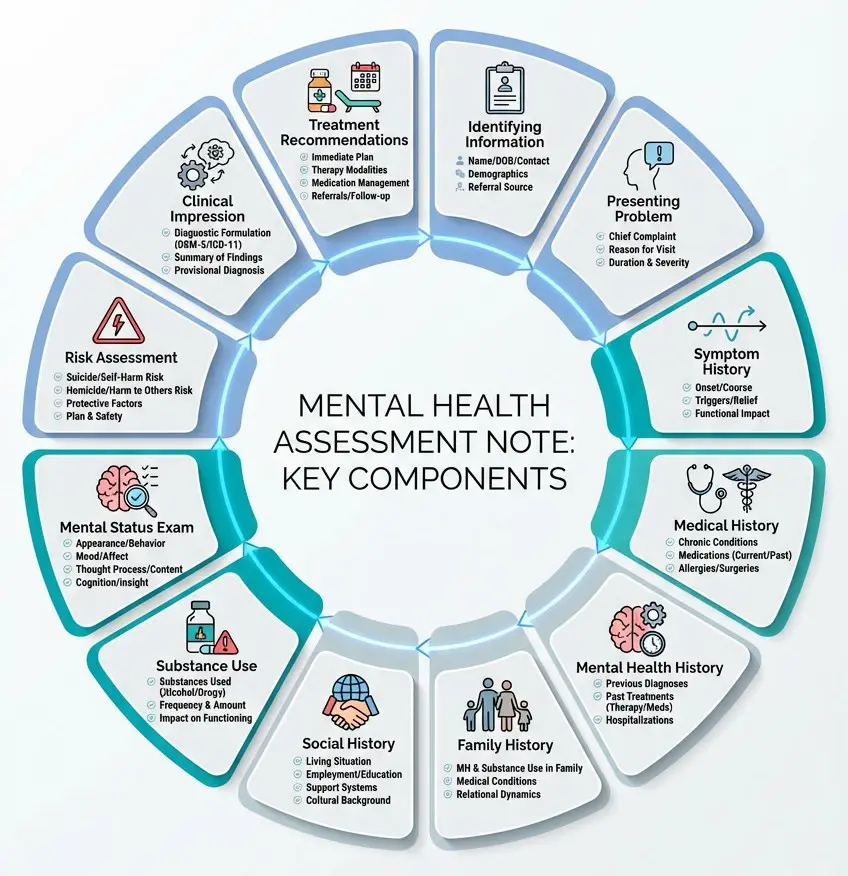
What to Include in an Assessment Note
A strong assessment note gives a complete baseline picture of the client. While the specific format may vary depending on your setting and payer requirements, most assessment notes should cover:
- Identifying information: Client name, date of birth, date of assessment, and referral source
- Presenting problem: The reason the client is seeking treatment, in their own words when possible
- Symptom history: Onset, duration, severity, and any previous treatment for the presenting issue
- Medical history: Current medications, relevant medical conditions, allergies
- Mental health history: Prior diagnoses, hospitalizations, previous therapy or counseling
- Family history: Relevant mental health or substance use history among family members
- Social history: Living situation, relationships, employment, education, legal involvement
- Substance use: Current and past use, frequency, impact on functioning
- Mental status exam findings: Appearance, behavior, mood, affect, thought process, cognition, insight, and judgment
- Risk assessment: Suicidal ideation, homicidal ideation, self-harm history, safety concerns
- Clinical impression: Preliminary diagnosis or diagnostic considerations
- Initial treatment recommendations: Recommended level of care, frequency, and modalities
2. Psychotherapy Notes
Psychotherapy notes are a clinician's private notes taken during or after sessions. They are not required for reimbursement and must be kept separate from the client's medical record. Under the HIPAA Privacy Rule, clients do not have a right to access your psychotherapy notes — though you may choose to share them if a client asks.
Since psychotherapy notes are optional, they do not need to follow a particular format. Their purpose is to help you do your job better. Depending on your needs, they may include your thoughts, impressions, hypotheses, and observations from a session — anything that helps you provide better care.
Related:
Psychotherapy Notes vs. Progress Notes — What Are the Key Differences?
3. Progress Notes
Progress notes are the clinical records you create after each therapy session to document a client's current status and progress toward treatment goals. Unlike psychotherapy notes, progress notes are part of the medical record and are meant to be shared with appropriate parties — including other providers, insurers, and auditors.
Progress notes are critical for receiving reimbursement. Insurance companies routinely review them to verify that services are medically necessary and that clients are making progress. These notes need to be concise, accurate, and compliant with HIPAA.
There are several standardized formats for writing mental health notes in a progress note structure. The most common are:
- SOAP (Subjective, Objective, Assessment, Plan) — widely used across healthcare settings
- DAP (Data, Assessment, Plan) — a streamlined alternative favored by many therapists
- BIRP (Behavior, Intervention, Response, Plan) — emphasizes in-session interaction and client response
The best format depends on your clinical setting, your documentation requirements, and your personal preference. What matters most is consistency, clarity, and compliance.
SOAP vs. DAP vs. BIRP: Common Progress Note Formats
Many clinicians use a structured note format to make progress notes faster to write and easier to review. SOAP, DAP, and BIRP are three of the most common options in behavioral health. Each format helps organize clinical thinking a little differently, but all three can support clear, compliant documentation.
SOAP
A classic healthcare format that separates client report, clinician observations, assessment, and next steps.
What It Stands For
- S – Subjective
- O – Objective
- A – Assessment
- P – Plan
Common Use
SOAP notes are widely used across healthcare settings and work well for clinicians who want a familiar, highly structured format that clearly separates what the client reports from what the clinician observes.
Why Clinicians Like It
It creates a consistent, audit-friendly framework and makes it easier to connect symptoms, clinical impressions, and treatment planning in a standardized way.
DAP
A streamlined format that combines subjective and objective information into one concise section.
What It Stands For
- D – Data
- A – Assessment
- P – Plan
Common Use
DAP notes are often favored by therapists and counselors who want a simpler structure for documenting session content, clinical interpretation, and the next steps in treatment.
Why Clinicians Like It
It is efficient, easy to repeat across sessions, and helps clinicians stay concise without losing the key information needed for continuity of care and reimbursement.
BIRP
A format that highlights what happened in session, what the clinician did, and how the client responded.
What It Stands For
- B – Behavior
- I – Intervention
- R – Response
- P – Plan
Common Use
BIRP notes are useful when you want to emphasize in-session interventions and document how the client reacted to the therapeutic work completed during the appointment.
Why Clinicians Like It
It clearly shows medical necessity by linking the client’s presentation, the intervention provided, the client’s response, and the follow-up plan in a very practical sequence.
For a complete guide to writing progress notes — including full SOAP, DAP, and BIRP templates with examples, billing guidance, and documentation tips — see our in-depth resource: How to Write Mental Health Progress Notes + Examples and Templates
Related:
4. Treatment Plans
A treatment plan is a structured, goal-oriented document that serves as a roadmap for a client’s care. It translates your clinical assessment into a clear plan of action, outlining what you’re working toward, how you’ll get there, and how progress will be measured over time. In most outpatient settings, treatment plans are developed early in care — often within the first one or two sessions—and updated regularly as the client progresses.
Effective treatment plans are not static documents. They should evolve alongside the client’s needs, symptoms, and circumstances. As new information emerges or goals are met, clinicians revise the plan to reflect current priorities and ensure continued medical necessity. Many payers require formal treatment plan reviews at set intervals (commonly every 90 days), making accuracy and alignment with progress notes especially important.
At their core, treatment plans should clearly connect three elements: the client’s diagnosis, the goals of treatment, and the interventions you’ll use. This connection is what demonstrates clinical intent and supports reimbursement. For example, if a client is diagnosed with generalized anxiety disorder, the treatment plan should include specific goals related to reducing anxiety symptoms, measurable objectives that track progress (such as frequency or intensity of symptoms), and evidence-based interventions like cognitive behavioral therapy or relaxation training.
A strong treatment plan also reflects collaboration. Whenever possible, goals should be developed with the client, using language that is meaningful and motivating to them. This not only improves
engagement but also increases the likelihood that the client will follow through on between-session work and long-term treatment recommendations.
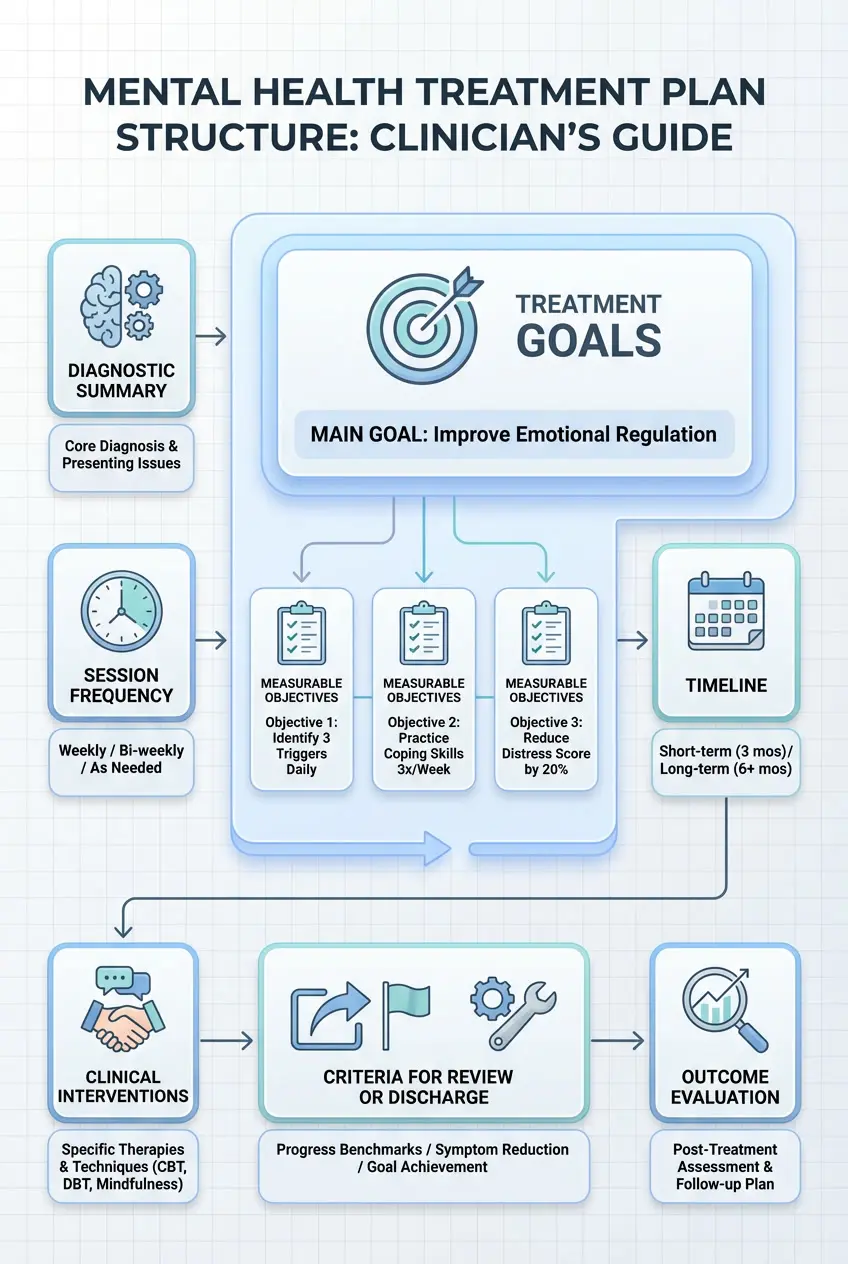
What to Include in a Treatment Plan
While formats may vary depending on your practice setting or payer requirements, most treatment plans include:
- Demographic and identifying information — client name, date of birth, and relevant administrative details
- Diagnostic summary — current diagnoses and key clinical impressions
- Goals — broad, outcome-focused statements describing what the client hopes to achieve
- Objectives — specific, measurable steps that indicate progress toward each goal
- Interventions — the therapeutic approaches, techniques, or services you will use
- Frequency and duration of services — how often sessions occur and expected length of treatment
- Timeline and review criteria — when progress will be evaluated and how success will be measured
- Discharge criteria — indicators that treatment goals have been met or services can be reduced or ended
Treatment plans help clinicians get authorized by insurers to continue providing services. Many insurance companies require regular treatment plan reviews and updates — typically every 90 days, though requirements vary by payer.
5. Discharge Summaries
Mental health professionals create discharge summaries when a client completes a treatment program, discontinues services, or is released from inpatient care. A discharge summary closes the loop on a course of treatment and ensures continuity for any providers who take over the client's care.
A discharge summary typically includes:
- Reason for treatment — the presenting problem and diagnosis at intake
- Summary of services provided — types and frequency of interventions delivered
- Progress made — how the client's symptoms and functioning changed during treatment
- Client's condition at discharge — current mental status, symptom severity, and functional level
- Reason for discharge — whether the client met treatment goals, transferred care, or discontinued services
- Aftercare and follow-up plan — referrals, recommended next steps, relapse prevention strategies, and emergency contact information
Discharge summaries are important for communicating aftercare instructions to clients and their families. They also provide a clinical handoff to other providers. Depending on the client's insurance carrier, discharge summaries may be required for final reimbursement.
Quick Reference: Types of Mental Health Notes at a Glance
This quick-reference table gives clinicians a simple overview of when each note type is created, who typically has access to it, and whether it is generally required for billing.
| Note Type | When It’s Created | Who Sees It | Required for Billing? |
|---|---|---|---|
| Assessment | Initial session or re-evaluation | Care team, insurers | Yes (establishes medical necessity) |
| Psychotherapy Notes | During or after sessions | Clinician only | No |
| Progress Notes | After each session | Care team, insurers, auditors | Yes |
| Treatment Plan | After initial assessment, updated periodically | Care team, insurers | Yes (often required for continued authorization) |
| Discharge Summary | At end of treatment | Care team, client/family, insurers | Varies by payer |
Common Mental Health Note Mistakes to Avoid
Even experienced clinicians can fall into documentation habits that create compliance risks, weaken reimbursement claims, or compromise care quality. Here are the most common mistakes to watch for when writing mental health notes.
- Using vague or subjective language. Phrases like "client seemed better" or "patient was in a good mood" don't give other providers or auditors anything concrete to work with. Instead of interpreting a client's state, describe what you actually observed — their affect, behavior, speech, and specific statements. Objective language strengthens your notes clinically and legally.
- Skipping required elements. Every mental health note needs basics like the client's name, your name and credentials, the date, session start and end times, and your electronic signature. It's easy to overlook these details when you're rushing through documentation, but missing them can trigger audit flags and create legal exposure.
- Writing notes days or weeks after a session. The longer you wait, the less accurate your notes become. Late documentation also raises red flags for auditors and insurers. Aim to complete your notes the same day — or at minimum, within 24 hours.
- Copying and pasting from previous notes. Reusing language from prior sessions makes it look like the client isn't progressing and can call medical necessity into question. Each note should reflect what actually happened in that specific session, even if you're addressing recurring issues.
- Including unnecessary personal opinions or assumptions. Mental health notes should document clinical facts, observations, and professional assessments — not personal judgments about the client. Avoid editorializing or speculating beyond what the clinical evidence supports.
- Not linking notes to the treatment plan. If your notes don't reference the client's treatment goals, it's difficult to demonstrate that your services are medically necessary. Always connect what happened in the session to the goals and objectives in the treatment plan.
- Relying on handwritten notes. Handwritten mental health notes are harder to read, easier to lose, and far more time-consuming to create than electronic documentation. Creating notes in an EHR system ensures legibility, security, and faster completion.
- Not staying current on documentation requirements. Record-keeping laws, ethical guidelines, and payer requirements can change. What was compliant two years ago may not be today. Make it a habit to review your state's documentation standards and the requirements of the insurance companies you work with at least annually.
Good vs. Bad Documentation: What Strong Mental Health Notes Look Like
One of the biggest differences between weak and defensible clinical notes is specificity. Vague language can leave too much open to interpretation, while clear, objective documentation helps support continuity of care, medical necessity, and compliance.
Weak or Vague Documentation
These examples are too general to paint a clear clinical picture or show why treatment was necessary.
“Client seemed upset.”
“Talked about stress.”
“Doing better.”
“Session went well.”
Stronger, More Defensible Documentation
These examples are more specific, clinically useful, and easier to support in the medical record.
“Client tearful throughout session and reported feeling overwhelmed by work deadlines and conflict with a supervisor.”
“Session focused on panic symptoms triggered by an upcoming custody hearing and the client’s fear of losing parenting time.”
“Client reported fewer nighttime awakenings this week and stated that breathing exercises reduced anxiety intensity from 8/10 to 5/10.”
“Session addressed cognitive distortions related to social rejection; client practiced reframing statements and demonstrated improved insight by the end of the visit.”
Tips for Writing Mental Health Notes
Now that you know what to avoid, here are positive habits that will help you write mental health notes that are concise, compliant, and clinically useful.
- Follow a consistent format. Using a standardized format — whether it's SOAP, DAP, BIRP, or your practice's preferred structure — gives you a repeatable framework for every session. It helps you focus on the essential elements without overthinking what to include.
- Keep it concise. Mental health notes don't need to be textbook-length documents. Focus on the most clinically relevant information — what relates to the client's diagnosis, treatment plan, and progress. If a detail doesn't serve a clinical purpose, leave it out. Writing mental health notes should take roughly 10–15 minutes per session. If it's taking you longer, look for areas where you can tighten up.
- Always include a risk assessment. Every progress note should address risk, even if there are no concerns. A simple statement like "Client denied suicidal and homicidal ideation; no current safety concerns noted" provides important clinical and legal protection.
- Include direct quotes when relevant. Using a client's own words adds specificity, shows individualized care, and gives other providers (and auditors) a clearer picture of the session. For example: "I feel like I'm stuck in the same cycle and don't know how to break it."
- Schedule dedicated documentation time. Block 10–15 minutes after each session for writing mental health notes. Treating documentation as part of your workflow — rather than something you squeeze in at the end of the day — helps you stay accurate and avoid a backlog.
- Use an EHR built for behavioral health. An electronic health record system like ICANotes allows you to use customizable, menu-based templates to document sessions with minimal typing. You can generate progress notes, treatment plans, discharge summaries, and other mental health notes in minutes rather than spending 30 minutes or more writing each one by hand.
Related:
Write Better and Faster Mental Health Notes with ICANotes
Crafting high-quality mental health notes doesn't have to be a burden. ICANotes transforms documentation into a fast, intuitive, and clinically robust process designed specifically for mental health providers.
- Menu-driven, narrative-style notes. Select pre-written, clinically validated phrases through a smart menu-based interface. These clicks generate polished, paragraph-style notes that read naturally — with about 80% less typing.
- Templates tailored for behavioral health. Choose from a library of templates covering progress notes, SOAP/DAP/BIRP formats, treatment plans, assessments, discharge summaries, and more. Every template is fully customizable to fit your specialty and documentation requirements.
- Compliance and coding support built in. ICANotes automatically maps your selected phrases to accurate CPT and ICD billing codes and structures documentation in audit-ready formats — reducing errors and improving reimbursement efficiency.
- Narrative depth with audit-ready structure. Notes maintain a natural narrative flow that conveys clinical nuance, while still meeting payer and legal requirements.
- Significant time savings. Clinicians report reducing documentation time from approximately 30 minutes per note to just 5 minutes — freeing up as much as 90 minutes daily for client care or personal time.
With ICANotes, you're not just charting faster — you're charting smarter. Request your free trial or schedule a live demo to see how it works for you.
Schedule a Live Demo
Experience the most intuitive, clinically robust EHR designed for behavioral health professionals—built to streamline documentation, improve compliance, and enhance patient care.
- Simplify clinical charting
- Stay organized with appointment scheduling
- Reduce no-shows with automated reminders
- Improve client engagement with a secure patient portal
- Provide flexible care with HIPAA-compliant telehealth
Simplify clinical charting
Stay organized with appointment scheduling
Reduce no-shows with automated reminders
Improve client engagement with a secure patient portal
Provide flexible care with HIPAA-compliant telehealth
Frequently Asked Questions About Mental Health Notes
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







