Blog > Documentation > Case Management Notes: Examples, Templates & Best Practices
How to Write an Effective Case Management Note (With Examples and Templates)
Writing effective case management notes is essential for tracking client progress, coordinating care, and ensuring documentation meets professional and legal standards. This comprehensive guide covers everything case managers and social workers need to know — from choosing the right note format (SOAP, DAP, BIRP) to documenting treatment plan progress and protecting client privacy in sensitive cases. You’ll find detailed case management notes examples and a downloadable case management notes checklist for easy reference.

Last Updated: March 18, 2026


What You'll Learn
- How to write clear, compliant case management notes using structured templates and real-world examples
- The essential components every case management note must include to support audits, billing, and continuity of care
- Best practices for writing objective, defensible, and privacy-conscious clinical documentation
- Common documentation mistakes (and how to fix them) to improve clarity and reduce audit risk
- Real-world case management note examples across multiple settings and formats (SOAP, DAP, BIRP, GIRP, PIRP)
Whether you're a social worker documenting a home visit, a mental health clinician tracking progress, or a case manager coordinating care across agencies, case management notes are the backbone of quality service delivery. This guide covers everything you need: what case management notes are, how to write them effectively, real-world examples across settings, free templates, and note format guidance for SOAP, DAP, BIRP, and GIRP documentation.
What Are Case Management Notes?
A case management note is a written record that documents a case manager’s interaction with a client. These notes serve multiple essential functions:
- Ensuring continuity of care across providers and shifts
- Tracking a client’s progress toward treatment goals
- Supporting accountability in multidisciplinary teams
- Justifying services for insurance reimbursement
- Providing legally defensible documentation in audits or court proceedings
- Coordinating referrals, resources, and follow-up actions
In mental health and social work, case management notes also carry clinical, operational, and ethical weight. A well-written note protects both the client and the clinician.
How to Write Case Management Notes: Step-by-Step
Effective case management notes share six core qualities: they are accurate, complete, clear, concise, timely, and objective. Here is how to achieve each in practice.
1. Complete Notes the Same Day
Write notes as soon as possible after client contact — ideally the same day. Memory fades quickly, and delayed notes introduce inaccuracies that can affect clinical decisions, billing, and legal standing. Block dedicated documentation time into your daily schedule and treat it as a non-negotiable part of case management.
2. Include All Required Identifying Information
Every note must include:
- Client full name and date of birth
- Medical record number or case ID
- Date and time of contact
- Type of contact (in-person, phone, telehealth, collateral)
- Clinician name, title, and credentials
- Signature and date of completion
3. Use Objective, Behavioral Language
Write in the third person and stick to observable facts. Avoid vague or judgmental language.
| ❌ Avoid | ✅ Use Instead |
|---|---|
| Client is doing better. | Client attended 3 of 3 scheduled sessions this week and reported reduced anxiety symptoms. |
| Client seems lazy. | Client reported difficulty completing household tasks due to ongoing fatigue. |
| Client is non-compliant. | Client did not attend scheduled appointment; reported transportation as a barrier. |
| Client appeared angry and frustrated. | Client raised voice during session and stated, “I feel like no one is listening to me.” |
| Pt. super stressed RN. | Client expressed high stress related to current housing instability. |
4. Align Notes with Treatment Plan Goals
Each note should tie the session or contact back to a specific goal or objective in the client’s treatment plan. For example, if a goal is ‘secure stable housing within 90 days,’ your note should reference the specific steps taken toward that goal: outreach made, applications submitted, barriers encountered, and next steps planned. By aligning notes with specific objectives, you create a clear record of how services provided support the client’s broader treatment plan, while also demonstrating accountability and progress over time.
5. Be Clear, Concise, and Organized
More is not always better. Focus on clinically relevant information and avoid lengthy narratives that bury the key details. Use a consistent note format (SOAP, DAP, BIRP, or GIRP) to create predictable, scannable documentation. Organize notes chronologically with the most recent contact appearing first.
6. Protect Client Privacy
Follow HIPAA, 42 CFR Part 2 (for substance use), and applicable state laws. Practical steps:
- Limit detail to what is clinically necessary
- Use non-identifying references for third parties (e.g., ‘partner,’ ‘family member’)
- Document sensitive topics (DV, immigration, legal) only when directly relevant to care
- Write as if the note may be reviewed in a legal or audit setting
- Consult your supervisor before including high-risk content
Free Download: Case Management Note Checklist
Download our free Case Management Note Checklist to ensure every note you write is clear, compliant, and aligned with your client’s goals—perfect for busy social workers who want stronger outcomes in less time.

Case Management Note Formats: SOAP, DAP, BIRP, GIRP, and PIRP
Different settings call for different documentation structures. Here is a quick guide to the most widely used formats, with a case management note example for each.
Related: PIRP vs GIRP vs BIRP Notes
Case Management Note Formats
Choose the structure that best fits your workflow, documentation requirements, and clinical setting.
| Format | Stands For | Best Used For | Ideal Setting |
|---|---|---|---|
| SOAP | Subjective, Objective, Assessment, Plan | Separating observed facts from clinical judgment | Mental health, medical case management, hospital discharge |
| DAP | Data, Assessment, Plan | Brief, facts-forward contacts | Outreach, check-ins, community services |
| BIRP | Behavior, Intervention, Response, Plan | Tracking observable behaviors and service outcomes | Community social work, substance use, advocacy |
| GIRP | Goal, Intervention, Response, Plan | Linking each contact to a treatment goal | Housing, employment, elder care, benefits navigation |
| PIRP | Problem, Intervention, Response, Plan | Effective for issue-focused updates (transportation barriers, missed appointments, paperwork hurdles) with clear actions and follow-up | Crisis follow-up, complex cases with multiple barriers |
Case Management Notes Examples
The following case management note examples illustrate how each format works across different practice settings. Use these as a reference when building your own documentation.
Social work case notes often document more than clinical care. Case managers working in social services may be coordinating across school, housing, court, and child welfare systems simultaneously — which makes documentation especially important.
Key considerations unique to social work documentation:
- Multidisciplinary collaboration: Notes may be read by educators, housing coordinators, attorneys, or child welfare workers. Write for a broad professional audience.
- Cultural sensitivity: Use inclusive, person-first language. Avoid cultural assumptions or stereotypes in your descriptions of client behavior.
- Strengths-based framing: Where appropriate, document the client’s resources, resilience, and progress alongside challenges.
- Advocacy and services rendered: Document not just clinical interventions but advocacy efforts, referrals made, and community resources connected.
- Legal exposure: Social work notes are more likely than clinical notes to be subpoenaed in family court, custody, or child protective proceedings. Write accordingly.
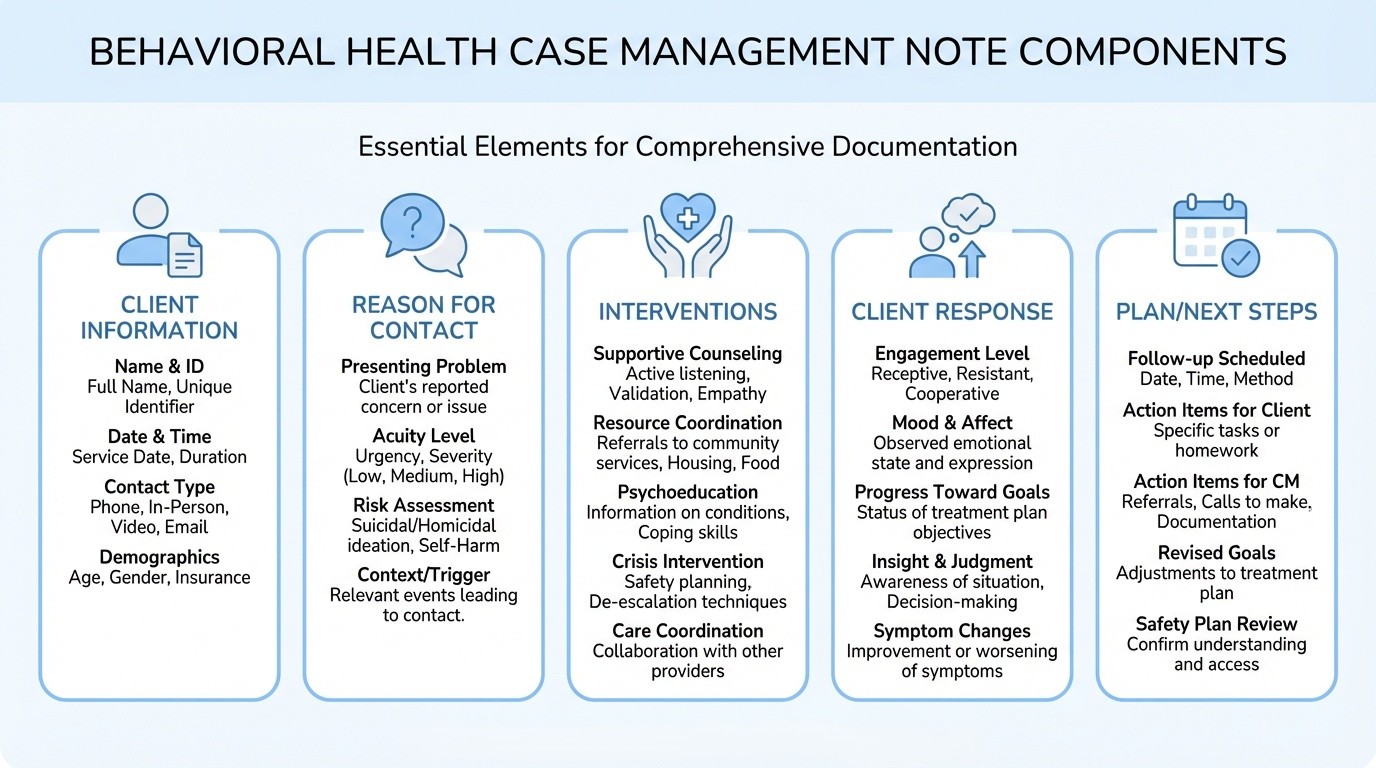
Case Management Notes Template: Key Components
Regardless of the format you use, a complete case management note template should include the following components. Use this as a checklist when reviewing your documentation.
Common Case Management Documentation Errors
Even experienced case managers can fall into documentation habits that create clinical, legal, or compliance risk. Here are the most common errors and how to correct them:
Frequently Asked Questions About Social Work Case Management Notes
Technology and Software for Case Management Notes
Documentation doesn’t have to be a burden. Modern case management EHR software like ICANotes streamlines documentation and helps you stay compliant with behavioral health standards.
Related: What is Case Management Software and Why Do I Need It?
Key features that improve documentation efficiency:
- Menu-driven note templates pre-built for case management, social work, and behavioral health
- Auto-populated client demographics and treatment plan goals in each note
- Integrated scheduling, billing, and secure messaging
- Patient portal for online intake, forms, and history
- Secure telehealth built into the documentation workflow
- Audit-ready structure that meets HIPAA, CARF, and Joint Commission requirements
Whether you’re writing case notes in social work, outpatient mental health, or community-based care, the right software can help you complete a case management note in 3 minutes or less. Book a demo or sign up for a free 30-day trial below.
Start Your 30-Day Free Trial
Experience the most intuitive, clinically robust EHR designed for behavioral health professionals, built to streamline documentation, improve compliance, and enhance patient care.
- Complete Notes in Minutes - Purpose-built for behavioral health charting
- Always Audit-Ready – Structured documentation that meets payer requirements
- Keep Your Schedule Full – Automated reminders reduce costly no-shows
- Engage Clients Seamlessly – Secure portal for forms, messages, and payments
- HIPAA-Compliant Telehealth built into your workflow

Related Posts
Donald Morrison graduated from UNC Charlotte in 2004. He has since worked as a school-based therapist, inpatient social work supervisor and outpatient clinician. Donald currently works in private practice, and he is also an adjunct faculty member at the UNC Charlotte School of Social Work. In addition, Donald serves as a clinical supervisor to LCSW associates, and he regularly presents at area mental health conferences and seminars.









Case Notes in Social Work: Unique Considerations