Blog > Documentation > Depression SOAP Note Example + 6 Copy-Ready Templates
Depression SOAP Note Example + 6 Copy-Ready Templates for Clinicians
Writing accurate, clinically sound SOAP notes for depression is essential for documenting severity, supporting medical necessity, and ensuring continuity of care. In this guide, you’ll find real-world depression SOAP note examples — including major depressive disorder (MDD), suicidal ideation, and comorbid presentations — along with step-by-step guidance on how to structure each section effectively. Whether you’re a therapist, psychiatrist, or behavioral health clinician, this resource will help you improve your documentation, reduce audit risk, and write clearer, more defensible notes in less time.

Last Updated: April 16, 2026


What You'll Learn
- How to write a depression SOAP note step-by-step (Subjective, Objective, Assessment, Plan)
- What to include when documenting major depressive disorder (MDD) and symptom severity
- How to properly document suicidal ideation, risk level, and safety considerations
- The key differences between strong vs weak depression SOAP notes
- How to use real-world examples to improve your clinical documentation
- Tips for supporting medical necessity and passing audits with better notes
A depression SOAP note needs to do more than record that a patient feels sad. To meet clinical standards, support medical necessity, and withstand payer scrutiny, your documentation must capture symptom severity, functional impairment, risk factors, diagnostic reasoning, and a treatment plan that reflects measurable clinical thinking.
Whether you’re documenting a first episode of major depressive disorder, a medication adjustment visit, or a session involving passive suicidal ideation, the quality of your SOAP note directly affects reimbursement, continuity of care, and legal protection.
This guide walks you through each section of a depression SOAP note step by step and provides six copy-ready depression SOAP note examples you can adapt for your own clinical documentation.
What is a Depression SOAP Note?
A SOAP note is a standardized clinical documentation format that organizes session information into four sections: Subjective, Objective, Assessment, and Plan. When used for depression-related encounters, the SOAP structure ensures clinicians capture the full scope of the patient’s presentation — from their self-reported mood and functional difficulties to the clinician’s diagnostic formulation and treatment decisions.
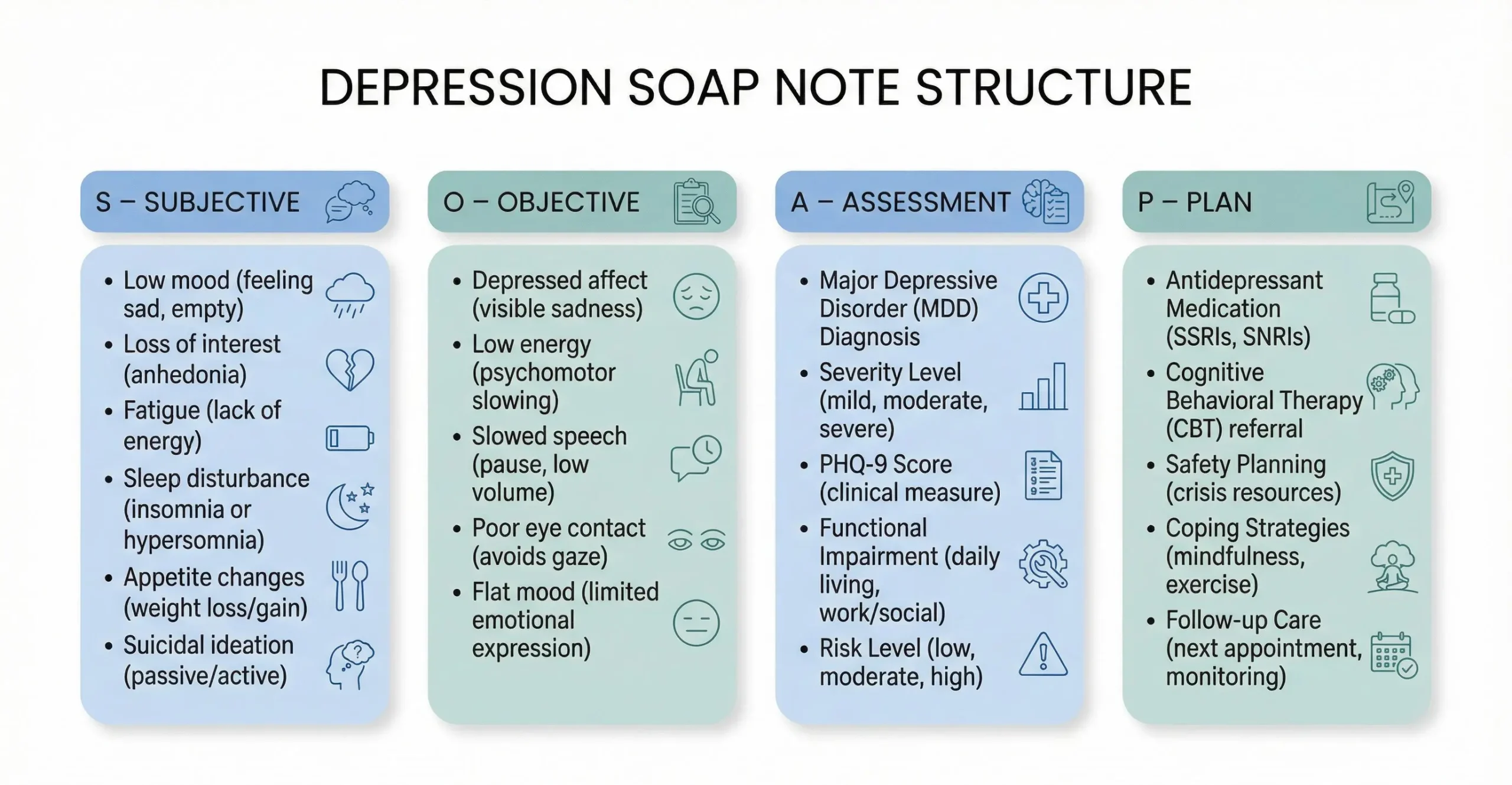
Subjective (S)
What the patient reports — mood, sleep, appetite, energy, concentration, motivation, anhedonia, medication side effects, and safety screening responses.
Objective (O)
What the clinician directly observes during the session, including mental status exam findings such as appearance, psychomotor activity, speech, affect, thought process, and insight/judgment./p>
Assessment (A)
The clinician’s diagnostic impression, severity classification, symptom trajectory, functional impact, risk level, and treatment response.
Plan (P)
Medication management, therapeutic interventions, safety planning, referrals, monitoring strategies, and follow-up scheduling.
The emphasis within each section can shift depending on the clinician’s role. A psychiatrist’s depression SOAP note may focus heavily on medication efficacy, lab monitoring, and biological symptoms, while a therapist’s note will center on session themes, therapeutic interventions, coping skill development, and psychosocial factors. The SOAP format accommodates both clinical perspectives.

Write Better Depression SOAP Notes With More Clarity and Less Stress
Download our free Mental Health SOAP Notes Guide to improve your depression documentation with real-world examples, stronger clinical language, and guidance for documenting severity, risk, and treatment planning.
- How to document mood, anhedonia, sleep, appetite, and functional impairment
- Best practices for documenting suicidal ideation and risk level clearly
- SOAP note examples and templates for MDD and complex presentations
- Tips to support medical necessity, compliance, and faster documentation
Get the guide instantly and start writing stronger depression SOAP notes today.
How to Write a Depression SOAP Note (Step by Step)
The following breakdown covers what to include in each section of a depression SOAP note, with specific clinical language that supports both treatment planning and documentation compliance.
Step 1: Subjective — What the Patient Reports
The Subjective section captures the patient’s reported experience of depressive symptoms, including emotional state, physical symptoms, and functional impact. This section should reflect the patient’s voice and clearly document severity and progression.
- Mood description (e.g., “low,” “empty,” “hopeless,” “numb,” or “overwhelmed”)
- Loss of interest or pleasure in previously enjoyed activities (anhedonia)
- Sleep disturbances, including insomnia, hypersomnia, early waking, or difficulty falling asleep
- Appetite changes, including decreased appetite or emotional eating, with or without weight changes
- Fatigue, low energy, reduced stamina for routine activities, difficulty getting out of bed, or feelings of physical heaviness
- Difficulty concentrating, making decisions, or maintaining focus at work or home
- Feelings of guilt, worthlessness, hopelessness, or excessive self-criticism
- Functional impairment affecting work, school, relationships, or daily routines
- Medication adherence: missed doses, side effects, concerns about treatment
- Suicidal ideation, passive death wishes, self-harm thoughts, or other safety concerns
Strong Depression Subjective Sections Often Include
Tip: Use direct quotes when possible. Statements like “I don’t see the point in anything anymore” provide stronger clinical clarity than general summaries.
Step 2: Objective — What the Clinician Observes
The Objective section includes observable findings from the mental status exam and clinical interaction. This should reflect clinician observation rather than patient self-report.
- Appearance: Hygiene, grooming, attire. Note changes from baseline (e.g., unkempt appearance in a patient who is typically well-groomed)
- Behavioral and psychomotor activity: psychomotor retardation or agitation (note eye contact and engagement level)
- Speech: rate, volume, tone, and spontaneity. Depression often presents with slow, soft, or monotone speech with reduced verbal output.
- Affect (flat, constricted, tearful, or blunted)
- Observed mood and congruence with reported mood
- Thought process: Linear, circumstantial or slowed. Note rumination, negativistic thinking patterns, or poverty of thought.
- Thought content: hopelessness, worthlessness, guilt, self-critical thinking, death wishes, or suicidal ideation
- Insight into depressive symptoms: does the patient recognize their symptoms as depression?
- Judgment and decision-making capacity: is the patient making reasonable treatment decisions?
Strong Depression Objective Sections Often Include
Tip: Avoid repeating what the patient said in the Subjective section. Focus on what you directly observe, including behavior, affect, and clinical presentation.
Step 3: Assessment — Clinical Impression and Severity
The Assessment synthesizes subjective and objective findings into a diagnosis, severity rating, and clinical interpretation.
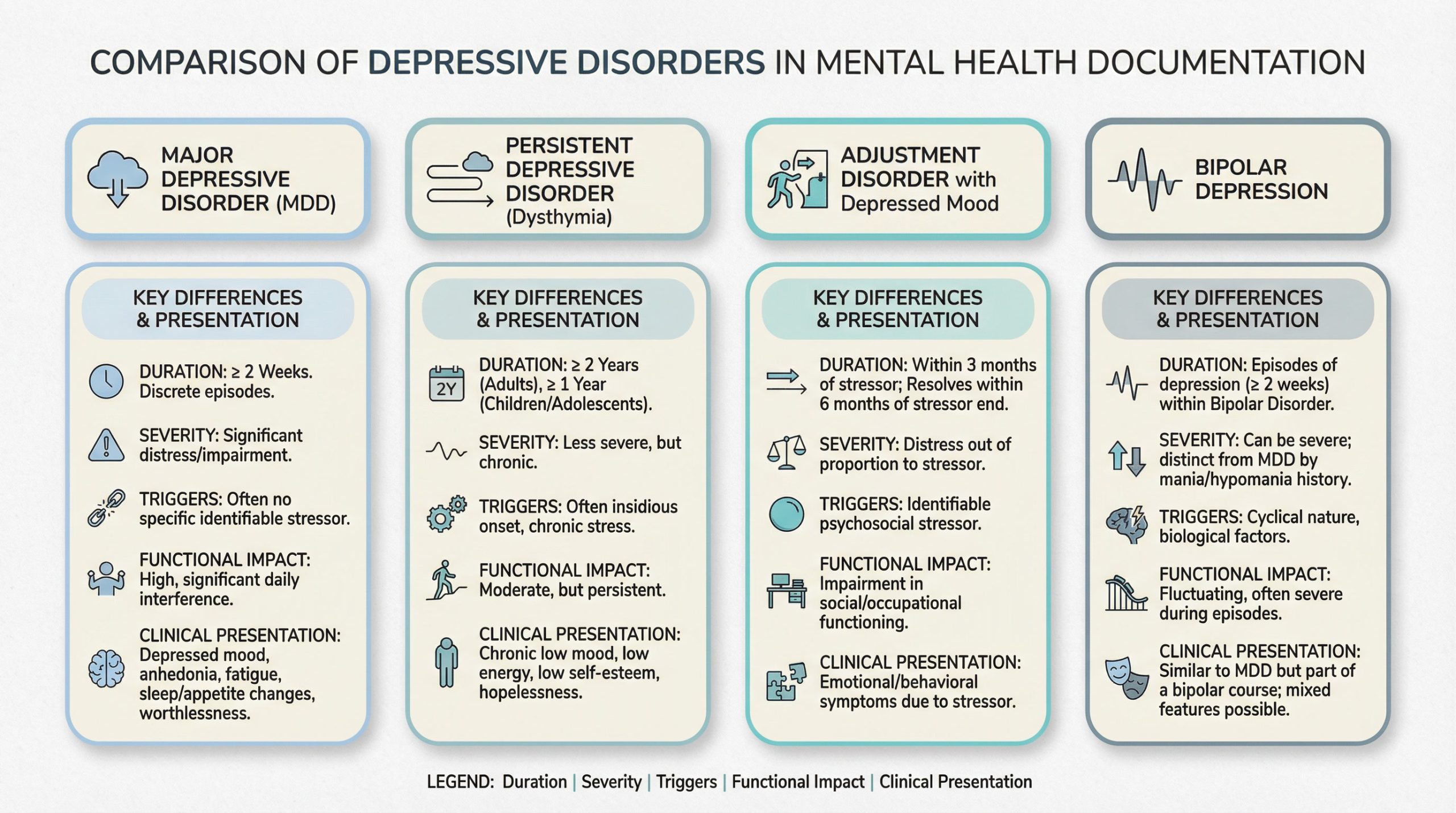
- Diagnosis: Use ICD-10 codes. Common depression diagnoses include Major Depressive Disorder, single episode (F32.0–F32.9) or recurrent (F33.0–F33.9), Persistent Depressive Disorder (F34.1), and Adjustment Disorder with depressed mood (F43.21).
- Severity: Mild, moderate, or severe, with or without psychotic features. Reference standardized measure scores (PHQ-9, BDI-II, Columbia Suicide Severity Rating Scale) to support your classification.
- Symptom progression: Is the patient improving, stable, or worsening compared to the previous session or baseline? Quantify where possible.
- Functional impairment: Specify domains affected — occupational, social, academic, self-care, or parenting.
- Risk level (low, moderate, or high) based on suicidal ideation or other safety concerns. State your rationale including protective and risk factors.
- Treatment response or symptom progression since last visit
Strong Depression Assessments Often Include
Tip: Use measurable data like PHQ-9 score changes over time to demonstrate progress and support medical necessity in audits.
Step 4: Plan — Next Steps in Treatment
The Plan outlines specific next steps in treatment and should clearly document interventions and follow-up care. A strong Plan section demonstrates active clinical reasoning and supports payer authorization.
- Medication management: Current medications with dosages, changes made (titrations, additions, discontinuations), rationale for changes, and monitoring needs (labs, vital signs, side effect checks).
- Therapeutic interventions: Specific modalities used or recommended—CBT, behavioral activation, IPT, DBT skills, ACT, psychoeducation, or supportive therapy. Note session focus.
- Safety planning: If suicidal ideation is present, document the safety plan in detail: warning signs, coping strategies, social supports, emergency contacts, means restriction, and crisis resources provided.
- Coping strategies or behavioral assignments
- Referrals: Psychiatry, primary care, lab work, intensive outpatient, group therapy, or social services.
- Follow-up: Next appointment date, session frequency, and between-session assignments or monitoring tasks.
Strong Depression Plans Often Include
Tip: Avoid vague plans like “continue therapy.” Specify interventions, skills, medications, and follow-up timing to clearly demonstrate clinical decision-making.
Depression SOAP Note Examples & Templates
Below are six depression SOAP note examples covering a range of clinical presentations and severity levels. Each is formatted in standard SOAP structure with copy-ready language you can adapt for your own documentation.
1. Moderate Major Depressive Disorder SOAP Note Example
Patient is a 42-year-old female presenting for a follow-up therapy session. She reports persistent low mood over the past two weeks, describing her mood as “flat” and “empty.” She endorses difficulty falling asleep (lying awake 1–2 hours most nights), decreased appetite with unintentional weight loss of approximately 5 pounds over the past month, fatigue that makes routine household tasks feel overwhelming, and difficulty concentrating at work. She reports reduced interest in socializing and has declined invitations from friends over the past three weeks. She continues to attend work but describes her performance as “going through the motions.” She is adherent to sertraline 100 mg daily and reports mild nausea that has improved since initiation. She denies suicidal ideation, self-harm urges, and homicidal ideation. PHQ-9 completed: score of 14.
Patient is appropriately dressed but appears fatigued, with slowed movements and reduced facial expressiveness. Eye contact is intermittent. Speech is soft and reduced in spontaneity, with longer-than-usual pauses before responding. Mood is “empty.” Affect is flat and constricted, with brief tearfulness when discussing social withdrawal. Thought process is linear but slowed, with ruminative themes centered on self-criticism and perceived inadequacy. Thought content includes feelings of worthlessness (“I’m letting everyone down”) but no suicidal ideation, hallucinations, or delusions. Psychomotor retardation is noted. Insight is fair—she recognizes her symptoms as depression. Judgment is intact.
Major Depressive Disorder, single episode, moderate (F32.1). PHQ-9 score of 14 is consistent with moderate severity, decreased from 18 at intake, indicating partial treatment response. Depression continues to impair occupational functioning (reduced concentration, diminished performance) and social engagement (withdrawal from peer relationships). Neurovegetative symptoms (insomnia, appetite loss, fatigue) persist. No acute safety concerns. Risk level: low.
Continue sertraline 100 mg daily. Continue weekly CBT with focus on behavioral activation to address social withdrawal and anhedonia. This session: reviewed activity scheduling and identified three low-effort social activities patient is willing to attempt this week. Introduced cognitive restructuring targeting core belief “I’m a burden to others.” Assigned mood and activity log for between-session tracking. Discuss possible sertraline dose increase at next session if PHQ-9 remains above 10. Follow-up in one week.
2. Mild Depression Follow-Up SOAP Note Example
Patient is a 29-year-old male presenting for a follow-up therapy session. He reports his mood has been “a little better this week” and notes improved motivation to complete daily tasks. He returned to his gym routine twice this week after a three-week absence. Sleep has improved—he is falling asleep within 30 minutes and sleeping approximately 6.5 hours per night, up from 5 hours at his last session. He reports persistent low-grade fatigue in the afternoons and occasional difficulty concentrating at work but describes these as “manageable.” Appetite has normalized. He is adherent to bupropion 150 mg daily and denies side effects. He denies suicidal ideation, self-harm urges, and homicidal ideation. PHQ-9 completed: score of 7.
Patient is well-groomed and casually dressed. He presents with improved affect compared to the previous session—more spontaneous smiling and increased verbal output. Eye contact is consistent. Speech is normal in rate, volume, and tone. Mood is “better.” Affect is mildly constricted but reactive, brightening when discussing gym attendance. Thought process is linear and goal-directed. Thought content is future-oriented, with some residual self-doubt about work performance but less pervasive than in previous sessions. No psychomotor abnormalities. Insight and judgment are good.
Major Depressive Disorder, single episode, mild (F32.0). PHQ-9 score of 7 reflects continued improvement from 14 at intake and 10 at last session. Patient is demonstrating meaningful gains in behavioral activation (exercise, daily task completion) and sleep quality. Residual symptoms of fatigue and mild concentration difficulty persist but are not significantly impairing functioning. No safety concerns. Risk level: low.
Continue bupropion 150 mg daily. Continue biweekly CBT. This session: reviewed behavioral activation progress and reinforced return to exercise as a mood-congruent activity. Explored residual cognitive distortions related to work performance using a thought record. Assigned continued mood logging and one additional pleasurable activity per week. Transition to biweekly sessions if PHQ-9 remains below 10 at next visit. Follow-up in two weeks.
3. Severe Depression With Passive Suicidal Ideation SOAP Note Example
Patient is a 51-year-old male presenting for a follow-up psychiatric appointment. He reports worsening depression over the past three weeks following a marital separation. He describes his mood as “hopeless” and states, “I don’t see the point anymore.” He endorses pervasive anhedonia, hypersomnia (sleeping 12–14 hours per day), significantly decreased appetite with 8-pound weight loss over the past month, profound fatigue, difficulty with basic self-care (reports not showering for several days), and feelings of worthlessness and guilt. He reports passive suicidal ideation, stating, “Sometimes I think everyone would be better off without me,” but denies active intent, plan, or access to means. He identifies his two children as protective factors. He has not attended his therapy appointments for the past two weeks. He is partially adherent to duloxetine 60 mg daily, reporting missed doses 2–3 times per week. He denies alcohol or substance use.
Patient appears disheveled and fatigued. Hair is unkempt, and he is wearing the same clothes as his last visit. Psychomotor retardation is prominent—slow gait, delayed response latency, minimal gestures. Eye contact is poor. Speech is slow, soft, and monotone with markedly reduced spontaneity. Mood is “hopeless.” Affect is flat with intermittent tearfulness. Thought process is linear but impoverished, with long pauses and brief responses. Thought content includes hopelessness, worthlessness, excessive guilt about the separation, and passive death wishes. He denies auditory or visual hallucinations and denies homicidal ideation. Insight is limited—he questions whether treatment can help. Judgment is impaired by hopelessness and medication nonadherence. PHQ-9 score: 23 (severe). C-SSRS: passive ideation without intent or plan.
Major Depressive Disorder, recurrent, severe, without psychotic features (F33.2). PHQ-9 score of 23 indicates severe depression, increased from 16 at last visit. Acute exacerbation likely precipitated by marital separation. Passive suicidal ideation is present without intent, plan, or access to lethal means. Protective factors include his relationship with his children and absence of substance use. Neurovegetative symptoms are significant (hypersomnia, appetite loss, self-care decline). Medication nonadherence is contributing to symptom worsening. Functional impairment is severe across all domains. Risk level: moderate.
Increase duloxetine to 90 mg daily. Strongly reinforced importance of daily medication adherence; problem-solved barriers (patient will set daily phone alarm). Safety plan reviewed and updated: warning signs (withdrawal, hopelessness increasing), coping strategies (calling his brother, walking, journaling), emergency contacts (brother, 988 Suicide and Crisis Lifeline), and means restriction discussed (patient confirms no firearms in the home). Crisis resources provided in writing. Coordinated with therapist to resume weekly therapy sessions. Shortened follow-up interval to one week for close monitoring. If symptoms worsen or suicidal ideation becomes active, patient instructed to present to the nearest emergency department or call 988. Patient verbalized understanding and agreement with the plan.
4. Depression Medication Adjustment Visit SOAP Note Example
Patient is a 36-year-old female presenting for a six-week medication follow-up. She was started on escitalopram 10 mg daily for major depressive disorder at her last visit. She reports partial improvement in mood, stating, “The really dark days are less frequent, but I still don’t feel like myself.” She describes ongoing low energy, difficulty initiating tasks, and anhedonia—noting that she has stopped reading, which was previously her primary hobby. Sleep has improved (now averaging 6–7 hours, up from 4–5 hours). Appetite is stable. She reports mild initial nausea that resolved after the first two weeks and mild sexual dysfunction (decreased libido) that she describes as “annoying but manageable.” She is fully adherent to her medication. She denies suicidal ideation, self-harm urges, and homicidal ideation. PHQ-9 completed: score of 11.
Patient is well-groomed and cooperative. She appears less fatigued than at her previous visit but retains a subdued quality. Eye contact is adequate. Speech is normal in rate and volume, with slightly reduced prosody. Mood is “meh.” Affect is mildly blunted but reactive, with appropriate smiling when discussing her cat. Thought process is linear and coherent. Thought content includes frustration with slow progress and residual self-critical themes, but without hopelessness. No perceptual disturbances. No psychomotor abnormalities. Insight is good. Judgment is intact. Vitals: BP 118/74, HR 68.
Major Depressive Disorder, single episode, moderate (F32.1). PHQ-9 score of 11, decreased from 17 at baseline, indicating partial response to escitalopram 10 mg. Sleep has improved, but anhedonia, low energy, and task initiation remain impaired. Sexual dysfunction is present as a mild side effect. Current dose may be subtherapeutic for full remission. No safety concerns. Risk level: low.
Increase escitalopram to 15 mg daily, with plan to increase to 20 mg in four weeks if residual symptoms persist and side effects remain tolerable. Discussed sexual dysfunction: patient prefers to continue current medication and monitor rather than switch. Recommended behavioral activation strategies to address anhedonia (schedule one pleasurable activity per day). Encouraged continued reading habit—starting with 10 minutes per day as a low-barrier reintroduction. Lab work ordered: TSH, CBC, CMP to rule out contributing medical factors. Follow-up in four weeks to reassess treatment response. Patient agrees with the plan.
5. Recurrent Major Depressive Disorder With Anxiety Features SOAP Note Example
Patient is a 47-year-old female presenting for a follow-up therapy session. She has a history of three prior depressive episodes. She reports her depression has “crept back” over the past month, coinciding with increased work stress and her mother’s declining health. She describes low mood most days, pervasive worry about her mother’s care needs, restlessness, irritability with her spouse and coworkers, difficulty concentrating, and a sense of being “overwhelmed by everything.” She reports middle insomnia (waking at 2–3 AM with racing thoughts and unable to return to sleep), reduced appetite, and withdrawal from her weekly book club. She is adherent to venlafaxine 150 mg daily and trazodone 50 mg at bedtime. She denies suicidal ideation, self-harm urges, and homicidal ideation. PHQ-9: 16. GAD-7: 13.
Patient is well-groomed but appears tense and fatigued. She is fidgeting in her chair and shifts position frequently. Eye contact is adequate. Speech is normal in rate but becomes rapid and pressured when discussing her mother’s health. Mood is “anxious and down.” Affect is dysphoric and anxious, congruent with stated mood. Thought process is linear but ruminative, toggling between depressive themes (guilt, inadequacy) and anxious themes (catastrophic worry about her mother). Thought content includes self-blame (“I should be doing more for her”) and anticipatory worry. No perceptual disturbances. Insight is good. Judgment is intact.
Major Depressive Disorder, recurrent, moderate, with anxious distress (F33.1). PHQ-9 of 16 and GAD-7 of 13 reflect moderate depression and moderate anxiety, consistent with the anxious distress specifier. Current episode appears precipitated by psychosocial stressors (occupational and caregiver burden). Anxiety and depressive symptoms are interacting—worry is disrupting sleep, and sleep deprivation is worsening mood and concentration. Functional impairment includes occupational irritability, social withdrawal, and disrupted sleep. No safety concerns. Risk level: low.
Continue venlafaxine 150 mg daily. Increase trazodone to 100 mg at bedtime to address middle insomnia. Continue weekly therapy. This session: identified the interaction between worry and sleep disruption as a treatment target. Introduced worry postponement technique (scheduled 15-minute worry window). Practiced cognitive restructuring targeting guilt-based beliefs about caregiving. Discussed referral to a caregiver support group. Assigned worry log and sleep diary for between-session monitoring. Follow-up next week. Consider venlafaxine increase to 225 mg if mood does not improve over the next two to three sessions.
6. Depression in an Adolescent SOAP Note Example
Patient is a 16-year-old male brought in by his mother for a follow-up therapy session. Mother reports the patient has been increasingly withdrawn at home, spending most of his time in his room and showing little interest in activities he previously enjoyed, including basketball and video gaming with friends. Patient describes his mood as “I don’t really feel anything.” He endorses difficulty concentrating in school, with a drop in grades from Bs to Ds this quarter. He reports hypersomnia (sleeping 11–12 hours on weekends), decreased appetite, and persistent fatigue. He denies substance use. When asked directly about suicidal thoughts, he states, “I’ve thought about it, like, what if I just wasn’t here, but I wouldn’t actually do anything.” He denies intent, plan, or prior self-harm. He identifies his mother and his dog as reasons to stay safe. He is not currently on medication.
Patient is dressed in a hoodie with the hood partially up. Grooming is adequate. He sits slumped in the chair with minimal movement. Eye contact is poor—directed mostly at the floor. Speech is slow, low in volume, and limited to brief responses. Mood is “nothing.” Affect is flat with no emotional variability throughout the session. Thought process is linear but impoverished. Thought content includes anhedonia, feelings of emptiness, and passive death wishes as described. No auditory or visual hallucinations. No homicidal ideation. Psychomotor retardation is present. Insight is limited—he does not fully attribute his symptoms to depression. Judgment is fair. PHQ-A score: 18 (moderately severe). C-SSRS: passive ideation without intent or plan.
Major Depressive Disorder, single episode, moderately severe (F32.2). PHQ-A score of 18 indicates moderately severe depression. Passive suicidal ideation is present without intent, plan, or prior self-harm. Protective factors include a supportive parent relationship and an identified reason for living. Depression is significantly impairing academic performance, social functioning, and daily activity engagement. Patient’s limited insight may reduce treatment engagement and warrants motivational strategies. No imminent safety concerns, but passive ideation requires close monitoring. Risk level: moderate.
Initiate weekly individual CBT with behavioral activation focus. This session: established rapport and psychoeducation about depression provided to both patient and mother. Developed initial safety plan with patient: warning signs (increased isolation, thoughts of “disappearing”), coping strategies (playing with dog, listening to music, shooting basketball outside), people to contact (mother, school counselor), crisis resources (988 Suicide and Crisis Lifeline). Mother given copy of safety plan. Referred to psychiatry for medication evaluation given symptom severity. Coordinated with school counselor regarding academic accommodations. Assigned brief mood check-in journal (rating mood 1–10 daily). Follow-up in one week. Mother instructed to contact the office or present to the ER if suicidal ideation worsens.
Risk Assessment Language for Depression SOAP Notes
Thorough safety documentation is one of the most important elements of a depression SOAP note. Even when a patient denies suicidal ideation, documenting that the screening was performed — and what the patient’s response was — demonstrates clinical diligence. Below are copy-ready phrases organized by risk level:
Low Risk (Denies Suicidal Ideation)
- Patient denies suicidal ideation, intent, or plan. Denies self-harm urges. Denies homicidal ideation.
- Safety screening performed using PHQ-9 item 9; patient endorsed “not at all.”
- No imminent safety concerns identified. Risk level assessed as low.
- Patient identifies multiple protective factors, including [family, employment, faith, pets].
Moderate Risk (Passive Ideation Without Intent)
- Patient endorses passive suicidal ideation, stating [direct quote]. Denies active intent, plan, or access to lethal means.
- C-SSRS administered: passive ideation present; no preparatory behavior or prior attempts reported.
- Protective factors include [specific factors]. Risk factors include [specific factors].

- Safety plan reviewed and updated. Emergency contacts confirmed. Crisis resources provided (988 Suicide and Crisis Lifeline, local crisis line).
- Follow-up interval shortened to [timeframe] for closer monitoring.
Higher Risk (Active Ideation or Escalating Concerns)
- Patient endorses active suicidal ideation with [vague/specific] plan. [Intent/no intent] expressed. [Access to means confirmed/denied].
- Means restriction discussed. Patient [agreed to/declined] removal of [specific means] from the home.
- Higher level of care evaluated. [Voluntary hospitalization recommended/patient declined/safety plan intensified as alternative].
- Collateral contact made with [family member/emergency contact] with patient’s consent.
- Patient instructed to present to nearest emergency department or call 988 if ideation intensifies.
Always document the specific screening tool used, the patient’s response, your clinical reasoning about risk level, and the steps taken in response. Payers and auditors expect to see that safety was actively assessed and addressed — not assumed.
Tip: If suicidal ideation is present, always document a clear safety plan. Not sure what to include? Review our guide on creating an effective safety plan for step-by-step guidance.
Common Mistakes in SOAP Notes for Depression
Even experienced clinicians can develop documentation habits that weaken the clinical and legal value of their depression SOAP notes. Here are the most common pitfalls:
- Missing or insufficient safety documentation. Every depression SOAP note should document that a safety screening was performed and record the patient’s response — even when the answer is “no.” Omitting this creates a significant legal and clinical vulnerability.
- Vague mood description. “Patient reports feeling depressed” is not clinically specific enough. Document the quality, intensity, duration, and impact of the mood disturbance. Use the patient’s own words where possible.
- No functional impairment documented. Payers require evidence of functional impairment to authorize ongoing treatment. If your note does not explain how depression affects the patient’s work, relationships, self-care, or daily activities, it may not support medical necessity.
- Weak or generic Plan section. “Continue current treatment” does not demonstrate active clinical reasoning. Specify the intervention modality, therapeutic focus, medication changes, homework, safety planning updates, and follow-up timing.
- No measurable symptom tracking between sessions. Using standardized tools like the PHQ-9 at regular intervals and referencing score changes in the Assessment section demonstrates treatment progress (or justifies a treatment plan change) in a way that narrative alone cannot.
- Blurring Subjective and Objective sections. The Subjective section captures what the patient reports. The Objective section captures what the clinician observes. Restating self-reported symptoms in the Objective section undermines the structure and credibility of the note.
How ICANotes Helps You Write Better Depression SOAP Notes
Writing thorough, clinically sound depression SOAP notes can be time-consuming — especially when you’re trying to capture symptom severity, document suicidal ideation appropriately, and ensure your notes support medical necessity. ICANotes is designed specifically for behavioral health clinicians to streamline this process without sacrificing quality.
With ICANotes, you can create structured, compliant depression SOAP notes in a fraction of the time by using intelligent templates built around real clinical workflows.
Here’s how ICANotes supports better depression documentation:
- Pre-built SOAP note templates for depression
Quickly document major depressive disorder (MDD), recurrent depression, and complex presentations with templates that guide you through each section. - Clinically relevant prompts for symptom detail
Capture key depressive symptoms — mood, anhedonia, sleep, appetite, energy, and cognitive changes — without missing important details. - Integrated tools for documenting severity and risk
Easily include PHQ-9 scores, track changes over time, and document suicidal ideation, risk level, and safety planning in a structured, defensible way. - Streamlined mental status exam (MSE) documentation
Document observable findings like affect, speech, thought content, and psychomotor changes with just a few clicks. - Faster note-writing without sacrificing quality
Reduce time spent on documentation while still producing clear, complete, and audit-ready notes. - Built for behavioral health workflows
Designed specifically for therapists, psychiatrists, and other mental health clinicians — so your notes reflect how you actually practice.

Write Better Depression SOAP Notes in Less Time
ICANotes helps you document depression more efficiently with structured templates designed for major depressive disorder, suicidal ideation, and complex clinical presentations—so you can create clear, compliant, and audit-ready notes without the extra time.
- Guided templates for documenting MDD, severity, and symptom progression
- Built-in support for PHQ-9 scoring and tracking outcomes over time
- Structured fields for documenting suicidal ideation, risk level, and safety planning
- Faster note-writing with clinically complete, defensible documentation
- No credit card required
Start Your Free Trial
Complete the form below to try ICANotes free for 30 days.
Related Resources for Better SOAP Notes and Depression Documentation
Continue improving your clinical documentation with these related guides on depression assessment, treatment planning, and SOAP note best practices.
Frequently Asked Questions About Depression SOAP Notes
What should be included in a depression SOAP note?
A thorough depression SOAP note should include the patient’s self-reported mood and symptoms (Subjective), mental status exam findings (Objective), a diagnosis with severity classification and risk assessment (Assessment), and a specific treatment plan with medication details, therapeutic interventions, safety planning, and follow-up scheduling (Plan). Standardized measure scores like the PHQ-9 strengthen the note’s clinical and billing value.
How do you document suicidal ideation in a SOAP note?
Document suicidal ideation with specificity. In the Subjective section, include the patient’s own words about their experience. Note whether ideation is passive (“I wish I could go to sleep and not wake up”) or active (“I’ve been thinking about how I would do it”), and whether intent or a plan is present. Record the screening tool used (e.g., C-SSRS, PHQ-9 item 9). In the Assessment, classify the risk level with rationale. In the Plan, document the safety plan, means restriction discussion, crisis resources provided, follow-up interval, and any collateral contacts made.
How long should a depression SOAP note be?
There is no required length, but a well-written depression SOAP note typically ranges from one to two pages. It should be detailed enough to establish medical necessity, document risk assessment, and capture your clinical reasoning—but concise enough for practical use across a full caseload. Structured EHR templates designed for behavioral health can help clinicians produce comprehensive notes without adding time to each session.
What makes a SOAP note billable?
A billable SOAP note demonstrates medical necessity for the services provided. This means the note should document a diagnosis, symptom severity, functional impairment, a clear treatment plan, and clinical reasoning that connects the patient’s presentation to the interventions used. The note should also reflect the appropriate level of complexity for the CPT code billed. Vague or formulaic notes are the most common reason for claim denials and audit findings in behavioral health.
Recent Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.





