Blog > Treatment Strategies > Intergenerational Trauma: Examples, Symptoms & Healing Strategies
Intergenerational Trauma: Examples, Symptoms, and Healing Strategies
Intergenerational trauma — also called generational trauma or transgenerational trauma — occurs when the effects of unresolved trauma are passed from one generation to the next through family relationships, attachment patterns, learned behaviors, and even biological stress responses. This guide explores common examples of intergenerational trauma, signs and symptoms clinicians should recognize, the different types of generational trauma, and evidence-based therapy approaches that support long-term healing for individuals and families.

Last Updated: May 14, 2026


What You'll Learn
- What intergenerational trauma is and how trauma patterns are passed across generations
- Common examples of intergenerational trauma in families, relationships, and communities
- The major types of intergenerational trauma, including historical, attachment-based, and behavioral transmission
- Signs and symptoms of generational trauma in children, adolescents, and adults
- How unresolved trauma affects attachment, emotional regulation, relationships, and mental health
- How clinicians can assess intergenerational trauma during intake and ongoing therapy
- Evidence-based treatment approaches for healing intergenerational trauma, including CBT, DBT, EMDR, and family therapy
- How to break the intergenerational trauma cycle and support long-term healing across generations
- Practical strategies for documenting trauma-related care and treatment planning in behavioral health settings
- How the free Intergenerational Trauma Assessment Tool can support case conceptualization and trauma-informed care
Contents
- Examples of Intergenerational Trauma
- Types of Intergenerational Trauma
- The Intergenerational Trauma Cycle
- Signs and Symptoms of Intergenerational Trauma
- How to Assess Intergenerational Trauma
- Therapy and Treatment for Intergenerational Trauma
- How to Heal from Intergenerational Trauma: The Role of Family Therapy
- FAQ: Intergenerational Trauma
- How ICANotes Supports Clinicians Treatment Intergenerational Trauma
Intergenerational trauma — sometimes called transgenerational trauma or generational trauma — affects far more people than are aware of it. This form of trauma passes from one generation to the next, shaping mental health, relationships, and even physical wellbeing in ways that often go unrecognized for years. For behavioral health clinicians, understanding how to identify and treat intergenerational trauma is essential to providing whole-person, family-centered care. This guide covers the definition, real-world examples, types, symptoms, and evidence-based healing strategies clinicians need to know.
What is Intergenerational Trauma?
Quick Definition
Intergenerational trauma: The transmission of the effects of trauma from a person who directly experienced a traumatic event to their children, grandchildren, and beyond — through disrupted attachment, learned behavioral patterns, epigenetic changes, and shifts in family communication and functioning.
Intergenerational trauma refers to the way unresolved trauma experienced by one generation is transmitted — biologically, behaviorally, and psychologically — to subsequent generations, even when those descendants have never directly experienced the original traumatic event.
Consider two families across multiple generations. In the first, a parent experiences childhood sexual abuse. That trauma shapes how they attach to their own child during infancy and early childhood, potentially creating insecure attachment patterns. The parent may struggle with peripartum depression, anxiety, or PTSD symptoms that make consistent caregiving harder. Their child grows up absorbing those emotional patterns — not because of direct trauma, but because of the ripple effects of the parent's unhealed wound.
In the second family, there is no significant unresolved trauma. That family will still face distress and hardship, but without the layer of intergenerational trauma, they are in a stronger position to process and recover. The contrast illustrates how powerfully unresolved trauma can shape a family system across generations.
Examples of Intergenerational Trauma
Intergenerational trauma can arise from many different types of experiences. Understanding specific examples helps clinicians recognize these patterns in clinical settings and helps clients make sense of their own family histories.
Historical and Collective Trauma
Among the most-studied examples of intergenerational trauma are those rooted in collective historical events. Research on the descendants of Holocaust survivors, enslaved people, Indigenous populations impacted by forced removal, and war refugees has documented measurable psychological and even physiological differences that persist across generations. Children and grandchildren of survivors often show elevated rates of anxiety, depression, and PTSD — even without direct trauma exposure
Childhood Abuse Cycles
Perhaps the most commonly recognized form of intergenerational trauma is the cycle of abuse. A parent who was physically or emotionally abused as a child may — without therapeutic intervention — repeat similar patterns with their own children, not out of malice, but because those behaviors represent their only model of family life. sexual abuse, emotional neglect, and harsh discipline patterns can all propagate across generations in this way.
Substance Use Disorders
Families with multi-generational substance use disorders are a clear example of intergenerational trauma in action. A child raised in a home affected by parental addiction may experience chronic unpredictability, emotional neglect, and developmental disruption. Those experiences increase their own risk for substance use disorders later in life — creating a cycle that can span multiple generations without targeted intervention.
Attachment Disruption and Emotional Unavailability
Trauma frequently impairs a parent's capacity for emotional attunement. A parent numbed by unresolved grief, depression, or PTSD may be physically present but emotionally unavailable to their child. That child may then develop insecure or disorganized attachment styles, which in turn affect their own parenting capacity, relationships, and mental health — passing emotional unavailability forward even when the original trauma is never discussed.
Poverty and Economic Trauma
Chronic economic insecurity is both a stressor and a consequence of other forms of trauma. Families experiencing generational poverty often face compounding stressors — housing instability, inadequate healthcare access, community violence — that accumulate and affect developmental outcomes for children. Economic trauma can interact with other forms of intergenerational trauma to intensify its effects.
Types of Intergenerational Trauma
Clinicians and researchers have identified several distinct mechanisms through which intergenerational trauma operates. Understanding these types helps inform assessment and treatment planning.
Historical/Collective Trauma
Trauma originating from large-scale societal events — war, genocide, systemic oppression, and forced displacement — that affects entire communities across generations.
Familial Behavioral Transmission
Trauma-influenced parenting patterns, communication styles, and coping mechanisms that are modeled and learned by children, perpetuating dysfunction across generations.
Attachment-Based Transmission
Disrupted caregiver-child attachment resulting from a parent's unresolved trauma, leading to insecure attachment styles and emotional difficulties in the next generation.
Epigenetic Transmission
Emerging research suggests trauma can alter gene expression in ways that are passed biologically to offspring. While still evolving, this research suggests that the body itself may carry the imprint of ancestral trauma.
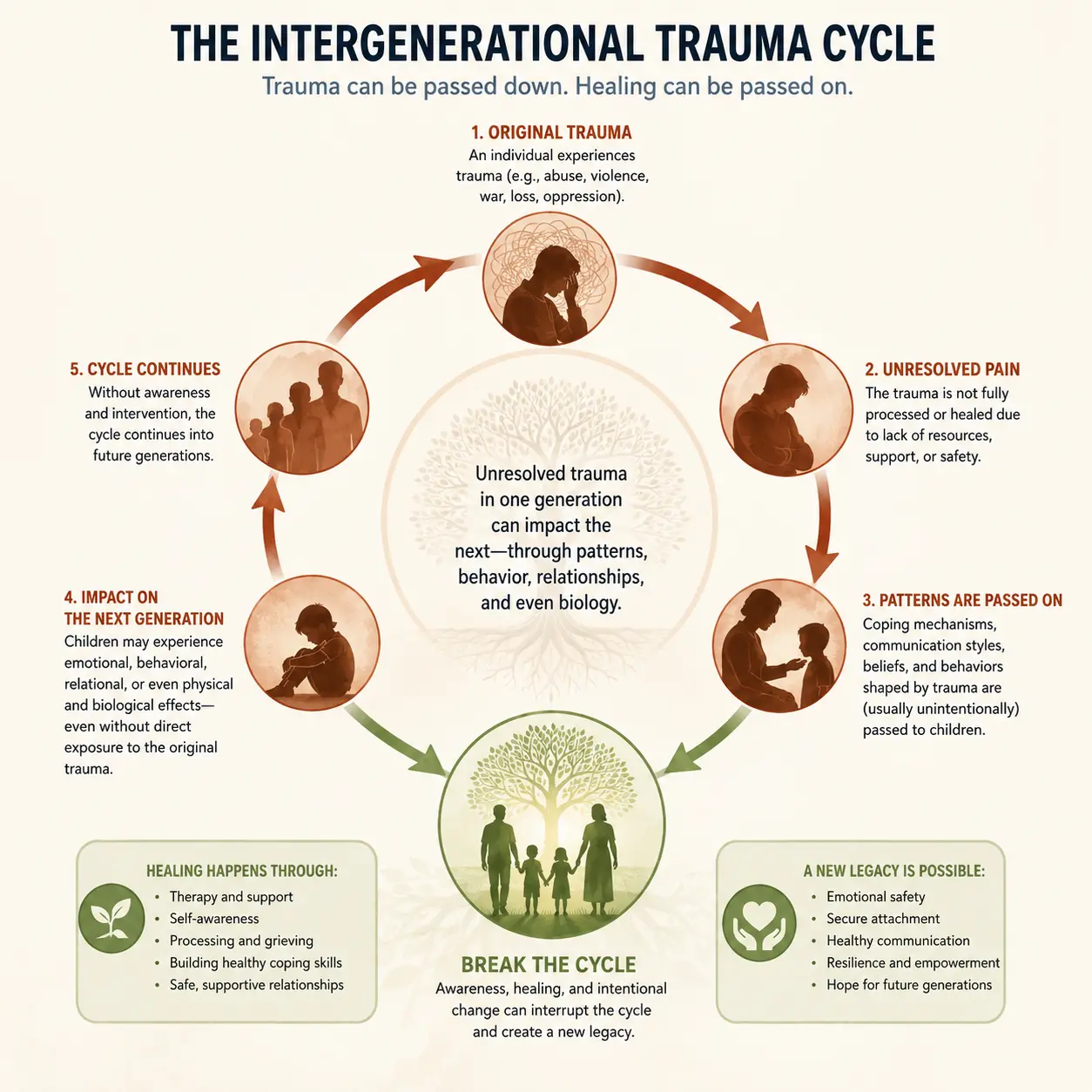
The Intergenerational Trauma Cycle
Intergenerational trauma perpetuates itself through a recognizable cycle that clinicians can learn to identify and interrupt:
- A traumatic event occurs and is not fully processed or healed.
- The affected individual develops coping strategies — including avoidance, emotional numbing, or aggression — that affect their parenting and relationships.
- Their children absorb these patterns through attachment, observation, and the family's emotional environment.
- Without intervention, those children carry the behavioral and emotional patterns into adulthood and their own families.
- The cycle continues until a generation receives effective therapeutic support — or circumstances change significantly enough to interrupt the pattern.
The critical insight for clinicians is that this cycle is interruptible. Effective treatment can stop the transmission, even generations after the original trauma.
Signs and Symptoms of Intergenerational Trauma
Because intergenerational trauma is such a pervasive force within a family system, its symptoms are wide-ranging. Some are direct results of trauma exposure; others reflect long-term dysfunction in the family's emotional environment. Common signs and symptoms include:
- Anxiety and chronic hypervigilance
- Depression and persistent low mood
- Substance use disorders
- Behavioral addictions (gambling, compulsive spending, excessive screen use)
- Anger, aggression, and difficulty managing intense emotions
- Personality disorders, including borderline and narcissistic personality disorder
- Poor or unstable interpersonal relationships
- Difficulty maintaining employment
- Poor academic or school performance in children
- Communication difficulties and chronic conflict
- Sleep disturbances
- Somatic symptoms and poor physical health
- Insecure or disorganized attachment styles
- Shame and low self-worth with no clear personal origin
What makes intergenerational trauma particularly challenging to identify is that clients often do not connect these symptoms to their family history. They may present with depression or relationship difficulties without recognizing that unresolved trauma in prior generations is a contributing factor.

How to Assess Intergenerational Trauma
Accurate assessment is the foundation of effective treatment. Too often, trauma questions are rushed or skipped during intake — either because they feel intrusive or because the clinician is focused on the presenting problem. A thorough intergenerational trauma assessment goes beyond asking "Is there a history of trauma?" It explores the client's direct trauma history and extends that inquiry across generations.
Key elements of a strong intergenerational trauma assessment include:
- Personal adverse childhood experiences (ACEs): physical, sexual, and emotional abuse; neglect; household dysfunction; early loss.
- Family trauma history: Substance use, mental health conditions, incarceration, domestic violence, immigration trauma, or significant losses in parents and grandparents.
- Family secrets and silence: Clients may know that an older relative "wasn't right" or "never talked about the war" without understanding the significance. These are often signals worth exploring.
- Attachment quality: How did the client experience their early relationships with caregivers? Were caregivers emotionally available and consistent?
- Minimization and family narratives: Families often create protective stories that downplay the severity of past trauma. The clinician's role is to gently probe beyond the family's official account.
Download the Intergenerational Trauma Assessment Tool
Support deeper assessment and more thoughtful case conceptualization with a practical tool designed to help clinicians explore how trauma patterns may echo across generations.
This guided clinical tool helps you explore family trauma patterns with your clients. Includes structured screening questions, family history prompts, and an interpretation framework for intake and ongoing therapy.
- Questions to help identify personal and family trauma exposure
- Prompts to explore secrecy, minimization, and intergenerational patterns
- A simple framework you can adapt to intake or ongoing therapy
Complete the form to access your free copy.

Therapy and Treatment for Intergenerational Trauma
Effective treatment for intergenerational trauma draws on many of the same evidence-based approaches used for trauma and PTSD more broadly, while also incorporating systems-level and family-focused interventions. The following modalities are particularly well-suited to this work:
Cognitive Behavioral Therapy (CBT)
CBT is one of the most versatile and widely researched treatment approaches for trauma. It helps clients examine the connections between their thoughts, feelings, and behaviors — allowing them to identify patterns rooted in family history and develop more adaptive responses. For intergenerational trauma, CBT is especially useful in helping clients challenge deeply internalized beliefs about themselves, their worthiness, and their capacity for change.
Dialectical Behavioral Therapy (DBT)
DBT's four core modules — mindfulness, distress tolerance, emotional regulation, and interpersonal effectiveness — address many of the most challenging symptoms associated with intergenerational trauma. Clients who grew up in emotionally unpredictable environments often struggle to regulate intense emotions and maintain stable relationships. DBT provides practical, skill-based tools to help them move from reactivity to intentional action.
Eye Movement Desensitization and Reprocessing (EMDR)
EMDR was specifically designed to process traumatic memories that remain unintegrated in the nervous system. While the original trauma of intergenerational transmission may be historical, clients often carry their own direct trauma experiences as well. EMDR can be highly effective at reducing the emotional charge of these memories, allowing clients to engage more fully in their relationships and parenting.
How to Heal from Intergenerational Trauma: The Role of Family Therapy
While individual therapy addresses the identified client's symptoms, healing intergenerational trauma in its fullest sense requires engaging the family system. Family therapy is not simply an add-on — for many clients, it is the most essential component of treatment.
Family therapy for intergenerational trauma can:
- Bring family members into a shared healing process, reducing the isolation that often accompanies unspoken trauma
- Provide education about how intergenerational trauma works — helping family members understand patterns without assigning blame
- Build self-monitoring skills so members can recognize when old trauma patterns are influencing their current behavior
- Shift communication from aggression or avoidance toward more assertive, emotionally honest dialogue
- Strengthen protective factors and build family cohesion
- Address co-occurring symptoms — depression, anxiety, ADHD, attachment disorders — within the family context
- Empower family members to become conscious cycle-breakers rather than passive carriers of inherited patterns
Some family members will resist engagement in treatment. This is normal and reflects the protective function that family silence often serves. Clinicians should be prepared to work with the family system as it is — not as it ideally would be — and to treat the motivated individuals who are present.
Therapy Pathway for Healing Intergenerational Trauma
Healing intergenerational trauma often involves moving from awareness and assessment to emotional processing, healthier family communication, and new coping patterns.
Awareness
Identify inherited trauma patterns, family narratives, and symptoms that may be connected across generations.
Assessment
Explore personal trauma history, family trauma patterns, attachment disruptions, and current clinical symptoms.
Emotional Processing
Use trauma-informed therapy to process grief, fear, shame, unresolved pain, and survival-based coping responses.
Family Communication
Shift family patterns from silence, avoidance, or conflict toward emotional honesty, boundaries, and repair.
New Coping Patterns
Build emotional regulation, secure attachment behaviors, healthy relationships, and intentional parenting patterns.
Healing Across Generations
Support long-term recovery by interrupting trauma cycles and creating healthier patterns for future generations.
CBT
Helps clients challenge inherited beliefs and develop healthier thought patterns.
DBT
Builds emotional regulation, distress tolerance, mindfulness, and relationship skills.
EMDR
Supports processing of traumatic memories and reduces emotional reactivity.
Family Therapy
Helps families name trauma patterns, improve communication, and build connection.
Frequently Asked Questions About Intergenerational Trauma
Final Thoughts on Healing Intergenerational Trauma
Intergenerational trauma is one of the most pervasive — and most frequently overlooked — forces shaping the clients who walk into behavioral health practices. It hides in plain sight: in the anxious parent who can't explain their fear, in the client who presents with depression but describes a family that "seemed fine," in the child whose behavior problems trace back to a grandparent's unspoken history.
With the right framework, a thorough assessment, and evidence-based therapeutic interventions, clinicians can interrupt cycles that may have persisted for generations. When therapists address intergenerational trauma directly, the benefits extend far beyond the individual client — they reach into the next generation, and the one after that.
How ICANotes Supports Clinicians Treating Intergenerational Trauma
Treating intergenerational trauma often requires clinicians to document complex family dynamics, trauma histories, attachment patterns, co-occurring mental health conditions, and long-term treatment goals across multiple sessions. ICANotes helps behavioral health providers simplify this process with built-in clinical documentation tools designed specifically for trauma-informed care.
ICANotes includes customizable templates for psychotherapy notes, trauma-focused treatment plans, psychiatric evaluations, and progress notes that help clinicians document symptoms, family history, coping patterns, and therapeutic interventions more efficiently. Providers can quickly chart evidence-based modalities commonly used in intergenerational trauma treatment — including CBT, DBT, EMDR, family therapy, and trauma-informed interventions — while maintaining clinically thorough and compliant documentation.
For clinicians conducting trauma assessments, ICANotes also supports structured intake workflows and behavioral health assessment tools that make it easier to capture multigenerational trauma patterns, attachment disruptions, adverse childhood experiences (ACEs), and related psychosocial stressors. Built-in treatment planning tools help providers track progress over time and connect clinical symptoms to measurable goals and interventions.
Because intergenerational trauma treatment frequently involves ongoing care coordination and longitudinal treatment, ICANotes helps clinicians maintain organized, accessible documentation that supports continuity of care across sessions and providers. This can be especially valuable when working with clients experiencing PTSD, anxiety, depression, substance use disorders, attachment difficulties, or family relationship concerns rooted in unresolved trauma.
By reducing time spent on documentation and administrative tasks, ICANotes allows clinicians to focus more fully on what matters most: helping clients process trauma, strengthen relationships, and interrupt harmful patterns across generations.
Free 30-Day Trial
Simplify Trauma-Focused Documentation with ICANotes
ICANotes is designed specifically for behavioral health clinicians treating trauma, PTSD, attachment issues, family dysfunction, and intergenerational trauma patterns. Reduce documentation time while maintaining thorough, compliant clinical records.
✓ Trauma-focused psychotherapy note templates
✓ Built-in assessment tools and treatment plans
✓ Documentation support for CBT, DBT, EMDR, and family therapy
✓ No credit card required to start your free trial
Start Your Free Trial
Spend less time charting and more time helping clients heal from trauma across generations.
Recent Posts
About the Author
Eric Patterson is a professional counselor who has been working for over a decade to help children, adolescents, and adults in western Pennsylvania reach their goals and improve their well-being.
Along the way, Eric worked as a collaborating investigator for the field trials of the DSM-5 and completed an agreement to provide mental health treatment to underserved communities with the National Health Service Corp.






