Blog > Treatment Strategies > Sexual Trauma Therapy: How to Respond, Treat, and Document
Sexual Trauma Therapy: How to Respond to Disclosure, Treat, and Document Effectively
Sexual trauma is a common yet complex clinical presentation that requires structured, trauma-informed care. In this guide, behavioral health clinicians will learn how to recognize sexual trauma symptoms across psychological, behavioral, relational, and somatic domains; respond effectively when clients disclose sexual assault or abuse; select evidence-based sexual trauma therapy approaches; and document care with clinical accuracy and compliance. Whether you’re treating acute sexual assault trauma or complex sexual abuse trauma, this resource provides practical frameworks, decision tools, and documentation strategies to support effective, ethical treatment.

Last Updated: April 27, 2026


What You'll Learn
- How to recognize sexual trauma symptoms across multiple clinical domains
- The key differences between sexual assault trauma and sexual abuse trauma presentations
- How to respond to sexual trauma disclosures with confidence and clinical precision
- What to say—and what to avoid—during the initial disclosure session
- How to choose the right sexual trauma therapy approach (CPT, EMDR, PE, and more)
- When to use phased treatment for complex sexual trauma cases
- How to assess safety, dissociation, and readiness for trauma processing
- Best practices for documenting sexual trauma disclosures and treatment
- How to use validated screening tools (PCL-5, DES-II, PHQ-9) in trauma care
- Practical strategies to support clients healing from sexual trauma over time
Contents
- Understanding Sexual Trauma in Clinical Context
- Recognizing Sexual Trauma Symptoms Across Presentations
- Sexual Assault Trauma Responses vs. Sexual Abuse Trauma Responses
- Sexual PTSD: Diagnostic and Differential Considerations
- Responding to Disclosure: Clinical Best Practices
- Evidence-Based Sexual Trauma Therapy Approaches
- Helping Clients Heal from Sexual Trauma: A Clinical Framework
- Documentation Best Practices for Sexual Trauma Cases
- FAQs: Sexual Trauma
Few moments in clinical practice demand as much composure, sensitivity, and clinical precision as the moment a client discloses sexual trauma. Whether the disclosure arrives in the first session or emerges months into treatment, the clinician’s response — verbal, nonverbal, and procedural — sets the trajectory for everything that follows. A well-handled disclosure builds the therapeutic alliance. A misstep can retraumatize the client and stall recovery before it begins.
This guide is written for behavioral health clinicians who treat clients affected by sexual assault trauma and sexual abuse trauma. It walks through the full clinical arc: recognizing sexual trauma symptoms in presentation, responding therapeutically to disclosures, selecting evidence-based sexual trauma therapy approaches, and documenting with accuracy and compliance. Along the way, you’ll find decision-support frameworks, session-ready language, and documentation guidance designed to strengthen both your clinical practice and your risk management.
Understanding Sexual Trauma in Clinical Context
Sexual trauma is not a single event category — it is a spectrum of experiences that includes sexual assault, childhood sexual abuse, coerced sexual contact, intimate partner sexual violence, trafficking, and ritual abuse. For clinicians, understanding this breadth matters because clients rarely arrive with a neatly labeled chief complaint. They present with sleep disturbance, relationship conflict, substance use, chronic pain, or emotional dysregulation, and the underlying sexual trauma may not surface until trust is established.
The CDC’s National Intimate Partner and Sexual Violence Survey estimates that roughly 1 in 3 women and 1 in 4 men have experienced some form of contact sexual violence in their lifetime. Among behavioral health populations — particularly clients with substance use disorders, eating disorders, and complex trauma histories — prevalence is significantly higher. These numbers make sexual trauma not an occasional clinical encounter but a routine one, and clinicians need structured protocols rather than improvised responses.
Key Clinical Distinctions
Two primary categories of sexual trauma carry distinct clinical implications:
- Sexual assault trauma typically refers to a discrete event or limited series of events — often involving force, coercion, or incapacitation. Clients with sexual assault histories may present with acute stress reactions, avoidance of reminders, hypervigilance, and flashbacks that are temporally anchored to identifiable incidents.
- Sexual abuse trauma more commonly describes prolonged or repeated victimization, often beginning in childhood and frequently perpetrated by someone known to the victim. Clinical presentations tend to be more complex: dissociation, identity disturbance, attachment disruption, affect dysregulation, and relational patterns marked by boundary confusion.
Recognizing whether a client’s history aligns more closely with sexual assault trauma or sexual abuse trauma helps guide your initial conceptualization, intervention selection, and treatment pacing — distinctions explored in detail below.
Recognizing Sexual Trauma Symptoms Across Clinical Presentations
Sexual trauma symptoms rarely announce themselves with a textbook presentation. Clients may not connect their symptoms to their trauma history, and some may not yet have language for what happened to them. Effective clinical practice requires pattern recognition across multiple domains.
Psychological and Emotional Symptoms
Intrusion Symptoms
Flashbacks, nightmares, intrusive images, or sensory fragments such as smells, sounds, or tactile sensations related to the traumatic event(s).
Avoidance
Behavioral avoidance of people, places, or situations associated with the trauma; emotional numbing or constriction of affect; reluctance to discuss sexual health or relationships.
Negative Cognitions
Persistent beliefs about self-blame (“It was my fault”), damaged identity (“I’m ruined”), or distrust (“No one is safe”).
Affect Dysregulation
Emotional reactivity disproportionate to context; difficulty identifying or labeling emotions; chronic irritability, shame, or guilt.
Dissociation
Depersonalization, derealization, gaps in memory, or trance-like states—particularly common in clients with childhood sexual abuse histories.
Behavioral and Relational Symptoms
Self-Destructive Behavior
Substance misuse, self-harm, disordered eating, and high-risk sexual behavior as attempts to manage intolerable affect.
Relational Disruption
Difficulty with trust, boundary maintenance, and intimacy; oscillation between enmeshment and avoidance in relationships.
Revictimization Patterns
Repeated involvement in abusive or exploitative relationships, sometimes linked to disrupted threat detection systems.
Somatic Complaints
Chronic pelvic pain, gastrointestinal distress, headaches, or unexplained physical symptoms without clear medical etiology.
Presentation Differences by Trauma Type
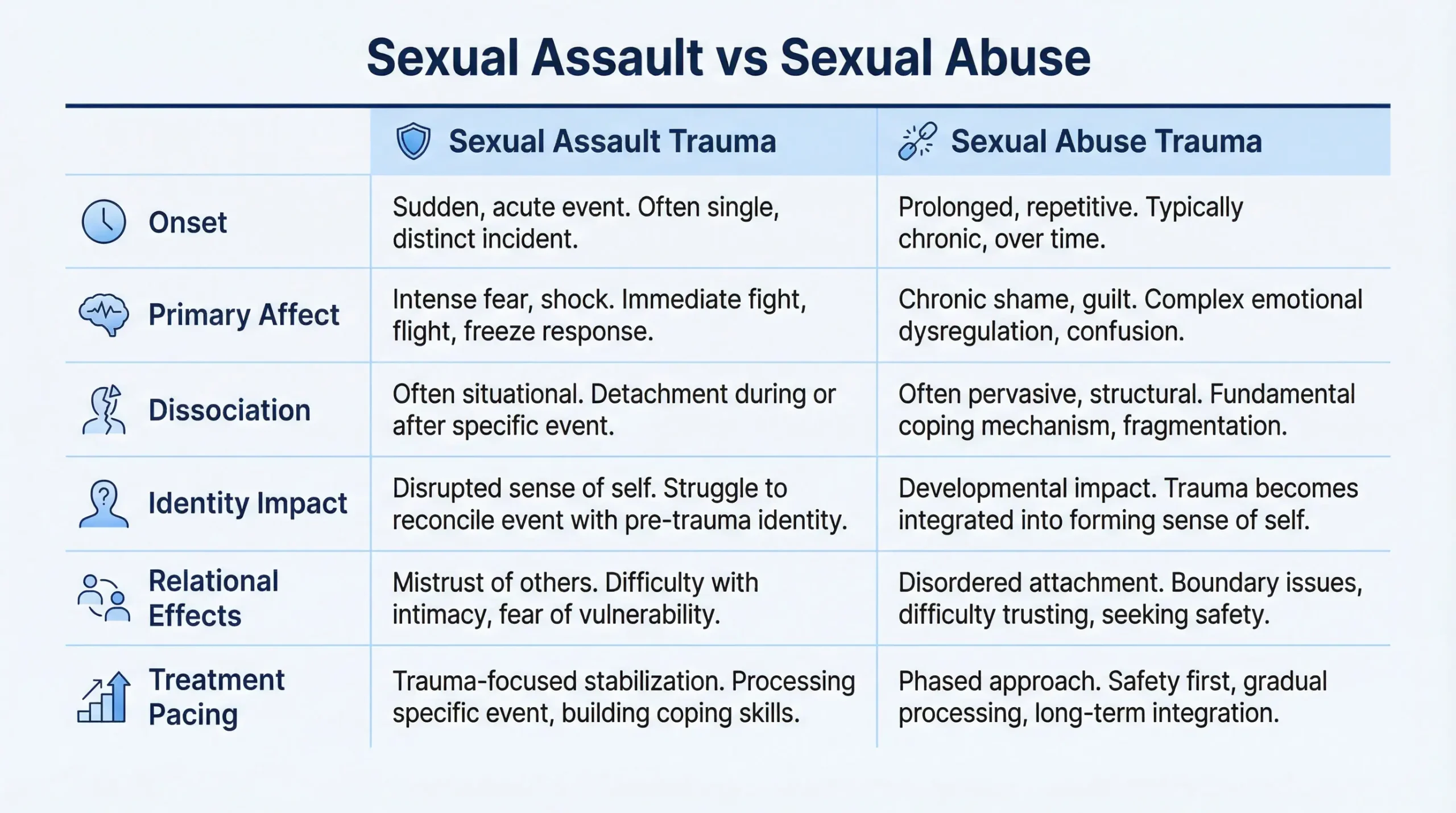
The distinction between sexual trauma symptoms associated with a single incident versus those arising from prolonged abuse is clinically significant. Acute sexual assault may produce a presentation that maps closely onto classic PTSD criteria, while childhood sexual abuse more often produces a complex, multimodal picture. The table below summarizes typical differences in clinical presentation.
Sexual Assault Trauma Responses vs. Sexual Abuse Trauma Responses
Understanding sexual assault trauma responses and sexual abuse trauma responses as distinct clinical phenomena — rather than interchangeable terms — improves both case conceptualization and intervention planning.
Sexual Assault Trauma Responses
Clients who have experienced sexual assault often present with sexual assault trauma responses that mirror the classic fear-conditioning model. The autonomic nervous system encodes the assault as a life-threatening event, producing:
- Fight, flight, freeze, or fawn responses that persist beyond the event
- Hyperarousal: exaggerated startle, sleep disturbance, scanning for threat
- Re-experiencing: sensory-driven flashbacks anchored to specific event details
- Avoidance organized around event-specific triggers (locations, times of day, physical characteristics of the perpetrator)
These responses are often well-suited to structured trauma-processing protocols such as Prolonged Exposure (PE) or Cognitive Processing Therapy (CPT), where a clearly defined index trauma can be targeted.
Sexual Abuse Trauma Responses
Sexual abuse trauma responses reflect adaptation to chronic threat within a relational context, typically during developmental years. The clinical picture is broader and more deeply embedded:
- Affect dysregulation as a core feature rather than a secondary symptom
- Structural dissociation: the client may shift between emotional parts, sometimes with amnesia for certain states
- Relational reenactments: unconscious repetition of abuser–victim dynamics in therapy and outside relationships
- Shame as an organizing emotion, distinct from the fear-based architecture of single-incident trauma
- Somatic encoding: traumatic experiences stored in body-based symptoms rather than narrative memory
These clients typically require a phased treatment approach, beginning with safety and stabilization, before any direct trauma processing is attempted. The clinician’s role during Phase 1 work is to help the client develop the emotional regulation capacities that the abusive environment prevented from developing naturally.
Sexual PTSD: Diagnostic and Differential Considerations
While “sexual PTSD” is not a formal DSM-5-TR diagnostic category, it is a widely used clinical shorthand for post-traumatic stress disorder arising from sexual victimization. Clinicians should be aware of several diagnostic considerations specific to trauma of a sexual nature.
DSM-5-TR PTSD Criteria in Sexual Trauma Contexts
Criterion A is met when a client has been exposed to actual or threatened sexual violence. Importantly, the DSM-5-TR explicitly lists sexual violence as a qualifying traumatic event separate from physical assault and serious injury, recognizing its distinct psychological impact. When assessing for sexual PTSD, clinicians should note:
- Intrusion symptoms (Criterion B) in sexual trauma cases often include sensory-dominant flashbacks—body memories, olfactory intrusions, and tactile re-experiencing—that may be more prominent than visual re-experiencing
- Avoidance (Criterion C) frequently extends to intimacy, gynecological or urological care, and sexuality-related conversations, sometimes creating secondary health consequences
- Negative alterations in cognition and mood (Criterion D) often center on shame, self-blame, and beliefs about being permanently damaged—distinct from the guilt and horror profiles seen in other trauma types
- Arousal and reactivity (Criterion E) may include sexual dysfunction as a specific manifestation of hyperarousal or numbing
Differential Diagnostic Considerations
Sexual trauma histories complicate differential diagnosis in several ways. Clinicians should consider:
Complex PTSD (ICD-11)
Clients with histories of prolonged sexual abuse may meet criteria for Complex PTSD, which includes disturbances in self-organization such as affect dysregulation, negative self-concept, and relational disturbance in addition to core PTSD symptoms.
Dissociative Disorders
Childhood sexual abuse is the most commonly reported antecedent to dissociative identity disorder (DID) and other specified dissociative disorder (OSDD). Screen for dissociation using validated tools such as the DES-II.
Borderline Personality Disorder (BPD)
The overlap between BPD and complex trauma presentations is well-documented. Before assigning a personality disorder diagnosis, evaluate whether symptoms are better explained by developmental sexual abuse trauma.
Somatic Symptom Disorders
Unexplained pain, conversion symptoms, and functional neurological symptoms may reflect somatic encoding of sexual trauma rather than primary somatic disorders.
Responding to Disclosure: Clinical Best Practices
The moment of disclosure is one of the most consequential in the treatment of sexual trauma. How a clinician responds — verbally, nonverbally, and procedurally — shapes the client’s willingness to continue engaging in treatment and their sense of safety in the therapeutic relationship.
Immediate Response Principles
- Regulate yourself first. Monitor your own physiological and emotional response. Clients are acutely attuned to clinician reactions — a visible flinch, a sharp intake of breath, or a change in eye contact can communicate shock or discomfort that the client may interpret as judgment. As Jessica Ronyak, LMHC, LPCC and founder of Lōmii Studio explains, “Your role, as the clinician, is to stay regulated, present, and attuned rather than become urgent or reactive.”
- Validate the act of disclosure. Acknowledge the courage required to share: “Thank you for trusting me with this. I know that took a lot of courage.” Do not rush past this moment.
- Affirm the client’s experience without interrogating. Avoid probing for details in the disclosure session. “I believe you” and “What happened to you was not your fault” are powerful orienting statements. Detailed trauma narratives belong later in treatment, within a structured protocol.
- Assess for immediate safety. Determine whether the client is currently safe from ongoing harm. If the disclosure involves a minor or an ongoing threat, address mandatory reporting obligations with transparency.
- Collaboratively plan next steps. Close the session with a clear, collaborative plan: “We don’t need to cover everything today. What feels most important to you right now?” Offer stabilization resources and confirm the next appointment.
“Most clients who disclose sexual trauma have spent a lot of effort figuring out whether it’s safe to say this out loud… they’re going to read your face, your body, and your tone very closely.”
— Dr. Caitlin Stamatis, Clinical Psychologist & Head of Research at Slingshot AI
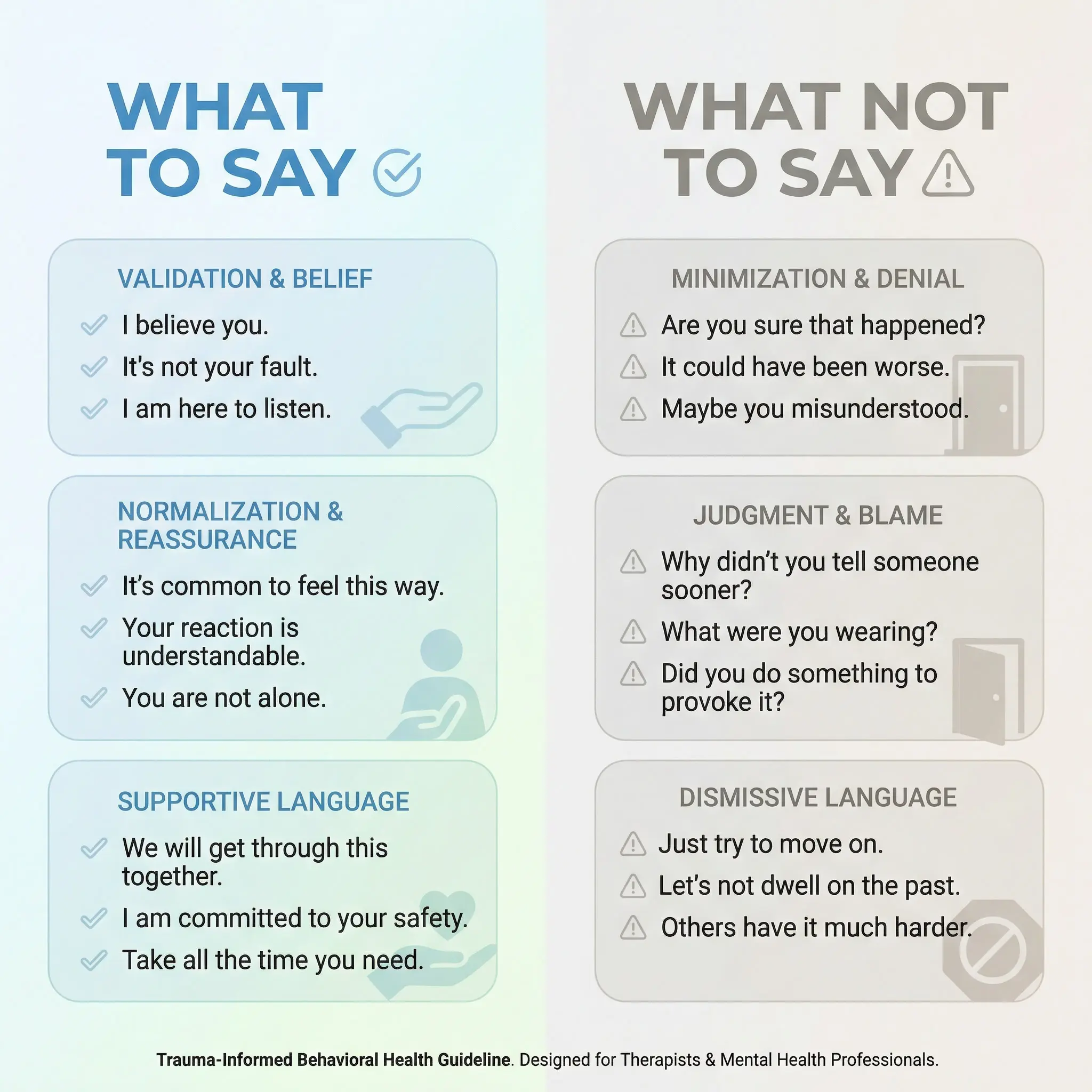
What Not to Do
As Jessica Ronyak, LMHC, LPCC notes, “Many clinicians are often too quick to try to get all the details or jump right into problem-solving before the client can start to feel safe and stabilized.” Even well-intentioned responses can undermine safety if they shift control, minimize the experience, or prioritize information-gathering over attunement.
- Do not express shock, horror, or excessive emotional response — this shifts the burden of emotional management onto the client
- Do not ask “Why didn’t you…?” questions (leave, report, fight back) — these reinforce self-blame
- Do not immediately launch into psychoeducation or treatment planning — the client needs to feel heard before they need to feel educated
- Do not minimize (“At least it wasn’t…”) or universalize (“This happens to a lot of people”) — both invalidate the individual’s experience
- Do not promise confidentiality you cannot guarantee — if mandatory reporting applies, disclose this clearly and early
Evidence-Based Sexual Trauma Therapy Approaches
Selecting the right sexual trauma therapy approach requires matching the intervention to the client’s presentation, trauma type, phase of recovery, and capacity for engagement. No single modality is universally best; the clinician’s skill lies in matching the approach to the individual.
First-Line Trauma-Focused Therapies
Prolonged Exposure (PE)
Involves systematic, repeated engagement with trauma-related memories and avoided situations. Strong evidence base for PTSD arising from sexual assault. Best suited for clients who can tolerate arousal and have a clearly defined index trauma. Contraindicated in active suicidality, severe dissociation, or untreated substance dependence.
Cognitive Processing Therapy (CPT)
Targets maladaptive cognitions (stuck points) related to the trauma, such as self-blame, distrust, and beliefs about safety. Particularly effective when shame and guilt are prominent features of the client’s presentation. Can be delivered in individual or group formats.
EMDR (Eye Movement Desensitization and Reprocessing)
Uses bilateral stimulation during reprocessing of traumatic memories. Effective for both single-incident and complex trauma, though complex cases may require extended preparation phases. May be preferred by clients who find verbal narration of trauma aversive.
Approaches for Complex Sexual Trauma
Phased Treatment / Trauma-Informed Stabilization
The international consensus model for complex trauma, including prolonged sexual abuse trauma, follows three phases: (1) safety, stabilization, and skill-building; (2) trauma processing; and (3) reconnection and integration. This framework is essential when clients present with dissociation, severe affect dysregulation, or attachment disorganization.
Dialectical Behavior Therapy (DBT)
While not a trauma-processing therapy per se, DBT provides the emotional regulation, distress tolerance, and interpersonal effectiveness skills that many sexual abuse survivors need before they can safely engage in trauma-focused work. DBT-PE integrates prolonged exposure within the DBT framework.
Sensorimotor Psychotherapy and Somatic Experiencing
Body-oriented approaches that address somatic encoding of sexual trauma. These are particularly relevant for clients whose symptoms are predominantly somatic or who become overwhelmed by cognitive or narrative approaches.
Internal Family Systems (IFS)
A parts-based approach that can be effective for clients with dissociative features or internal conflict related to their trauma history. IFS offers a framework for working with shame, self-blame, and protective parts without requiring early direct trauma confrontation.
Intervention Selection Considerations
Selecting the right sexual trauma therapy approach depends on the client’s presentation, stability, and readiness for processing. Use the decision pathway below to guide clinical decision-making.
Sexual Trauma Therapy Decision Tree
Match treatment approach to client presentation, stability, and readiness for trauma processing.
Start Here
Assess the client’s trauma history, symptom presentation, and current level of stability before selecting an intervention.
Single-Incident Sexual Assault
Clear index trauma, stable functioning, and capacity to tolerate direct trauma work.
Strong evidence base for direct trauma processing when arousal is manageable.
Complex Childhood Sexual Abuse
Chronic trauma history, affect dysregulation, attachment disruption, or identity disturbance.
Premature trauma processing may increase destabilization risk.
Prominent Dissociation
Structural dissociation, amnesia, derealization, or poor dual awareness.
Build grounding, stabilization, and present-moment capacity first.
Somatic Predominance
Body-based symptoms predominate, or verbal trauma narration is overwhelming.
Bottom-up approaches can better support regulation and trauma integration.
Co-Occurring Substance Use Disorder
Substance use is active, unstable, or likely to interfere with safe trauma processing.
Stabilize substance use before or alongside trauma-focused work as clinically indicated.
Clinical Reminder
Reassess safety, dissociation, symptom severity, and readiness for processing at regular intervals. Treatment planning for sexual trauma should remain flexible, phased, and responsive to the client’s window of tolerance.
For a more detailed comparison, see the breakdown below.
Helping Clients Health from Sexual Trauma: A Clinical Framework
Clinicians are often asked — by clients, by families, and by their own internal sense of purpose — how to heal from sexual trauma. The answer, of course, is that healing is nonlinear and deeply individual. But clinicians can apply a structured framework that supports recovery across the three core domains most affected by sexual trauma: safety, meaning-making, and reconnection.
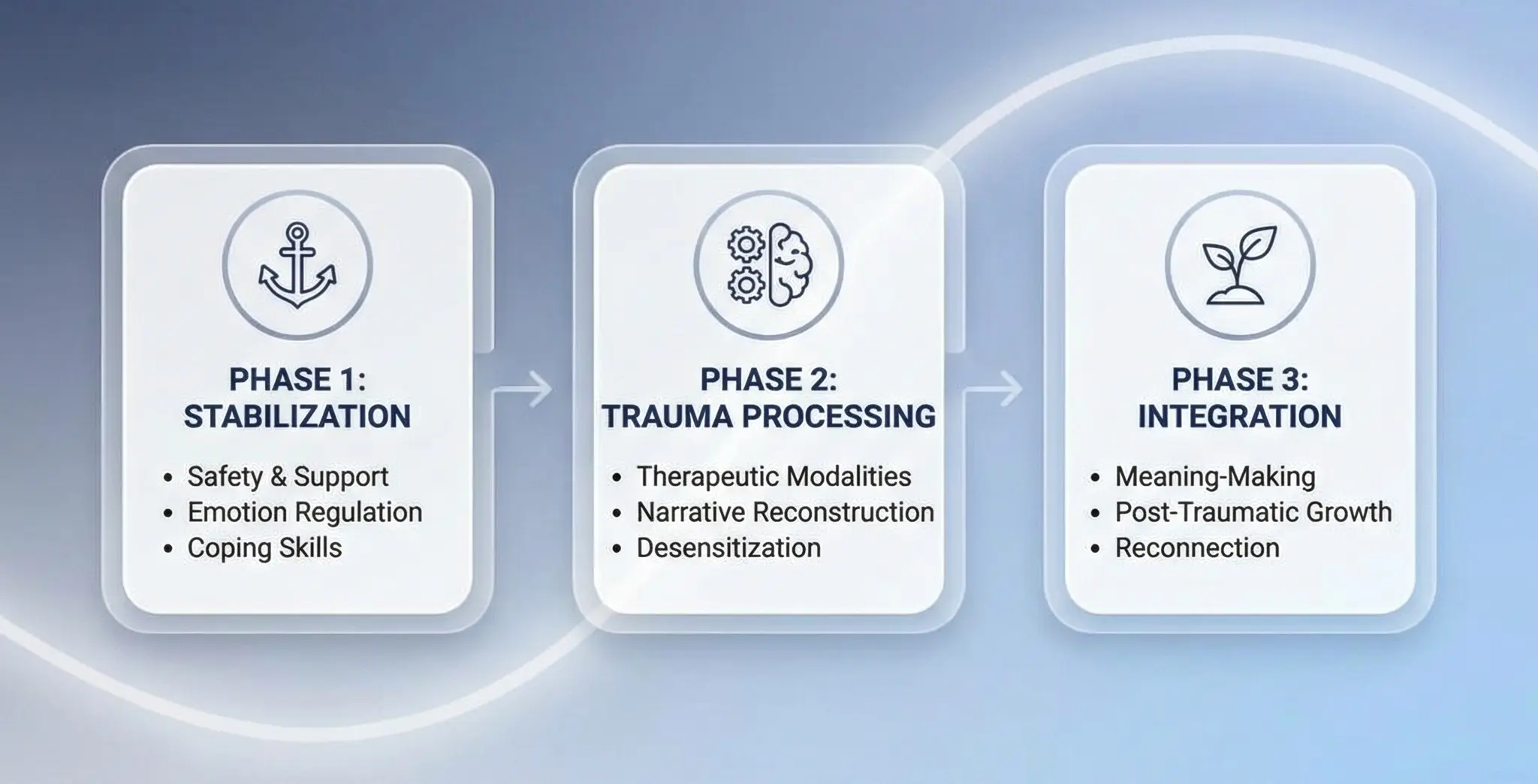
Domain 1: Safety and Stabilization
Before any trauma processing begins, the client needs a foundation of safety — both external (physical safety, stable housing, freedom from ongoing abuse) and internal (the ability to regulate affect, tolerate distress, and remain present). Clinical priorities in this phase include:
- Establishing a strong therapeutic alliance built on transparency, consistency, and predictability
- Teaching and reinforcing grounding techniques, affect regulation skills, and distress tolerance strategies
- Addressing co-occurring concerns (substance use, self-harm, suicidality, eating disorders) that may destabilize the client during later phases
- Psychoeducation about trauma responses — normalizing symptoms without pathologizing the client
Jessica Ronyak, LMHC, LPCC notes "I'm usually looking for whether the client has consistent access to regulation . . . can they notice activation and return to baseline with support?"
Domain 2: Processing and Meaning-Making
When the client has sufficient stabilization and coping capacity, the clinician introduces structured trauma processing — using the evidence-based approach best matched to the client’s presentation. Goals during this phase include:
- Reducing the emotional charge of traumatic memories through controlled re-engagement
- Challenging maladaptive cognitions (self-blame, damaged identity, beliefs about trust and safety)
- Integrating fragmented or dissociated trauma material into coherent autobiographical memory
- Facilitating the client’s development of a trauma narrative that supports post-traumatic growth rather than reinforcing victimization
Domain 3: Reconnection and Integration
The final phase focuses on helping the client re-engage with life beyond trauma. Clinically, this involves:
- Supporting the client in rebuilding or establishing healthy relationships and attachment patterns
- Addressing sexual health and intimacy concerns that are often uniquely affected by sexual trauma
- Helping the client develop a future-oriented identity that integrates, but is not defined by, their trauma history
- Relapse prevention planning: identifying triggers, early warning signs, and coping strategies for future activation
Understanding how to heal from sexual trauma as a phased, clinician-guided process — rather than a single intervention — helps set appropriate expectations for both the client and the treatment team.
“If someone can’t handle a little bit of stress without feeling like they’re losing control, then trying to process trauma will only make things worse.”
— Shari B. Kaplan, LCSW, Integrative Mental Health Clinician and Founder of Cannectd Wellness
Documentation Best Practices for Sexual Trauma Cases
Clinical documentation in sexual trauma cases carries unique weight. Notes may be subpoenaed in legal proceedings, reviewed by insurance companies, or accessed by other providers. Accurate, clinically appropriate documentation protects the client, supports continuity of care, and reduces risk for the clinician.
General Documentation Principles
- Document disclosures factually. Record what the client reported using the client’s own language where possible. Use quotation marks for direct statements: “Client stated, ‘My uncle touched me when I was eight.’” Avoid interpretive language or editorial framing. Jessica Ronyak LMHC, LPCC adds, "It's important to distinguish between what the client reports and what is clinically observed, using clear, non-assuming language."
- Avoid unnecessary detail. Document the clinical significance of the disclosure — not a blow-by-blow account of the traumatic event. Excessive detail serves no clinical purpose and may cause harm if records are accessed inappropriately. As Dr. Caitlin Stamatis explains, "Document the minimum necessary detail for clinical purposes . . . be sparing with graphic content, especially since records may be subpoenaed."
- Use clinical language, not legal language. Write “client reports sexual abuse by a family member” rather than “client was molested.” Document what the client reported; do not render legal conclusions about what occurred.
- Record your clinical response. Document the interventions provided in the session: safety assessment, stabilization techniques, psychoeducation offered, and the collaborative treatment plan developed. This demonstrates standard of care.
- Document mandatory reporting actions. If the disclosure triggered a mandatory report, document that the report was made, to which agency, and that the client was informed of the reporting obligation. Note the client’s response to being informed.
- Track symptom severity and functional impact. Use validated measures (PCL-5, PHQ-9, DES-II) at regular intervals to document treatment response. Quantitative data strengthens both clinical decision-making and insurance justification.
Documentation Pitfalls to Avoid
- Writing notes that read as if the clinician has determined facts rather than recorded the client’s report
- Including graphic trauma details that exceed what is clinically necessary
- Failing to document safety assessments — especially when clients disclose active self-harm or suicidality alongside sexual trauma
- Using stigmatizing language (“victim,” “accused,” “alleged”) when clinical terminology is more appropriate
- Omitting treatment rationale for selected interventions — this is critical for medical necessity documentation and malpractice protection
How EHR Tools Support Sexual Trauma Documentation
Behavioral health EHR systems designed for the clinical workflow can significantly reduce the documentation burden associated with sexual trauma cases. Features like structured note templates, customizable treatment plan builders, and integrated outcome-tracking tools help clinicians capture the right information — at the right level of detail — without spending excessive time on charting. When your EHR includes built-in templates for trauma-informed assessments, safety planning, and progress notes, documentation becomes a clinical asset rather than an administrative burden.
Strengthening Your Clinical Response to Sexual Trauma
“Slow down and trust that the client knows their own pace better than you do.”
— Dr. Caitlin Stamatis, Clinical Psychologist & Head of Research at Slingshot AI
Treating sexual trauma effectively requires more than empathy — it requires clinical structure. From the moment of disclosure through ongoing sexual trauma therapy and into documentation, every step benefits from evidence-based protocols, validated tools, and a clear understanding of the unique sexual trauma symptoms your clients bring into the room.
When clinicians are equipped with the right frameworks — and supported by clinical documentation tools designed for behavioral health — they can provide trauma-informed care that is both clinically rigorous and deeply human. Whether you are working with a client navigating the aftermath of a single sexual assault or supporting someone through the long process of healing from childhood sexual abuse, structured clinical practice makes the difference between survival and recovery.
Frequently Asked Questions About Sexual Trauma in Clinical Practice
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.





