Blog > Documentation > Biopsychosocial Assessment: How to Write One (+ Examples & Template)
How to Write a Biopsychosocial Assessment: Questions, Examples & Template
A biopsychosocial assessment is a clinical evaluation used during mental health intake to understand how biological, psychological, and social factors affect a client’s functioning. In this guide, you’ll learn how to write a biopsychosocial assessment step by step, with sample questions, a complete example, and a downloadable checklist to support accurate, audit-ready documentation.

Last Updated: April 2, 2025


What You'll Learn
- What a biopsychosocial assessment is and what it should include across biological, psychological, and social domains
- Key questions to ask in each domain, plus example notes that show how to translate client responses into clinical documentation
- How to use the "Ps" framework (predisposing, precipitating, perpetuating, protective) to build a clinical formulation
- A complete biopsychosocial assessment example — including a mental status exam and treatment plan — to guide your clinical writing
- How to synthesize assessment data into a coherent narrative that supports diagnosis, treatment planning, and medical necessity
- Best practices for assessment quality, common documentation errors, and how standardized tools can strengthen your formulation
Contents
- What Is a Biopsychosocial Assessment?
- What Is Included in a Biopsychosocial Assessment?
- Biopsychosocial Assessment Checklist: 25 Documentation Standards
- Biopsychosocial Assessment Questions by Domain
- How to Write a Biopsychosocial Assessment
- Biopsychosocial Case Formulation: The "Ps" Framework
- How to Synthesize a Biopsychosocial Assessment Narrative
- Biopsychosocial Assessment Example
- Tips for Writing a Biopsychosocial Assessment
- FAQ: Biopsychosocial Assessments
- Why Use ICANotes for Biopsychosocial Assessments?
A strong biopsychosocial assessment forms the foundation for effective treatment. It helps you understand the full picture of a client’s health, identify underlying issues, and align care with their needs and goals. Done well, it also improves collaboration with other providers and supports accurate diagnoses and treatment planning.
What is a Biopsychosocial Assessment?
A biopsychosocial assessment is a clinical tool used to evaluate how biological, psychological, and social factors affect a client’s mental and physical health. It is typically completed during the intake process to support diagnosis, guide treatment planning, and document medical necessity. Biopsychosocial assessments are used across behavioral health disciplines — including social work, counseling, psychology, and psychiatry — as the standard framework for comprehensive clinical evaluation.
The biopsychosocial model, developed by Dr. George Engel in 1977, emphasizes that health is influenced by physical conditions, mental states, behaviors, relationships, and environment.
In behavioral health settings, this approach helps identify underlying causes of symptoms, such as trauma or social stressors. It also supports more accurate documentation and allows for personalized, whole-person care.
What is Included in a Biopsychosocial Assessment?
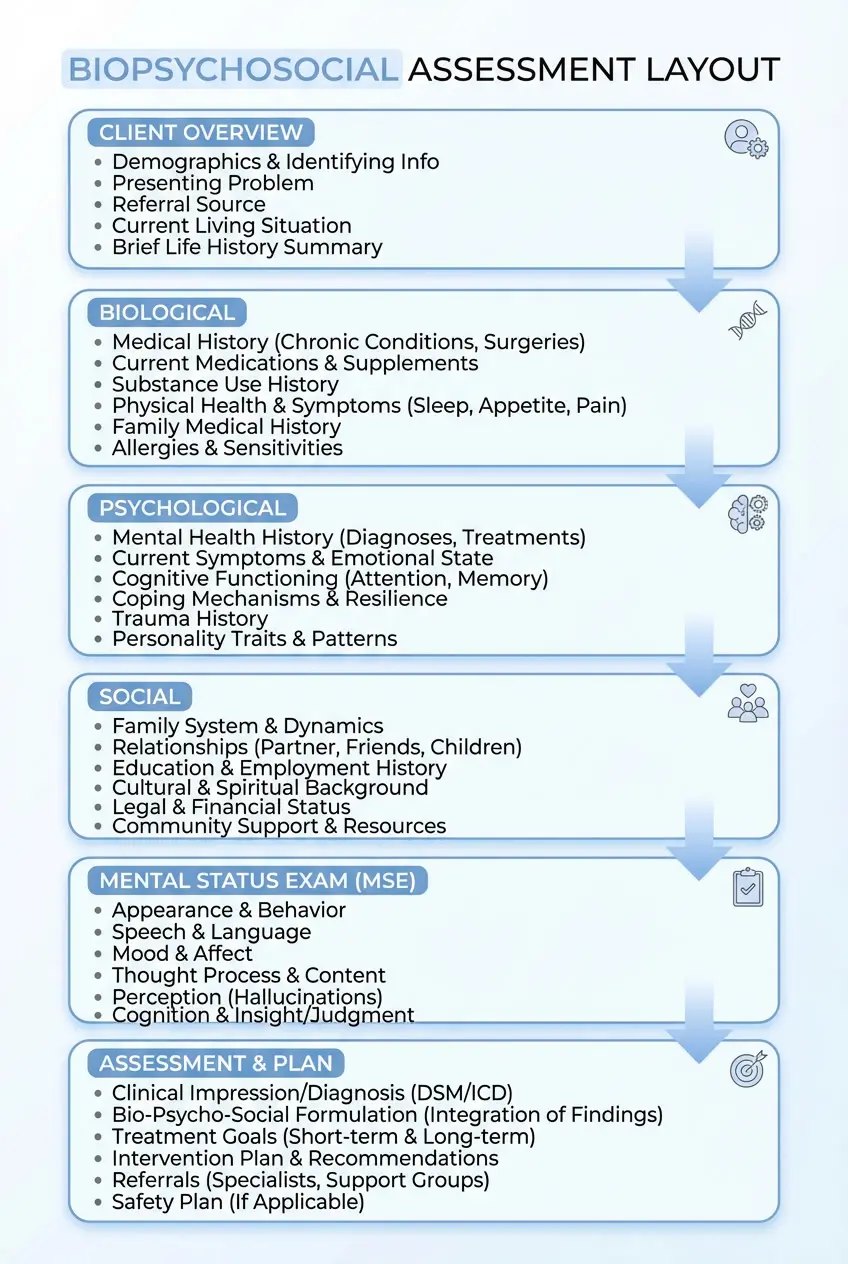
A biopsychosocial assessment typically includes detailed information across three core domains: biological, psychological, and social. Together, these areas offer a full picture of a client’s health, functioning, and environment.

1. Biological Factors
Biological factors in a biopsychosocial assessment include a client’s physical health, medical history, and genetic background. This may involve chronic illnesses, current medications, past surgeries, sleep habits, diet, substance use, and family history of medical or mental health conditions.
Clinicians assess these areas to understand how physical health may be contributing to mental or emotional symptoms.
Useful biological domains to assess include: genes, age, immune response, infections, environmental toxins, physical traumas, diet, appetite, hormones, and sleep/exercise habits.
2. Psychological Factors
Psychological factors include a client’s thoughts, emotions, behaviors, and coping skills. These internal experiences are central to mental health and often interact with physical symptoms. For instance, over 36% of people with chronic pain report depressive symptoms, and more than 55% experience anxiety or depression.
This part of the assessment explores how clients handle stress, regulate emotions, and manage mental health symptoms. It also includes mental health history, prior diagnoses, treatment experiences, and current psychological functioning.
Common psychological domains to assess include: personality, psychological traumas, stress, coping skills, suicidal ideation, and reaction to illness.
3. Social Factors
Social factors include the external conditions that influence a client’s relationships, identity, and access to resources. These may involve family dynamics, income, education, housing, cultural background, and community ties.
Research shows that social determinants like income, education, and neighborhood safety strongly affect mental health. Stable housing and financial security support well-being, while poverty, unemployment, and discrimination can increase stress and worsen symptoms. Assessing these areas helps identify both barriers and supports that influence treatment.
Common social domains to assess include: family relationships, social support, marital status, cultural influences, food security, income level, discrimination, living situation, military service, spiritual or religious background, hobbies and recreational activities, sexual history, financial status, legal history, educational background, employment status and work history, and access to affordable healthcare.
Biopsychosocial Assessment Checklist: 25 Documentation Standards
Before writing your biopsychosocial assessment — or after completing one — use this checklist to verify your documentation covers the 25 elements that payers, licensing boards, and accreditation reviewers look for during audits. A complete assessment covering all five domains is the foundation of defensible, billable behavioral health care.
Use the interactive checklist to audit your assessment in real time, or download the PDF version to keep at your desk.
Don’t Miss Critical Elements in Your Biopsychosocial Assessment
Use this Biopsychosocial Assessment Checklist to make sure your intake documentation covers the standards payers, supervisors, and reviewers expect to see.
This practical tool helps you review your assessment across biological, psychological, social, risk, and formulation domains so you can catch gaps before they become audit or reimbursement problems.
- ✔ Review 25 essential documentation elements
- ✔ Strengthen medical necessity and audit readiness
- ✔ Use it interactively or as a downloadable reference
A simple way to benchmark your assessment before finalizing the note.
Get the Checklist
Instant access after submission.
The checklist covers five domains: biological (medications, medical diagnoses, psychiatric history, substance use, family history), psychological (chief complaint, mental status exam, trauma history, coping patterns, cognitive functioning), social (living situation, support system, employment, cultural factors, legal history), risk and safety (suicidal ideation, homicidal ideation, self-harm, access to means, safety planning), and clinical formulation (integrated narrative, DSM-5/ICD-10 diagnosis, functional impairment, strengths, and level of care recommendation).
Biopsychosocial Assessment Questions by Domain
Asking the right questions during intake is essential for building a complete biopsychosocial assessment. The questions below are organized by domain and designed to surface clinically relevant information efficiently. Not every question needs to be asked of every client — use your clinical judgment to prioritize what's most relevant to the presenting concern.
Risk & Safety Workflow
A Simple Flow for Risk & Safety Screening
Use this process to guide direct, calm safety screening during intake and to document risk with greater specificity.
Documentation reminder
Avoid vague phrasing like “denies SI” without context. Stronger documentation specifies current ideation, plan, intent, history, access to means, protective factors, and the clinician’s response or recommendation.
Efficient Intake Framework
A Simple Structure for a 45-Minute Intake Session
This intake flow helps clinicians gather high-value biopsychosocial information efficiently while preserving rapport, supporting safety screening, and leaving time for treatment direction.
Documentation tip: Not every question needs to be asked in every intake. Prioritize what is most relevant to the presenting concern, document safety clearly, and defer lower-priority history when it does not affect immediate diagnosis or treatment planning.
Run More Efficient Intakes Without Missing What Matters
Want a structured, print-ready version of these questions organized for a 45-minute intake session?
The Efficient Intake Guide includes high-impact biopsychosocial assessment questions across all domains, a suggested session structure with time allocations, documentation reminders, and clinical tips on what to listen for—and what can be deferred.
- Stay on track without missing critical information
- Balance thoroughness with real-world time constraints
- Strengthen documentation and medical necessity support
Designed for real clinical workflows—not theoretical checklists.

Get the Guide
Instant access after submission.
How to Write a Biopsychosocial Assessment
After you've gathered data about your client, you can write a biopsychosocial assessment report. Your report will help you understand your client as a whole individual to devise an effective treatment plan. You can also share your assessment with colleagues or physicians to coordinate care.
Here's a biopsychosocial assessment outline to help you get started.
Basic Information
Begin your report with basic information about your client. This should include:
- Identifying information: Include the client’s name, gender, date of birth, and marital status.
- Referral: Name the person or agency that referred the client and the reason for the referral.
- Presenting problem: Summarize why the client is seeking help, how long the issue has been present, their perspective on the problem, and any past attempts to address it.
- Source of data: List tools or methods used to collect information (e.g., interviews, questionnaires, records). Note how involved the client was in the process.
- General description of the client: Describe the client’s appearance, mood, and engagement during the session. Note any issues with memory, thinking, speech, or signs of distress.
Client's History and Current Functioning
Summarize key areas of the client’s background and current functioning that impact their mental health:
- Family history: Include relationships during childhood and any family history of substance use, legal issues, or psychiatric conditions.
- Education: Note academic history, challenges, and current goals.
- Employment: Outline current job status, work history, and relevant skills or training.
- Spiritual beliefs: Mention religious or spiritual affiliation and community involvement.
- Military service: Indicate if the client served, with their role, service dates, major stressors, and discharge type.
- Medical history: Include current health status, major illnesses or injuries, medications, and family medical history.
- Mental health: Describe past and current experiences with mental illness, trauma, or abuse.
- Substance use: Summarize history of alcohol or drug use, including treatment or rehab.
- Social life: Note support system, relationships, hobbies, and community involvement.
- Daily functioning: Assess the ability to meet basic needs like housing, food, and personal care.
- Legal history: Mention past or current legal concerns, including domestic issues.
- Strengths and coping: Identify coping skills, strengths, and areas of resilience.
- Other factors: Include any relevant environmental or psychosocial issues, such as discrimination or identity-related stress.
Your Assessment and Recommendations
After you provide an overview of your client's current and past psychological, biological, and social states, it's time to include your professional assessment. You might offer the following information:
- Brief summary: In about three to five sentences, summarize what you've already written in your report, including your client's primary problem and any associated factors. Describe your client's level of urgency regarding the problem. Mention any secondary issues or concerns your client shared.
- Client's appearance: Describe how your client appeared during the interview, including signs of anxiety or depression and any memory or speech issues. If you also conducted a mental status exam during your initial meeting with a client, include it in this section.
- Your observations: Provide your observations of the client and their current state. Discuss your assessment of the client's motivation to use your service and modify behaviors.
- Diagnosis: Include your diagnosis and any diagnoses your client claimed they'd been given in the past by other therapists.
- Goals and recommendations: Identify long-term and short-term goals. Describe the type of treatment you think is best for your client and any suggestions for services and resources. Include how long you think your client should receive treatment.
Biopsychosocial Case Formulation: The "Ps" Framework
The "Ps" of the biopsychosocial assessment refer to a clinically useful framework that helps behavioral health clinicians organize and synthesize information into a clear case formulation. These "Ps" guide the clinician in identifying why a client is experiencing symptoms, what's keeping those symptoms going, and what strengths or supports could aid recovery.
While variations exist, the most widely used version includes four core components. Some clinicians also include a 5th "P" (Presenting Problem) as a foundation, and a 6th "P" (Plan) to guide interventions.
The 4 Ps
1. Predisposing Factors — Historical or biological factors that increase a person's vulnerability to developing a mental health condition. Why is this person at risk?
2. Precipitating Factors — Recent events or changes that triggered the current symptoms or episode. Why now?
3. Perpetuating Factors — Ongoing conditions or behaviors that maintain or worsen symptoms. What's keeping it going?
4. Protective Factors — Strengths, skills, supports, or conditions that reduce symptom severity or increase resilience. What can help?
How to Use the "Ps" in Your Assessment
During the clinical interview, ask targeted questions that correspond to each "P." Clinicians often organize intake findings using the 4Ps framework to guide case formulation and treatment planning.
CLINICAL FRAMEWORK
CASE FORMULATION EXAMPLE
Formulation Example Using the 4Ps
This framework allows the clinician to clearly show how past and present factors interact, and which elements can be targeted for intervention. For example, therapy may focus on exposure to avoided situations (perpetuating), building support networks (protective), and processing past trauma (predisposing).
How to Synthesize a Biopsychosocial Assessment Narrative
Synthesizing data from a biopsychosocial assessment into a clear, concise narrative is one of the most important — and challenging — skills for behavioral health clinicians. It transforms raw information into a clinical formulation that highlights what's driving the client's current struggles, what factors may help or hinder treatment, and how best to intervene.
A strong synthesis does more than restate facts. It weaves together biological, psychological, and social insights into a unified picture of the client's functioning, offering a foundation for diagnosis and treatment planning.
The "3 C's" Approach
Tips for Effective Synthesis
Avoid simply listing facts — focus on cause-effect relationships and interaction between domains. Use narrative, not bullet points; think like a case formulation, not a summary checklist. Balance breadth and focus: you don't need to mention every detail, just what's most relevant to diagnosis and treatment. And incorporate the client's voice — reflecting how the client understands their struggles builds alliance and clinical specificity.
Biopsychosocial Assessment Example
To bring all the elements together, here’s a sample biopsychosocial assessment written in a structured format. This example shows how information from the biological, psychological, and social domains can be integrated into a cohesive clinical narrative. It also follows a format commonly used in intake documentation across behavioral health settings.
Sample Biopsychosocial Assessment
Client Overview
Name: Maria L.
Age: 35
Date of Assessment: November 15, 2025
Referral Source: Self
Presenting Problem: Maria reports increased anxiety, difficulty sleeping, and persistent low mood over the past several months, affecting her work and personal life.
Biological
Maria has a history of hypothyroidism and seasonal allergies. She is currently prescribed levothyroxine 75 mcg daily. She denies any recent hospitalizations or surgeries. Sleep is disrupted (4–5 hours per night), and appetite is reduced. She does not use alcohol, tobacco, or recreational drugs. No known drug allergies. Family history includes depression (mother) and high blood pressure (father).
Psychological
Maria describes a pattern of persistent worry, fatigue, and occasional panic attacks. She reports difficulty concentrating and feeling overwhelmed at work. Symptoms began approximately six months ago following the loss of a close friend. She denies current suicidal ideation but has experienced passive thoughts of hopelessness. Maria was previously in therapy during college for mild depression. She identifies journaling and walking as helpful coping strategies. No history of psychiatric hospitalization.
Social
Maria lives alone in an apartment and works as a marketing coordinator. She reports a high level of job-related stress and limited work-life balance. She is close to her sister, who lives nearby, but reports minimal social interaction outside of work. She expresses interest in joining a support group but is unsure how to start. Financially stable with moderate student loan debt. No legal issues or military service. Identifies as Catholic but is not currently practicing.
Mental Status Exam
Client is alert, oriented x3, and appropriately groomed. Eye contact is limited but improves with rapport. Mood is described as "anxious and tired," with congruent affect. Speech is clear and goal-directed. No delusions or hallucinations noted. Thought content is focused on recent loss and work stress. Insight and judgment are fair.
Assessment and Plan
Maria presents with symptoms consistent with generalized anxiety disorder and possible adjustment disorder with depressed mood. Symptoms appear to be exacerbated by recent grief and occupational stress. She shows motivation to engage in therapy and has several protective factors, including stable housing and family support.
- Begin weekly individual therapy focused on anxiety management and grief processing
- Provide psychoeducation on GAD and healthy coping techniques
- Refer to the primary care physician for thyroid evaluation and sleep concerns
- Recommend support group options and assist with initial outreach
- Reassess symptom severity in 4 weeks using GAD-7 and PHQ-9
Would Your Assessment Pass a Review?
Evaluate your biopsychosocial assessment against the same standards used in utilization reviews.
This Biopsychosocial Assessment Stress Test checks your documentation across 25 critical elements—helping you identify what’s solid, what’s missing, and what could put reimbursement at risk.
Check Your Assessment Now →Takes about 6 minutes. Immediate results.
Tips for Writing a Biopsychosocial Assessment
A clear, well-structured biopsychosocial assessment helps other providers understand the client’s clinical picture, contributes to diagnostic accuracy, and supports coordinated care. Use the following tips to strengthen your assessment writing process.
The difference between weak and strong documentation often comes down to specificity, clinical language, and functional impact, as shown below.
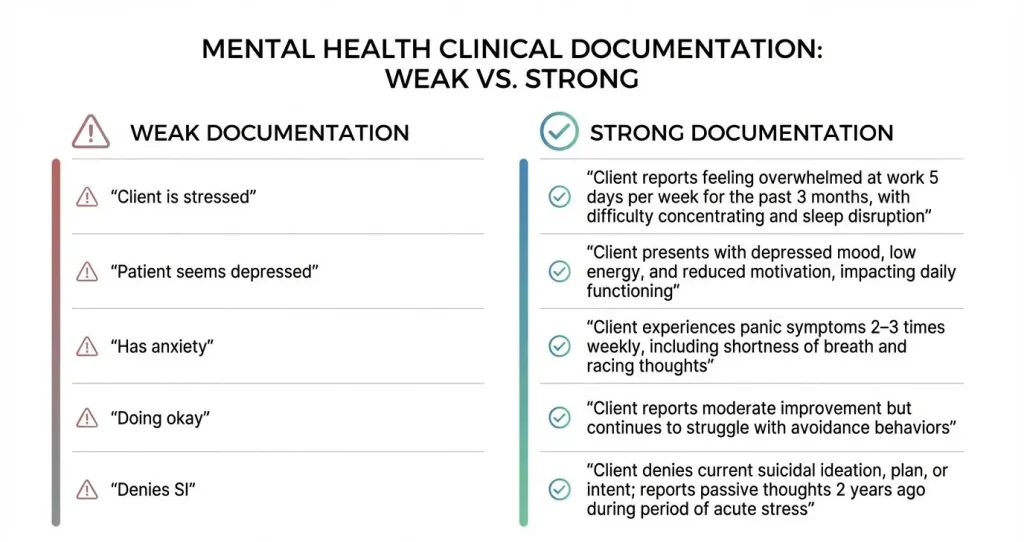
1. Distinguish Objective Facts from Subjective Impressions
Be intentional about separating what the client reports from your clinical observations.
- Objective information includes direct quotes, reported symptoms, or past diagnoses.
- Subjective impressions reflect your clinical judgment, such as observed affect, tone of voice, or behavior during the session.
Always clarify the source. For example:
- “Client reports difficulty sleeping for the past three months.”
- “Clinician observed flat affect and minimal eye contact.”
This distinction supports documentation accuracy and helps other providers interpret your findings.
2. Provide a Balanced Perspective
Your assessment should present a well-rounded view of the client’s functioning. Include not only symptoms and challenges but also protective factors, coping strategies, and personal strengths. This helps reduce stigma and supports a strengths-based, person-centered treatment approach.
3. Prioritize the Most Pressing Issues
Identify the most urgent or clinically significant concerns and lead with those. While all information is valuable, not every detail needs equal emphasis. Focus your narrative on the symptoms or factors that most directly impact functioning, safety, or treatment direction. For example, suicidal ideation, active substance use, or recent trauma may need deeper exploration and planning than more chronic, low-impact issues.
4. Ensure Clinical Accuracy
Your report may be referenced by other clinicians, case managers, or insurers. Be precise when summarizing symptoms, history, and treatment needs. Double-check that diagnoses are supported by the documented data and that terminology is used correctly. Avoid speculation, exaggeration, or assumptions. If a statement is based on the client’s report or your impression, make that clear in your wording.
5. Focus on Relevant Details
Keep your documentation concise by filtering out tangents or information that does not contribute to clinical understanding or treatment planning. It’s also acceptable if one area (biological, psychological, or social) yields less data.
6. Maintain Consistency with Findings
Make sure your narrative and diagnostic impressions align. If you diagnose major depressive disorder, your assessment should describe hallmark features like low mood, fatigue, guilt, sleep or appetite changes, or suicidal ideation. Inconsistent or vague notes can undermine the credibility of your documentation.
7. Clarify Ambiguous Responses
Clients may describe their experiences in broad or emotional terms. Ask gentle follow-ups to clarify duration, frequency, intensity, and impact.
For example:
- “I’m really stressed” becomes, “I feel overwhelmed at work 5 days a week, and it’s been building for 3 months.”
- “I’ve been down lately” becomes, “I’ve had low mood most days, and it’s starting to affect my appetite and motivation.”
These details strengthen your formulation and support an accurate diagnosis.
8. Use Standardized Assessment Tools When Appropriate
Supplementing your clinical interview with validated tools can improve reliability and objectivity. Commonly used tools include PHQ-9 for depression, GAD-7 for anxiety, K10 for psychological distress, MDQ for mood disorders, HAM-A for anxiety symptoms, and LEC-5 for trauma history. These instruments can support diagnosis, justify medical necessity, and help monitor change over time.
Related Clinical Assessment & Documentation Guides
Explore additional guidance on substance abuse assessment and treatment for behavioral health clinicians.
Using Technology to Simplify Documentation
Clinical documentation is a core part of behavioral health care, but it can be time-consuming without the right support. In addition to biopsychosocial assessments, providers often manage progress notes, treatment plans, consent forms, and other records that require accuracy, organization, and compliance.
ICANotes is a mental health EHR built to reduce your documentation burden. With ICANotes, you can:
- Scan and store digital forms
- Access records securely from any device
- Keep documentation organized and HIPAA-compliant
- Use prebuilt templates and auto-populate fields to save time
- Create accurate, legible notes that support better care and faster reimbursement
- Improve client satisfaction through a secure patient portal.
ICANotes helps you work more efficiently so you can focus more on clinical care.
Why Use ICANotes for Biopsychosocial Assessments?
ICANotes makes it easy to complete biopsychosocial assessments by allowing clients to enter their intake information through a secure, mobile-friendly form. This data flows directly into the clinician’s assessment note, reducing duplicate entry and saving time during documentation.
Clinicians can use ICANotes’ menu-driven templates to generate detailed, structured assessments with just a few clicks. Built-in tools like PHQ-9, GAD-7, and ASI scales are included to help collect standardized data and support compliance.
ICANotes helps behavioral health professionals document faster, reduce errors, and focus more on patient care. Start a 30-day free trial or schedule a demo to see it in action.
Build Complete, Audit-Ready Assessments—Without the Guesswork
ICANotes helps you create structured, compliant biopsychosocial assessments that meet documentation standards for medical necessity, audits, and reimbursement—every time.
With built-in prompts across all domains, embedded risk screening, and guided clinical formulation, you’ll document faster while ensuring nothing important gets missed.
- ✔ Structured templates covering all biopsychosocial domains
- ✔ Built-in risk & safety screening and MSE documentation
- ✔ Prompts that support medical necessity and defensible notes
- ✔ Complete assessments in minutes—not hours
No credit card required. Full access to all features.
Start Your Free Trial
Get started in minutes. No credit card required.
Frequently Asked Questions: Biopsychosocial Assessments
Related Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) from Aspen University and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.






