Blog > Treatment Strategies > Social Media Addiction Therapy: Evidence-Based Clinical Strategies
Social Media Addiction Therapy: Evidence-Based Clinical Strategies for Treatment
Social media addiction therapy is becoming an essential skill set for today’s mental health clinicians as digital addiction and excessive screen time increasingly impact client well-being. This guide explores evidence-based treatment approaches — including CBT-IA, motivational interviewing, exposure therapy, and ACT — to help clients manage phone addiction, reduce compulsive use, and build healthier digital habits. Learn how to create an effective digital wellness plan, incorporate screen time tracking, and support sustainable behavior change through digital detox strategies and values-based interventions.

Last Updated: May 4, 2026


What You'll Learn
- How to assess social media addiction, phone addiction, and digital addiction across the clinical continuum
- Evidence-based approaches for social media addiction therapy, including CBT-IA, ACT, motivational interviewing, and ERP
- The difference between phone addiction and platform-specific social media addiction — and how it impacts treatment
- How to design and implement a digital wellness plan that supports long-term behavior change
- When and how to use a digital detox as a structured clinical intervention
- How to use screen time tracking as a therapeutic tool to increase awareness and guide treatment
- Practical strategies and tools to reduce compulsive use and improve digital wellness
- How to manage relapse and support clients in building a sustainable, values-driven relationship with their devices
Contents
- The 6 Core ACT Processes
- 2 ACT Psychoeducation Tools Clients Actually Remember
- ACT Techniques for Depression You Can Use Right Away
- Case Vignettes: ACT Interventions for Depression in Context
- ACT Metaphors That Work Especially Well for Depression
- ACT and Suicidal Thoughts
- FAQ: ACT for Depression
- How ICANotes Supports ACT-Informed Depression Care
Social media addiction therapy is an increasingly critical area of clinical practice. As smartphones and social platforms become woven into daily life, mental health professionals are seeing more clients whose screen use has crossed the line from high engagement into compulsive, hard-to-control behavior. Clinicians now use terms like digital addiction and phone addiction to describe these overlapping presentations — and research and clinical experience offer several evidence-based strategies for treatment. These approaches help clients regain control, reconnect with their values, and rebuild the parts of life that excessive screen use has eroded.
This guide covers the leading therapeutic frameworks for treating social media addiction, phone addiction, and related forms of digital addiction, along with guidance on building a digital wellness plan, running a structured digital detox, and using screen time tracking as a clinical tool.
Social media addiction exists on a continuum from high engagement to behavioral addiction.
- High engagement: Frequent use without negative consequences
- Problematic use: Interference with sleep, mood, or relationships
- Behavioral addiction: Compulsive use despite harm, withdrawal-like symptoms
Understanding this distinction is essential for selecting the appropriate level of social media addiction therapy.
Understanding the Continuum: From High Engagement to Behavioral Addiction
High Engagement
Frequent digital use that remains balanced with responsibilities, relationships, and overall well-being.
Problematic Use
Screen time begins to interfere with sleep, mood, productivity, or relationships, but remains somewhat controllable.
Behavioral Addiction
Compulsive, hard-to-control use with withdrawal-like symptoms and continued engagement despite negative consequences.
Before selecting a treatment approach, clinicians need to accurately identify where a client falls on the technology use continuum. Not all frequent use is problematic — a college student who spends hours daily on digital design apps but still balances school, sleep, and relationships is highly engaged, not addicted.
Problematic use begins when screen time interferes with sleep, mood, productivity, or relationships, though the person can still reduce or modify their use with effort. A professional scrolling social media late into the night, causing fatigue at work and conflict with a partner, falls into this category.
Behavioral addiction involves compulsive, hard-to-control use with withdrawal-like symptoms and continued use despite serious consequences. A teen who feels anxious and irritable without gaming, skips meals and schoolwork, and keeps playing despite mounting consequences is exhibiting signs of behavioral addiction. Understanding this continuum guides both the intensity and type of social media addiction therapy you select. (For validated screening tools and a structured assessment framework, see our companion article, Technology Addiction Assessment Tools for Clinicians.)
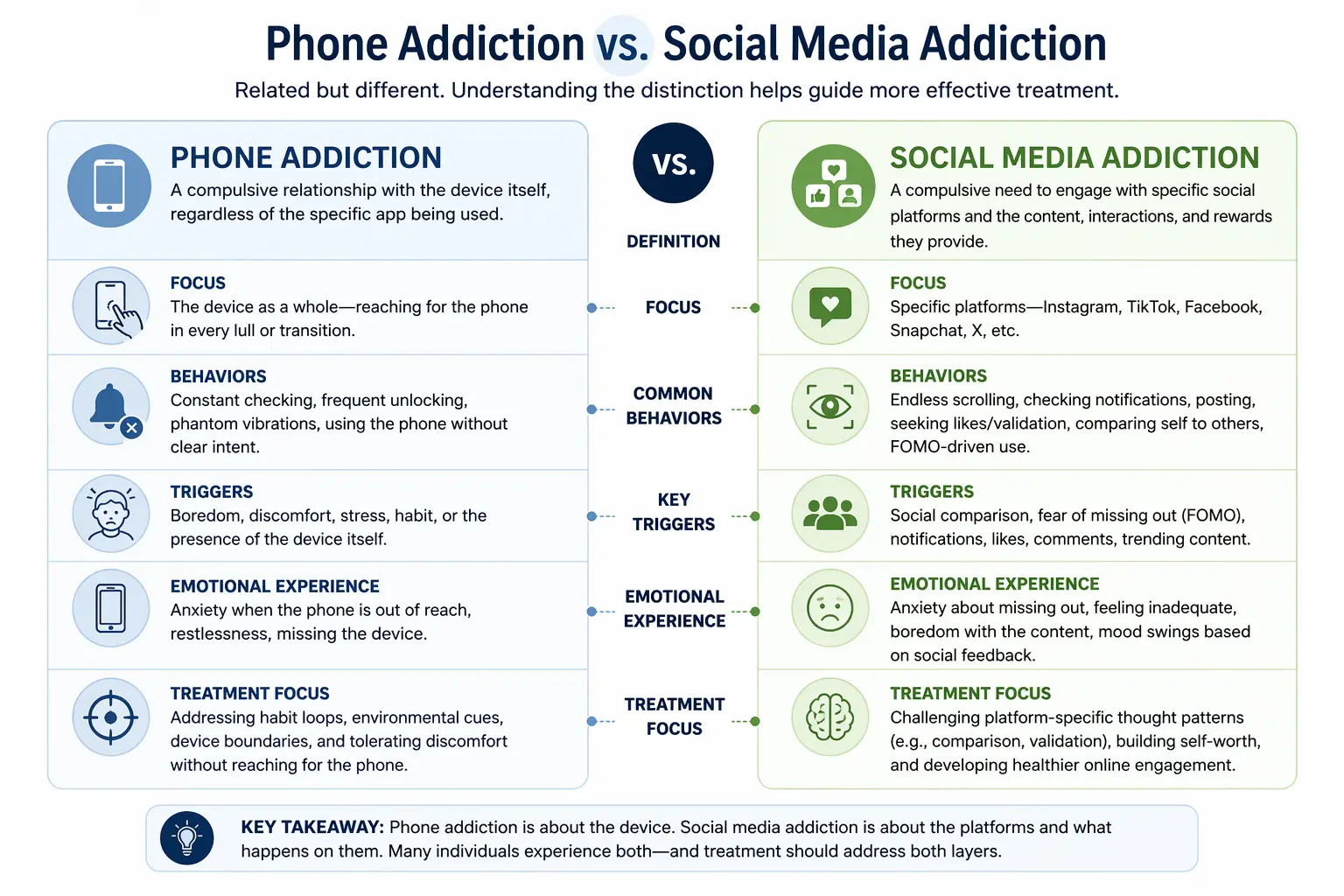
Phone Addiction as a Distinct Presentation
While social media addiction describes compulsive engagement with specific platforms, phone addiction captures something slightly different: a compulsive relationship with the device itself. Clients with phone addiction may not be drawn to any single app in particular. Instead, they reach for the phone during every lull, feel anxious when it's out of reach, check it dozens of times an hour without intent, and experience phantom vibrations or the urge to pick it up even when nothing has notified them.
Phone addiction and social media addiction often overlap, but they are worth distinguishing in assessment. A client whose primary concern is constant phone-checking may benefit more from interventions targeting environmental cues, habit loops, and boundary-setting around the device itself, while a client whose compulsive behavior centers on Instagram or TikTok may need more focused work on the cognitive distortions specific to social comparison and fear of missing out. Research on problematic smartphone use has found that device-level behaviors — unlocks per day, first-use-of-day, nighttime use — often predict functional impairment as reliably as total screen time (Busch & McCarthy, 2021).

Free Download: Technology Use Assessment Toolkit
Assess social media addiction, phone addiction, and digital overuse with a structured, clinician-ready toolkit designed for real-world practice.
- Clinical continuum: high engagement → behavioral addiction
- Seven-domain assessment checklist
- Validated screening tools
- Red flag indicators + session scripts
Takes less than 60 seconds to access.
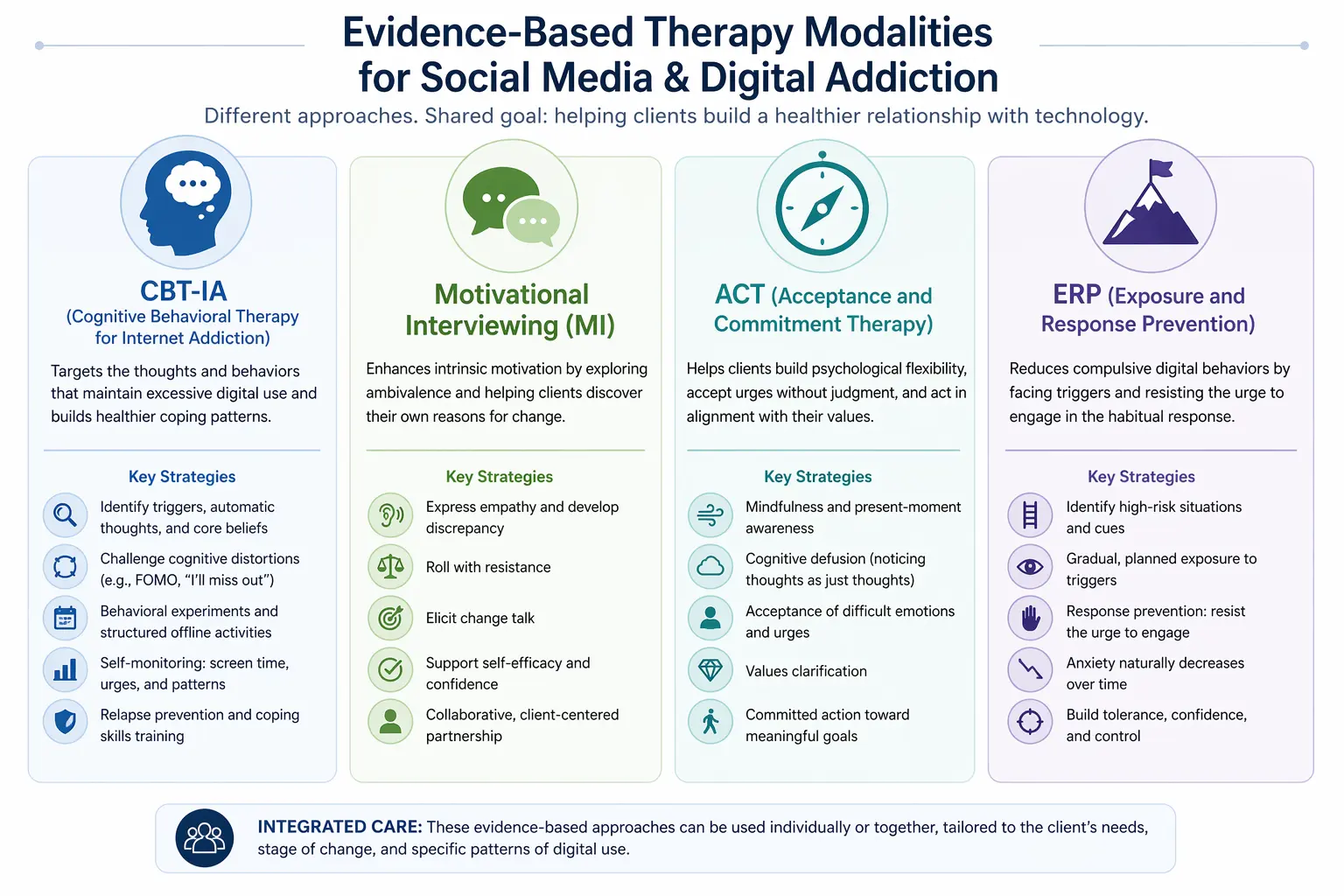
Evidence-Based Therapy Modalities for Social Media Addiction
No single therapeutic approach works for every client presenting with compulsive screen use. The modalities below are the most well-supported options in the current literature, and most clinicians end up drawing from several of them depending on the client's readiness for change, the specific behavior at the center of the problem, and whether family dynamics are part of the picture. Cognitive behavioral therapy and its internet-specific adaptation address the thought patterns and habits that sustain overuse. Motivational interviewing meets clients who are ambivalent about change. Exposure and response prevention builds distress tolerance for the moments when the urge to scroll or check is strongest. Acceptance and commitment therapy reframes the work around values rather than elimination. Family-based interventions and reality therapy add essential leverage when a client's use is entangled with relationships or unmet needs. What follows is a practical look at each, with clinical examples you can adapt to your own caseload.
CBT and CBT-IA for Social Media Addiction
Cognitive behavioral therapy — particularly the internet addiction adaptation known as CBT-IA — is among the most well-researched approaches for digital addiction treatment. CBT-IA was developed specifically for internet-related compulsive behaviors and targets the cognitive distortions and behavioral patterns that maintain overuse.
In practice, this looks like helping a young adult who compulsively checks social media identify the triggers and thought distortions driving their behavior. A client might believe, “If I don’t post, I’m missing out,” or “Everyone is watching to see if I respond.” The therapist works to surface these cognitions, challenge their accuracy, and develop adaptive coping strategies. Mindfulness exercises increase awareness of urges, while acceptance-based strategies reduce the judgment and shame that often accompany problematic use.
CBT-IA also emphasizes behavioral interventions such as self-monitoring screen time, logging urges, and scheduling structured offline activities. A college student might track daily screen time, note the triggers that lead to excessive scrolling, and set app timers to reinforce healthier boundaries.
Motivational Interviewing for Digital Behavior Change
Motivational interviewing (MI) is a natural fit for social media addiction therapy because it was originally designed to address ambivalence in addiction treatment. Many clients with problematic technology use are not fully committed to change — they enjoy being online, it helps them relax, and at the same time they feel drained, distracted, or more anxious afterward. MI provides a framework for exploring that ambivalence without pushing the client into resistance.
Consider a client who spends hours gaming and expresses mixed feelings about cutting back. Through MI, the therapist explores the ambivalence, elicits the client’s own reasons for change, and reinforces intrinsic motivation to regain time for work and relationships. The goal is not to tell the client what to do, but to help them discover their own motivation.
Clinicians can use MI scripts such as:
- “It sounds like part of you enjoys being online — it helps you relax and stay connected. And at the same time, there’s another part of you that feels drained afterward. Would it be okay if we explored that ambivalence together?”
- “What do you wish your relationship with your phone looked like? If you could change one part of your screen use, what would it be?”
- “When you imagine your life with a bit more control over your screen use — more calm, more presence, more time — what emotions come up for you?”
Exposure Therapy and Response Prevention for Screen Overuse
Exposure and response prevention (ERP) — traditionally associated with OCD treatment — is emerging as a valuable tool in treating digital addiction and phone addiction. The goal is to reduce compulsive use by gradually exposing clients to triggers while preventing the habitual escape behavior (checking, scrolling, gaming).
Clinicians create an exposure hierarchy, starting with the least distressing task and progressing upward. For a client struggling with social media, the first step might involve checking a notification but waiting ten to fifteen minutes before responding, using mindfulness to manage anxiety. For gaming, exposure therapy could start with sitting at the computer during usual gaming hours without logging in, practicing what’s known as urge surfing — riding the wave of the urge without acting on it.
For online shopping addiction, exposure exercises might involve opening the shopping app, browsing for a short period, and closing it without making a purchase while using coping strategies. The intention is not to cut the person off from their devices entirely. Rather, it’s to build their capacity to sit in discomfort and discover that they can tolerate not engaging in the compulsive behavior. Many clients find that through these experiments, they realize they can survive — and even thrive — with more space from their devices.
Acceptance and Commitment Therapy (ACT) for Compulsive Digital Use
ACT offers a values-driven framework for social media addiction therapy that focuses on building psychological flexibility rather than simply eliminating behavior. The core idea is that clients learn to notice urges to scroll or check their phones without automatically obeying those urges, then redirect their energy toward actions aligned with their values.
ACT’s six core processes apply directly to technology overuse:

- Present-moment awareness: Help clients notice automatic scrolling and “time loss” on screens. Use 20–30 second mindful check-ins before and after screen use.
- Cognitive defusion: Help clients step back from sticky thoughts like “I need to check” or “I’ll miss out.” Techniques include labeling thoughts (“I’m having the thought that I need to check right now”) and the silly voice technique.
- Acceptance: Allow difficult feelings — loneliness, boredom, anxiety — to exist without escaping into screens. “Instead of fighting the urge to pick up your phone, what if we made space for that urge? Let it rise and fall like a wave, without obeying it.”
- Self as context: Build an observing self separate from urges, likes, and notifications. “Notice there’s a part of you that experiences the craving to scroll — and another part that notices the craving. That noticing part doesn’t have to act on the urge.”
- Values clarification: Explore what excessive screen use pulls clients away from. “How aligned is your screen use with the person you want to be?”
- Committed action: Create small, values-aligned experiments — phone in a separate room at night, a 10-minute pause before social media, or intentional check-in times.
ACT metaphors can be especially powerful in this context. The "social media hook" metaphor compares apps to fishing hooks — bright, shiny, baited with rewards. Being hooked isn't a character flaw; it means the bait worked. ACT helps clients unhook by noticing it's in their mouth, relaxing their jaw, and gently unhooking so they can swim where they actually want to go.
Family-Based Interventions and Reality Therapy
When a teen's device use is causing conflict at home, family-based interventions are essential. The therapist works with parents and the teen to set mutually agreed-upon limits, improve communication, and create offline family routines. Parents are encouraged to model healthy screen behavior, since parental patterns strongly shape youth habits.
Resources like ScreenSanity — a nonprofit created by two mothers concerned about their own children's problematic screen use — offer parent guides, values exercises, and structured tools like the Plugged-In Planner for children through middle school. Clinicians working with families can recommend these materials to support boundary-setting between sessions.
Reality therapy, grounded in choice theory, is another effective approach. It guides clients to examine the unmet needs behind their digital use — belonging, fun, achievement, freedom — and plan concrete actions that satisfy those needs in healthier ways. A client who excessively shops online might discover that the behavior is driven by loneliness, then work with the therapist to find alternative ways to fulfill that need for connection.
Digital Detox as a Clinical Intervention
A digital detox — a structured, time-limited period of reduced or eliminated screen use — can be a powerful clinical intervention when used thoughtfully. Outside of therapy, the term has become associated with wellness retreats and pop-culture purity challenges, but in a clinical context, a digital detox is best understood as an experiment: a collaborative test that generates data about a client's relationship with their devices, and that builds evidence of their capacity to tolerate discomfort without escaping into a screen.

When a Digital Detox is Appropriate
A digital detox is most useful when a client is curious about what their life looks like without constant screen engagement, when they want to interrupt a compulsive pattern and create a clean starting point for new habits, or when the overwhelm of their current screen use is making smaller, gradual changes feel impossible. It is less appropriate when a client's online engagement is tied to a primary source of social support (for example, an isolated client whose only meaningful community is online), when device removal would increase safety risk, or when the client has not yet agreed that a change is warranted — a detox imposed without buy-in tends to generate rebound use.
Designing a Structured Digital Detox
Clinicians can collaboratively design a detox with the client rather than prescribing one. A workable structure includes:
- Scope. Which devices, apps, or platforms are included? A full phone detox is one option; a narrower detox from social media apps while keeping texting and calls is often more realistic.
- Duration. Common lengths include a 24-hour detox, a weekend detox, or a structured week. Shorter detoxes are more likely to be completed and still yield useful data.
- Replacement activities. What will fill the time? Clients should plan replacement activities aligned with their values—a walk with a friend, a creative project, sleep, time outdoors—rather than white-knuckling through unstructured hours.
- Support structure. Who knows about the detox? What does the client do when urges spike? A coping plan for hard moments prevents a single craving from ending the experiment.
- Post-detox review. The real clinical value of a digital detox often shows up afterward, when the client reviews what they noticed, what was harder or easier than expected, and what they want to carry into their ongoing digital wellness plan.
Research on digital detox interventions shows mixed but promising results. A systematic review by Radtke and colleagues (2022) found that while studies vary widely in design and outcomes, participants frequently report improvements in mood, sleep, and sense of presence — particularly when detoxes are paired with reflection or structured support. Clinicians should set realistic expectations with clients: a detox is rarely a cure, but it is often a catalyst.
What is Digital Wellness?
Digital wellness refers to the intentional and balanced use of technology in ways that support mental, emotional, and physical well-being.
Rather than eliminating technology, digital wellness helps clients build awareness of how screen time and digital habits affect their lives — and make intentional changes aligned with their values.
From a clinical perspective, digital wellness reframes treatment goals. Instead of focusing only on reducing use, clinicians help clients develop sustainable habits that improve functioning and quality of life.
Building a Digital Wellness Plan
Across every modality described above, effective treatment tends to converge on the same practical deliverable: a written, collaboratively-built digital wellness plan. Rather than framing success as the elimination of bad habits, a digital wellness plan centers what a healthy relationship with screens looks like for this particular client — aligned with their values, sensitive to the real role digital tools play in their life, and specific enough to act on.
A useful plan typically includes five components:
1. Self-Assessment
Review current screen time, most-used apps, triggers, and how the client feels before, during, and after digital use.
2. Values Clarification
Identify what matters most and explore what excessive screen use is pulling the client away from in daily life.
3. Goals and Boundaries
Set specific changes such as device-free times, device-free zones, app limits, and intentional check-in windows.
4. Tools and Supports
Add supports like screen time tracking, app blockers, mindfulness tools, and environmental changes that reduce friction.
5. Review and Adjust
Revisit the plan regularly, review progress, and refine goals based on what is working and where the client is getting stuck.
- Self-assessment. A snapshot of current use—typical daily screen time, most-used apps, time of day and emotional state around peak use, and a brief log of how the client feels before, during, and after screen sessions.
- Values clarification. What does the client want their life to look like? What are they missing because of current screen use, and what would they move toward if they had the time and attention back?
- Goals and boundaries. Concrete, specific changes: device-free zones (the bedroom, the dinner table), device-free times (the first hour of the day, after 9 p.m.), app-specific time limits, and intentional check-in windows rather than constant availability.
- Tools and supports. Which apps, environmental changes, and behavioral strategies the client will use to support the plan (detailed below).
- Review cadence. When and how the client will review their progress—weekly self-check, monthly review in session, and planned adjustments.
Presented this way, a digital wellness plan is not a restriction list; it is a design document. It gives clients a framework for intentional choice and a baseline to return to when they drift.
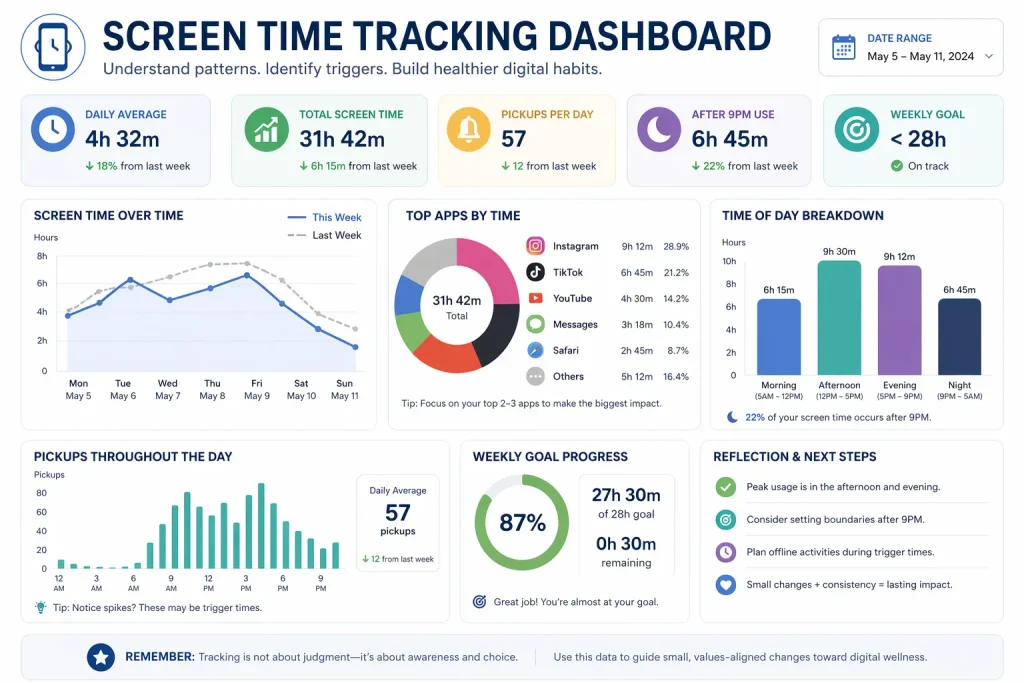
Screen Time Tracking as a Clinical Tool
Screen time tracking deserves its own focus within any digital wellness plan. Built-in features on most modern devices — Apple's Screen Time and Google's Digital Wellbeing — generate detailed data on total screen time, pickups, first-use-of-day, per-app time, and notification volume. Used well, this data transforms a vague sense that "I'm on my phone too much" into something clients can see, discuss, and respond to.
A few practical notes for clinicians:
- Self-report is unreliable. A systematic review and meta-analysis by Parry and colleagues (2021) found meaningful discrepancies between how much screen time people report and how much their devices actually log, with most people underestimating. Pulling the live data together in session is almost always more useful than asking.
- Pickups and first-use matter as much as total time. A client who uses their phone two hours a day but picks it up 150 times has a very different pattern than one who uses it two hours in a few focused blocks. First-use-of-day — the moment the phone enters the morning — often correlates strongly with how the rest of the day unfolds.
- Frame the data without shame. Screen time reports can trigger self-criticism that shuts down curiosity. Introduce the data as information, not a verdict. Focus on what the numbers reveal about triggers, routines, and values — not on whether a given number is "good" or "bad."
- Review the data together. Some of the most useful clinical moments come from looking at the week's screen time report together in session, noticing what stands out to the client, and deciding on one small experiment for the coming week.
Other Behavior Change Tools
Screen time tracking is most powerful alongside other practical supports:
App and Website Blockers
Tools like Freedom, StayFocusd, and Cold Turkey can temporarily block distracting apps or sites, reducing decision fatigue in high-risk moments.
Habit Tracking and Self-Monitoring
Apps like Habitica help clients track urges, mood, and triggers to identify patterns beyond raw usage data.
Physical and Environmental Strategies
Placing devices in another room, switching the phone to grayscale to reduce visual stimulation, and charging the phone outside the bedroom can all help reduce compulsive use.
Mindfulness and Meditation Apps
Headspace and Calm support the mindfulness practice that underpins many of the clinical techniques described above.
Notification Management
Turning off non-essential notifications reduces the constant prompts that trigger habitual checking, and is often the single highest-leverage change a client can make.
These tools work best when paired with values-based reflection. A client who identifies creativity and connection as core values might replace late-night scrolling with painting and weekly calls to a friend — aligning their behavior with what matters most to them.
Managing Relapse and Maintaining Progress
Just as with substance use disorders, relapse is a normal part of recovery from compulsive digital use. Clients should be prepared for setbacks, and clinicians should normalize them rather than treat them as failures. When a client relapses into late-night gaming after a stressful week, the therapist explores the triggers, validates the difficulty, and collaboratively plans strategies to reduce future relapses.
Ongoing monitoring is essential. Revisiting screen time data, mood logs, and the digital wellness plan at regular intervals helps clients track their progress and adjust interventions as needed. Web-based and app-based support interventions — such as mindfulness apps for managing urges or online support forums for individuals reducing screen time — can complement in-person therapy and provide continuity between sessions.
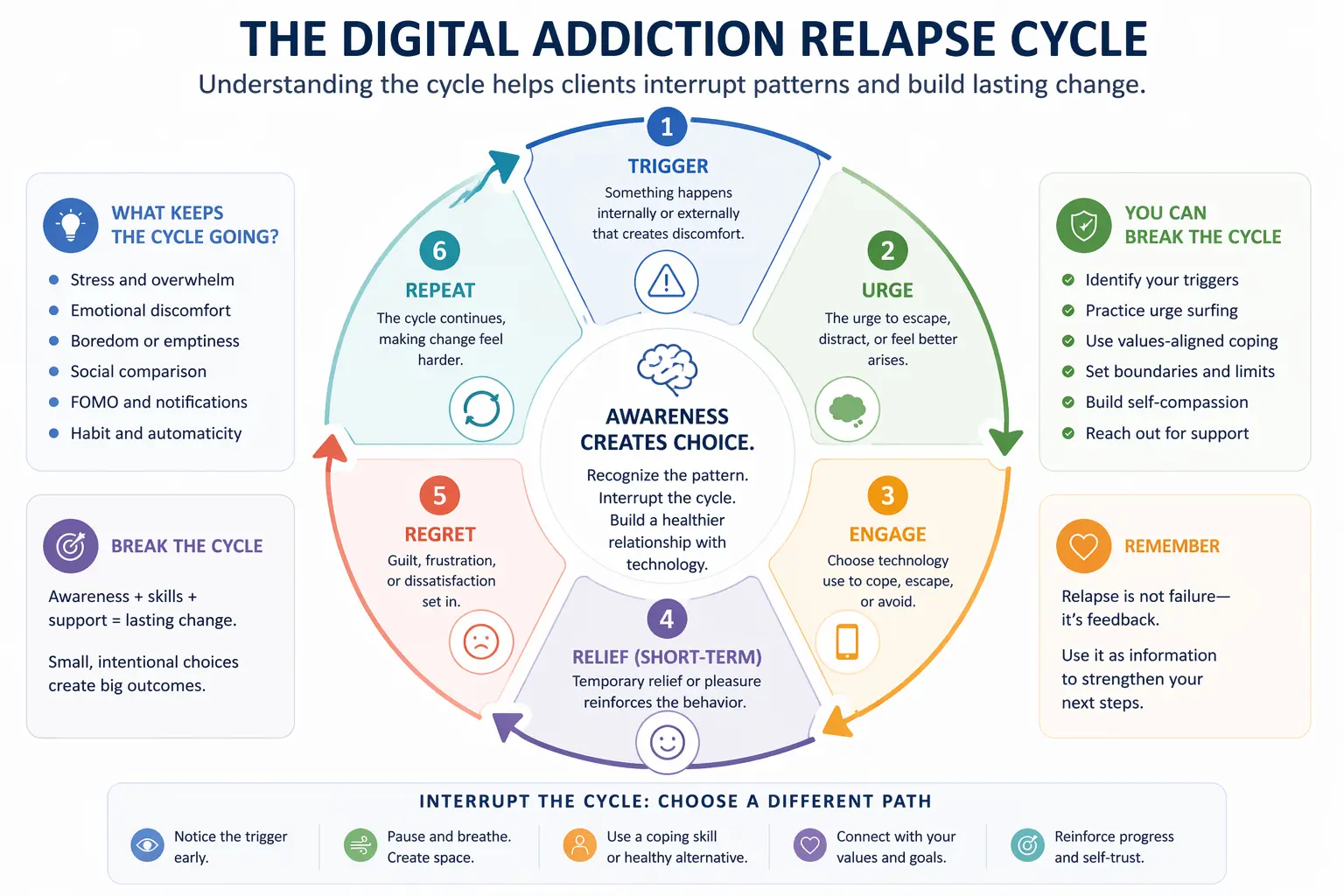
The visual below illustrates the relapse cycle commonly seen in digital addiction and highlights where clinicians can intervene.
Getting Started: Integrating Social Media Addiction Therapy Into Your Practice
The first step in effective treatment is thorough assessment. Before selecting interventions, clinicians need a clear picture of a client's digital use patterns, functional impact, level of control, emotional drivers, and readiness for change. Our companion article on assessment tools for clinicians provides a detailed guide to validated screening instruments, structured assessment frameworks, and a clinical continuum table you can use at intake and throughout treatment.
With the right assessment in place, clinicians can match the appropriate level and type of intervention to the client's needs — CBT-IA for a young adult compulsively checking social media, motivational interviewing for a gamer who's ambivalent about change, family-based interventions for a teen in conflict with parents over device use, a structured digital detox to interrupt a compulsive pattern, or an ACT-based approach that builds psychological flexibility and values-aligned action. In most cases, the therapeutic work is anchored by a collaboratively-built digital wellness plan that keeps progress visible and intentional, supported by honest screen time tracking between sessions.
Digital devices and social platforms are not going away. The goal of social media addiction therapy is not to eliminate them from a client's life, but to help them develop a healthier, more intentional relationship with screens — one that supports rather than undermines their well-being, their relationships, and the life they want to live.
Frequently Asked Questions: Social Media Addiction Therapy
Related Resources for Technology Addiction Assessment and Treatment
Anxiety Assessment Tools
Explore validated screening tools and how to interpret results in clinical practice.
Depression Assessment Tools
Learn how to assess depression using structured tools and clinical frameworks.
How to Write a Biopsychosocial Assessment
Build comprehensive intake assessments that support diagnosis and treatment planning.
Strength-Based Assessment in Mental Health
Learn how to incorporate strengths into your clinical assessment process.
Identifying and Treating Gaming Addiction
Understand assessment and treatment strategies for gaming-related behavioral addiction.
Treating Co-Occurring Disorders
Explore how to address underlying conditions that drive technology addiction.
Behavioral Health Documentation Best Practices
Improve documentation quality, compliance, and clinical clarity in your notes.
Technology Addiction Assessment & Treatment
Assess and treat technology addiction with validated tools and screening frameworks.
How ICANotes Supports Clinicians in Documenting Social Media Addiction Therapy
Effective social media addiction therapy doesn’t stop at intervention — it requires clear, compliant, and clinically meaningful documentation. As digital addiction and phone addiction become more common in practice, clinicians need efficient ways to capture complex behavioral patterns, justify medical necessity, and track progress over time. This is where ICANotes can play a valuable role.
ICANotes is designed specifically for behavioral health, making it easier to document the nuances of technology-related concerns within structured clinical workflows. Instead of starting from a blank page, clinicians can use pre-built templates and guided prompts to quickly capture key elements of social media addiction therapy, including presenting problems, functional impairments, and contributing factors such as excessive screen time or compulsive phone use.
Structured Documentation for Digital Addiction
ICANotes supports detailed documentation of digital addiction by helping clinicians:
- Clearly describe patterns of social media use, phone addiction, and screen time behaviors
- Document functional impairments (sleep disruption, mood changes, relationship strain, productivity issues)
- Capture client-reported triggers and emotional drivers (e.g., boredom, anxiety, social comparison)
- Link symptoms and behaviors to diagnostic criteria and medical necessity
This level of structure is especially important for audits, utilization reviews, and reimbursement—areas where vague documentation can lead to denials.
Efficient Progress Notes for Ongoing Treatment
As treatment progresses, ICANotes allows clinicians to efficiently document interventions across modalities such as CBT-IA, ACT, motivational interviewing, and exposure therapy. Clinicians can:
- Record specific interventions used (e.g., cognitive restructuring, urge surfing, values clarification)
- Track client response to digital detox experiments or digital wellness plans
- Document measurable progress using screen time tracking data and behavioral goals
- Maintain consistency across sessions without duplicating effort
This helps ensure that progress notes clearly demonstrate ongoing medical necessity and clinical improvement.
Supporting Digital Wellness Plans and Treatment Planning
ICANotes also streamlines treatment planning for digital addiction by enabling clinicians to:
- Create structured goals tied to digital wellness plans
- Document behavioral targets such as reduced screen time or improved boundaries
- Track adherence to interventions like app limits, device-free routines, and notification management
- Update treatment plans as clients progress or encounter setbacks
Because these plans are documented within the same system as progress notes, clinicians maintain a clear, cohesive record of care.
From Social Media Addiction Therapy to Audit-Ready Notes — In Minutes
Treating social media addiction, phone addiction, and digital addiction is only part of the work. Clear documentation is what supports reimbursement, compliance, and continuity of care.
ICANotes helps you translate CBT-IA, ACT, motivational interviewing, digital detox strategies, and digital wellness plans into structured, defensible documentation in minutes.
- Pre-built templates for digital addiction treatment
- Structured notes that support medical necessity
- Tools to track screen time and behavioral progress
- Faster documentation with clinically relevant language built in
Start your free 30-day trial — no credit card required.
Takes less than 60 seconds to get started
Recent Posts
About the Author
Diane Bigler, LCSW, LSCSW, is a Licensed Clinical Social Worker in Missouri and Kansas with over 25 years of experience in the mental health field. She has held clinical positions as an outpatient and in-home therapist and clinical supervisor in diverse settings. Diane was an Adjunct Professor of Social Work for 10 years at The University of Kansas, School of Social Welfare and a Field Liaison and Field Instructor. She has also held administrative positions as a Program Director and Coordinator. Diane is a popular local and national trainer on a wide variety of mental health and workplace development topics for clinicians and corporations and has facilitated over 500 training courses in the last few years. Visit her website http://www.






What is Social Media Addiction?