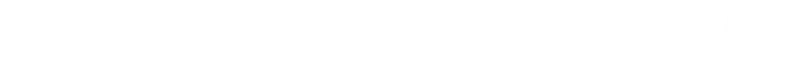Purpose-Built
Psychiatry EHR Software
ICANotes is psychiatry EHR software built from the ground up for psychiatric workflows — not adapted from a general medical platform. Psychiatrists and PMHNPs use it to write narrative psychiatric evaluations, progress notes, and medication management visits in minutes using menu-driven templates. Integrated e-prescribing with EPCS and PDMP, automated E&M coding, and built-in billing tools make ICANotes a complete psychiatric EMR for solo practices, group practices, and multi-site programs alike.

Built for Every Psychiatric Setting
Tailored tools for every type of psychiatric professional, clinical setting, and workflow
For Psychiatrists
ICANotes delivers a psychiatry EHR built around how psychiatric workflows actually work — specialty-specific menu-driven templates, integrated e-prescribing and medication management, electronic lab orders, and audit-ready documentation that saves time and supports compliance.
Psychiatric Nurse Practitioners
ICANotes streamlines med management visits with customizable note templates, rating scales, and eRx tools — while also supporting supervisory and collaborative workflows so physicians and NPs can document seamlessly together.
Inpatient & Residential Settings
ICANotes empowers multidisciplinary teams with group and shift notes, treatment team planning, medication administration records, SUD workflows, and compliance features tailored for psychiatric hospitals and residential treatment centers.

Why Psychiatrists Choose ICANotes Over General-Purpose EHRs
Tailored to psychiatrists and PMHNPs
ICANotes was designed from the ground up for behavioral health — not adapted from a general medical platform. Unlike general medical systems, our platform includes psychiatry-specific note templates, a library of rating scales, and features that reflect the real workflow of psychiatrists and psychiatric nurse practitioners. The result: faster notes, greater accuracy, and documentation that pays for itself in time saved.
Customizable Menu-Driven Note Templates
Ready-to-use menu-driven templates for rapidly writing narrative psychiatric evaluations, progress notes, and treatment plans. Automatic E&M coding to the highest reimbursable code supported by your note.
Powerful Integrated Medication Management & Labs
Integrated e-prescribing with in-workflow PDMP checks and support for controlled substances. Order labs and receive results electronically.
Practice Management & Patient Engagement
HIPAA-compliant portal, telehealth, scheduling, and billing, all in one place.
Key Psychiatry EHR Software Features That Work for You
ICANotes gives psychiatric professionals the psych EMR tools to work faster, communicate better, and focus on patient care.
Faster Charting
Write psychiatric evaluations, progress notes, and treatment plans in minutes using smart templates that reduce typing and improve consistency.
Medication Management
Integrated e-prescribing with EPCS for controlled substances, in-workflow PDMP checks, and drug-drug interaction checks. Lab ordering and results integration for medication monitoring.
Secure Patient Portal
Fully digital intake pre-populates your initial psychiatric evaluation with history information and rating scale scores. Share documents and message patients securely. Send patient statements to the portal and accept online payments.
Integrated Billing
Maximize reimbursement, reduce claim errors, and simplify revenue cycle management with fully integrated billing tools. Submit claims electronically, auto-post payments, and access optional full-service RCM support.
Privacy & Security
Protect patient data with encrypted backups, cloud access, and user permissions that meet HIPAA standards.
Telehealth
Start video visits from your calendar and document in real time using integrated, HIPAA-compliant telehealth tools.
A Psych EMR Designed for Faster, Smarter Charting
ICANotes offers a menu-driven psych EMR that turns clicks into complete, narrative notes. Psychiatric evaluations, treatment plans, and progress notes can be documented in minutes, freeing you from typing and reducing after-hours charting. Key details carry over from previous notes so everything stays connected and consistent. Whether you’re seeing patients in-person or via telehealth, ICANotes ensures your documentation is fast, accurate, and compliant. Watch our video to see how a med management note can be written in 2 minutes.
Why Psychiatrists Choose ICANotes
ICANotes supports your practice with a psychiatric EMR built to reduce admin time and enhance clinical excellence.
Fast, Narrative Psychiatric Documentation
ICANotes' menu-driven templates generate complete, narrative-style psychiatric evaluations, progress notes, and med management visits with clicks — no dictating, no blank-page typing. Most clinicians complete a standard psychiatric progress note in under three minutes. Key details carry forward automatically between visits, keeping documentation consistent and connected across the chart.
Integrated Medication Management & e-Prescribing
Prescribe directly from within the psychiatric note with full EPCS support for controlled substances. ICANotes performs PDMP checks inside the workflow, runs drug-drug and drug-allergy interaction checks, and allows you to order labs and receive results electronically — all without leaving the chart. Medication history pulls forward automatically to support continuity across visits.
Audit-Ready Compliance for Psychiatric Practices
ICANotes is ONC-certified under the 2015 Edition Cures Update and supports MACRA and MIPS reporting. Documentation templates are aligned with DSM-5 and ICD-10, and automatic E&M coding assigns the highest reimbursable code supported by your documentation — so you're never leaving money on the table or vulnerable to a payer audit. Psychotherapy notes are stored separately from general health records in accordance with HIPAA privacy requirements.
Psychiatry Billing Software Built Into the EHR
ICANotes connects clinical documentation directly to your billing workflow. Submit CMS-1500 claims electronically, verify insurance eligibility in real time, and auto-post ERAs and EOBs. Automated E&M coding and built-in compliance checks reduce claim denials before they happen. Practices that need additional support can access full-service revenue cycle management through ICANotes, with specialists who understand behavioral health billing.
Full Practice Management for Psychiatric Professionals
Scheduling, telehealth, a patient portal, automated appointment reminders, and HIPAA-compliant messaging are all built into ICANotes — no third-party add-ons needed. Patients complete digital intake forms before their first visit, and the information pre-populates your initial psychiatric evaluation automatically. For telehealth visits, you can document in real time within the same interface, and prescribe from within the note.
Expert 24x7 Support
ICANotes provides live phone and chat support around the clock — staffed by people who understand behavioral health workflows, not generic help desk scripts. Every new practice receives a personalized onboarding plan and 1:1 training for clinicians and staff, with a full library of self-guided resources available anytime.
Frequently Asked Questions: Psychiatry EHR Software
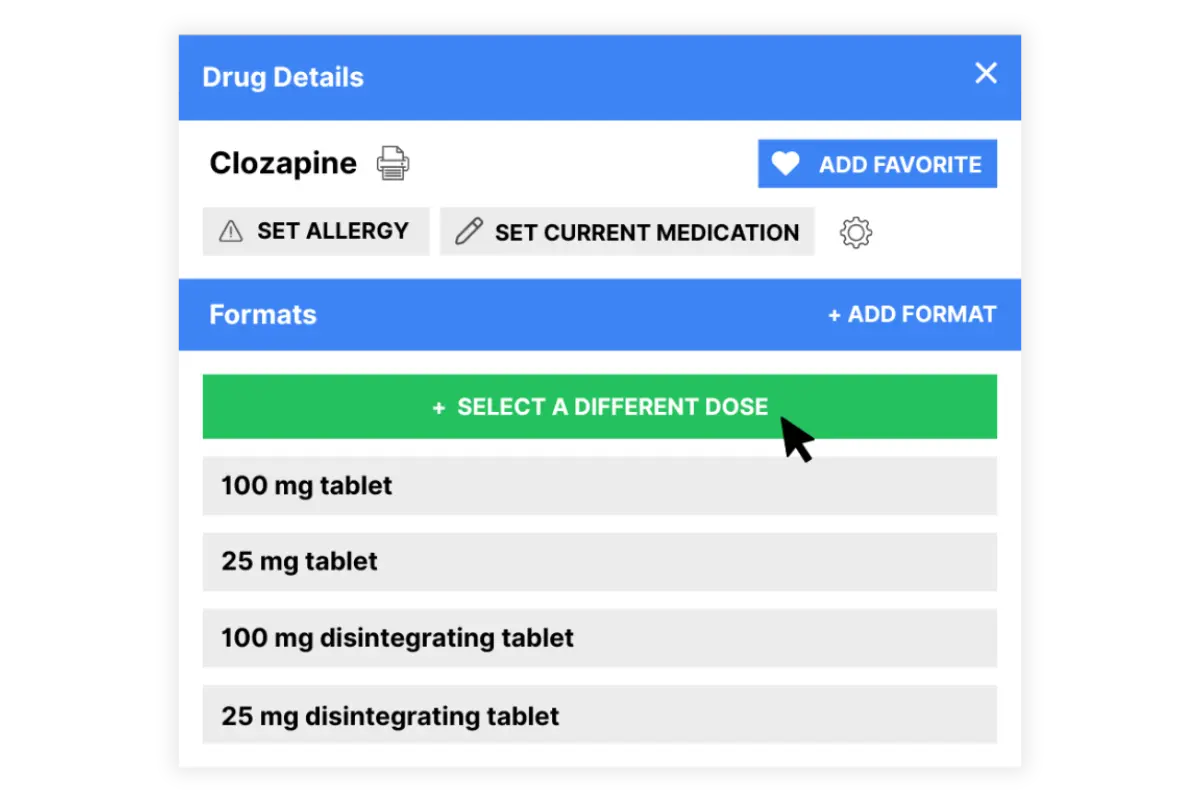
What is a Psychiatry EHR?
A psychiatry EHR (electronic health record) is software designed specifically to meet the clinical, documentation, and compliance needs of psychiatrists and psychiatric nurse practitioners. Unlike general medical systems, a psychiatric EMR includes specialty-specific templates for evaluations, mental status exams, and progress notes, along with integrated tools for medication management, e-prescribing, and outcome tracking. The best EHR for psychiatry also supports secure telehealth, patient engagement through a portal, and audit-ready documentation that satisfies payer and regulatory requirements.
Try ICANotes: Transform Your Psychiatric Charting
Experience how fast and intuitive psychiatric charting can be. View more mental health charting examples, schedule a live demo, or start your free trial today.
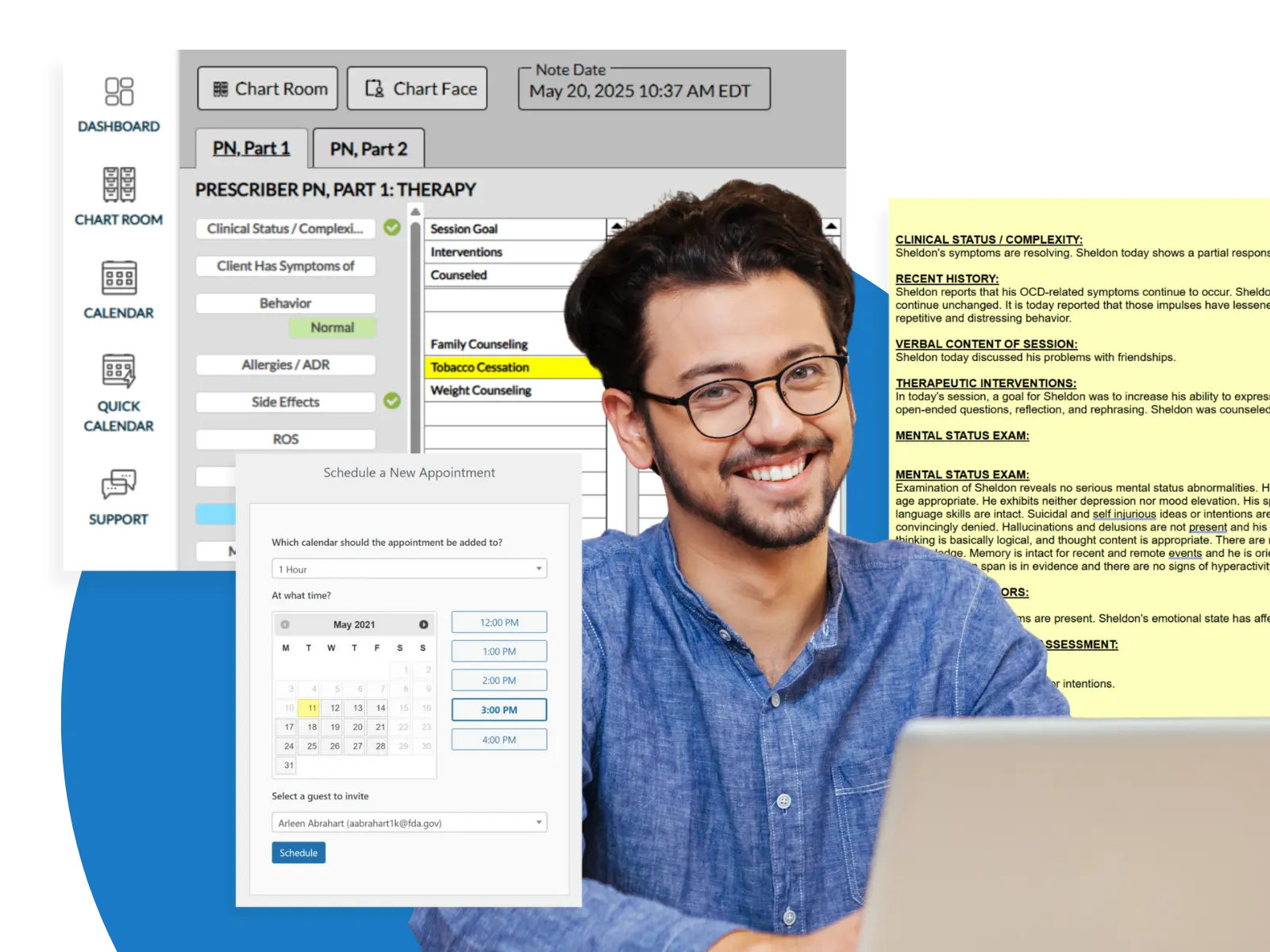
Schedule a Live Demo
Experience ICANotes — a clinically robust EHR built specifically for behavioral health, with narrative documentation tools, compliance support, and integrated billing in one platform.
- Simplify clinical charting
- Stay organized with appointment scheduling
- Reduce no-shows with automated reminders
- Improve client engagement with a secure patient portal
- Provide flexible care with HIPAA-compliant telehealth
Simplify clinical charting
Stay organized with appointment scheduling
Reduce no-shows with automated reminders
Improve client engagement with a secure patient portal
Provide flexible care with HIPAA-compliant telehealth