Blog
EHR Cost: What Mental Health Providers Can Expect to Pay in 2025
EHR Cost: What Mental Health Providers Can Expect to Pay in 2025 If you’re a mental health provider, choosing the right electronic health record (EHR)…
Top Evidence-Based Supplements for Mental Health
Top Evidence-Based Supplements for Mental Health: Adjunctive Nutraceutical and Lifestyle Interventions This evidence-based guide explores top adjunctive supplements and lifestyle interventions for enhancing mental health…
Clinical Documentation Tips for Passing a Behavioral Health Utilization Review
Clinical Documentation Tips for Passing a Behavioral Health Utilization Review Behavioral health utilization reviews can disrupt care and reimbursement if your documentation doesn’t hold up…
Navigating Boundaries and Building Trust: Working with Clients with BPD
Navigating Boundaries and Building Trust: Clinical Strategies for Working with Clients with Borderline Personality Disorder This blog post explores evidence-based strategies for addressing BPD and…
Mental Health Discharge Summary Sample & Template | Free Examples
Mental Health Discharge Summary Sample and Template: What “Good“ Looks Like A mental health discharge summary is a critical clinical document that outlines a client’s…
Why Narrative Behavioral Health Progress Notes Matter
Why Narrative Behavioral Health Progress Notes Matter: How ICANotes Makes Charting Effortless and Accurate In a digital world filled with checkbox templates and time-consuming clinical…
Informed Consent and AI in Healthcare: Ethical Considerations for Behavioral Health Providers
Informed Consent and AI in Healthcare: Ethical Considerations for Behavioral Health Providers The integration of artificial intelligence (AI) into healthcare, particularly behavioral health, is transforming…
Anxiety and Substance Use: Breaking the Cycle
Anxiety and Substance Use: Breaking the Cycle Anxiety and substance use frequently occur together, creating a complex and often self-perpetuating cycle that can be difficult…
Utilizing Practice Management Tools to Streamline Your Mental Health Documentation Workflow
Utilizing Practice Management Tools to Streamline Your Mental Health Documentation Workflow Confidentiality is essential for building trust between therapists and clients, but there are times…
Grief During Pregnancy: Supporting Maternal Mental Health After Perinatal Loss
Grief During Pregnancy: Supporting Maternal Mental Health After Perinatal Loss Pregnancy after loss brings a unique and often unspoken form of grief that can significantly…
Exploring the Real Connections Between Trauma, Addiction and Loss
Exploring the Real Connections Between Trauma and Addiction and Loss Explore the complex relationship between trauma, addiction, and loss-how they intertwine, reinforce each other, and…
Harm Reduction and Alcohol: A Practical Approach for Behavioral Health Clinicians
Harm Reduction and Alcohol: A Practical Approach for Behavioral Health Clinicians April is Alcohol Awareness Month, making it the perfect time for behavioral health clinicians…
The Impact of Mood Disorders on Personality
Blog > Treatment Strategies > The Impact of Mood Disorders on Personality The Impact of Mood Disorders on Personality Understanding how mood disorders influence personality…
Understanding Body Grief: Navigating Loss and Acceptance
Blog > Emerging Trends > Understanding Body Grief Understanding Body Grief: Navigating Loss and Acceptance Body Grief refers to the emotional response to changes in…
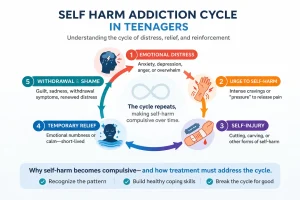
Self Harm Addiction in Teens: Withdrawal & Treatment Guide
Self Harm Addiction in Teenagers: Understanding the Cycle, Withdrawal, and Treatment Self harm addiction in teenagers is often misunderstood as purely behavioral rather than compulsive.…