Blog > Treatment Strategies > Self Harm Addiction in Teens: Withdrawal & Treatment Guide
Self Harm Addiction in Teenagers: Understanding the Cycle, Withdrawal, and Treatment
Self harm addiction in teenagers is often misunderstood as purely behavioral rather than compulsive. This guide explores how self-injury can function like an addiction, the role of reinforcement and emotional relief, common self harm withdrawal symptoms, and evidence-based self harm addiction treatment approaches clinicians can use to support recovery.

Last Updated: March 25, 2026

What You'll Learn
- How self harm addiction develops and why it can become compulsive
- The role of reinforcement, emotional relief, and behavioral conditioning
- Key signs and patterns clinicians should assess in teens
- What self harm withdrawal symptoms look like in practice
- Evidence-based self harm addiction treatment strategies (DBT, CBT, harm reduction)
- How to interrupt the cycle and support long-term recovery
Contents
Self-harm in teenagers is often framed as a coping strategy — but for many clients, it functions much more like an addiction.
Repeated self-injury can activate the brain’s reward system, creating a powerful cycle of emotional distress, temporary relief, and reinforcement. Over time, this cycle can become compulsive, with teens reporting cravings, loss of control, and difficulty stopping despite negative consequences.
Understanding self harm addiction through this lens helps clinicians move beyond surface-level interventions and address the deeper behavioral and neurological patterns that maintain the cycle.
Importance of Recognizing Self-Harm Patterns and Addiction
Teenagers may avoid talking about self-harm behaviors, so it's important to notice signs and patterns. Individuals may engage in the following types of self injury:
- Cutting oneself
- Pinching, biting or scratching oneself
- Piercing the skin
- Inserting sharp objects under the skin
- Pulling hair out
- Bruising various parts of the body
- Burning the skin
- Purposely picking at scabs
- Hitting oneself
- Binge eating or purging food after eating
- Restricting food intake
- Overexercising
Self harm can potentially lead to injury or health complications like infections. Recognizing and addressing self injury early is vital for protecting teenagers, preventing adverse effects and helping them develop safe coping strategies. Talking to a client about suspected self injury in a productive way lets them know they are safe to discuss all of their challenging thoughts and feelings with you.
Common Self-Harm Signs and Symptoms
The following signs and symptoms may indicate a teenager engages in self harm:
- Scars appearing in patterns
- Unexplained fresh wounds, such as scratches, cuts or bite marks
- Frequent accidental injury reports
- A habit of carrying sharp objects with them
- Wearing long pants or long sleeves on hot days
- Refusal to change clothes in social settings, such as a school's changing room
- Frequent use of bracelets or wristbands
- Blood stains on clothing
- Reports of isolation or withdrawal from friends and family
- An extreme increase or decrease in food intake
- Exercising to the point of exhaustion or injury
- A tendency toward emotional dismissal or suppression
- Alexithymia, or an inability to recognize and express emotions
- Self-blame and internalization of challenges
- Low self-esteem or self-concept
- A co-occurring condition, such as depression, anxiety or post-traumatic stress disorder (PTSD)
Understanding Self Harm Addiction
While the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR) does not recognize self-harm as an official addiction, it can affect individuals like a behavioral addiction. Individuals may develop a compulsive self-harm habit to relieve or cope with challenges, replacing intense emotions with physical sensations. Teenagers may continue engaging in self-harm despite negative effects because behaviors can trigger the brain's reward system.
The brain naturally produces mood-regulating neurotransmitters like serotonin and dopamine to help people feel motivated, happy, focused and satisfied when they engage in beneficial behaviors. However, the brain may also release these chemicals when an individual engages in self-harm, which is why some people may feel like they have a self-harm addiction. Over time, this cycle can reinforce the behavior, making self harm addiction treatment essential for helping individuals break the pattern and develop healthier responses to emotional distress.
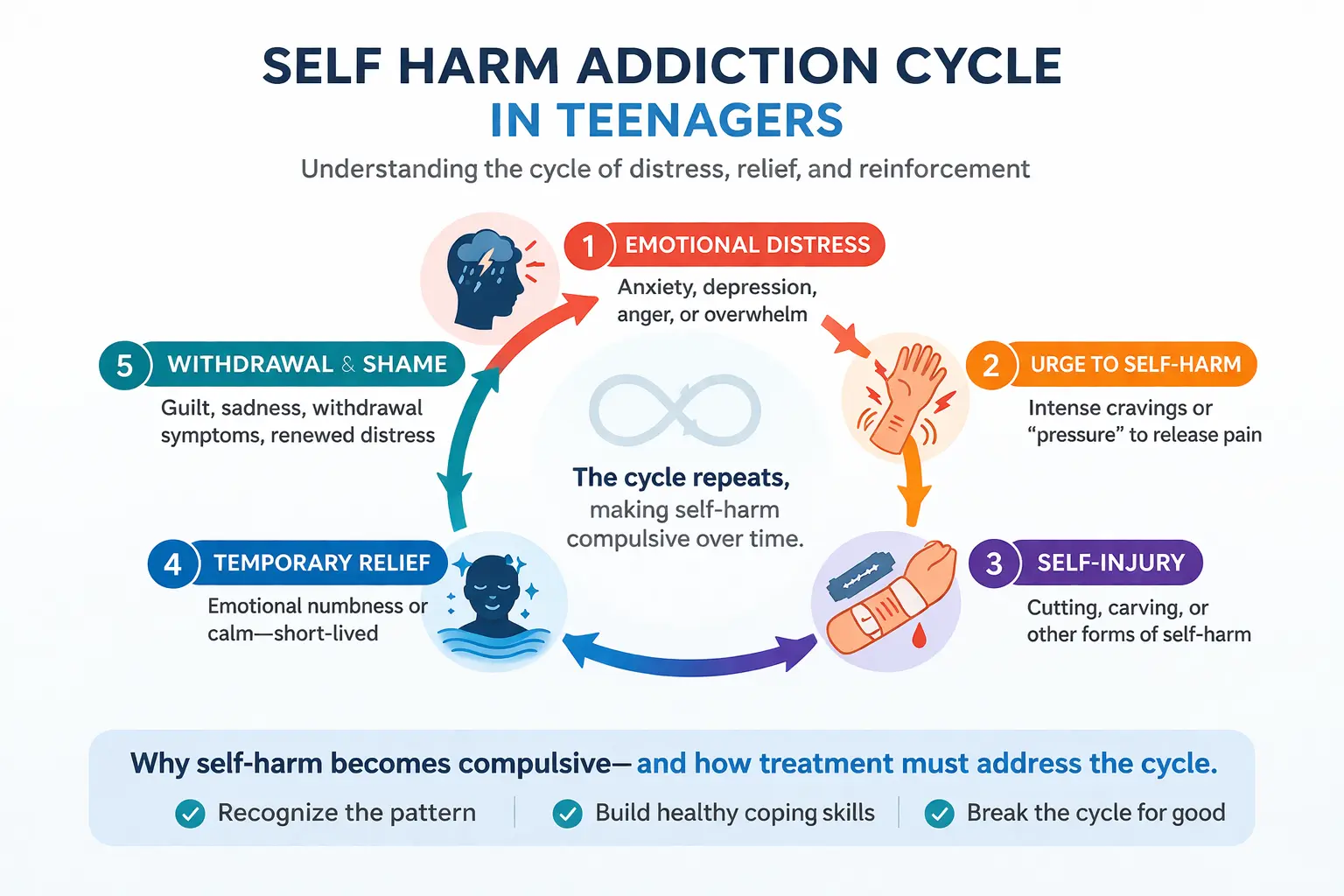
Self-harm becomes addictive when it is repeatedly used to regulate emotional distress and is reinforced by immediate psychological relief. The cycle below illustrates how self harm addiction is reinforced over time, making the behavior increasingly difficult to stop without targeted intervention.
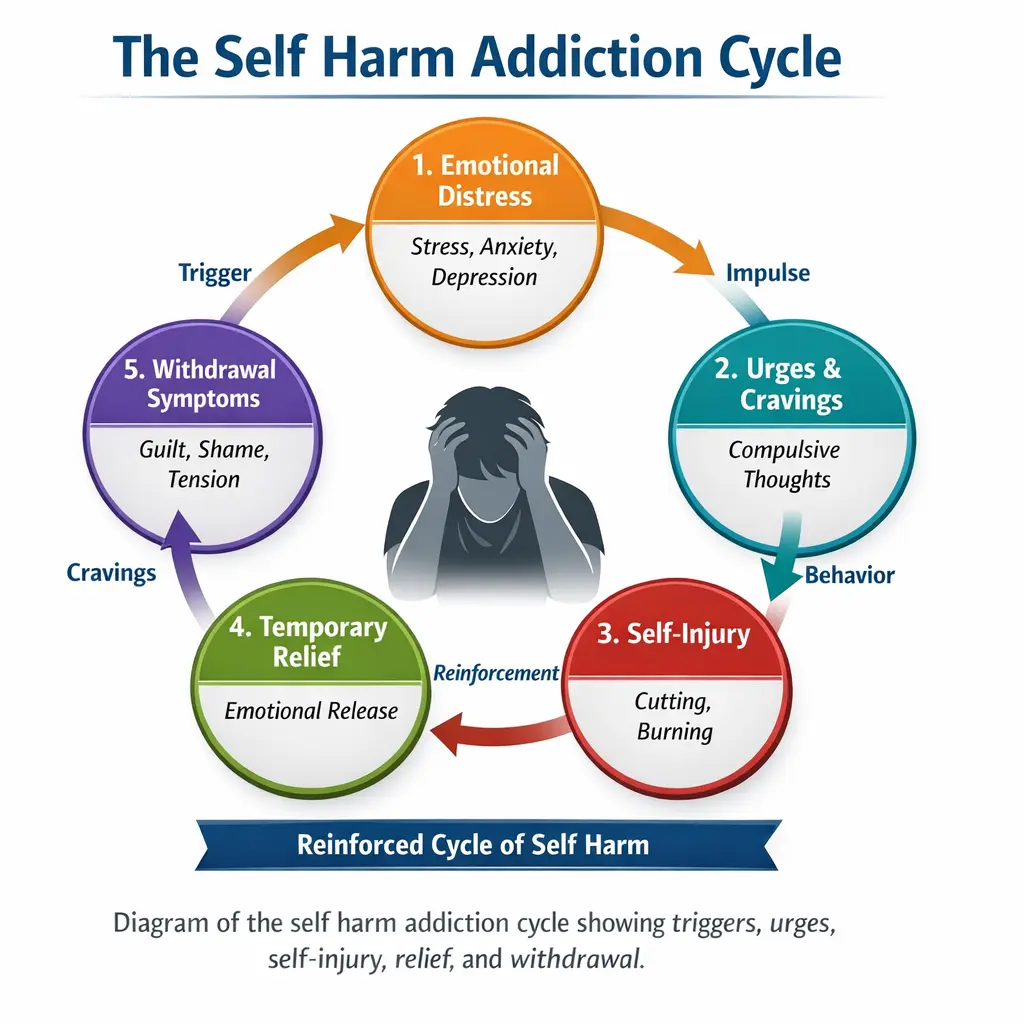
Research shows that nonsuicidal self-injury (NSSI) is often used to cope with intense emotional states such as anger, anxiety, or depression . The relief that follows self-injury can act as a form of negative reinforcement, increasing the likelihood that the behavior will occur again.
Over time, this creates a cycle:
- Emotional distress builds
- Urge to self-harm increases
- Self-injury occurs
- Temporary relief follows
- Shame or guilt returns
- The cycle repeats
For some adolescents, this pattern begins to mirror addiction — where the individual feels driven to engage in the behavior despite wanting to stop.
Signs of Self Harm Addiction in Teenagers
Clinicians should assess for addiction-like features, including:
- Increasing frequency or severity of self-harm
- Failed attempts to stop
- Strong urges or “cravings” to self-injure
- Using self-harm as a primary coping strategy
- Continued behavior despite consequences
Some teens describe the behavior as something they “need” to feel better, reinforcing the compulsive nature of the cycle
Self Harm Withdrawal Symptoms
When teens attempt to stop self-harming, they may experience self harm withdrawal symptoms that resemble other behavioral addictions.
These can include:
- Increased anxiety or agitation
- Emotional overwhelm or dysregulation
- Irritability or restlessness
- Intrusive thoughts or urges to self-harm
- Difficulty concentrating
- Heightened distress tolerance challenges
Because self-harm often functions as a rapid emotional regulation tool, removing it without replacement coping strategies can leave clients feeling destabilized.
This is why treatment should never focus on stopping the behavior alone, but instead on building alternative skills that address the underlying emotional needs.

Self Harm Addiction Treatment
Several effective self-harm addiction treatment approaches can help teenagers break the cycle of self-injury. Some of the methods below work best in one-on-one sessions, while others may be better for group therapy settings. For a deeper look at structuring clinical interventions, see our guide on self-harm treatment plan interventions and goals.
1. Prioritize Open Communication
Providing a space for younger clients to feel safe opening up is key. Prioritize an empathetic, nonjudgmental approach by actively listening to each client and validating their feelings. It's also important to make eye contact, speak in calm tones, remain neutral and respond objectively when clients disclose self-harm.
If a teenager attends mandated therapy against their desire, you can strengthen the therapeutic relationship by asking them how they would like to spend their time in therapy and honoring their preferences. Acknowledging a teenager's feelings and giving them some autonomy during sessions can increase trust and help them openly discuss self-harm experiences. It's also vital to explain the following details to maintain honest communication with your client and help them feel empowered throughout the process:
- Specific interventions and techniques for addressing self-harm
- Mandated reporting and your duty to protect your client if they show signs of needing additional support or intervention
- The types of information you must share with parents or caregivers if the client is under 18
2. Assess Self Harm and Suicide Risk
Not all individuals who engage in self-harm experience thoughts of suicide. Referring a client to the hospital unnecessarily can decrease their trust and hinder the therapeutic relationship, so it's important to avoid making assumptions. However, it's also essential to assess suicide risk during intake and at periodic intervals. You can use the following instruments to screen for self-injury, assess the functions of self-injury and monitor a client's risk of suicide:
- Kim Gratz's Deliberate Self-Harm Inventory questionnaire
- Matthew Nock's Self-Injurious Thoughts and Behaviors Interview
- Catherine Glenn and David Klonsky's Inventory of Statements About Self-Injury
3. Focus on Underlying Causes and Alternative Coping Mechanisms
Clients may have a strong reliance on self-harm when they first begin therapy. Stopping behaviors abruptly can potentially cause self-harm withdrawal symptoms, such as restlessness, irritability, anxiety and strong urges to engage in self-injury. Because self-harm withdrawal can be intense, it's important to take a gradual, supportive approach. If a client does not feel ready to fully change self-harm habits at first, you can begin with the following goals:
- Addressing the root causes of their self-harm
- Diminishing risks
- Realizing and focusing on their strengths
- Helping them enhance alternative coping mechanisms
After working through challenging emotions and strengthening beneficial coping mechanisms, you can help the client work toward stopping self-harm behaviors.
4. Implement Evidence-Based Treatment Methods
Mental health professionals often use the following self harm addiction treatment methods to help clients work through self-injury challenges:
- Dialectical behavior therapy (DBT): DBT remains the gold standard. You can implement DBT in treatment plans to help clients improve distress tolerance, develop safer coping mechanisms, regulate their emotions and reduce self-harm.
- Cognitive behavioral therapy (CBT): CBT can help individuals identify emotions, thoughts and situations that trigger self-injury behaviors and challenge their patterns.
- Mentalization-based therapy (MBT): MBT methods help clients understand the connection between mental state and behavior.
- Family interventions: Family interventions may be necessary if a client's self-harm is related to strained family relationships. Improving attachment and family cohesion can make a significant difference in a client's emotional regulation and self-esteem. You can also provide psychoeducation to the family and encourage family support for the individual.

5. Evaluate Your Personal Feelings About Self-Harm
Self-harm can be challenging to treat, and mental health professionals often experience burnout or challenging emotions when addressing it. Reflect on your feelings and reactions frequently, and work through specific challenges in supervision so you can remain empathetic, open and present with your clients.
For clinicians developing structured interventions, a comprehensive approach to goal-setting and documentation is essential. This guide on Self-Harm Treatment Plan: Interventions and Goals That Support Healing and Safety walks through how to create measurable goals, apply evidence-based interventions, and document care in a way that supports both client outcomes and compliance.
Clinical Implications: Treating Self Harm as an Addiction
Reframing self-harm as an addiction can significantly shift how clinicians assess, conceptualize, and treat the behavior.
Rather than viewing self-injury as an isolated coping strategy, this perspective recognizes it as a reinforced behavioral cycle driven by emotional distress, temporary relief, and recurring urges. For many teens, this pattern closely mirrors addiction, including craving-like urges, loss of control, and difficulty stopping despite negative consequences.
This has important implications for both assessment and treatment.
Clinicians should move beyond simply asking whether a client is self-harming and instead explore:
- The frequency, intensity, and progression of the behavior
- The emotional and situational triggers that precede self-injury
- The function the behavior serves (e.g., relief, numbing, expression)
- The presence of urges, cravings, or self harm withdrawal symptoms when the behavior is interrupted
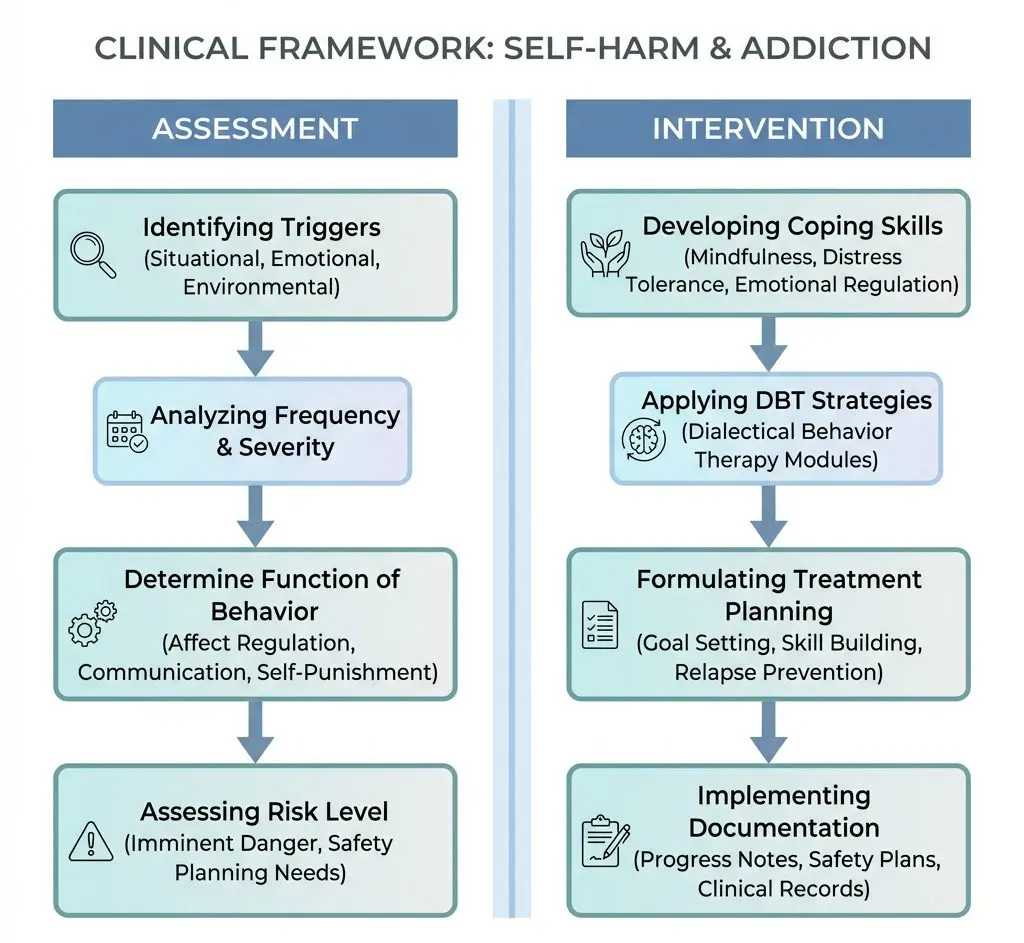
Understanding these elements helps identify where a teen is within the addiction cycle — and where intervention is most likely to be effective.
From a treatment perspective, this model emphasizes that stopping the behavior alone is not sufficient. Teens need alternative strategies that serve the same regulatory function as self-harm, particularly during periods of heightened distress or withdrawal.
This is where structured, evidence-based approaches — such as DBT skills, urge surfing, and gradual behavior replacement — become essential components of self harm addiction treatment.
It also shifts expectations around progress. Like other addictive behaviors, self-harm may involve cycles of reduction, lapse, and recovery. Normalizing this process can reduce shame and help clients stay engaged in treatment rather than disengaging after setbacks.
Finally, clinicians must ensure that their documentation clearly reflects both the severity of the behavior and the medical necessity of treatment. Accurately capturing patterns of reinforcement, functional impairment, and ongoing risk is critical — not only for clinical clarity, but also for supporting reimbursement and audit readiness.
By approaching self-harm through an addiction-informed lens, clinicians can better align assessment, intervention, and documentation — leading to more effective, sustainable outcomes.
Breaking the Cycle of Self Harm Addiction
Self harm addiction in teenagers is not simply a behavioral issue — it is a patterned, reinforced cycle that requires targeted intervention.
By understanding how emotional distress, relief, and reinforcement interact, clinicians can move beyond surface-level symptom management and begin addressing the underlying drivers of the behavior.
Effective treatment focuses on:
- Disrupting the addiction cycle
- Building alternative coping strategies
- Supporting clients through self harm withdrawal symptoms
- Creating structured, measurable treatment plans
With the right framework, clinicians can help teens reduce reliance on self-injury and develop healthier, more sustainable ways to regulate emotional distress.
Why Trust ICANotes for Self-Harm Therapy Documentation?
Clinicians need tools that support both effective treatment and defensible documentation — especially when working with complex patterns like self harm addiction. ICANotes was built specifically for behavioral health clinicians — by a psychiatrist who understood the complexity of documenting care for mental health conditions.
Simplify self-harm documentation and treatment planning with ICANotes
When working with teens experiencing repetitive self-injury, clear documentation matters. ICANotes helps behavioral health clinicians create faster, more consistent notes, support medical necessity, and document treatment plans with greater confidence.
Start your free 30-day trial to see how ICANotes can help you streamline charting, reduce documentation burden, and stay focused on client care.
- ✔ Behavioral health-specific note templates
- ✔ Faster progress notes and treatment planning
- ✔ Built-in billing, scheduling, and patient engagement tools
- ✔ No credit card required
Whether you’re documenting self harm addiction, tracking treatment progress, or preparing for audits, ICANotes helps ensure your notes are both clinically meaningful and compliant. Join thousands of behavioral health clinicians who rely on ICANotes to simplify documentation and improve practice efficiency.
Frequently Asked Questions: Self Harm Addiction
Related Posts
Lindsay Rutter, MA, NCC, LPC, is a Licensed Professional Counselor with a Master's Degree in Clinical Counseling. She has nearly 15 years of clinical and supervisory experience with extensive knowledge of mental health diagnoses, their etiology and evidence-based treatments. Lindsay is the Clinical Director of a nonprofit community mental health center and the owner of a private practice in Chester County, PA.






