Blog > Documentation > Geriatric SOAP Notes: Alzheimer's & Dementia Progress Note Examples
Geriatric SOAP Notes: Alzheimer’s & Dementia Progress Note Examples
Writing effective geriatric SOAP notes requires more than standard documentation, especially when working with patients experiencing Alzheimer’s disease or other forms of dementia. Clinicians must capture cognitive decline, functional status, behavioral symptoms, caregiver input, and safety risks with precision. In this guide, you’ll learn how to write geriatric SOAP notes step by step, along with five copy-ready examples for Alzheimer’s, dementia with agitation, wandering behaviors, and early-stage cognitive decline to help you document more clearly, support medical necessity, and improve clinical care.

Last Updated: April 20, 2026


What You'll Learn
- How to write geriatric SOAP notes for Alzheimer’s and dementia patients
- What to include in each section: Subjective, Objective, Assessment, and Plan
- How to document cognitive decline, ADLs/IADLs, and behavioral symptoms
- Best practices for capturing caregiver input and safety risks
- How to write notes that support medical necessity and audit readiness
- 5 copy-ready geriatric SOAP note examples you can adapt immediately
Documenting geriatric mental health encounters — particularly for patients with Alzheimer’s disease or other forms of dementia — requires a level of specificity that goes well beyond a standard progress note. Clinicians must capture cognitive status, functional abilities, behavioral and psychological symptoms, caregiver observations, capacity concerns, and safety risks, often across a clinical picture that changes gradually and unpredictably.
Whether you’re charting an Alzheimer’s progress note, a dementia follow-up with behavioral agitation, or an early-stage cognitive decline evaluation, a well-structured SOAP note protects your practice, supports medical necessity, and creates a reliable longitudinal record of the patient’s trajectory.
This guide walks you through each section of a geriatric SOAP note step by step and provides five copy-ready examples—including sample charting for dementia patients — that you can adapt for your own clinical documentation.
What Makes Geriatric SOAP Notes Different?
While every SOAP note follows the same four-section structure — Subjective, Objective, Assessment, and Plan — geriatric mental health documentation introduces several clinical and documentation demands that are less prominent in general adult psychiatry or therapy notes.
- Emphasis on cognition and memory: Unlike most adult mental health encounters, geriatric SOAP notes must systematically document the patient’s cognitive status, including orientation, memory (short-term and long-term), attention, language, and executive function. Changes from baseline should be tracked over time.
- ADLs and IADLs: Functional status documentation is central. Geriatric notes should capture the patient’s ability to perform activities of daily living (ADLs) — bathing, dressing, toileting, eating, and transferring — as well as instrumental activities of daily living (IADLs) such as managing finances, medications, transportation, cooking, and housekeeping.
- Behavioral and psychological symptoms of dementia (BPSD): Agitation, aggression, wandering, sundowning, paranoia, hallucinations, and sleep-wake cycle disturbances are common in dementia and must be documented with specificity — including frequency, severity, triggers, and impact on care.
- Caregiver involvement: Geriatric documentation frequently relies on collateral information from family members or caregivers, especially when the patient’s self-report is unreliable due to cognitive impairment. Documenting who provided the information and their relationship to the patient is essential.
- Capacity and safety documentation: Clinicians must document observations relevant to the patient’s decision-making capacity, driving safety, risk of elopement or wandering, fall risk, and vulnerability to exploitation or self-neglect. These observations carry legal and ethical weight.
Understanding these unique demands is the foundation for writing geriatric SOAP notes that are clinically thorough, legally defensible, and compliant with payer requirements.
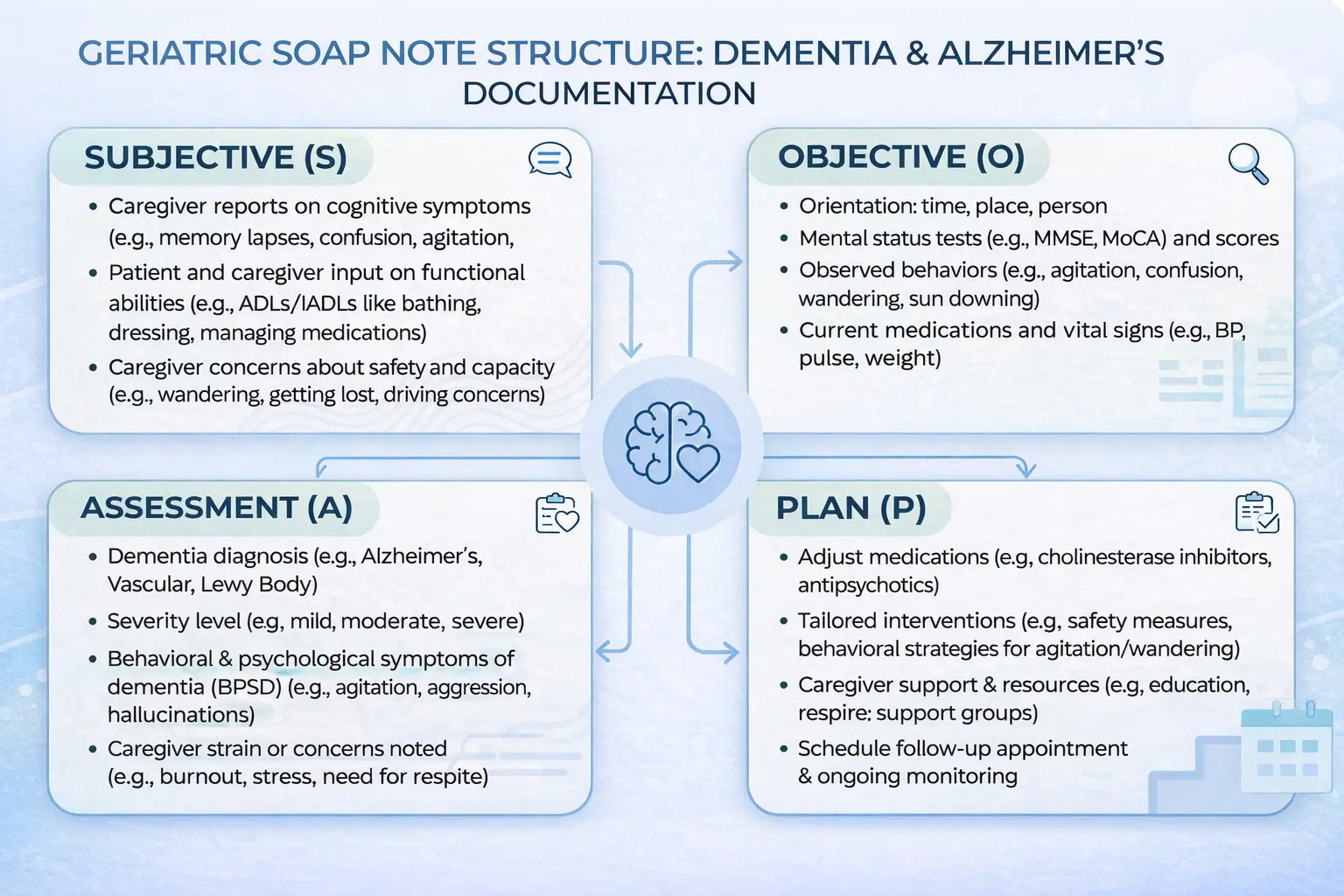
Subjective (S)
Patient and caregiver reports of cognitive changes, memory loss, confusion, behavioral symptoms (e.g., agitation, wandering), functional decline (ADLs/IADLs), sleep patterns, and safety concerns such as falls or getting lost.
Objective (O)
Clinician observations including orientation (person, place, time), mental status exam findings, speech and language changes, observed confusion, functional abilities, and cognitive screening scores (e.g., MMSE, MoCA).
Assessment (A)
Diagnosis of neurocognitive disorder (e.g., Alzheimer’s, vascular dementia), stage and severity, functional impact, behavioral symptom profile, safety risk level, and progression compared to baseline.
Plan (P)
Medication management, behavioral and environmental interventions, caregiver education and support, safety planning (e.g., fall prevention, wandering risk), referrals, and follow-up care coordination.
It’s worth noting that the focus of each section may vary depending on the provider’s role and the complexity of the patient’s condition. A psychiatrist’s geriatric SOAP note may emphasize medication management, comorbid medical conditions, and cognitive testing results, while a therapist or behavioral health clinician may focus more on functional decline, behavioral symptoms, caregiver dynamics, and psychosocial stressors. In many geriatric cases, documentation also incorporates caregiver input and safety considerations such as fall risk, wandering, or capacity concerns. The SOAP structure is flexible enough to capture these different perspectives while supporting clear, comprehensive dementia documentation.

Write Better Geriatric SOAP Notes With More Clarity and Confidence
Download our free Mental Health SOAP Notes Guide to improve your documentation for dementia, Alzheimer’s, and other geriatric conditions with practical examples, stronger clinical language, and tips that support medical necessity and compliance.
- How to document cognitive decline, ADLs/IADLs, and functional status
- Best practices for capturing caregiver input and safety concerns
- SOAP note examples and formatting tips for dementia documentation
- Write faster, more complete notes without sacrificing clinical quality
Get the guide instantly and start writing stronger geriatric SOAP notes today.
How to Write Geriatric SOAP Notes (Step by Step)
The following step-by-step breakdown covers what to include in each section of a geriatric SOAP note, with specific attention to the documentation needs of patients with Alzheimer’s disease, dementia, and other neurocognitive disorders.
Step 1: Subjective — Patient and Caregiver Report
The Subjective section captures reported symptoms and concerns. In geriatric encounters, this information often comes from both the patient and a caregiver or family member. Clearly attribute the source of each piece of information.
- Patient-reported symptoms (if reliable): Document the patient’s own account of their mood, memory concerns, confusion, sleep, appetite, and pain. Note the degree to which the patient’s self-report appears consistent with objective findings.
- Caregiver observations: Record observations from the caregiver, family member, or facility staff. Include their name, relationship to the patient, and specific concerns—such as increased confusion, repeated questions, getting lost in familiar places, personality changes, or difficulty managing medications.
- Memory decline: Document the nature and timeline of memory changes. Is the patient forgetting recent conversations? Misplacing items? Failing to recognize familiar people? Distinguish between short-term and long-term memory complaints.
- Behavioral changes: Agitation, aggression, paranoia, hallucinations, disinhibition, apathy, wandering, or sundowning. Document onset, frequency, duration, triggers, and severity.
- Sleep and appetite: Note changes in sleep-wake patterns (insomnia, daytime somnolence, nighttime wandering), appetite, and weight.
- Safety concerns: Document any incidents since the last visit—falls, leaving the stove on, getting lost, driving incidents, medication errors, or vulnerability to financial exploitation.
- Medication adherence: Note whether the patient is managing their own medications or if a caregiver assists. Document any missed doses, duplicated doses, or side effects.
Strong Geriatric Subjective Sections Often Include
Tip: In moderate-to-advanced dementia, the caregiver’s account may make up most of the Subjective section. Always note when information comes from collateral sources.
Step 2: Objective — Cognitive and Functional Observations
The Objective section records the clinician’s direct observations and exam findings. For geriatric patients, this section should emphasize cognitive and functional status.
- Mental status exam: Document appearance, behavior, cooperation, eye contact, and general engagement level. Note if the patient required redirection or prompting.
- Orientation: Specify whether the patient is oriented to person, place, time, and situation. Use specific language (e.g., “Oriented to person and place; disoriented to date and day of the week”).
- Speech and language: Note fluency, word-finding difficulty, paraphasias, reduced verbal output, perseveration, or echolalia.
- Observed confusion: Document specific instances of confusion during the session—calling the clinician by the wrong name, not knowing why they are at the appointment, or confabulation.
- Functional observations: If observable, note gait, balance, ability to follow multi-step instructions, fine motor coordination, and self-care status (grooming, hygiene, attire).
- Cognitive test scores: Record results from any administered instruments, such as the MMSE, MoCA, SLUMS, or clock drawing test. Include the score and any notable areas of deficit.
- Affect and mood: Document observed affect (flat, labile, irritable, anxious, apathetic) and reported mood. Note congruence.
Strong Geriatric Objective Sections Often Include
Tip: The Objective section should clearly separate what the caregiver reports from what you directly observe or measure during the visit.
Step 3: Assessment — Diagnosis, Severity, and Risk
The Assessment synthesizes findings into a clinical formulation. For geriatric SOAP notes, include:
- Diagnosis: Use ICD-10 codes. Common diagnoses include Alzheimer’s disease (G30.0/G30.1/G30.9), Dementia in Alzheimer’s disease (F02.80/F02.81), Vascular dementia (F01.50/F01.51), Unspecified dementia (F03.90/F03.91), and Major or Mild Neurocognitive Disorder due to various etiologies.
- Stage and severity: Specify mild, moderate, or severe. Reference cognitive test scores, functional status, and behavioral symptom burden to support your classification.
- Functional decline: Document specific changes in ADLs or IADLs compared to baseline or previous visit. Use clear, measurable language (e.g., “Patient can no longer manage finances independently; was able to do so six months ago”).
- Behavioral symptoms: Summarize the current behavioral symptom profile—agitation, wandering, paranoia, sleep disturbance—and note trajectory (new, worsening, stable, improved).
- Safety risk level: Document your assessment of the patient’s safety risk, including elopement/wandering risk, fall risk, driving safety, self-neglect, and vulnerability to exploitation.
- Treatment response: Is the current treatment plan effective? Are medications being tolerated? Is the patient or caregiver benefiting from behavioral interventions or psychoeducation?
Strong Geriatric Assessments Often Include
Tip: Clear comparisons to prior visits help establish progression, justify interventions, and support payer review.
Step 4: Plan — Treatment, Safety, and Care Coordination
The Plan documents clinical decisions and next steps. For geriatric patients, the plan often involves coordination with caregivers and other providers. Include:
- Medication management: Current medications and dosages, changes (cholinesterase inhibitors, memantine, SSRIs for comorbid depression, antipsychotics for severe BPSD if indicated), rationale, and monitoring needs. Note awareness of Beers Criteria and anticholinergic burden.
- Behavioral interventions: Non-pharmacological strategies recommended or reviewed—redirection techniques, structured daily routines, environmental modifications, music therapy, activity engagement, or validation approaches.
- Caregiver education and support: Psychoeducation provided, caregiver stress assessment, referral to support groups or respite care, and communication strategies.
- Home safety measures: Specific recommendations—door alarms, stove safety devices, medication lockboxes, removal of fall hazards, supervision level adjustments, or GPS tracking for wandering risk.
- Referrals: Neurology, neuropsychological testing, primary care, occupational therapy, social services, adult protective services, elder law attorney, or higher level of care (assisted living, memory care).
- Follow-up: Next appointment date, frequency of visits, and between-visit monitoring tasks for the caregiver.
Strong Geriatric Plans Often Include
Tip: Specific caregiver instructions and safety measures are especially important in geriatric notes, where risk management is often central to the plan.

Geriatric SOAP Note Examples
Below are five geriatric SOAP note examples covering common clinical presentations in Alzheimer’s and dementia care. Each is written with copy-ready clinical language you can adapt for your own documentation.
1. Alzheimer’s SOAP Progress Note Example
Patient is a 78-year-old female with a diagnosis of Alzheimer’s disease, moderate stage, presenting for a follow-up psychiatric visit accompanied by her daughter (primary caregiver). Daughter reports a gradual decline in the patient’s short-term memory over the past two months. The patient frequently repeats questions within minutes, has forgotten the names of two grandchildren, and left the stove on twice in the past month. The patient was found outside the home in her nightgown last week and could not explain where she was going. Daughter reports increased difficulty managing the patient’s medications, noting the patient takes her morning pills twice or skips them entirely without supervision. The patient describes her mood as “fine” and denies memory problems, stating, “I don’t know why everyone is making such a fuss.” Appetite is stable. Sleep is fragmented, with the patient waking 2–3 times per night and occasionally wandering the house. No reported falls. No agitation or aggression. Daughter reports increasing caregiver fatigue and frustration.
Patient is well-groomed (daughter assists with dressing). She is pleasant and cooperative but appears mildly confused about the purpose of the visit. She initially calls the clinician by her daughter’s name, then self-corrects. Oriented to person; disoriented to place (“a doctor’s office somewhere”), date (states the year as 2019), and day of the week. Speech is fluent but notable for word-finding pauses and occasional circumlocution (describes a watch as “the thing that tells you what time it is”). Affect is pleasant and somewhat inappropriately cheerful given the context. Thought process is circumstantial with loose associations when discussing daily activities. Thought content is notable for anosognosia regarding cognitive decline. No hallucinations, delusions, or paranoia reported or observed. No psychomotor abnormalities. Judgment is impaired—patient does not recognize safety risks. MMSE score: 16/30 (previous score six months ago: 20/30). Clock drawing test: significant errors in number placement and hand positioning.
Major Neurocognitive Disorder due to Alzheimer’s disease, moderate (F02.81 [G30.1]). MMSE decline from 20 to 16 over six months indicates progressive cognitive deterioration. Patient demonstrates impaired short-term memory, disorientation to place and time, word-finding difficulty, and anosognosia. Functional decline is significant—patient can no longer independently manage medications or safely operate the stove. Nocturnal wandering and one elopement episode represent meaningful safety risks. No behavioral or psychological symptoms of dementia beyond nighttime wandering at this time. Caregiver stress is elevated. Risk level: moderate (elopement, self-neglect, medication safety).
Continue donepezil 10 mg daily. Add melatonin 3 mg at bedtime for sleep fragmentation and nocturnal wandering. Caregiver education provided: reviewed redirection strategies, the importance of structured daily routines, and environmental safety modifications (door alarms, stove knob covers, medication lockbox). Recommended daughter transition to full medication management. Referred to occupational therapy for home safety evaluation. Discussed respite care options and provided caregiver support group referral. Discussed driving safety—recommended formal driving evaluation through the DMV or occupational therapy given elopement behavior and disorientation. Follow-up in six weeks, or sooner if wandering or safety incidents increase. Daughter agrees with the plan and will contact the office with any acute concerns.
2. Dementia SOAP Progress Note Example With Agitation
Patient is an 82-year-old male residing in an assisted living memory care unit, presenting for a follow-up psychiatric visit. Information provided by the facility’s charge nurse, who accompanies the patient. Nurse reports a significant increase in agitation and verbal aggression over the past three weeks, primarily occurring in the late afternoon and early evening (sundowning pattern). Patient has been refusing care from staff during evening routines—shouting at aides, pushing hands away during bathing, and throwing food at dinner. He accused a staff member of stealing his wallet (wallet was found in his dresser drawer). He has been pacing the hallways for extended periods and attempting to exit the unit. No physical aggression toward other residents. Appetite is reduced—eating approximately 50% of meals. Sleep is disrupted, with the patient awake and agitated between 2–4 AM several nights per week. Current medications include memantine 10 mg twice daily and sertraline 50 mg daily. Patient is unable to provide a reliable self-report. When asked how he feels, he responds, “I want to go home. They won’t let me leave.”
Patient is dressed in facility-provided clothing. Grooming is fair (staff-assisted). He is alert but restless, standing and sitting multiple times during the interview. He is suspicious and guarded, asking, “Who are you? What do you want?” Eye contact is intermittent. Oriented to person only; disoriented to place (“a hotel”), time, and situation. Speech is notable for reduced fluency, perseveration (“I need to go home” repeated throughout the session), and occasional word salad. Affect is irritable and labile, shifting between anger and tearfulness. Thought process is disorganized with tangential associations. Thought content includes paranoid ideation (staff is stealing from him, people are trying to keep him prisoner). No clear auditory or visual hallucinations endorsed or observed during the session, though staff reports he has been talking to “someone” in his room at night. Psychomotor agitation is prominent. Insight is absent. Judgment is severely impaired. MMSE: unable to complete due to agitation and inattention (estimated 8–10 range based on items completed). MoCA was not attempted.
Major Neurocognitive Disorder due to Alzheimer’s disease, severe, with behavioral disturbance (F02.81 [G30.9]). Patient is exhibiting significant behavioral and psychological symptoms of dementia, including sundowning-pattern agitation, verbal aggression, paranoid ideation, care refusal, pacing, exit-seeking behavior, and possible visual hallucinations. Behavioral symptoms have escalated over three weeks and are now impairing nutrition (reduced intake), staff’s ability to provide care, and the patient’s quality of life. Paranoid themes are consistent with disease progression rather than a primary psychotic disorder. Current medication regimen (memantine + sertraline) is insufficient to manage behavioral symptoms. Risk level: moderate to high (elopement attempts, care refusal, reduced nutrition).
Continue memantine 10 mg twice daily. Increase sertraline to 75 mg daily to target irritability and mood symptoms. Initiate risperidone 0.25 mg at 4:00 PM and 0.25 mg at bedtime for agitation and paranoia, with clear documentation that non-pharmacological interventions have been attempted and that the severity of behavioral symptoms poses a safety risk to the patient and care staff. Informed facility nurse of FDA black box warning regarding antipsychotic use in elderly dementia patients; benefits and risks discussed with the patient’s daughter (healthcare proxy) by phone, and verbal consent obtained. Non-pharmacological behavioral plan reviewed with facility staff: structured afternoon activities to reduce sundowning triggers, consistent care staff assignments, calming music during evening routine, reduced environmental stimulation after 5:00 PM, and redirection rather than confrontation during paranoid episodes. Requested facility monitor and log behavioral incidents (frequency, time, trigger, duration) for the next two weeks. Follow-up in two weeks to assess risperidone response and tolerability. Goal is lowest effective dose for shortest duration. Daughter will be contacted with update after follow-up.
3. Early-Stage Dementia Follow-Up SOAP Note Example
Patient is a 71-year-old male presenting for a follow-up therapy session accompanied by his wife. He was diagnosed with mild neurocognitive disorder (early-stage Alzheimer’s disease) four months ago. He reports feeling “frustrated” and “embarrassed” by his memory lapses, describing recent incidents of forgetting a lunch appointment with a friend and being unable to recall a movie he watched two days ago. He states, “I used to be sharp—this is humiliating.” He endorses mild anxiety about disease progression and increased irritability with his wife. He continues to drive, manage his finances, and cook simple meals independently but reports needing lists and phone reminders more than before. Sleep and appetite are stable. He is adherent to donepezil 5 mg daily and reports no side effects. His wife notes that he occasionally repeats stories within the same conversation and has become less engaged in social outings. He denies depressed mood, suicidal ideation, and self-harm urges.
Patient is well-groomed and appropriately dressed. He is cooperative and engaged, with appropriate humor and social skills intact. Eye contact is consistent. Oriented to person, place, and time (states the correct date after brief hesitation). Speech is fluent with occasional word-finding pauses that he self-corrects. Mood is “frustrated.” Affect is mildly anxious and reactive, with appropriate range. Thought process is linear and coherent. Thought content includes worry about disease progression and loss of independence. No paranoia, hallucinations, or psychotic features. Insight is good—he recognizes his cognitive changes and their implications. Judgment is intact for current daily functioning. MoCA score: 22/30 (previous score four months ago: 24/30). Primary deficits noted in delayed recall and visuospatial/executive function.
Mild Neurocognitive Disorder due to Alzheimer’s disease (G30.0, F02.80). MoCA score of 22 reflects a mild decline from 24 at diagnosis four months ago, consistent with gradual progression. Patient retains functional independence in ADLs and most IADLs but is increasingly reliant on compensatory strategies (lists, reminders). Adjustment-related frustration and mild anxiety about disease trajectory are clinically appropriate and not currently meeting threshold for a comorbid mood or anxiety diagnosis. Social withdrawal is mild and warrants monitoring. No behavioral or psychological symptoms of dementia. No safety concerns at this stage. Risk level: low.
Continue donepezil 5 mg daily; discuss titration to 10 mg with prescribing physician at next medication visit. Continue biweekly supportive therapy focused on adjustment to diagnosis, coping with cognitive changes, and maintaining social engagement. This session: validated frustration and normalized the adjustment process. Introduced cognitive compensatory strategies (calendar system, consistent item placement, written daily checklist). Discussed maintaining physical exercise and social routines as protective factors. Provided psychoeducation to wife on communication strategies (allowing extra time for responses, avoiding quizzing or correcting in real time). Recommended the patient and wife attend an early-stage memory loss support group. Monitor for signs of depression, increased anxiety, or functional decline. Discussed advance care planning—encouraged patient and wife to consult an elder law attorney while the patient retains decision-making capacity. Follow-up in two weeks.
4. Dementia With Wandering and Safety Risk SOAP Note Example
Patient is a 79-year-old female with moderate-stage vascular dementia, presenting for a follow-up visit accompanied by her son (primary caregiver). Son reports two wandering incidents in the past month. In the first, the patient left the house through the back door while the son was in the shower and was found by a neighbor three blocks away, confused and unable to state her address. In the second, the patient attempted to leave the home at 11:00 PM, stating she needed to “pick up the children from school” (her children are adults). Son has installed a chain lock but reports the patient becomes agitated when she cannot open the door. She has also been more confused at night, turning on all the lights and rearranging furniture. She fell once while moving a chair but was not injured. Appetite is fair, with a preference for only sweets. She is not managing any medications independently; son administers all medications. She has been taking memantine 10 mg twice daily and citalopram 20 mg daily. Son reports significant caregiver burden and states, “I don’t know how much longer I can do this at home.” Patient states she is “fine” and “doesn’t need help.”
Patient is clean but wearing a stained sweater and mismatched shoes (son reports she resists clothing changes). She is pleasant but distractible, frequently looking at the door during the session. Oriented to person only; identifies the setting as “a school” and the month as June (it is not). Speech is reduced in fluency, with word-finding difficulty and occasional perseveration. Affect is labile—shifts between pleasant and mildly irritable when asked about her daily routine. Thought process is tangential, with confabulation (describes “dropping the kids off this morning”). Thought content includes no paranoia, hallucinations, or suicidal ideation. Psychomotor activity is notable for restlessness and intermittent attempts to stand during the interview. Insight is absent. Judgment is severely impaired. MMSE: 13/30 (previous: 17/30, eight months ago).
Major Neurocognitive Disorder due to vascular dementia, moderate, with behavioral disturbance (F01.51). MMSE decline from 17 to 13 over eight months confirms progressive cognitive deterioration. Wandering behavior is an active safety risk—two elopement incidents in one month, one involving nighttime exit-seeking with temporal disorientation and confabulation. Fall risk is present (one fall during furniture rearrangement). Nutritional intake is narrowing. Patient has no insight into her deficits and resists safety interventions. Caregiver burden is high and approaching the threshold where home-based care may no longer be sustainable. Risk level: high (elopement, falls, self-neglect).
Continue memantine 10 mg twice daily and citalopram 20 mg daily. Recommended comprehensive home safety modifications: door and window alarms with audible alerts, GPS tracking device (wearable), removal of furniture rearrangement opportunities in high-traffic areas, nightlights in hallways and bathrooms, and a structured evening routine to reduce nighttime confusion. Provided psychoeducation to son on wandering management: lock-and-alarm systems, identification bracelet, notifying neighbors and local police of patient’s condition, and Project Lifesaver enrollment if available locally. Discussed caregiver burnout openly; referred son to local Alzheimer’s Association support group and respite care services. Discussed the possibility of memory care placement if wandering behavior continues to escalate; son will tour two local facilities this month. Referred to neurology for updated imaging given the pace of cognitive decline. Referred to occupational therapy for home safety evaluation. Follow-up in four weeks. Son instructed to contact the office immediately if another elopement occurs.
5. Sample Charting for Dementia Patients (Narrative Format)
Not all documentation settings use a strict SOAP format. Below is a sample narrative progress note for a dementia patient, written in the integrated charting style commonly used in facility-based and long-term care settings.
Documentation Language for Cognitive and Behavioral Symptoms
Precise, consistent language strengthens geriatric SOAP notes and creates a reliable longitudinal record. Below are copy-ready phrases organized by common documentation domains in Alzheimer’s and dementia care.
Orientation Deficits
- Oriented to person only; disoriented to place, time, and situation.
- Oriented to person and place; disoriented to date (stated the year as [year]).
- Fully disoriented to person, place, time, and situation.
- Partial orientation—identified the city correctly but unable to name the facility or floor.
Short-Term Memory Impairment
- Unable to recall any of three objects after a five-minute delay.
- Recalled one of three objects with cueing; spontaneous recall absent.
- Repeats the same question within minutes of receiving an answer.
- Unable to recall the events of the current day or the purpose of the visit.
Sundowning
- Behavioral symptoms follow a sundowning pattern, with onset in the late afternoon.
- Agitation increases predictably after 4:00 PM.
- Nighttime wandering and confusion are consistent with a sundowning pattern.
Agitation and Aggression
- Verbal agitation observed: raised voice, repetitive vocalizations, and care refusal.
- Physical aggression: patient struck caregiver's hand during [specific care activity].
- Agitation appears triggered by [specific trigger] and typically lasts [duration].
- Responds to redirection within [timeframe]; does not require PRN intervention at this time.
Wandering and Elopement
- Patient was found outside without supervision on [date/time].
- Exit-seeking behavior observed: patient repeatedly attempts to open doors and asks to leave.
- Patient wanders the hallways but does not attempt to exit the unit; redirectable.
- GPS tracking device in place and functional.
Caregiver Burden & Capacity
- Caregiver reports increased stress, fatigue, difficulty managing care.
- Caregiver feels overwhelmed and alone; referred to support and respite resources.
- Zarit Burden Interview score: [score] ([severity level]).
- Patient's decision-making capacity appears impaired based on inability to appreciate consequences of [specific decision].
- Healthcare proxy/power of attorney has been activated; [name, relationship] is the designated decision-maker.
Common Mistakes in Geriatric Documentation
Geriatric mental health documentation carries unique clinical and legal weight. Avoiding these common mistakes strengthens the clinical and reimbursement value of your notes:
- Omitting caregiver input. In many geriatric encounters, the caregiver is the primary historian. Failing to document who provided information, their relationship to the patient, and their specific observations creates gaps in the clinical record and undermines the note’s reliability.
- Failing to document orientation status. Orientation is a foundational measure of cognitive function. Every geriatric SOAP note should specify the patient’s orientation to person, place, time, and situation—not just state “oriented” or “disoriented” without detail.
- Missing safety assessment. Wandering, falls, medication mismanagement, driving safety, self-neglect, and exploitation risk must be addressed in every encounter. Omitting safety documentation creates significant legal exposure in the event of an adverse outcome.
- Not tracking functional decline over time. A single note that says “needs help with ADLs” is far less useful than a note that specifies which ADLs are affected and how the patient’s functional status has changed since the previous visit. Tracking functional decline over time is essential for care planning, level-of-care decisions, and payer authorization.
- Vague behavioral descriptions. “Patient was agitated” is not specific enough. Document the behavior (verbal aggression, pacing, care refusal), the trigger (if identifiable), the frequency, the duration, and the response to intervention.
- Neglecting to document capacity observations. Even when a formal capacity evaluation is not performed, clinicians should note observations relevant to the patient’s ability to understand, appreciate, reason about, and express choices regarding their care. These observations become critical if capacity is later contested.
How ICANotes Helps You Write Better Geriatric SOAP Notes
Writing high-quality geriatric SOAP notes takes time — especially when you’re documenting cognitive decline, functional status, caregiver input, and safety risks while managing a full caseload. ICANotes is designed specifically for behavioral health clinicians to make that process faster, easier, and more consistent.
With ICANotes, you can generate structured, compliant SOAP notes using intuitive point-and-click templates tailored to geriatric conditions such as Alzheimer’s disease, vascular dementia, and other neurocognitive disorders. Instead of starting from scratch, the system guides you through clinically relevant prompts, helping you capture key details like cognitive changes, ADLs/IADLs, behavioral symptoms, and caregiver observations.
ICANotes also helps ensure your documentation supports medical necessity by organizing your notes into clear, defensible Subjective, Objective, Assessment, and Plan sections. Built-in phrasing and customizable options make it easier to document safety concerns — such as fall risk, wandering, medication management, and capacity — while maintaining a complete clinical picture.
The result? More thorough geriatric documentation, stronger support for audits and medical necessity, and more time to focus on patient care and caregiver support instead of your notes.

Write Better Geriatric SOAP Notes in Less Time
ICANotes helps behavioral health clinicians create faster, more complete, and more defensible geriatric SOAP notes by simplifying documentation for dementia, Alzheimer’s disease, and other neurocognitive disorders.
- Built-in templates for dementia, Alzheimer’s, and related conditions
- Structured prompts for cognitive status, ADLs/IADLs, and caregiver input
- Clinical language that supports medical necessity and safety documentation
- No credit card required
Start Your Free Trial
Complete the form below to try ICANotes free for 30 days.
Related Resources for Geriatric SOAP Notes and Clinical Documentation
Continue improving your geriatric documentation with these related guides on dementia care, medical necessity, and behavioral health documentation best practices.
Frequently Asked Questions About Geriatric SOAP Notes
Below are answers to common questions about documenting dementia, Alzheimer’s disease, cognitive decline, and safety concerns in geriatric SOAP notes.
Geriatric SOAP notes should include the patient’s cognitive status (orientation, memory, attention, language), functional abilities (ADLs and IADLs), behavioral symptoms, caregiver observations, safety assessment (wandering, falls, driving, medication management, exploitation risk), a diagnosis with severity and stage, and a detailed treatment plan that addresses medication, behavioral interventions, caregiver support, and follow-up. Always attribute information to its source—patient self-report, caregiver, or clinician observation.
Document the Alzheimer’s diagnosis using the appropriate ICD-10 codes (G30.0 for early onset, G30.1 for late onset, G30.9 for unspecified, paired with F02.80 or F02.81 for dementia with or without behavioral disturbance). Specify the stage (mild, moderate, or severe) and support your classification with cognitive test scores, functional status data, and behavioral observations. Track changes from baseline at every visit to create a longitudinal record of disease progression.
Chart cognitive decline by documenting specific cognitive domains affected (memory, orientation, language, executive function, visuospatial ability), using standardized instruments (MMSE, MoCA, SLUMS, clock drawing test) at regular intervals, comparing scores to previous results, and recording functional impact. Avoid vague statements like “cognitive decline noted”—instead, specify what has changed, when the change was first observed, and how it affects daily functioning.
Dementia safety documentation should address wandering and elopement risk (including specific incidents), fall history and fall prevention measures, medication management (who administers, any errors), driving safety, cooking and appliance safety, vulnerability to financial exploitation, and self-neglect (nutrition, hygiene, medical compliance). For each risk area, document the current concern, the mitigation strategy in place, and whether the strategy is adequate or needs to be escalated.
Geriatric progress notes should be detailed enough to capture the patient’s cognitive status, functional abilities, behavioral symptoms, safety profile, and treatment plan—and to track changes over time. A thorough note typically runs one to two pages. The level of detail should support medical necessity for the services billed, provide a clear clinical picture for any provider who reviews the chart, and demonstrate that safety was assessed and addressed. Structured EHR templates designed for behavioral health can help clinicians produce comprehensive geriatric notes without adding significant time to each encounter.
Recent Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.





