Behavioral Health EHR and EMR Software for Mental Health Clinicians
Complete notes in under 3 minutes with template-driven efficiency and AI innovation. ICANotes gives behavioral health clinicians ONC-certified charting, integrated billing, telehealth, and scheduling — in one platform built for mental health, not adapted from a general medical EHR..
• No credit card required

Trusted by Leading Organizations in Behavioral Health
An EHR Built Exclusively for Behavioral Health
ICANotes is a purpose-built mental health EMR and EHR platform designed to reduce documentation time, strengthen compliance, and simplify practice management. Designed exclusively for behavioral health clinicians, our ONC Cures Certified platform combines menu-driven documentation with advanced features that give clinicians more time in session and less time on paperwork.
Built by Clinicians
Developed by behavioral health professionals who understand the real-world challenges of documenting and delivering care in mental health EMR and EHR systems.
Founded in 1999
Designed by a practicing psychiatrist who built ICANotes to be the most intuitive electronic medical records system for mental health
- Founded in 1999
- Designed by a practicing psychiatrist who built ICANotes to be the most intuitive electronic medical records system for mental health
Clinical Documentation
Customizable menu-driven note templates and AI-powered assistance that help you complete behavioral health electronic medical records faster and more accurately.
3 minutes
Average note completion time
All-in-One EHR Platform
An all-in-one mental health EMR and behavioral health EHR software platform with integrated telehealth, labs, e-prescribing, scheduling, and billing — no need to juggle multiple systems.
8+
Mental health software tools in one platform
Strengthen Client Relationships
Keep clients connected and supported throughout their care journey with secure messaging, telehealth, a patient portal, and engagement tools — all seamlessly integrated into your behavioral health EMR and EHR software.
Secure Messaging
Integrated Telehealth
Patient Portal
Automated Reminders
- Secure Messaging
- Client Portal
- Integrated Telehealth
- Automated Reminders
Ready to see what a behavioral health EHR built for clinicians actually looks like?
Book a demo or start your free trial today and discover why thousands of clinicians nationwide trust ICANotes as the top choice for mental health EMR and EHR software

4.8/5 from 500+ reviews
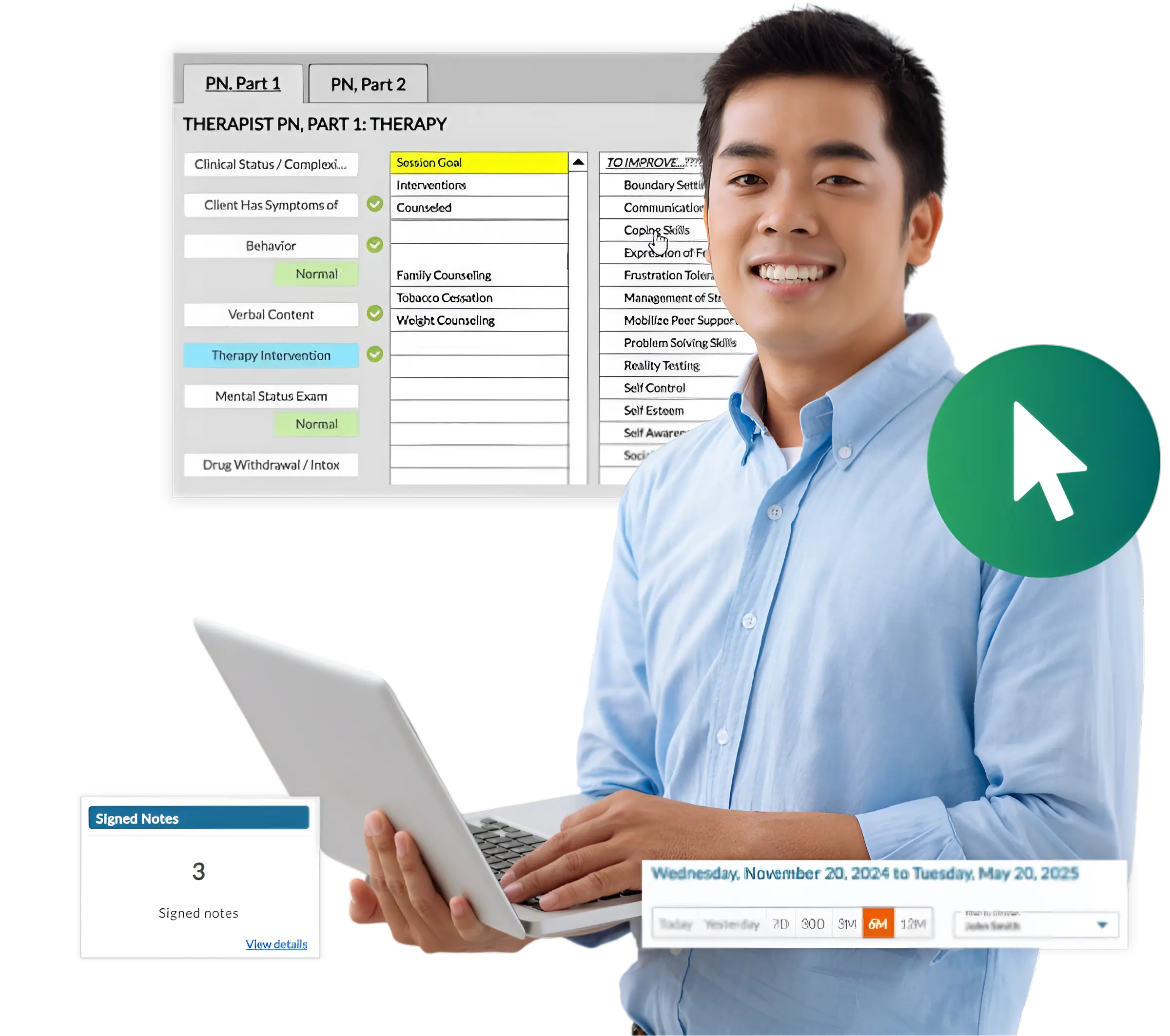
All-in-One Mental Health Practice Management & EHR Software
From documentation to billing, ICANotes combines the tools you need into one secure, ONC-certified electronic medical records system for mental health practices.
Charting
Complete assessments, treatment plans, and progress notes in minutes with AI-powered, menu-driven templates.
Scheduling
Streamline intake and scheduling in your behavioral health EHR software with online forms, self-scheduling, and automated reminders.
Communication
HIPAA-compliant virtual care, secure messaging, and real-time document sharing through the client portal, all seamlessly integrated with the EHR.
Assessment
Access over 100 clinical rating scales directly within ICANotes to measure symptoms, track severity, and inform care decisions.
Treatment
Build custom treatment plans using evidence-based goals, problems, and interventions, then track progress over time, all documented in ICANotes.
Billing
Verify insurance, submit claims electronically, auto-post payments, and track performance with billing workflows.
Mental Health EMR Software That Complete Notes in Under 3 Minutes
Create powerful, audit-ready notes in minutes with customizable menu-driven templates, trusted by thousands of clinicians using our mental health EMR and behavioral health EHR software.
Initial Assessments
Capture first encounters with customizable intake templates built into your electronic medical records for mental health.
Progress Notes
Track patient progress clearly and consistently with structured templates in your mental health EMR system.
SOAP Notes
Document sessions with the standard SOAP format directly in your behavioral health EHR software.
Treatment Plans
Build personalized, goal-focused treatment plans and keep them audit-ready within your mental health EMR software.
BIRP & DAP Notes
Use flexible note formats, including BIRP and DAP, in a behavioral health EMR system tailored to your workflow.
Group Therapy Notes
Streamline notes for group sessions with templates designed specifically for behavioral health electronic medical records.
Case Management & PRP Notes
Coordinate case management and PRP services seamlessly in your mental health EHR system to support continuity of care.
Discharge Summaries
Summarize outcomes and next steps in your mental health EHR software to ensure smooth transitions and continuity of care.

Experience the full ICANotes workflow
Join thousands of clinicians who trust our behavioral health software to simplify documentation and improve compliance.
HIPAA-Compliant & Audit-Ready
Everything You Need in One Mental Health EHR System
Reduce complexity and focus on care with a fully integrated behavioral health EHR software platform.
• Spend Less Time Writing and More Time Treating
Mental Health Charting
Create accurate, audit-ready notes in minutes with menu-driven templates and an ambient AI scribe, all built into your behavioral health EMR software.
Smart, prebuilt templates for every note type
Menu-driven, low-typing documentation
Ambient AI scribe listens and creates notes from your sessions
- Smart, prebuilt templates for every note type
- Menu-driven, low-typing documentation
- Ambient AI scribe listens and creates notes from your sessions
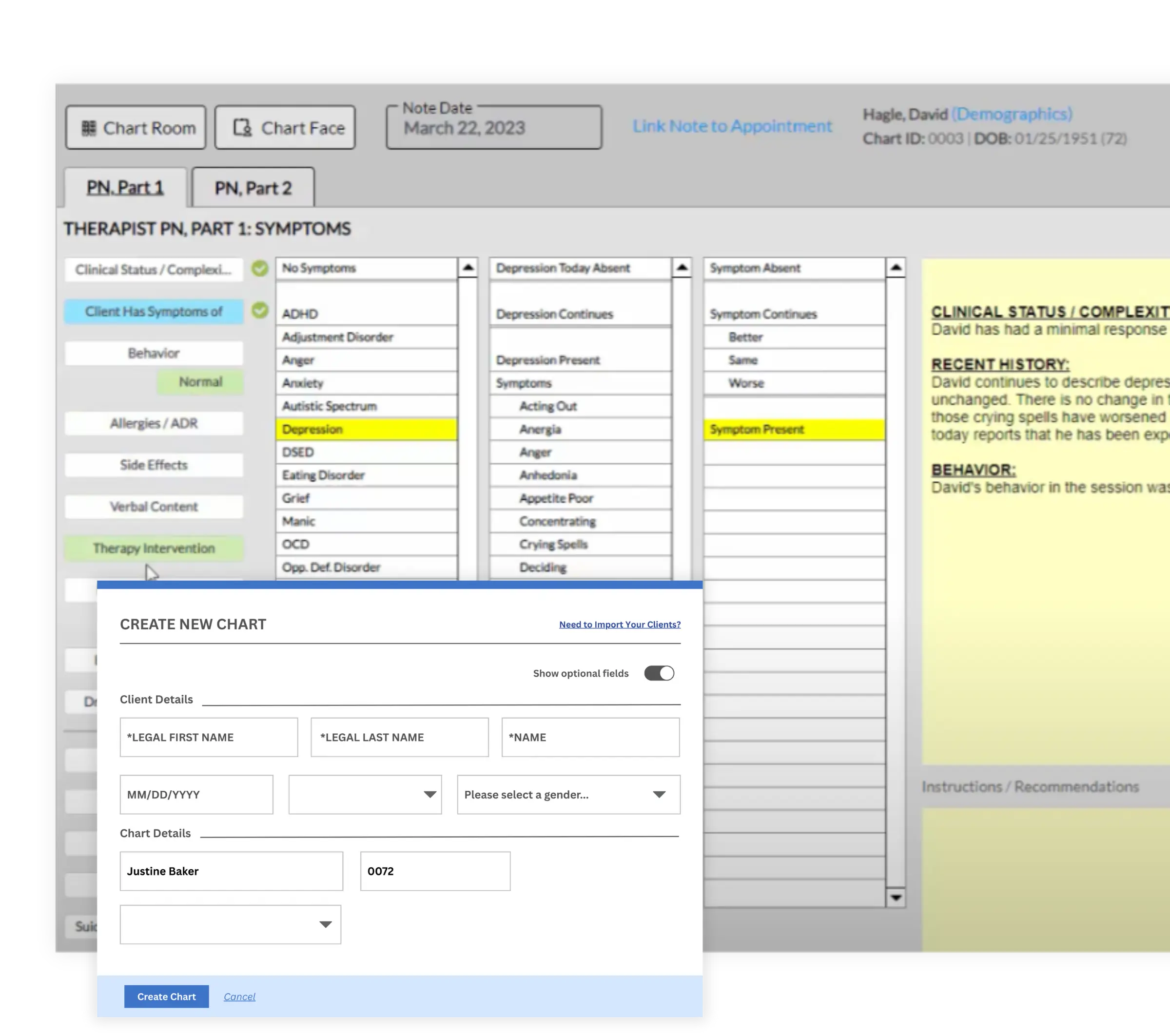
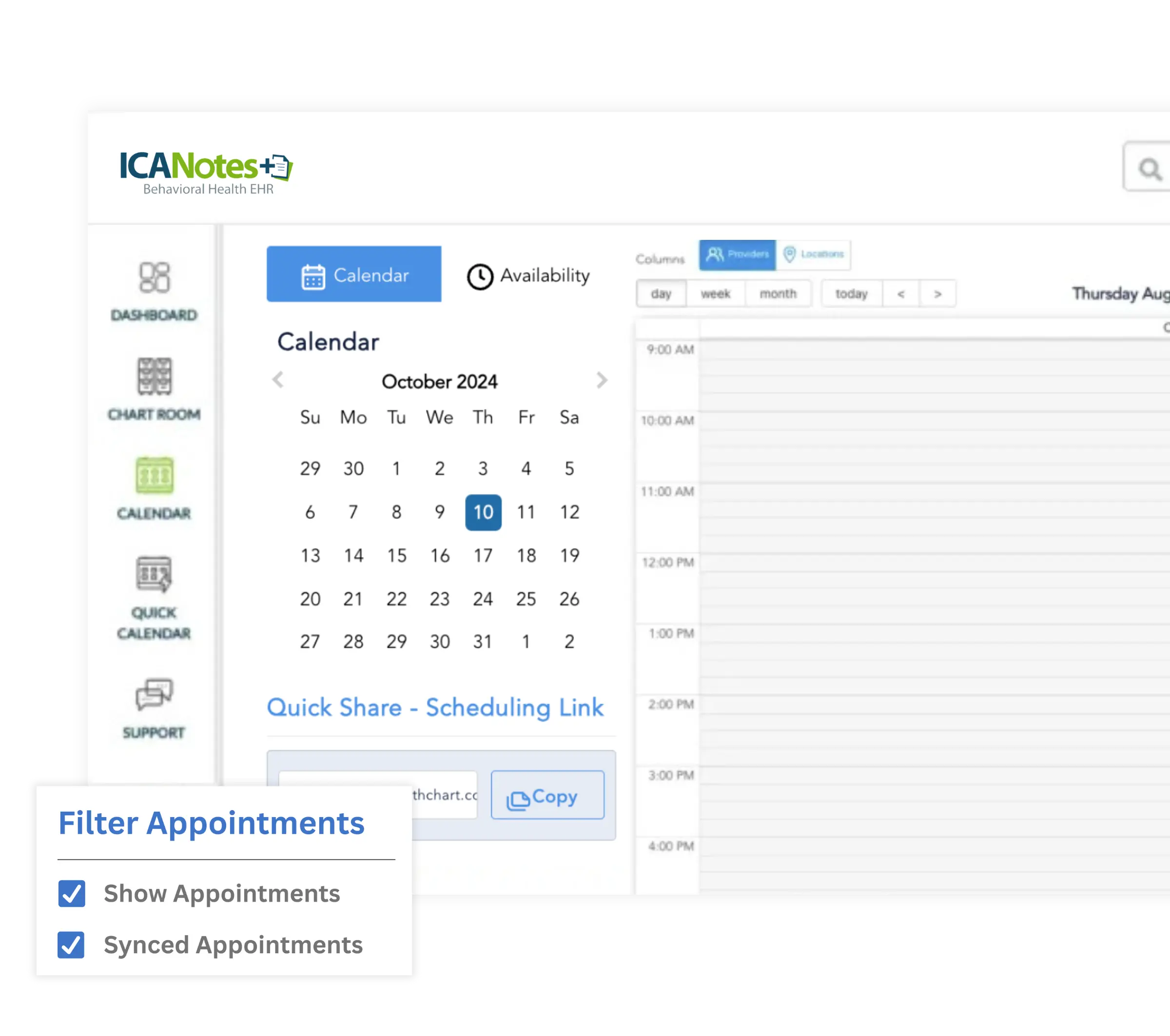
• Keep Your Front Office Running Efficiently
Practice Management
ICANotes streamlines front-office tasks with scheduling, reminders, and digital intake tools, making your team more efficient while reducing no shows and paperwork.
Reduce no-shows with automated scheduling and reminders
Eliminate paperwork by collecting histories, intake forms, and rating scales electronically
- Reduce no-shows with automated scheduling and reminders
- Improve coordination with secure, HIPAA-compliant messaging built into your mental health EMR system
- Eliminate paperwork by collecting histories, intake forms, and rating scales electronically
• Empower Clients With 24/7 Access
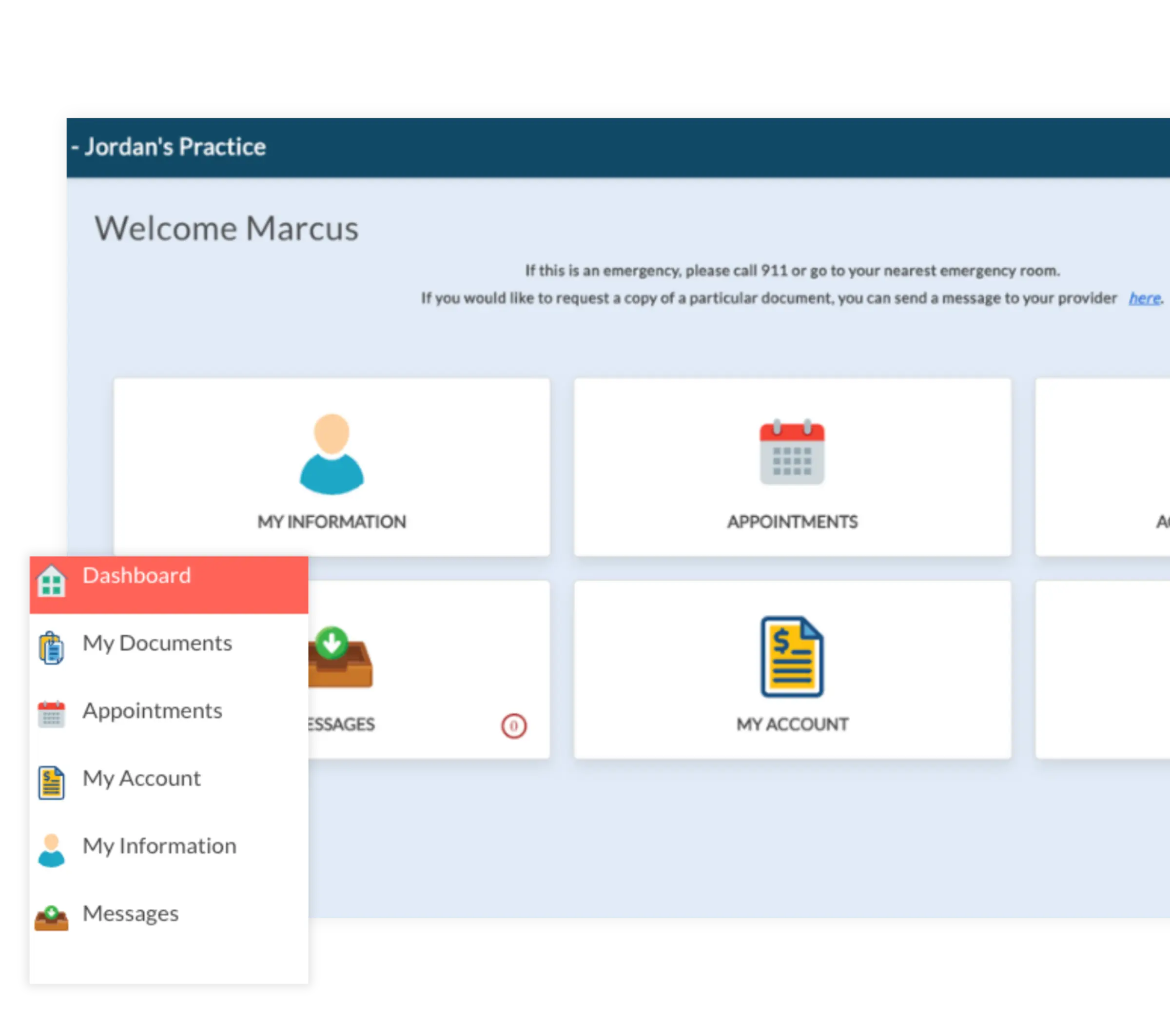
Patient Portal
Let clients manage appointments, complete forms, and make payments securely through a patient portal built into your mental health EHR software.
Enable clients to book appointments anytime
Share clinical history and documents securely
Send patient statements and accept online payments seamlessly within your EHR software.
- Enable clients to book appointments anytime
- Share clinical history and documents securely
- Send patient statements and accept online payments seamlessly within your EHR software.
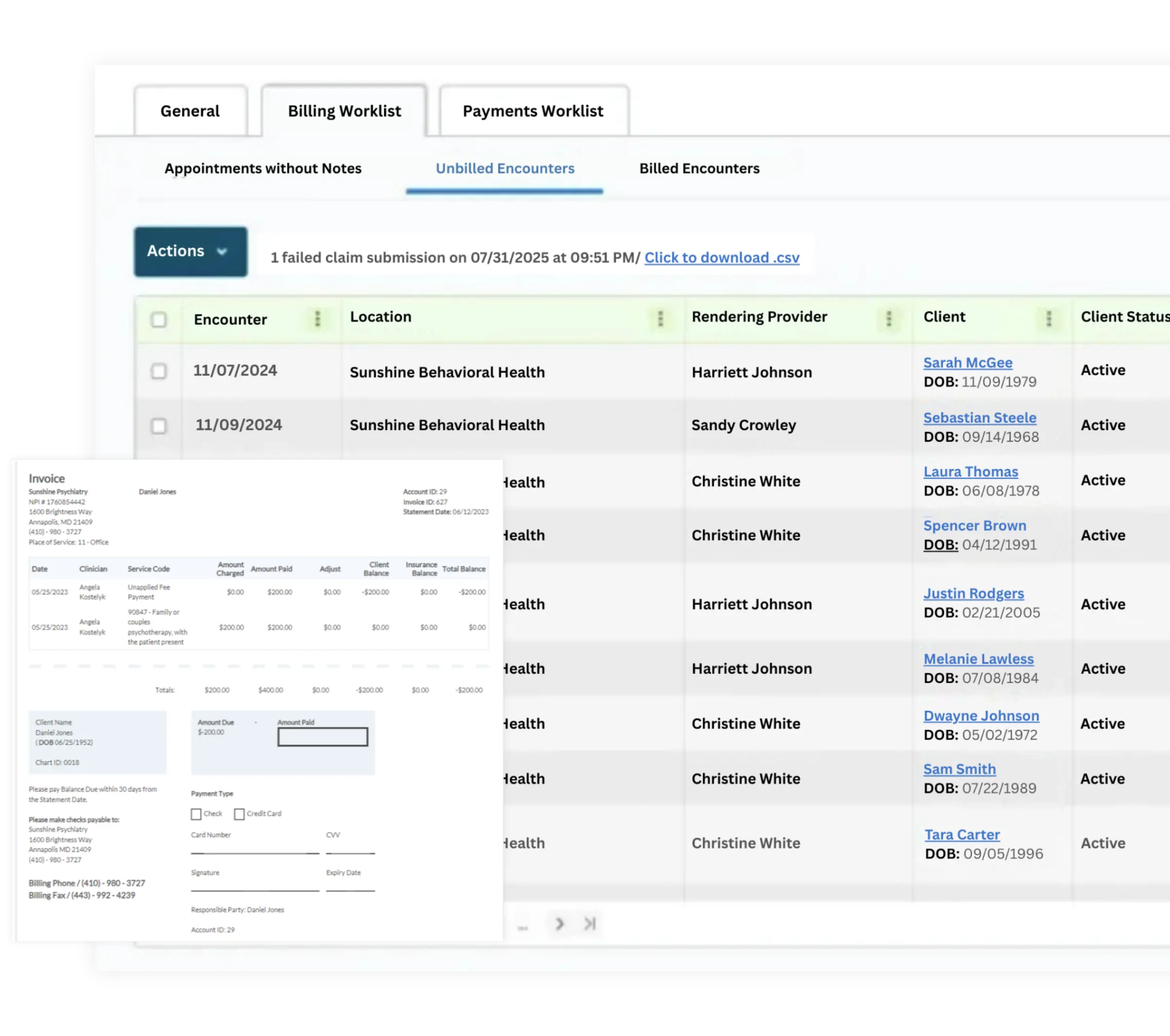
Billing
Automate your entire revenue cycle and improve cash flow with integrated behavioral health billing software.
Submit insurance claims and collect payments
Automatically send invoices and payment reminders
Track revenue and remittances with built-in reporting
- Submit insurance claims and collect payments
- Automatically send invoices and payment reminders
- Track revenue and remittances with built-in reporting
Everything Clinicians Need in One Mental Health EHR
Designed by and for behavioral health professionals, ICANotes puts smarter charting, e-prescribing, telehealth, and integrations into a single platform, so you can spend less time managing technology and more time with clients.

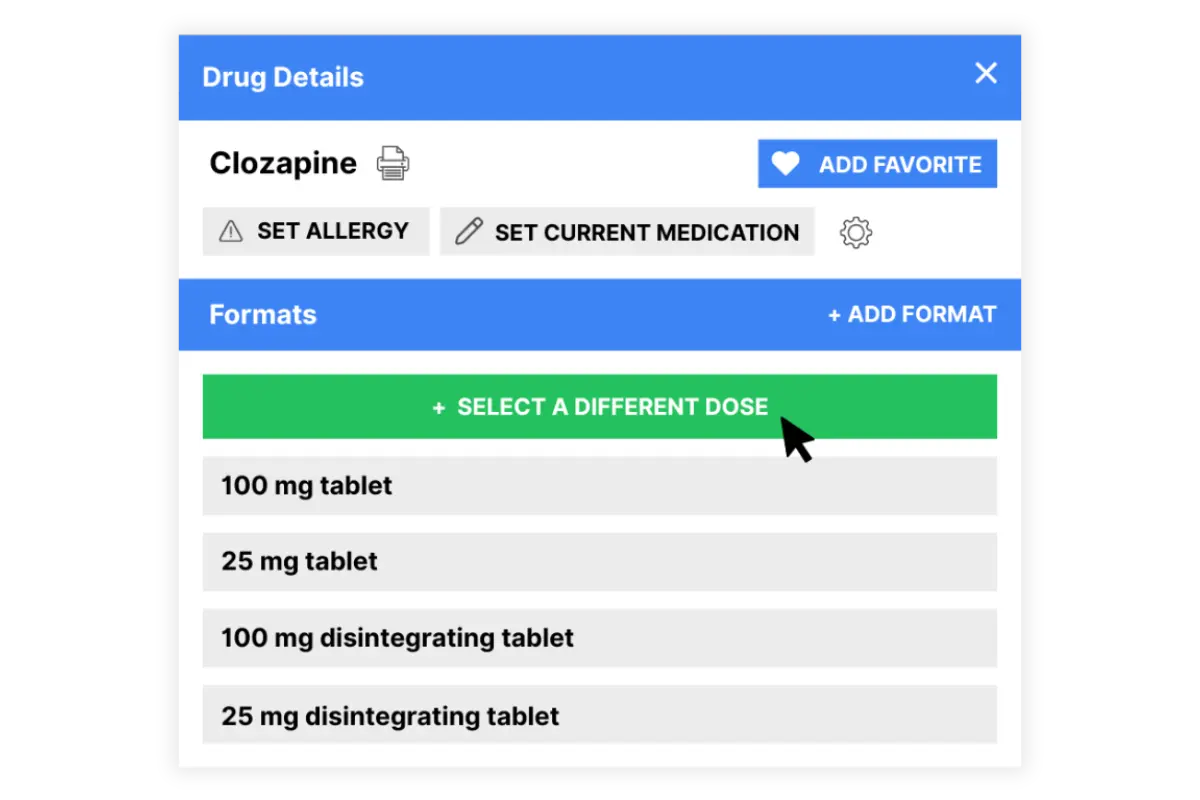
ePrescribing
Prescribe safely and securely with EPCS-compliant tools and integrated PDMP checks, all built into your mental health EMR system.
Smarter Notes with AI
Save time and reduce effort with AI that supports smarter note creation and clinical efficiency.

Integrations
Connect seamlessly with labs, clearinghouses, HIEs, and billing systems.







Built-In Telehealth
Easily schedule, launch, and document virtual visits directly in your behavioral health EHR system without switching platforms.
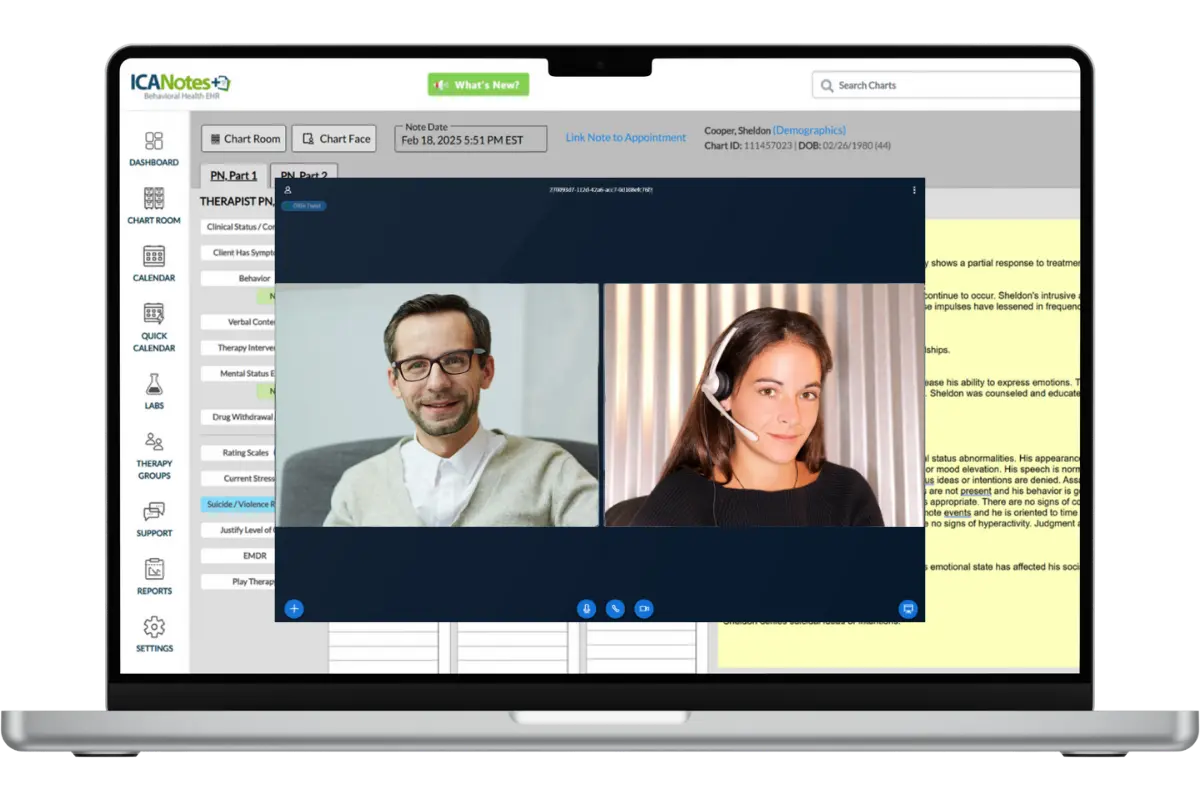
Find out why providers choose ICANotes
Transform your workflow with the mental health EHR built for speed and compliance.
Trusted by 20,000+ clinicians

Tailored EMR & EHR Software for Every Behavioral Health Discipline
ICANotes is purpose-built to meet the unique needs of professionals across the behavioral health spectrum.
Therapists

Smarter Mental Health Charting: Fast, Flexible, and Comprehensive
Customizable Therapy Note Templates
Choose from a library of menu-driven mental health charting templates, such as SOAP, BIRP, DAP, couples therapy, PRP, case management, and group therapy documentation.
Goal-Focused Treatment Planning Tools
Build clear, goal-focused, and actionable treatment plans tailored to each client’s needs.
Progress Tracking Across Clients
Record therapy outcomes for individuals, couples, families, and groups.
Social Workers

Simplify Case Management with Mental Health EHR Software
Case Management Note Templates
Document outreach, follow-ups, and care coordination with menu-driven templates
Integrated with Treatment Plans
Align case notes with life skills, housing, vocational services, and social functioning goals.
Audit-Ready Documentation
Meet Medicaid and insurance compliance requirements with confidence.
Psychologists

EMR for Psychologists that Supports Evidence-Based Care
Built-In Assessment Tools
Use standardized psychological tests and rating scales for accurate evaluation
Evidence-Based Psychology Treatment Plans
Create care plans grounded in proven methodologies
Outcomes Measurement & Tracking
Monitor client progress with standardized measures inside your EHR system.
Psychiatrists

Psychiatry EHR Software for Clinical Decision-Making
Medication Management
Prescribe, adjust, and track medications securely with integrated ePrescribing
Psychiatric Evaluations
Document assessments and mental status exams quickly with menu-driven templates for psychiatry notes
Progress Monitoring
Measure outcomes and refine treatment plans effectively
Nurse Practitioners

Mental Health EMR Tools for Psychiatric Nurse Practitioners
Clinical Documentation
Record visits, exams, and treatment in nurse practitioner notes efficiently with low-typing templates
Medication Management
Prescribe confidently with EPCS-compliant ePrescribing and PDMP checks
Care Coordination
Share records securely with supervisors and care teams using psychiatry EHR software.
Group Therapists

Group Therapy Software for Faster, Compliant Documentation
Group Therapy Note Templates
Document group sessions quickly with the ability to auto-generate individualized group notes for each participant.
Progress Tracking Across Participants
Link session notes to each client’s treatment plan goals, ensuring measurable progress for audits and insurance.
Flexible Documentation Formats
Choose SOAP, DAP, or BIRP styles for group work, while maintaining compliance and clinical clarity.
Expert Support for Your Behavioral Health EMR & EHR Software
Get fast, reliable help from a team that knows behavioral health inside and out — with support tailored to your clinical workflows, documentation, billing, and compliance needs.
Personalized
Onboarding
One-on-one onboarding and implementation designed for mental health EMR workflows included at no extra cost.
Unlimited
Support
Get unlimited support from experts in behavioral health EHR software, available by phone, email, or chat, with no extra fees.
Get Help
on Demand
Whether it’s billing, charting, integrations, or compliance, our team provides on-demand guidance tailored to behavioral health practices.
Accessible
Training
Access live webinars, how-to videos, and an extensive help center, all designed to help you get the most from your EHR software.
Available
24/7
Enjoy 24/7 support — evenings, weekends, and holidays included — so your mental health EMR system is always backed by experts.
What Behavioral Health Clinicians Are Saying About ICANotes
ICANotes stands out among mental health EHR systems for speed, accuracy, and ease of use.
90 minutes
Free Time Gained Daily
Average time saved per clinician
30+
Extra Sessions Billed Monthly
Through improved efficiency
98%
Customer Satisfaction Rate
Clinicians who recommend ICANotes
Frequently Asked Questions: ICANotes Mental Health EHR
Our Recent Posts

Try the Behavioral Health EHR Clinicians Recommend
Join 20,000+ clinicians who've discovered the power of purpose-built behavioral health software.
Complete notes in under 3 minutes
Reduce no-shows by up to 40%
Stay fully HIPAA compliant

“User-friendly and makes note writing a breeze — with excellent support, it’s the best system I’ve ever used.”

Start Your Free Trial
No credit card required • Cancel anytime