Blog > Treatment Strategies > ASPD and ADHD: How to Differentiate Antisocial Personality Disorder vs ADHD
ASPD and ADHD: Understanding the Link Between Antisocial Personality Disorder and ADHD
ASPD and ADHD can present with overlapping traits such as impulsivity, emotional dysregulation, and rule-breaking behavior — which often leads to diagnostic confusion. However, antisocial personality disorder and ADHD are fundamentally different conditions with distinct developmental pathways, neurobiology, and treatment approaches. This clinical guide explores the relationship between ADHD and antisocial personality disorder, clarifies common misconceptions about sociopathy and ADHD, and provides practical guidance for differential diagnosis, risk assessment, and treatment planning for mental health professionals.

Last Updated: April 3, 2026


What You'll Learn
- The key differences between ASPD and ADHD and why they are often confused in clinical practice
- How antisocial personality disorder and ADHD overlap in impulsivity, aggression, and rule-breaking behavior
- Why searches for sociopathy and ADHD or “ADHD sociopath” reflect common misconceptions
- The clinical differences between sociopath vs ADHD presentations
- How ADHD antisocial behavior can appear similar to antisocial personality disorder
- Why some individuals with ADHD want to be alone and how this differs from antisocial withdrawal
- Risk factors that increase the likelihood of antisocial traits in individuals with ADHD
- How clinicians can accurately assess ADHD and antisocial behavior during differential diagnosis
- Evidence-based treatment approaches when ADHD and antisocial personality disorder co-occur
- Best practices for documenting complex ADHD antisocial personality disorder presentations in clinical records
ASPD vs ADHD: Quick Answer
ADHD is a neurodevelopmental disorder characterized by impulsivity, inattention, and emotional dysregulation, while antisocial personality disorder (ASPD) involves a persistent pattern of rule violation, lack of remorse, and interpersonal exploitation. Although both conditions may include impulsive behavior, ADHD-related actions are typically unintentional and followed by regret, whereas ASPD behaviors are often deliberate and associated with reduced empathy.
Introduction
The relationship between ASPD and ADHD has long been a subject of debate among clinicians, researchers, and mental health advocates. Both conditions can surface as behavioral difficulties, impulsivity, and social friction — which makes differential diagnosis challenging but critically important. Clinicians evaluating impulsivity should consider broader patterns of adult ADHD assessment when symptoms have been overlooked.
Antisocial personality disorder and ADHD are separate diagnoses with different developmental pathways, neurobiological substrates, and long-term trajectories. However, they share overlapping traits — particularly impulsivity, poor inhibition, emotional reactivity, and difficulty regulating behavior — that can create diagnostic confusion.
Clinicians frequently encounter clients who present with a complex, overlapping picture including:
- Chronic impulsivity and difficulty with self-control
- Conduct problems that emerged in adolescence
- Significant emotional dysregulation and reactive anger
- Risk-taking and sensation-seeking behaviors
- Social detachment or patterns that appear antisocial
- Troubled interpersonal relationships and occupational instability
This raises critical diagnostic questions that every clinician must address:
- Is this ADHD and antisocial behavior stemming from neurodevelopmental dysregulation?
- Is it a co-occurring presentation of antisocial personality disorder and ADHD?
- Are we mislabeling ADHD-related social withdrawal or reactive impulsivity as sociopathy?
Understanding the distinction between ADHD and antisocial personality disorder is not merely academic — it directly shapes treatment planning, risk assessment, prognosis, and the therapeutic alliance. Misattributing ADHD symptoms to ASPD can lead to stigma, inadequate treatment, and poorer long-term outcomes.
What Is ADHD? A Neurodevelopmental Overview
Attention-Deficit/Hyperactivity Disorder (ADHD) is a neurodevelopmental condition estimated to affect approximately 5-7% of children and 2-5% of adults worldwide. It is one of the most researched psychiatric conditions, yet it remains frequently misunderstood — particularly when ADHD antisocial behavior patterns are present.
Core ADHD Symptom Domains
ADHD is characterized by three core symptom clusters:
- Inattention: Difficulty sustaining focus, frequent careless mistakes, losing items, becoming easily distracted
- Hyperactivity: Excessive motor activity, inability to stay seated, talking excessively, restlessness in adults
- Impulsivity: Acting before thinking, difficulty waiting, interrupting others, emotional reactivity
Critically, impulsivity in ADHD typically stems from deficits in inhibition and executive self-regulation — not from a lack of empathy, moral reasoning, or disregard for others' rights. This distinction is foundational to separating ADHD from antisocial personality disorder.
The Neurobiological Basis of ADHD
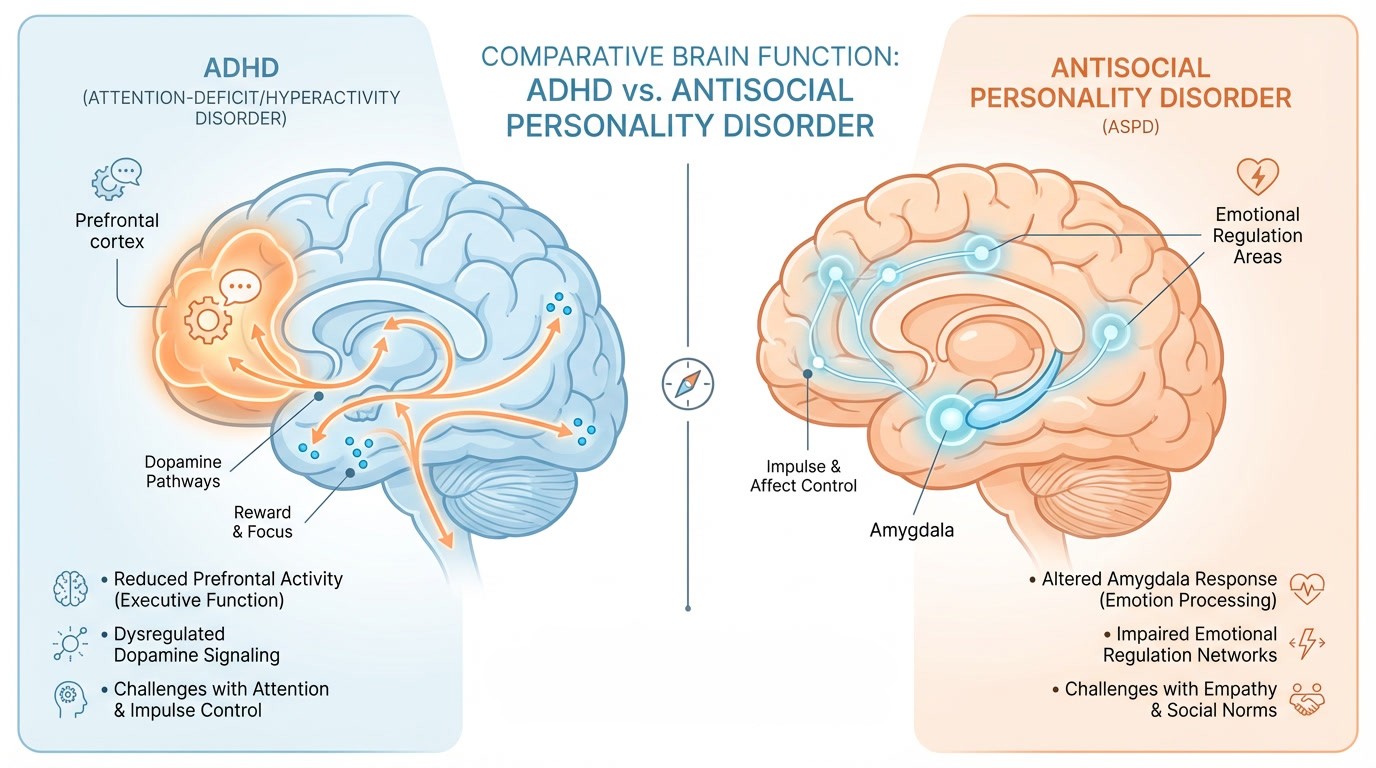
ADHD involves structural and functional differences in the prefrontal cortex, anterior cingulate cortex, and subcortical systems, particularly the dopaminergic and noradrenergic pathways. Neuroimaging studies consistently show reduced volume in frontal-striatal circuits, delayed cortical maturation, and altered connectivity in default mode networks.
This neurobiological foundation explains why ADHD-related impulsivity is reactive and situation-dependent rather than patterned and instrumental. When an individual with ADHD interrupts a conversation, acts without thinking, or struggles to follow rules, it reflects a deficit in the neurological architecture of self-control — not deliberate exploitation or manipulation.
Common Functional Presentations in ADHD
- Acting without thinking through consequences
- Interrupting others mid-sentence without malicious intent
- Strong emotional reactivity and difficulty regulating mood
- Difficulty delaying gratification and tolerating frustration
- Trouble sustaining attention on tasks that lack immediate reward
- Disorganization, forgetfulness, and difficulty managing time
- Rejection sensitive dysphoria — intense emotional pain in response to perceived criticism or failure
While some individuals with ADHD antisocial behavior patterns may struggle significantly in social and occupational settings, the root cause is neurological dysregulation rather than intentional exploitation, manipulation, or callous disregard for others.
What Is Antisocial Personality Disorder (ASPD)?
Antisocial Personality Disorder (ASPD) is a Cluster B personality disorder defined in the DSM-5 by a pervasive pattern of disregard for and violation of the rights of others. Unlike ADHD — which is a neurodevelopmental condition present from childhood — ASPD reflects a deeply ingrained, personality-level pattern of relating to the world.
DSM-5 Diagnostic Criteria for ASPD
To receive a diagnosis of antisocial personality disorder, an individual must be at least 18 years old and show a pervasive pattern of disregarding and violating others' rights since age 15, indicated by three or more of the following:
- Failure to conform to social norms and laws, including repeated grounds for arrest
- Deceitfulness: repeated lying, using aliases, or conning others for personal gain
- Impulsivity or failure to plan ahead
- Irritability and aggressiveness, including repeated physical fights or assaults
- Reckless disregard for one's own safety or the safety of others
- Consistent irresponsibility in work and financial obligations
- Lack of remorse: indifference to or rationalization of having hurt, mistreated, or stolen from another person
Crucially, the diagnosis also requires evidence of Conduct Disorder with onset before age 15. This developmental requirement is essential — and is one of the key diagnostic differentiators when evaluating antisocial personality disorder and ADHD presentations.
The Role of Empathy and Remorse in ASPD
One of the most clinically significant features distinguishing ASPD from ADHD is the nature of empathy and remorse. While individuals with ADHD typically retain emotional empathy — they may feel genuine guilt or distress when they hurt others — individuals with ASPD often demonstrate marked limitations in remorse, empathy, and concern for the consequences of their behavior on others.
This is not merely a surface-level difference. It reflects fundamentally different motivational architectures. ADHD impulsivity is ego-dystonic (unwanted and distressing to the individual). ASPD behavioral patterns are often ego-syntonic — the individual may not perceive a problem with their behavior.
ASPD and ADHD: Where the Overlap Occurs
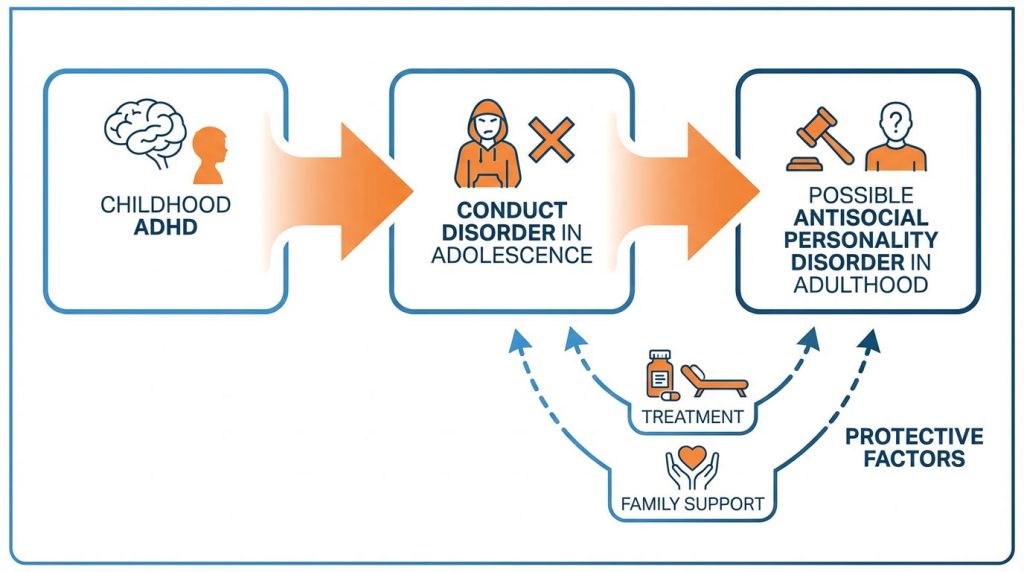
Research consistently demonstrates a significant correlation between childhood ADHD and later conduct problems. Longitudinal studies have shown that untreated ADHD — particularly when combined with environmental risk factors like adverse childhood experiences, inconsistent parenting, peer rejection, or substance use — can increase the likelihood of developing antisocial traits over time.
This developmental trajectory does not mean ADHD causes ASPD. Rather, ADHD represents a neurobiological vulnerability that, in unfavorable environments, may increase risk for conduct disorder and downstream antisocial outcomes. The pathway is moderated by a complex interaction of genetic, environmental, and developmental factors.

Shared Features: ADHD and Antisocial Personality Disorder
| Overlapping Trait | ADHD | ASPD |
|---|---|---|
| Impulsivity | Present — reactive, unplanned | Present — can be calculated or reactive |
| Risk-taking behavior | Present — often seeks stimulation | Present — often self-serving |
| Irritability / Aggression | Present — emotionally reactive | Present — may be predatory |
| Difficulty following rules | Present — often unintentional | Present — often deliberate |
| Emotional dysregulation | Present — core feature | Variable — may mask emotions |
| Substance use risk | Elevated | Elevated |
| Occupational instability | Common | Common |
| Relationship difficulties | Common | Common |
ASPD vs ADHD: Key Differences Clinicians Should Know
Despite these overlaps, several features clearly differentiate the two conditions. Understanding adhd antisocial personality disorder presentations requires close attention to:
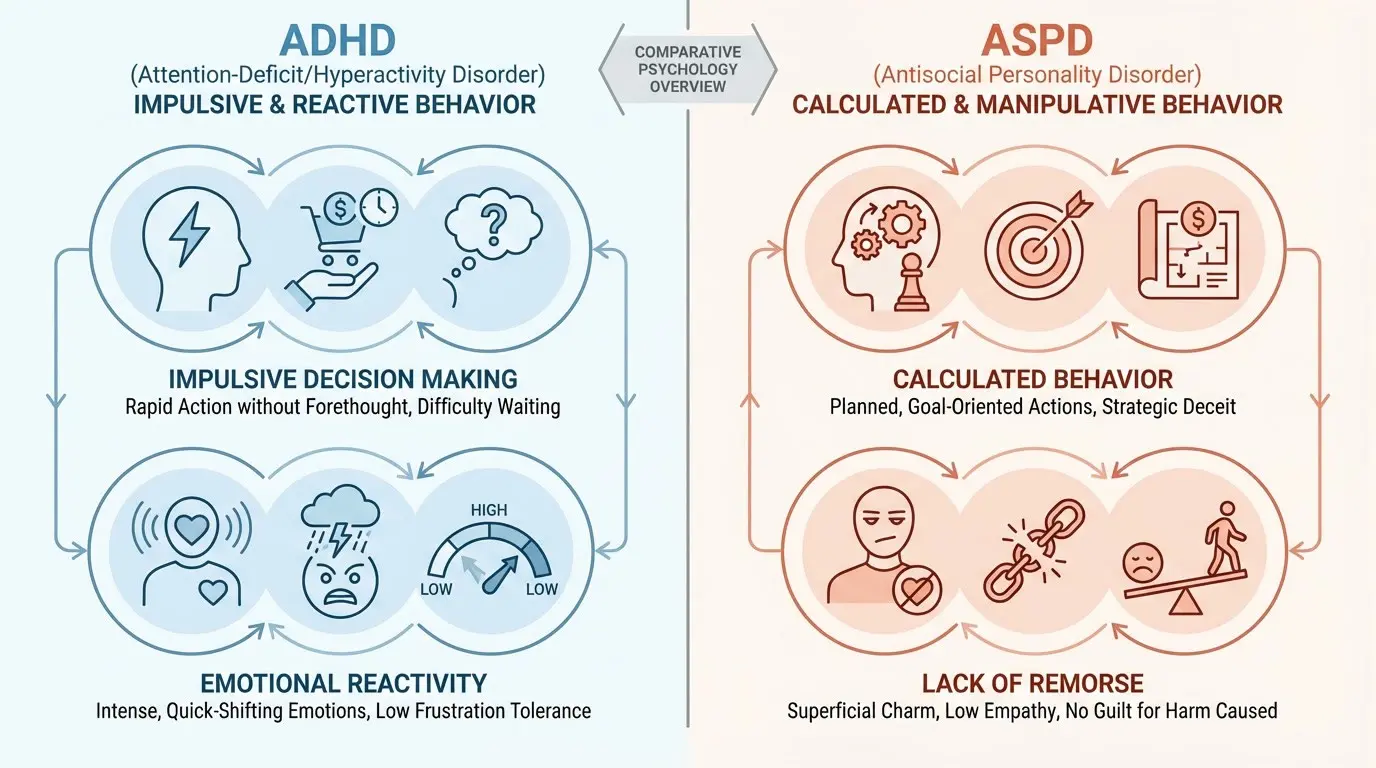
- Intent and Motivation: ADHD impulsivity is typically reactive, unplanned, and ego-dystonic. The individual often regrets impulsive actions afterward. ASPD behavior, by contrast, is frequently strategic, patterned, and ego-syntonic — the individual may show little remorse or even rationalize harmful behavior.
- Empathy Capacity: Most individuals with ADHD retain emotional empathy. They may feel guilty, anxious, or ashamed when they harm others. ASPD involves a significantly diminished capacity for remorse and concern for others' suffering.
- Developmental History: ADHD is identifiable from early childhood as a neurodevelopmental pattern. ASPD requires a documented history of Conduct Disorder before age 15. The absence of this history should prompt reconsideration of an ASPD diagnosis.
- Response to Structure and Support: Individuals with ADHD often show meaningful improvement with appropriate treatment — medication, therapy, environmental accommodations. ASPD shows more limited treatment response, and engagement itself is often more challenging.
- Pattern vs. Situational Behavior: ASPD involves pervasive, cross-situational patterns of interpersonal exploitation. ADHD behaviors, while consistent, are more context-dependent and often improved in structured, engaging environments.
Sociopathy and ADHD: Separating Myth from Clinical Reality
Terms like sociopathy and ADHD or "ADHD sociopath" circulate frequently in online spaces, generating significant confusion among individuals, families, and even less-experienced clinicians. It is essential to address these terms directly and accurately.
"Sociopathy" is not a formal DSM-5 diagnosis. It is a colloquial term historically used to describe traits associated with antisocial personality disorder — particularly rule-breaking, lack of remorse, and interpersonal exploitation. Some researchers distinguish sociopathy from psychopathy, associating sociopathy with more environmentally determined antisocial development, but neither term carries formal diagnostic weight in current U.S. clinical practice.
When people search for sociopath ADHD or ADHD and sociopathy, they are often trying to make sense of impulsive, socially disruptive behavior that can resemble either condition superficially. The clinical reality is more nuanced.
The differences between sociopathy and ADHD often become clearer when comparing clinical traits side-by-side.
Sociopath vs ADHD: Clinical Differences Between ASPD and ADHD
| Clinical Feature | ADHD | Sociopathy (ASPD Traits) |
|---|---|---|
| Core issue | Executive dysfunction, neurological dysregulation | Personality pathology, interpersonal exploitation |
| Remorse for harm | Typically present and genuine | Often absent, minimized, or feigned |
| Rule-breaking | Impulsive, situational, unintentional | Patterned, persistent, often deliberate |
| Desire to harm others | Rare; behavior affects others incidentally | May be present; behavior can target others |
| Lying and deception | May occur impulsively or defensively | Patterned deceitfulness for personal gain |
| Treatment responsiveness | Often responds well to treatment | More limited treatment response |
| Relationship to others | Wants connection; often struggles socially | Instrumental; uses relationships for gain |
| Self-awareness | Often high; may be distressed by symptoms | Often limited; behavior feels justified |
Clinical Note: Conflating ADHD and sociopathy can cause serious harm. It may lead to stigmatizing clients, applying inappropriate treatment models, and missing the real neurodevelopmental diagnosis — or vice versa. The distinction requires careful developmental history, collateral information, and longitudinal observation.
The differences between ASPD and ADHD often become clearer when clinicians assess symptom onset, remorse, conduct history, and whether the behavior is reactive or deliberate. While the table above highlights the key clinical differences between sociopathy and ADHD, the following pathway illustrates how clinicians may approach differential diagnosis in practice.
ASPD vs ADHD: A Simple Differential Diagnosis Pathway
When evaluating impulsive, disruptive, or antisocial-appearing behavior, clinicians should look beyond surface symptoms and assess developmental history, empathy, remorse, and behavioral patterns over time.
- Symptoms begin in childhood
- Impulsivity is reactive and unplanned
- Remorse is present after harm occurs
- Behavior improves with structure or treatment
- Social problems stem from dysregulation, not exploitation
- History of conduct disorder before age 15
- Rule-breaking is persistent and often deliberate
- Remorse is limited, absent, or feigned
- Pattern of manipulation or exploitation
- Behavior reflects pervasive personality-level traits
ADHD and Antisocial Behavior in Adolescence
Adolescence represents a critical developmental window where the trajectories of ADHD and potential antisocial development intersect most meaningfully. Understanding this intersection is essential for clinicians working with youth and families.
Youth with ADHD face elevated risk for a range of externalizing problems, including:
- Oppositional Defiant Disorder (ODD): Affects approximately 40-60% of children with ADHD
- Conduct Disorder (CD): Affects approximately 14-25% of children with ADHD
- Substance use initiation at earlier ages
- Academic failure and school dropout
- Peer rejection and social marginalization
- Juvenile justice system involvement
However, it is critical to emphasize: not all youth with ADHD develop conduct disorder, and not all youth with conduct disorder go on to develop antisocial personality disorder. The relationship is probabilistic and moderated by a range of protective and risk factors. Early intervention using behavioral therapy for ADHD, including structured approaches like ABA, can significantly reduce the risk of conduct-related difficulties. Access to structured ADHD interventions for children and adolescents can play a critical role in preventing escalation into more severe behavioral patterns.
Risk Factors That Increase ADHD-to-Antisocial Trajectories
- Untreated or undertreated ADHD with persistent impulsivity
- Adverse Childhood Experiences (ACEs) including abuse, neglect, or household dysfunction
- Inconsistent or harsh parenting practices
- Peer group with antisocial norms
- Early substance use
- Trauma exposure
- Comorbid Oppositional Defiant Disorder
- Callous-unemotional traits in childhood
Protective Factors That Mitigate Risk
- Early, accurate ADHD diagnosis and treatment initiation
- Consistent medication management that reduces impulsivity
- Evidence-based behavioral interventions (Parent Management Training, CBT)
- Stable, warm, and supportive family systems
- Social skills training and peer support programs
- Educational accommodations that reduce academic frustration
- Positive mentoring relationships with non-family adults
When evaluating ADHD antisocial behavior in adolescents, clinicians should assess environmental influences alongside neurological vulnerability rather than attributing all behavioral problems to a single diagnosis.
ADHD and Wanting to Be Alone: Understanding Social Withdrawal
A surprisingly common search query is "ADHD and wanting to be alone" — and it reflects a real and often misunderstood experience for many individuals with ADHD. This is not antisocial behavior in the clinical sense, but it is frequently misinterpreted as such.
Social withdrawal in ADHD is a multidimensional phenomenon that can stem from several overlapping sources:
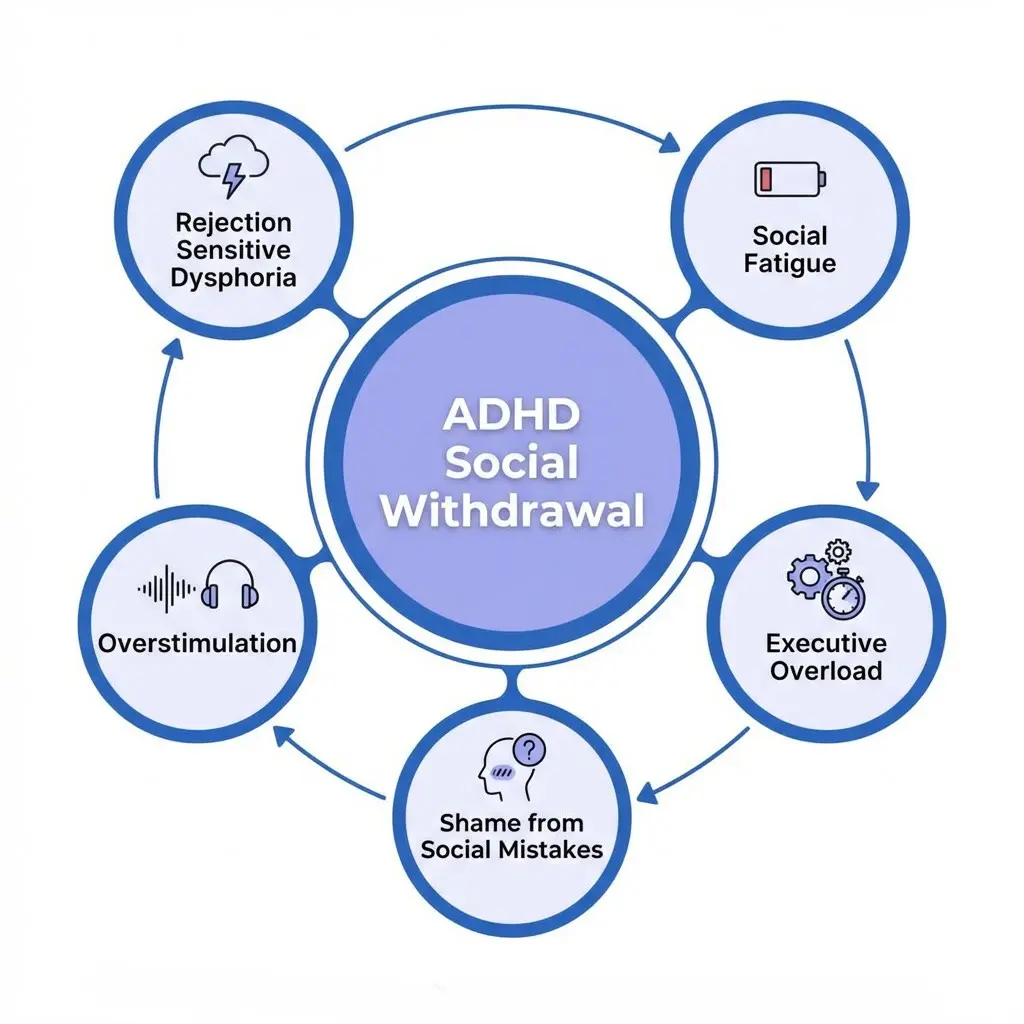
Why Individuals with ADHD May Withdraw Socially
Social fatigue: Social interactions require significant executive resources — tracking conversation, managing impulses, reading social cues. For individuals with ADHD, sustained social engagement can be genuinely exhausting.
Rejection sensitive dysphoria (RSD): Many individuals with ADHD experience intense, sometimes overwhelming emotional pain in response to perceived rejection, criticism, or failure. Withdrawal may be a protective strategy to avoid this pain.
Overstimulation: Environments with high sensory input, competing conversations, or unpredictable social demands can trigger dysregulation. Solitude provides regulation and recovery.
Executive function overload: Managing social reciprocity, small talk, timing, and emotional modulation simultaneously strains already-taxed executive systems.
Shame and self-protection: After repeated social missteps — interrupting, missing cues, saying the wrong thing — individuals with ADHD may withdraw to avoid further embarrassment.
Sensory sensitivity: Comorbid sensory processing differences, common in ADHD, can make crowded or noisy environments genuinely aversive.
Key Distinction: ADHD-related social withdrawal is typically protective, rooted in dysregulation, and involves genuine desire for connection — even when avoidance behavior predominates. Antisocial withdrawal in ASPD reflects a fundamentally different relationship with others: instrumental, indifferent, or exploitative. ADHD and antisocial patterns are not the same phenomenon.

Assessment Considerations for Clinicians: Differential Diagnosis
Accurately differentiating antisocial personality disorder ADHD presentations requires a comprehensive, multi-method assessment approach. No single measure or clinical interview is sufficient. The following framework provides a structured approach. Clinicians should also consider identifying undiagnosed ADHD in adults, particularly when impulsivity and functional impairment have been present but previously misattributed.
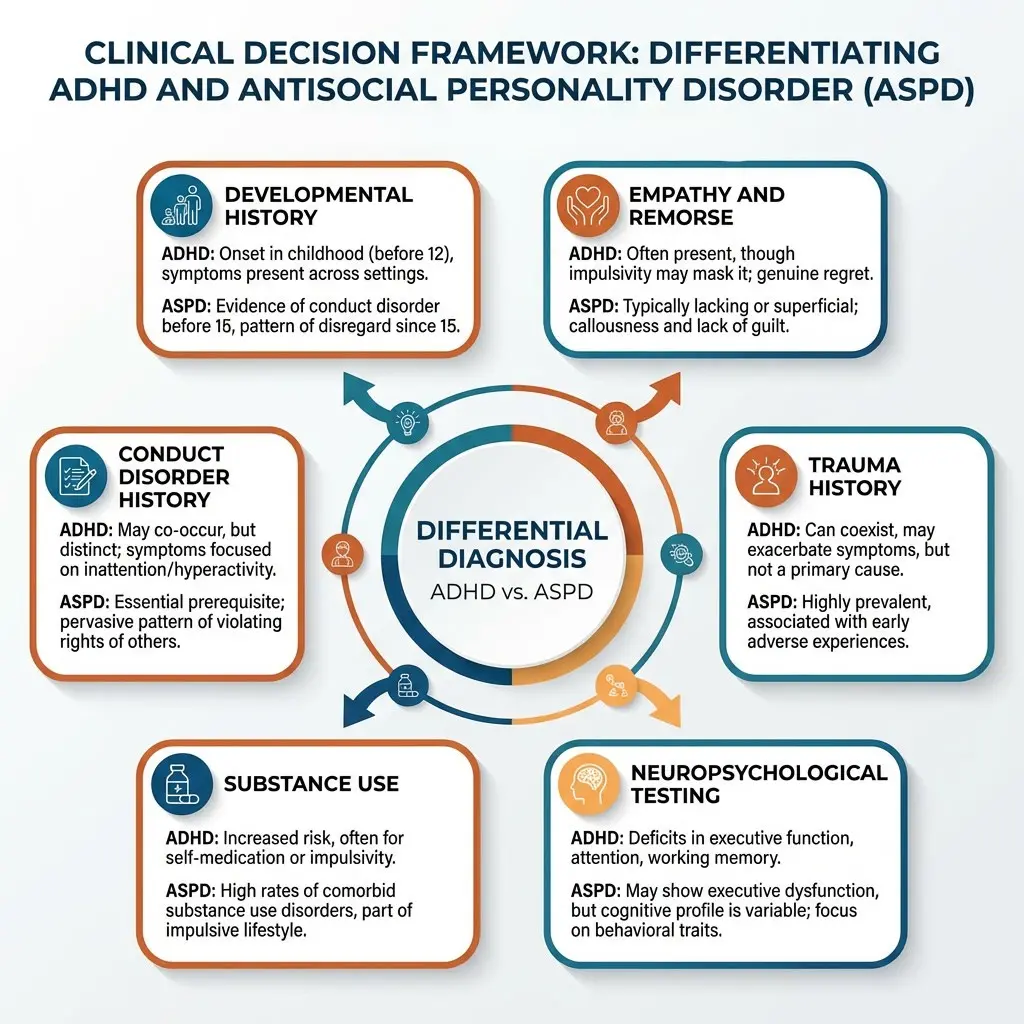
Core Assessment Domains
A thorough differential diagnosis of ASPD and ADHD requires a structured, multi-domain assessment process that looks beyond surface-level impulsivity or rule-breaking behavior.
Developmental and Longitudinal History
Document the onset and developmental progression of symptoms. ADHD symptoms should be traceable to early childhood before age 12. ASPD requires evidence of Conduct Disorder before age 15. Collateral history from parents, school records, and prior evaluations is essential.
Conduct Disorder Evaluation
Systematically evaluate for conduct disorder criteria, including aggression to people or animals, destruction of property, deceitfulness or theft, and serious rule violations. The absence of childhood conduct disorder essentially rules out an ASPD diagnosis.
Empathy and Remorse Assessment
Assess the individual’s capacity for genuine remorse and empathy. Distinguish between absence of remorse, which may indicate ASPD, and impaired access to emotional states caused by dysregulation, which is more consistent with ADHD.
Pattern vs. Situational Analysis
Determine whether problematic behavior is cross-situational and pervasive, which may indicate ASPD, or context-dependent and variable, which is more consistent with ADHD. Assess functioning across work, relationships, finances, legal history, and family systems.
Neuropsychological Profile
Consider standardized neuropsychological testing to document executive functioning deficits consistent with ADHD. Measures of inhibition, working memory, and sustained attention can help distinguish neurological impulsivity from intentional behavior.
Trauma and Adverse Experience History
Trauma can produce behavioral profiles that overlap with both ADHD and ASPD. A thorough trauma history helps contextualize the behavior and identify underlying drivers.
Substance Use Assessment
Substance use is elevated in both ADHD and ASPD and can significantly complicate symptom presentation. Clarify the timeline of substance use relative to behavioral symptoms.
Structured and Semi-Structured Instruments
Consider validated tools including ADHD rating scales such as ADHD-RS-5 and CAARS, Conners’ Adult ADHD Rating Scales, the PCL-R or similar instruments for antisocial trait evaluation, the SCID-5-PD, and collateral behavioral rating scales where possible.
Treatment Implications: Tailoring Interventions to the Correct Diagnosis
The treatment approach for ADHD differs fundamentally from treatment for ASPD — and misdiagnosis in either direction has meaningful clinical consequences. When both conditions co-occur, treatment planning requires careful sequencing and integration.
Treating ADHD: Evidence-Based Approaches
Pharmacological Interventions: Stimulant medications (methylphenidate, amphetamine salts) are first-line treatments and can significantly reduce impulsivity, inattention, and hyperactivity. Non-stimulant options (atomoxetine, guanfacine, bupropion) are available for individuals with substance use concerns, cardiovascular contraindications, or poor stimulant response.
Cognitive-Behavioral Therapy (CBT): CBT adapted for ADHD targets executive functioning deficits, time management, emotional regulation, and dysfunctional thinking patterns. Structured, skills-based formats are most effective. For clinicians exploring ADHD treatment without medication, behavioral and skills-based interventions can significantly improve functioning when tailored appropriately.
Emotional Regulation Training: DBT skills, mindfulness-based interventions, and emotion-focused strategies can help individuals manage rejection sensitive dysphoria, emotional reactivity, and impulse control challenges.
Organizational Skills Training: Direct training in planning, prioritization, task management, and routine development addresses functional impairments that drive occupational and relational difficulties.
Environmental Accommodations: Workplace accommodations, structured routines, and environmental modifications can dramatically improve functioning by reducing executive demands.
Treating ASPD: Evidence-Based and Harm-Reduction Approaches
Motivational Interviewing: MI is often the most viable early intervention, meeting the individual where they are and building intrinsic motivation for change without confrontation.
Structured Behavioral Approaches: Clear, consistent behavioral contracting with predictable consequences. Schemas-based therapy approaches show some promise in research settings.
Substance Use Treatment Integration: Given the high co-occurrence of substance use disorders with ASPD, integrated dual-diagnosis treatment is often necessary.
Risk Management and Safety Planning: For individuals with significant violence risk, structured risk assessment tools (HCR-20, VRAG) inform safety planning and treatment intensity.
Long-Term Therapeutic Alliance: ASPD treatment rarely produces rapid change. Building a stable, consistent therapeutic relationship over years — not months — is the foundation of whatever progress is possible.
When ADHD and ASPD Co-Occur
Comorbid presentations require careful treatment sequencing. Addressing ADHD symptoms first — particularly impulsivity through medication — may reduce behavioral dyscontrol and create a more workable foundation for addressing antisocial patterns. Clinicians should avoid using ASPD comorbidity as a reason to deny ADHD treatment, as untreated ADHD impulsivity can worsen antisocial outcomes.
Important: Misdiagnosing ADHD and antisocial personality disorder — in either direction — can result in ineffective treatment at best and harmful treatment at worst. Accurate differential diagnosis is an ethical obligation and is essential for building an effective mental health treatment plan.
Why Accurate Clinical Documentation Matters
When documenting cases involving ASPD and ADHD, clinicians carry both a clinical and ethical responsibility to distinguish accurately between neurodevelopmental impulsivity and personality-based behavioral patterns. Inadequate documentation in complex presentations creates risk — for the client, for the clinician, and for the treatment team.
What Documentation Should Address in ASPD/ADHD Cases
- Clear delineation of neurodevelopmental impulsivity versus personality-level behavioral patterns
- Documented developmental history, including conduct disorder onset and ADHD symptom timeline
- Evidence base for diagnosis, including assessment instruments used and clinical reasoning
- Empathy, remorse, and interpersonal relationship patterns
- Environmental factors and contextual influences on behavior
- Comorbid conditions including substance use, trauma history, and mood disorders
- Risk indicators and safety planning documentation
- Functional impairment across life domains
- Treatment rationale and plan responsiveness to documented diagnosis
Following mental health documentation best practices in these cases supports ethical diagnosis, medical necessity justification, risk management, audit protection, and coordinated care across treatment providers. It also protects clinicians in the event of adverse outcomes or regulatory review.
Related Resources for Clinicians
Explore additional guides on ADHD assessment, behavioral interventions, and differentiating complex clinical presentations.
Explore non-medication approaches to ADHD treatment.
Learn how to recognize overlooked ADHD symptoms in adults.
Understand behavioral therapy approaches for ADHD.
Compare personality disorders with overlapping features.
Access tools and strategies for children and adolescents.
How ICANotes Supports Complex Differential Diagnosis Documentation
For clinicians working with overlapping presentations like ADHD and antisocial personality disorder, documentation clarity is not just a quality concern — it is a risk management and clinical ethics issue. ICANotes provides the structured infrastructure clinicians need to document complex differential diagnoses with precision and defensibility.
ICANotes features that support ADHD and ASPD documentation include:
- Structured diagnostic templates for ADHD, conduct disorder, and personality disorders that prompt clinicians to document criteria-specific evidence.
- Built-in rating scales and symptom checklists that capture quantitative symptom data over time.
- Longitudinal tracking of behavioral patterns across sessions, enabling pattern versus situational behavior analysis.
- Integrated risk assessment documentation prompts that capture safety-relevant data consistently.
- Progress note templates that distinguish impulsivity from persistent antisocial traits across clinical encounters.
- DSM-5 aligned diagnostic language that supports medical necessity and audit defensibility.
Clear, structured documentation reduces liability risk and supports defensible clinical reasoning — especially in complex cases involving ADHD antisocial behavior patterns where the stakes of misdiagnosis are high.
Start a 30-Day Free Trial (no credit card required) — Explore how ICANotes helps streamline differential diagnosis documentation for complex presentations.
Experience ICANotes — Free for 30 Days
ICANotes helps behavioral health clinicians document complex cases with structured, audit-ready notes and built-in clinical tools designed specifically for mental health workflows.
Start your free trial to see how ICANotes simplifies clinical documentation, supports differential diagnosis, and streamlines behavioral health practice management.
Purpose-built for mental health clinicians, therapists, and psychiatric providers.
Capture detailed, compliant documentation with less typing.
Built-in assessments, treatment plans, scheduling, and billing tools.
Start Your Free Trial
Complete the form below to create your ICANotes account.
Frequently Asked Questions
Final Thoughts: The Clinical Imperative of Accurate Diagnosis
The overlap between ASPD and ADHD lies primarily in impulsivity — but impulsivity alone does not equal antisocial personality disorder. The clinical imperative is to look beneath the surface behavior to understand its origins, its developmental history, its motivational architecture, and its relationship to empathy and remorse.
Careful assessment, longitudinal observation, collateral information, and precise documentation are the foundations of distinguishing ADHD-related dysregulation from emerging or established antisocial personality disorder. This is not merely a diagnostic exercise — it determines the treatment trajectory, therapeutic relationship, risk management approach, and ultimate prognosis for the individuals in our care.
For clinicians, understanding the nuance between antisocial personality disorder and ADHD prevents stigma, improves treatment outcomes, supports ethical practice, and strengthens diagnostic accuracy. When we get this distinction right, our clients are better served — and that is the fundamental purpose of clinical excellence.
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.





