Blog > Treatment Strategies > Interventions for Depression: Evidence-Based Techniques (CBT, ACT, DBT)
Interventions for Depression: Evidence-Based Techniques for Clinicians
Depression treatment requires more than a one-size-fits-all approach. This guide explores the most effective interventions for depression, including CBT interventions for depression, ACT techniques, DBT skills, and nonpharmacological interventions such as behavioral activation and lifestyle strategies. You’ll learn how to match therapeutic interventions for depression to each client’s presentation using a practical, evidence-based framework designed for real-world clinical settings.

Last Updated: April 8, 2026


What You'll Learn
- The five core categories of interventions for depressive disorders — cognitive, behavioral, somatic, psychoeducational, and lifestyle — and how to apply each in clinical practice
- How to choose and match the right intervention to each client using a practical, in-session decision framework
- Evidence-based techniques including CBT, behavioral activation, IPT, and mindfulness-based cognitive therapy for depression
- Real-world tools to improve client engagement, including activity scheduling, symptom tracking, and structured prompts
- How to document depression interventions, treatment plans, and progress efficiently and compliantly using ICANotes
Contents
How to Choose the Right Intervention for Depression
How to Match Interventions for Depression to Each Client
Understanding Depressive Disorders and Clinical Presentation
Core Therapeutic Interventions for Depressive Disorders
Using Depression Assessment Tools to Measure Treatment Outcomes
Depression is one of the most prevalent mental health conditions in the United States, affecting approximately 8.4% of adults in any given year and ranking among the leading causes of disability worldwide. For clinicians, the challenge isn’t just diagnosis — it’s selecting the most effective interventions for depression based on each client’s unique presentation.
With a wide range of evidence-based interventions for depression available — from cognitive behavioral therapy (CBT) and behavioral activation to interpersonal therapy (IPT) and mindfulness-based cognitive therapy (MBCT) — selecting the right technique requires careful clinical reasoning. The most effective depression treatment plans don’t rely on a single method, but instead match therapeutic interventions for depression to each client’s symptom profile, comorbidities, and functional impact.
This guide breaks down the most effective evidence-based interventions for depression, including CBT interventions for depression, ACT techniques, DBT skills, and nonpharmacological interventions such as behavioral activation and lifestyle strategies. Rather than relying on a one-size-fits-all approach, you’ll learn how to match therapeutic interventions for depression to cognitive, behavioral, interpersonal, and somatic symptom patterns.
Whether you’re treating a client with persistent negative thinking, behavioral withdrawal, or recurrent depressive episodes, this article provides a practical framework you can use in session to choose, apply, and adjust interventions with confidence.
What are the most effective interventions for depression?
The most effective interventions for depression include cognitive behavioral therapy (CBT), behavioral activation, acceptance and commitment therapy (ACT), interpersonal therapy (IPT), and mindfulness-based approaches. The best intervention depends on the client’s primary symptoms, such as negative thinking, withdrawal, interpersonal stress, or relapse risk.
How to Choose the Right Intervention for Depression
Not every client with depression needs the same treatment approach. The most effective interventions for depression depend on what is driving the client’s symptoms, how those symptoms manifest in daily life, and whether there are complicating factors such as anxiety, trauma, substance use, chronic medical conditions, or limited motivation — often identified through standardized screening and depression assessment tools.
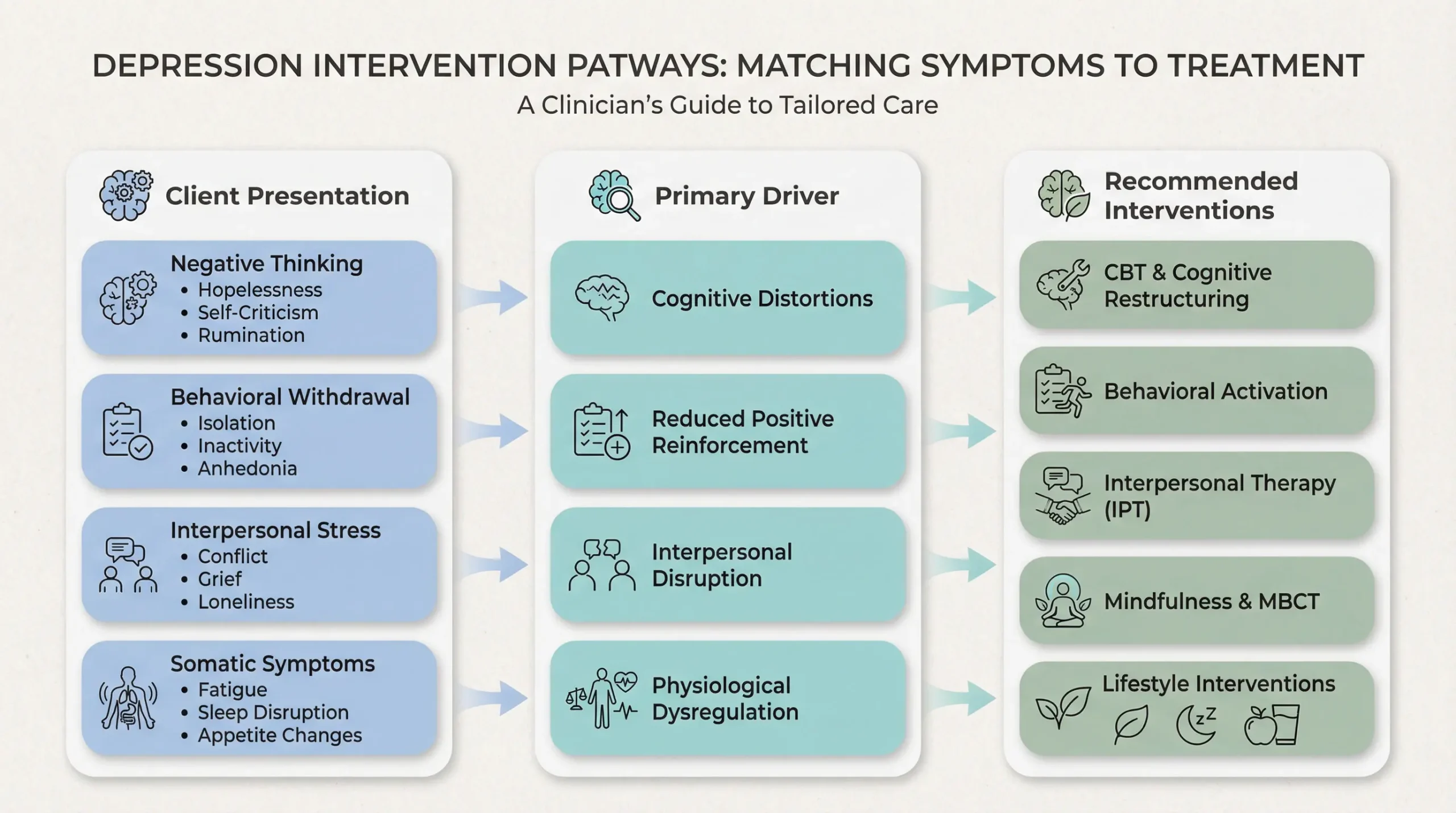
A client whose depression is driven primarily by negative cognitive patterns — self-criticism, hopelessness, rumination — may respond well to cognitive restructuring and other CBT interventions for depression. A client whose life has narrowed due to withdrawal and inactivity may benefit more from behavioral activation. For clients whose depression is rooted in interpersonal conflict, role transitions, or social isolation, interpersonal therapy (IPT) offers a structured framework. And for clients with recurrent depression who need skills to prevent relapse, mindfulness-based cognitive therapy (MBCT) provides tools for recognizing early warning signs.
The goal is not to choose one intervention category permanently. In practice, clinicians often begin with the pathway that best matches the client’s primary presentation, then adjust over time based on outcomes, engagement, and comorbid needs. Using this kind of structured decision-making can make your treatment planning more efficient and your interventions more targeted.
Not sure where to start? Use this quick decision framework to match your client’s presentation with the most effective intervention pathway.
Depression Intervention Decision Tree
Use this decision tree to match the client’s dominant presentation with the most appropriate starting point. Most clients benefit from a blended approach, but beginning with the primary pattern can improve engagement and clinical momentum.
Then adjust for complexity
Consider comorbid anxiety, trauma history, substance use, chronic medical conditions, personality factors, suicidal ideation, developmental stage, or treatment resistance. Modify pacing, integrate modalities, and reassess regularly using tools like the PHQ-9 to guide clinical decisions.
How to Match Interventions for Depression to Each Client
Choosing an intervention category is only the first step. In practice, effective treatment requires clinicians to adapt and combine interventions for depression based on each client’s presentation, comorbidities, and response to treatment over time.
Match the primary driver of depression (cognitive, behavioral, interpersonal, somatic) before layering additional techniques.
Combine CBT, behavioral activation, IPT, mindfulness, or skills-based techniques to address multiple symptom pathways.
Integrate anxiety management, trauma-informed pacing, substance use considerations, chronic pain adaptations, or personality-related needs as appropriate.
Use tools like the PHQ-9 to track progress and adjust interventions when symptom improvement plateaus or clinical needs change.
In real-world practice, clinicians rarely rely on a single technique. For example, a client with depression characterized by social withdrawal may begin with behavioral activation to rebuild routine and engagement, while also using cognitive restructuring to challenge beliefs like “Nothing will ever get better” and interpersonal strategies to address relationship strain that reinforces isolation.
Treatment planning should remain flexible. If a client is not responding to a chosen intervention after several sessions, clinicians should reassess the underlying drivers of depression and consider shifting approaches or integrating additional modalities. Depression measurement tools like the PHQ-9 can help guide these decisions objectively.
Ultimately, the most effective therapeutic interventions for depressive disorders are those that evolve alongside the client’s progress and needs.
Understanding Depressive Disorders and Clinical Presentation
Depression involves more than sadness. It is characterized by persistent low mood, diminished interest or pleasure, and a constellation of cognitive, behavioral, and somatic symptoms that impair daily functioning. Clients may present with cognitive symptoms (hopelessness, worthlessness, difficulty concentrating, indecisiveness), behavioral symptoms (social withdrawal, reduced activity, psychomotor retardation or agitation), somatic symptoms (fatigue, sleep disruption, appetite changes, chronic pain), and emotional symptoms (pervasive sadness, irritability, emotional numbness, guilt).
Common depressive disorders include Major Depressive Disorder (MDD), Persistent Depressive Disorder (Dysthymia), Premenstrual Dysphoric Disorder (PMDD), Seasonal Affective Disorder (SAD), Postpartum Depression, and Adjustment Disorder with Depressed Mood. Depression frequently co-occurs with anxiety disorders, PTSD, substance use disorders, ADHD, chronic pain conditions, and medical illnesses such as diabetes, cardiovascular disease, and autoimmune disorders.
Using standardized tools can help track symptom progression over time and inform treatment decisions — especially when paired with structured approaches like those covered in our depression assessment tools guide.
Core Therapeutic Interventions for Depressive Disorders
Interventions for depressive disorders can be divided into five categories: cognitive, behavioral, somatic, psychoeducational, and lifestyle-based techniques. The following sections detail how these categories function and which evidence-based strategies fall into each one. For many clients, an integrative approach that draws from multiple categories produces the strongest outcomes.
CBT Interventions for Depression: Techniques Clinicians Can Use in Session
Cognitive-behavioral therapy (CBT) is one of the most extensively researched and effective therapeutic interventions for depressive disorders. CBT interventions for depression target the self-reinforcing cycle of negative thinking, behavioral withdrawal, and low mood, helping clients build more adaptive patterns over time.
Rather than focusing on a single technique, CBT for depression typically combines cognitive and behavioral strategies that help clients evaluate their thoughts, test their assumptions, and re-engage with meaningful activities.
How CBT Works in Depression Treatment
CBT helps clients identify automatic negative thoughts such as “I’m worthless” or “Nothing will change,” evaluate the evidence behind those thoughts, and develop more balanced alternatives.
This process is reinforced through structured tools like thought records, behavioral experiments, and activity tracking, which help clients move from insight to real-world change. Over time, clients learn to recognize depressive thinking patterns earlier and respond to them more flexibly, reducing the intensity and duration of depressive episodes.
CBT Thought Record Example
A client records the triggering situation, the automatic thought (“I’m a failure at everything”), the evidence for and against that thought, and a replacement thought (“I’m struggling in one area, but I’ve succeeded in others and can ask for support”). Over time, this practice helps clients recognize patterns in their thinking and develop greater cognitive flexibility.
Core CBT and Cognitive Interventions for Depression
CBT interventions for depression can be used individually or combined based on the client’s needs:
- Thought challenging and cognitive restructuring help clients identify distortions such as all-or-nothing thinking, overgeneralization, and self-blame, then replace them with more balanced perspectives.
- Behavioral experiments allow clients to test depressive predictions in real-world situations, helping disconfirm beliefs like “Nothing I do matters” or “No one wants to hear from me.”
- ACT and cognitive flexibility techniques help clients change their relationship to depressive thoughts by increasing acceptance, defusion, and values-based action rather than trying to eliminate thoughts entirely.
- Mindfulness-Based Cognitive Therapy (MBCT) supports clients in recognizing early warning signs of relapse and disengaging from rumination before it escalates.
- Journaling and emotional processing help clients track patterns in mood, triggers, and thinking, building insight into how their internal experiences influence behavior.
For clinicians who want to implement CBT systematically, our guide to treatment goals for depression explains how to align CBT interventions with SMART goals and measurable outcomes.
Why CBT is Effective for Depression
Depression is maintained by a feedback loop between thoughts, behaviors, and mood. CBT directly targets this loop by helping clients:
- Interrupt negative thinking patterns
- Increase engagement with rewarding activities
- Test and revise unhelpful beliefs
- Build long-term coping skills
Because CBT is structured, measurable, and adaptable, it is often used as a foundational approach that can be combined with behavioral, somatic, and interpersonal interventions.
Download the Depression Intervention Cheat Sheet
Need a faster way to match symptoms to treatment? This practical cheat sheet gives clinicians a structured, quick-reference guide to evidence-based interventions for depression.
Cognitive Interventions for Depression: Thought Restructuring, ACT, and MBCT Techniques
Beyond structured CBT programs, several cognitive techniques can be used as standalone interventions or integrated into a broader treatment plan. These approaches help clients identify, challenge, and change their relationship to the unhelpful thought patterns that maintain depression.
Help clients identify and reframe depressive thinking patterns such as hopelessness, self-criticism, and persistent rumination.
Best for: Negative self-talk, hopelessness, cognitive distortions, and rumination
Use evidence testing, alternative interpretations, and balanced replacement thoughts to reduce the impact of depressive beliefs.
Best for: All-or-nothing thinking, self-blame, guilt, and overgeneralization
Test depressive predictions in real life so clients can compare expected outcomes with what actually happens.
Best for: Defeatist beliefs, social withdrawal, and assumptions like “nothing will help” or “no one cares”
Help clients change their relationship to depressive thoughts by increasing acceptance, defusion, and values-based action.
Best for: Chronic depression, stuck patterns, experiential avoidance, and loss of meaning
Combine mindfulness with cognitive awareness to help clients notice depressive thought patterns earlier and interrupt relapse cycles.
Best for: Recurrent depression, relapse prevention, and repetitive negative thinking
Use structured journaling to help clients track triggers, emotional patterns, and the connection between mood, thoughts, and behavior.
Best for: Building insight, identifying patterns, and supporting emotional processing between sessions
Thought Challenging and Cognitive Restructuring
This technique helps clients step back from automatic negative thoughts and evaluate them more objectively. Clinicians may use Socratic questioning (“What would you say to a friend in this situation?”) or work with clients to identify cognitive distortions such as overgeneralization, personalization, or mental filtering. Over time, clients develop the ability to catch distorted thinking in real time and generate more balanced alternatives.
Behavioral Experiments for Depression
Behavioral experiments help clients test the accuracy of depressive beliefs in real-world situations. Rather than relying on assumptions like “Nothing will help” or “No one wants to hear from me,” clients are encouraged to make predictions, take action, and compare expected outcomes with what actually happens.
For example, a client who believes reaching out will lead to rejection might agree to send a message to a friend and then evaluate the response. Over time, these structured experiments help weaken rigid, negative beliefs and replace them with more flexible, evidence-based thinking.
Acceptance and Cognitive Flexibility
Acceptance and Commitment Therapy (ACT) and Mindfulness-Based Cognitive Therapy (MBCT) teach clients to observe difficult thoughts and emotions without becoming fused with them. ACT interventions for depression focus on increasing psychological flexibility rather than eliminating depressive thoughts. Clients learn to notice them with curiosity, defuse from their literal content, and redirect attention toward values-based action. MBCT is particularly effective for recurrent depression, with research showing it can reduce relapse rates by approximately 50% in clients with three or more prior episodes.
Mindfulness-Based Cognitive Therapy (MBCT) for Depression
Mindfulness-Based Cognitive Therapy (MBCT) combines cognitive therapy principles with mindfulness practices to help clients disengage from rumination and recognize early warning signs of relapse.
Rather than trying to eliminate depressive thoughts, MBCT teaches clients to observe them without judgment and return attention to the present moment. Techniques such as the three-minute breathing space, body scans, and mindful awareness exercises can reduce reactivity and improve emotional regulation.
MBCT is particularly effective for clients with recurrent depression, with research showing it can significantly reduce relapse risk when practiced consistently.
Journaling and Emotional Processing
Structured journaling allows clients to identify mood triggers, log their emotional responses, and track recurring thought patterns. Prompts such as “What drained my energy today and what gave me even a small sense of accomplishment?” help clients build insight and begin to recognize the connection between thoughts, behaviors, and mood states.
Behavioral Interventions for Depression: Activation, IPT, and Skills-Based Techniques
Behavioral interventions reduce depression by helping clients re-engage with meaningful activities, rebuild social connections, and interrupt the withdrawal-inactivity cycle that maintains depressive symptoms. These action-oriented depression treatment techniques are especially effective for clients whose primary symptoms include anhedonia, low motivation, social isolation, and loss of routine.
Helps clients re-engage with meaningful activities to interrupt the withdrawal-inactivity cycle that maintains depression.
Best for: Anhedonia, low motivation, social withdrawal, and loss of routine
Uses planned activities, graded task assignment, and pleasure/mastery tracking to rebuild momentum even when motivation is low.
Best for: Clients who feel stuck, inactive, or disconnected from rewarding daily experiences
Focuses on the connection between mood and relationships by addressing grief, role transitions, interpersonal disputes, and social isolation.
Best for: Depression linked to conflict, loss, loneliness, or major life changes
Group-based interventions can normalize depression, reduce isolation, and help clients practice coping strategies in a supportive social context.
Best for: Clients with significant social withdrawal who benefit from peer support and shared learning
Builds practical supports such as coping cards, activity menus, structured worksheets, and problem-solving tools clients can use between sessions.
Best for: Strengthening self-efficacy, daily functioning, and skill generalization outside therapy
Integrates mindfulness, emotion regulation, distress tolerance, and interpersonal effectiveness skills into depression treatment when emotional dysregulation is prominent.
Best for: Emotional dysregulation, chronic suicidal ideation, or co-occurring personality-related challenges
Behavioral Activation
Behavioral activation (BA) is one of the most effective standalone interventions for depression. BA operates on the principle that depression leads to withdrawal, which reduces exposure to positive reinforcement, which deepens depression. By systematically scheduling activities — starting with small, manageable tasks and building toward more meaningful engagement — clients begin to break this cycle. Activity scheduling, pleasure and mastery tracking, and graded task assignment are core BA tools.
Behavioral Activation Plan Example
A client with depression who has stopped exercising, socializing, and maintaining household routines might start by scheduling one 10-minute walk per day and one brief phone call to a friend per week. Each activity is rated for pleasure and mastery, providing concrete evidence that engagement — even when motivation is low — can improve mood. Over time, the schedule expands as the client rebuilds their behavioral repertoire.
Interpersonal Therapy (IPT)
IPT is a time-limited, evidence-based treatment that focuses on the connection between mood and interpersonal functioning. IPT addresses four key problem areas: grief and loss, role transitions, interpersonal disputes, and interpersonal deficits (social isolation). By improving communication patterns, processing relational losses, and building social support, IPT helps clients resolve the interpersonal issues that trigger and maintain depression.
Group Therapy and Peer Support
Group-based interventions can normalize clients’ experiences and reduce the isolation that often accompanies depression. Group CBT programs, behavioral activation groups, and support groups help clients learn coping strategies from peers, practice social engagement in a structured setting, and receive validation. These formats are particularly effective for clients whose depression includes significant social withdrawal
Skills Training and Coping Toolkits
Helping clients build a personalized set of coping tools enhances self-efficacy and supports skill generalization outside the therapy room. These may include mood-based coping cards, activity menus for low-energy days, structured worksheets for challenging negative thoughts, and problem-solving frameworks for managing daily stressors. Clinicians might also teach practical skills such as assertiveness training, time management, or communication skills that address functional deficits contributing to depression.
Dialectical Behavior Therapy (DBT) Skills for Depression
DBT interventions for depression draw from dialectical behavior therapy’s four core skill modules: mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness. While DBT was originally developed for borderline personality disorder, its structured skills-based approach has shown efficacy for depression — particularly in clients with emotional dysregulation, chronic suicidal ideation, or co-occurring personality pathology. Clinicians can integrate individual DBT skills into a broader depression treatment plan without implementing the full DBT protocol, using techniques such as opposite action (behaving contrary to the depressive urge to withdraw), emotional regulation worksheets, and interpersonal effectiveness scripts to improve communication and reduce isolation.
Somatic Interventions for Depression: Mindfulness, Movement, and Body-Based Techniques
Somatic techniques target the physiological and body-based components of depression, including fatigue, psychomotor slowing, sleep disruption, and emotional numbing. Because depression often involves both heightened stress responses and states of shutdown or disconnection, these approaches help clients reconnect with their bodies and build regulation capacity.
These somatic techniques can be integrated directly into sessions or assigned as between-session practices to support regulation, awareness, and behavioral activation.
Help clients disengage from rumination and observe depressive thoughts without becoming fused with them, supporting relapse prevention.
Best for: Rumination, recurrent depression, and relapse prevention
Support nervous system regulation through diaphragmatic breathing and grounding, helping reduce physiological shutdown or dysregulation.
Best for: Emotional dysregulation, comorbid anxiety, and somatic symptoms of depression
Helps clients identify and release physical tension while improving awareness of how body states influence mood.
Best for: Physical tension, sleep disruption, and clients with strong mind-body symptom patterns
Gentle movement such as walking, stretching, or yoga can improve energy, reduce fatigue, and reconnect clients with their bodies.
Best for: Low energy, fatigue, behavioral withdrawal, and psychomotor slowing
Provide nonverbal pathways for processing depressive experiences through art, music, or movement, especially when emotions are difficult to articulate.
Best for: Emotional numbness, difficulty verbalizing feelings, and clients resistant to traditional talk therapy
Mindfulness and MBCT for Depression
Mindfulness practices help clients shift out of rumination by anchoring attention in the present moment. Rather than trying to eliminate depressive thoughts, clients learn to observe them without becoming fused with them.
Mindfulness-Based Cognitive Therapy (MBCT) is particularly effective for recurrent depression, helping clients recognize early warning signs and interrupt relapse cycles before symptoms escalate. Techniques such as body scans, grounding exercises, and brief mindfulness practices can reduce reactivity and improve emotional regulation.
“Breathe in for four counts… hold… and breathe out slowly. Notice where you feel heaviness in your body right now. You don’t need to change it — just notice it. Let your thoughts come and go without holding on to any one of them.”
Breathing and Nervous System Regulation
Depression is often associated with dysregulation of the autonomic nervous system, including both hyperarousal and hypoarousal states.
Breathing techniques such as diaphragmatic breathing can support parasympathetic activation, while grounding strategies help stabilize attention and reduce dissociation or emotional blunting. These techniques are especially useful for clients with comorbid anxiety or trauma histories.
Progressive Muscle Relaxation and Body Awareness
Progressive muscle relaxation (PMR) helps clients identify and release chronic tension while increasing awareness of how physical states influence mood.
By systematically tensing and relaxing muscle groups, clients develop a greater connection between body sensations and emotional experience, which can improve regulation and reduce somatic distress.
Movement-Based Interventions
Movement-based approaches such as walking, stretching, yoga, or light exercise can play a critical role in depression treatment.
Even small amounts of physical activity can increase energy, improve mood, and counteract the inertia and fatigue that often accompany depression. Movement also helps re-engage clients with their environment and provides a behavioral pathway out of withdrawal.
Creative and Expressive Therapies
Creative and expressive interventions offer nonverbal pathways for processing depression, particularly when clients struggle to articulate their internal experience.
Art therapy, music, and movement-based expression can support emotional processing, insight, and regulation. These approaches are especially helpful for clients who feel emotionally numb, disconnected, or resistant to traditional talk therapy.
Psychoeducational Interventions for Depression: Education and Symptom Tracking
Psychoeducational interventions help clients understand how depression works and provide concrete tools for recognizing patterns, tracking symptoms, and applying coping strategies between sessions. These approaches are especially valuable early in treatment, when clients may feel confused, discouraged, or self-critical about their symptoms.
By increasing insight and reducing self-blame, psychoeducation creates a foundation for more targeted therapeutic work.
Help clients understand how thoughts, behaviors, and mood interact to maintain depression, reducing self-blame and increasing insight.
Best for: Early treatment, low insight, and clients experiencing self-blame or confusion about their symptoms
Use logs or structured tools to track mood, daily activities, and patterns, helping clients identify what improves or worsens symptoms.
Best for: Identifying patterns, increasing awareness, and supporting behavioral activation
Reinforce progress with between-session activities such as thought records, behavioral activation logs, and structured reflection prompts.
Best for: Skill reinforcement, increasing engagement, and improving follow-through between sessions
Teach caregivers to support activity engagement, reinforce coping skills, and avoid patterns that unintentionally maintain withdrawal or helplessness.
Best for: Children, adolescents, and clients whose environment influences mood and functioning
Incorporate mood-tracking apps, guided exercises, or digital tools that support structure, consistency, and skill reinforcement between sessions.
Best for: Between-session support, structure building, and clients who benefit from guided or tech-assisted tools
Depression Cycle Education
Helping clients understand the depression cycle — how thoughts, behaviors, and mood reinforce one another — can be a powerful first step in treatment.
For example, low mood can lead to withdrawal, which reduces exposure to positive reinforcement, which in turn deepens depression. When clients see this pattern clearly, they are more likely to engage in interventions like behavioral activation and cognitive restructuring.
Mood and Activity Tracking
Tracking mood alongside daily activities helps clients identify patterns that may not be obvious in session.
Clients may begin to notice that even small actions — such as leaving the house, completing a task, or connecting with someone — are associated with slight improvements in mood. This insight reinforces the connection between behavior and emotional state, supporting treatment progress.
Therapeutic Homework and Between-Session Practice
Homework assignments extend therapeutic work beyond the session and support skill development over time.
These may include thought records, behavioral activation logs, journaling prompts, or structured reflection exercises. Consistent between-session practice helps clients build confidence, reinforce learning, and apply new strategies in real-world contexts.
Caregiver and Family Education
For children, adolescents, and some adult clients, involving caregivers or family members can significantly improve outcomes.
Educating caregivers about depression helps them understand that symptoms are not due to laziness or lack of effort. It also equips them to support activity engagement, reinforce coping skills, and avoid patterns that may unintentionally maintain withdrawal or helplessness.
Digital Tools and Guided Supports
Digital tools can provide additional structure and support between sessions. Mood-tracking apps, guided exercises, and digital worksheets can help clients stay engaged with treatment and maintain consistency.
For some clients, these tools offer a more accessible or less overwhelming way to practice skills, especially when motivation is low.
Lifestyle Interventions for Depression: Exercise, Sleep, and Daily Habits
Lifestyle-focused interventions address the foundational habits that influence mood, energy, and emotional resilience. These nonpharmacological interventions for depression — including healthy sleep, nutrition, physical activity, and routine stabilization — can significantly enhance treatment outcomes and support long-term recovery.
Exercise, Diet, and Sleep Hygiene
Lifestyle factors strongly influence depressive symptoms. Regular physical activity — even moderate exercise like 30-minute walks — has been shown to produce antidepressant effects comparable to medication for mild-to-moderate depression. A balanced diet with adequate omega-3 fatty acids, B vitamins, and stable blood sugar supports mood regulation, while consistent sleep patterns improve cognitive functioning and emotional regulation. Clinicians can help clients identify specific, achievable changes and build these into treatment plans as measurable goals.
Summary of Therapeutic Interventions for Depression by Category
Use this quick-reference table to identify the most appropriate intervention category based on your client’s presentation.
| Category | Examples of Interventions |
|---|---|
| Cognitive | CBT, cognitive restructuring, thought challenging, behavioral experiments, journaling, ACT, MBCT |
| Behavioral | Behavioral activation, activity scheduling, IPT, group therapy, skills training, DBT skills, graded task assignment |
| Somatic | Mindfulness, MBCT, breathing exercises, grounding, progressive muscle relaxation, movement-based interventions, creative therapies |
| Psychoeducational | Depression cycle education, mood tracking, activity tracking, therapeutic homework, caregiver education, digital support tools |
| Lifestyle | Physical activity, sleep hygiene, nutrition support, routine stabilization, substance use reduction, daily habit changes |
Using Depression Assessment Tools to Measure Treatment Outcomes
Standardized depression assessment tools can help clinicians measure symptom severity, track treatment outcomes, and support documentation. Common assessments include the Patient Health Questionnaire-9 (PHQ-9), Beck Depression Inventory-II (BDI-II), Hamilton Depression Rating Scale (HAM-D), Columbia Suicide Severity Rating Scale (C-SSRS), and the Quick Inventory of Depressive Symptomatology (QIDS). Routine measurement supports clinical decision-making by providing objective data on whether interventions are producing meaningful change.
Related Resources for Treating Depression
Explore additional guides on depression assessment, treatment planning, and evidence-based interventions to support your clinical work.
Frequently Asked Questions About Interventions for Depression
In practice, clinicians often combine approaches based on the client’s presentation. For a structured way to align interventions with treatment planning, see our guide to treatment goals for depression .
Clinicians should also consider preferences, comorbidities, and treatment history. Using validated tools like depression assessment tools can help guide decision-making.
For clinicians integrating cognitive and values-based approaches, see our guide to ACT for depression .
These approaches help clients leave session with a clear next step. To structure these interventions within a broader framework, see our guide to creating a depression treatment plan .
Population-specific considerations may also apply. Learn more in our guide to depression in older adults .
Using consistent measures supports better clinical decision-making and improves outcomes through measurement-based care.
How ICANotes Supports Depression Intervention Documentation
High-quality documentation is essential when delivering structured interventions for depressive disorders. ICANotes, an EHR designed specifically for behavioral health clinicians, offers:
- Built-in depression assessments like the PHQ-9
- Templates for CBT, behavioral activation, IPT, and psychoeducation
- Progress note and treatment plan templates tailored to behavioral interventions
Effective depression treatment requires a thoughtful combination of clinical skill and supportive tools. Whether you’re using cognitive restructuring, behavioral activation, or mindfulness practices, your interventions are more powerful when backed by strong documentation and organization.
Get started with a free trial of ICANotes today — no credit card required — and see how a behavioral health EHR built for your needs can elevate your work with clients experiencing depression.
From Intervention Selection to Audit-Ready Notes — In Minutes
Choosing the right intervention is only the first step. Documenting interventions for depression clearly is what supports reimbursement, compliance, and continuity of care.
ICANotes helps you translate CBT, behavioral activation, ACT, MBCT, and other evidence-based interventions into structured, defensible documentation in minutes.
- Pre-built templates for depression interventions
- Structured notes that support medical necessity
- Integrated outcome measures like PHQ-9
- Faster documentation with clinically relevant language built in
Start your free 30-day trial — no credit card required.
Takes less than 60 seconds to get started
Related Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







