Blog > Documentation > Initial Psychiatric Evaluation Template [Free PDF + Example]
The Essential Components of an Initial Psychiatric Evaluation Template
A structured initial psychiatric evaluation template is essential for accurate diagnosis, treatment planning, and audit-ready documentation. In this guide, we break down the key components of a comprehensive psychiatric evaluation, map them to APA-recommended domains, and provide a detailed psychiatric evaluation example to help psychiatrists and PMHNPs document efficiently. You’ll also see how ICANotes streamlines the process with structured templates, built-in clinical content, and seamless PDMP integration.

Last Updated: April 9, 2026


What You'll Learn
- How to structure a complete initial psychiatric evaluation using APA-recommended domains
- The 13 essential components every psychiatric evaluation template should include
- What a full psychiatric evaluation looks like in practice with a step-by-step sample assessment walkthrough
- The difference between a psychiatric evaluation form vs. template — and how to use both efficiently
- Common documentation mistakes that can impact billing, compliance, and audit risk — and how to avoid them
- How to ensure your documentation supports CPT codes 90791 and 90792
- What payers look for when evaluating medical necessity and level of care justification
- How ICANotes helps clinicians complete psychiatric evaluations faster while improving documentation quality
Contents
- Recommended Aspects of the Initial Psychiatric Evaluation
- Key Components of a Comprehensive Psychiatric Evaluation Template
- Psychiatric Evaluation Example: Sample Initial Assessment
- Psychiatric Evaluation Form vs. Template: What's the Difference?
- Why a Comprehensive Psychiatric Evaluation Template Matters
- How ICANotes Makes Psychiatric Evaluations More Efficient
- FAQ: Initial Psychiatric Evaluations
Accurate and thorough documentation is foundational to quality psychiatric care. For psychiatrists and psychiatric nurse practitioners, the initial psychiatric evaluation is more than just a clinical requirement — it sets the stage for diagnosis, treatment planning, and ongoing care. Yet, with increasing time constraints and administrative burdens, it's easy to miss key details or fall into inefficient workflows.
Whether you're refining your current documentation process or adopting a new EHR, having a structured psychiatric documentation workflow and initial psychiatric evaluation template can save time, improve compliance, and lead to better outcomes for both patients and providers.
In this post, we break down every component of a comprehensive psychiatric evaluation template, map them to the APA's recommended evaluation domains, and include a sample psychiatric evaluation walkthrough so you can see what a complete initial assessment looks like in practice. Plus, learn how ICANotes streamlines the entire process — from structured templates to seamless PDMP integration.
What Is an Initial Psychiatric Evaluation?
An initial psychiatric evaluation is a comprehensive assessment of a patient’s mental, emotional, and behavioral health. It typically takes place during a first appointment and includes a detailed history, clinical observations, and formulation of a diagnostic impression and treatment plan.
This evaluation is often billed under CPT code 90791 (psychiatric diagnostic evaluation) or 90792 (with medical services). Understanding how to properly document for CPT codes ensures accurate reimbursement and reduces audit risk. The resulting documentation becomes the foundation for future encounters — informing medication decisions, therapy recommendations, and coordination with other healthcare providers. A thorough initial assessment also supports medical necessity, justifies the level of care, and reduces liability risk.
Recommended Aspects of the Initial Psychiatric Evaluation (APA Practice Guidelines)
The American Psychiatric Association's Practice Guidelines for the Psychiatric Evaluation of Adults outlines a set of recommended aspects that should be addressed in every initial evaluation. These guidelines (commonly referenced as "Table 2" in the APA text) provide the clinical gold standard for what a comprehensive psychiatric assessment should include.
The table below maps the APA's recommended evaluation domains to the corresponding template components covered in this post:
| APA Recommended Evaluation Domain | Template Section | Key Elements |
|---|---|---|
| Reason for evaluation | Chief Complaint / Reason for Referral | Presenting problem in patient's own words; referral context |
| History of present illness | HPI (Section 3) | Onset, duration, severity, triggers, functional impact, prior interventions |
| Past psychiatric history | Past Psychiatric History (Section 4) | Prior diagnoses, hospitalizations, medication trials, psychotherapy history |
| Substance use history | Substance Use History (Section 6) | Alcohol, illicit drugs, prescription misuse; withdrawal or overdose history |
| Medical history | Medical History (Section 5) | Chronic conditions, surgeries, current medications, allergies, neurological concerns |
| Family history | Family History (Section 7) | Psychiatric and medical diagnoses in family; substance use, suicide, violence |
| Developmental, social, and occupational history | Social and Developmental History (Section 8) | Childhood and upbringing; education; employment; housing; legal issues; trauma; support systems |
| Review of systems | Medical History / HPI | Relevant somatic complaints and systems review |
| Mental status examination | MSE (Section 9) | Appearance, behavior, mood, affect, speech, thought process, cognition, insight, judgment |
| Physical examination (when indicated) | Medical History (Section 5) | Relevant physical findings, vitals, neurological exam as applicable |
| Functional assessment | HPI (Section 3) / Treatment Plan (Section 12) | Impact on work, relationships, ADLs; level-of-care justification |
| Risk assessment | MSE (Section 9) / Treatment Plan (Section 12) | Suicidal/homicidal ideation; violence risk; safety planning |
| Diagnostic formulation | Diagnosis (Section 10) / Clinical Formulation (Section 11) | DSM-5 diagnoses, differentials, biopsychosocial formulation |
| Treatment planning | Treatment Plan (Section 12) | Medications, therapy referrals, lab workup, safety plan, follow-up |
By structuring your initial psychiatric evaluation template around these APA-recommended domains, you ensure both clinical completeness and alignment with professional standards of care. Clinicians can also use structured tools and templates to improve consistency and audit readiness, as outlined in our guide to behavioral health chart audits. Each of the sections below expands on these components in detail.
Key Components of a Comprehensive Psychiatric Evaluation Template
The ideal psychiatric assessment template balances structure with clinical flexibility. Here are the essential components that should be included:
1. Identifying Information / Demographics
- Patient name, DOB, MRN
- Date of evaluation
- Provider name and credentials
2. Reason for Referral / Chief Complaint
- Patient’s presenting problem in their own words
- Context of referral (self, primary care, emergency, etc.)
A clear chief complaint anchors the evaluation and helps structure the HPI. Document the exact reason for the visit — whether it's a new symptom, a medication concern, a crisis, or a transfer of care.
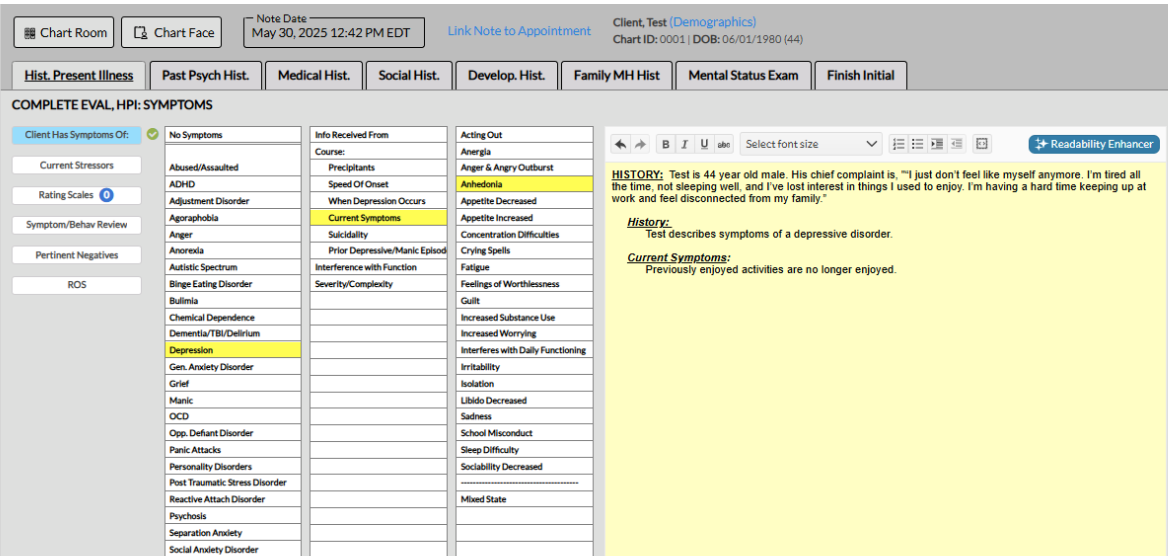
This is the HPI section of the comprehensive psychiatric evaluation template built into ICANotes. A fully narrative psychiatric assessment report is generated by clicking the relevant menu options. The menu content is fully customizable. With the mobile-friendly psychiatric intake module, most of the history is pre-populated by the patient, saving the clinician valuable documentation time.
3. History of Present Illness (HPI)
The psychiatric HPI is the narrative core of the initial evaluation and often the most time-consuming section to document. A thorough psychiatric HPI should address key elements that support golden thread documentation, including :
- Onset and timeline: When symptoms began and how they have progressed
- Symptom characterization: Nature, severity, frequency, and duration of current symptoms
- Triggers and context: Precipitating events, psychosocial stressors, or life changes
- Exacerbating and relieving factors: What makes symptoms better or worse
- Functional impact: Effects on work, relationships, self-care, and daily activities
- Prior treatment and response: Medications tried (with doses and outcomes), psychotherapy history, hospitalizations
- Current safety concerns: Suicidal ideation, self-harm, homicidal ideation (expanded in MSE)
- Rating scale results: Scores from validated instruments (e.g., PHQ-9, GAD-7, AUDIT-C, Columbia Suicide Severity Rating Scale)
Psychiatric HPI Example
Why This Works (Click to Expand)
- Clear chief complaint in patient’s own words: Establishes clinical relevance and aligns with payer expectations.
- Time-bound symptom history: Includes onset, duration, and progression, which supports diagnostic accuracy and medical necessity.
- Symptom specificity: Identifies cognitive, emotional, and somatic features of anxiety, strengthening diagnostic clarity.
- Objective measures included: PHQ-9 and GAD-7 scores provide quantifiable severity indicators for tracking outcomes.
- Prior treatment history documented: Medication trial and response support clinical decision-making and justify next steps.
- Risk assessment addressed: Explicit denial of suicidal ideation is critical for safety documentation.
- Functional impairment clearly stated: Demonstrates impact on work and social functioning—key for medical necessity and reimbursement.
4. Past Psychiatric History
- Previous diagnoses
- Hospitalizations (including dates, duration, and reason)
- Medication trials and adherence history
- Prior psychotherapy or substance use treatment
- Prior ECT, TMS, or other somatic treatments
- History of involuntary holds or commitments
5. Medical History
- Chronic conditions, surgeries, current medications
- Neurological concerns (seizures, head injuries, cognitive changes)
- Allergies and adverse drug reactions
- Relevant lab results or imaging
- Current primary care provider
6. Substance Use History
- Alcohol, illicit drugs, prescription misuse
- Frequency, duration, and consequences
- History of withdrawal or overdose
- Previous treatment (detox, rehab, MAT)
- Current sobriety status and recovery supports
- PDMP check results (when applicable)
7. Family History (Psychiatric and Medical)
- Mental health diagnoses in first-degree relatives
- Family medical history
- Substance use, suicide attempts or completions, violence, or chronic illness in the family
- Family response to mental health treatment (can suggest pharmacogenomic patterns)
8. Social and Developmental History
The social and developmental history captures the broader context of the patient's life and is often where clinicians identify trauma exposure, adverse childhood experiences, and psychosocial stressors that directly inform the diagnostic formulation and treatment approach.
- Childhood and upbringing (including adverse childhood experiences)
- Education and employment history
- Housing and financial stability
- Relationship and marital status
- Legal history (current or past involvement with the justice system)
- Trauma history (physical, sexual, emotional abuse; neglect; combat exposure)
- Cultural, spiritual, and religious factors
- Current support systems
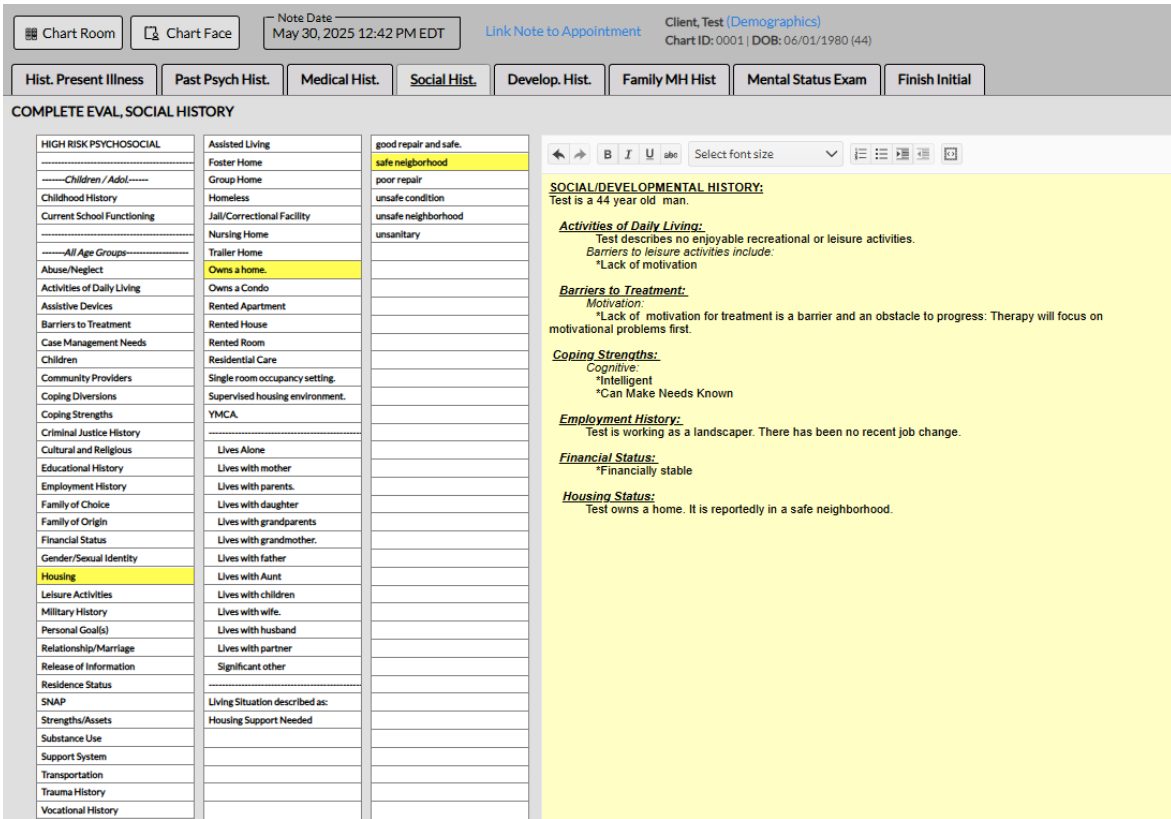
This is the Social History section of the inital psychiatric evaluation template in ICANotes. Comprehensive multi-level menus organized in a clinically logical way allow the psychiatrist or nurse practitioner to quickly produce a detailed narrative.
9. Mental Status Examination (MSE)
The MSE is the psychiatric equivalent of the physical exam. It documents the clinician's objective observations at the time of the evaluation:
- Appearance: Grooming, hygiene, attire, apparent age vs. stated age
- Behavior and psychomotor activity: Eye contact, cooperation, agitation, retardation
- Mood: Patient's subjective report (in their own words)
- Affect: Clinician-observed emotional expression (range, congruence, appropriateness)
- Speech: Rate, rhythm, volume, spontaneity
- Thought process: Linear, tangential, circumstantial, loose associations, flight of ideas
- Thought content: Delusions, obsessions, preoccupations, phobias
- Perceptual disturbances: Hallucinations (auditory, visual, tactile), illusions
- Cognition: Orientation, attention, concentration, memory
- Insight and judgment: Awareness of illness, capacity for decision-making
- Suicidal and homicidal ideation: Current ideation, plan, intent, means, protective factors
The MSE is also a critical component of defensible documentation during audits and utilization reviews — learn more about how to structure notes in our guide to passing a mental health utilization review.
Sample MSE Documentation
Why This Works (Click to Expand)
- Clear appearance and behavior: Documents grooming, cooperation, and psychomotor activity, which are foundational to the MSE.
- Mood and affect are distinguished: Subjective mood is quoted, while affect is objectively described and assessed for congruence.
- Speech and thought process are specified: Captures rate, tone, and organization of thinking—key for diagnostic clarity.
- Thought content is clinically relevant: Identifies preoccupations and rules out psychosis, obsessions, and other abnormalities.
- Perceptual disturbances assessed: Explicit denial of hallucinations strengthens documentation completeness.
- Cognition is objectively evaluated: Orientation and attention testing (e.g., serial 7s) provide measurable findings.
- Insight and judgment are supported: Goes beyond labeling by including behavioral evidence.
- Organized and narrative-driven: Flows logically while still capturing all required MSE domains—ideal for audits and clinical communication.
A structured MSE template ensures each domain is addressed consistently, even under time pressure. ICANotes' click-to-insert MSE module organizes all domains in a clinically logical sequence and generates a complete narrative from menu selections.
10. Risk Assessment
A structured risk assessment should be documented as part of every initial psychiatric evaluation, even when the patient denies active suicidal ideation. Key elements include:
- Suicidal ideation assessment: Frequency, duration, plan, intent, means, prior attempts
- Homicidal ideation assessment: Identified targets, plan, access to weapons
- Violence risk factors: History of aggression, command hallucinations, active substance use
- Protective factors: Social support, reasons for living, treatment engagement, future orientation
- Risk level determination: Low, moderate, or high — with clinical justification
- Safety plan: Coping strategies, emergency contacts, means restriction, crisis resources
Templates that include a structured risk assessment section help ensure this critical component is never overlooked.
Risk Assessment Documentation Examples
Why This Works (Click to Expand)
- Explicit assessment of ideation, intent, and plan: Clearly documents the core elements required for suicide risk evaluation.
- Risk and protective factors are both included: Demonstrates balanced clinical reasoning and supports risk stratification.
- Historical risk is documented: Prior attempts and family history significantly influence current risk level.
- Means access is addressed: Firearm and medication access documentation is critical for liability and safety planning.
- Substance use is quantified: Objective measures (e.g., AUDIT-C) strengthen clinical credibility.
- Clear risk level designation: “LOW” vs “MODERATE” ties clinical findings to decision-making.
- Action steps are documented: Safety planning, follow-up, and crisis resources demonstrate appropriate intervention.
- Patient understanding is confirmed: Documentation of agreement and comprehension strengthens defensibility.
Get the Initial Psychiatric Evaluation Checklist
Make sure every initial psychiatric evaluation covers the essential clinical and documentation elements. This free two-page checklist helps psychiatrists and PMHNPs document more thoroughly, support medical necessity, and reduce the risk of missing critical details.
You’ll also get a practical psychiatric HPI documentation guide with prompts and sample language to help you write stronger evaluations faster.
- APA-aligned checklist covering 14 essential evaluation components
- Step-by-step HPI documentation prompts and sample language
- Helpful for HPI, MSE, risk assessment, diagnosis, and treatment planning
- Designed for psychiatrists and psychiatric nurse practitioners
Download the Free Checklist
Enter your information below to get instant access.
11. Diagnosis
- DSM-5 diagnoses (primary and secondary)
- Rule-outs, differential, or provisional diagnoses
- ICD-10 codes for billing
12. Clinical Formulation and Psychiatric Impression
The clinical formulation synthesizes all gathered information into a cohesive narrative that explains the patient's presentation. It should include:
- Summary of key findings from the evaluation
- Biopsychosocial understanding of the case (biological vulnerabilities, psychological factors, social context)
- How the formulation supports the DSM-5 diagnoses
- Level of care justification (e.g., outpatient vs. intensive outpatient vs. inpatient)
- Prognosis considerations
A strong clinical formulation also supports continuity across documentation types, including clinical summaries and progress notes.
Diagnostic Impression Example
Why This Works (Click to Expand)
- Primary diagnosis is clearly supported: The impression ties symptom pattern, duration, and impairment directly to Generalized Anxiety Disorder.
- Differential thinking is documented: The depressive symptoms are acknowledged without overstating certainty, which shows sound clinical judgment.
- Objective data is incorporated: PHQ-9 results strengthen the impression and help justify ongoing assessment.
- Biopsychosocial factors are included: Psychosocial stressors, family history, and treatment history all contribute to a more complete formulation.
- Level of care is justified: Outpatient treatment is supported by social stability, insight, and motivation.
- Prior treatment response informs planning: The SSRI discussion shows how past medication experience shapes next-step recommendations.
- The formulation is clinically useful: It goes beyond naming diagnoses and helps explain why this treatment approach makes sense.
This type of formulation connects the clinical data to the diagnosis, justifies the treatment approach, and demonstrates the medical decision-making that supports billing for complex evaluation codes.
13. Treatment Plan
- Medication recommendations and rationale (including alternatives discussed)
- Therapy referrals or treatment modality (CBT, DBT, EMDR, etc.)
- Lab tests or diagnostic workup (e.g., CBC, CMP, TSH, lipid panel, HbA1c, UDS)
- Safety planning (if applicable)
- Follow-up schedule and next appointment
- Patient education and informed consent documentation
- Coordination with other providers (PCP, therapist, case manager)
14. CPT Codes and Billing
- Service codes appropriate for the visit (e.g., 90791, 90792, 99205)
- Ensure documentation supports medical necessity and complexity level
- Time-based documentation for extended evaluations
- Add-on codes for interactive complexity (90785) when applicable
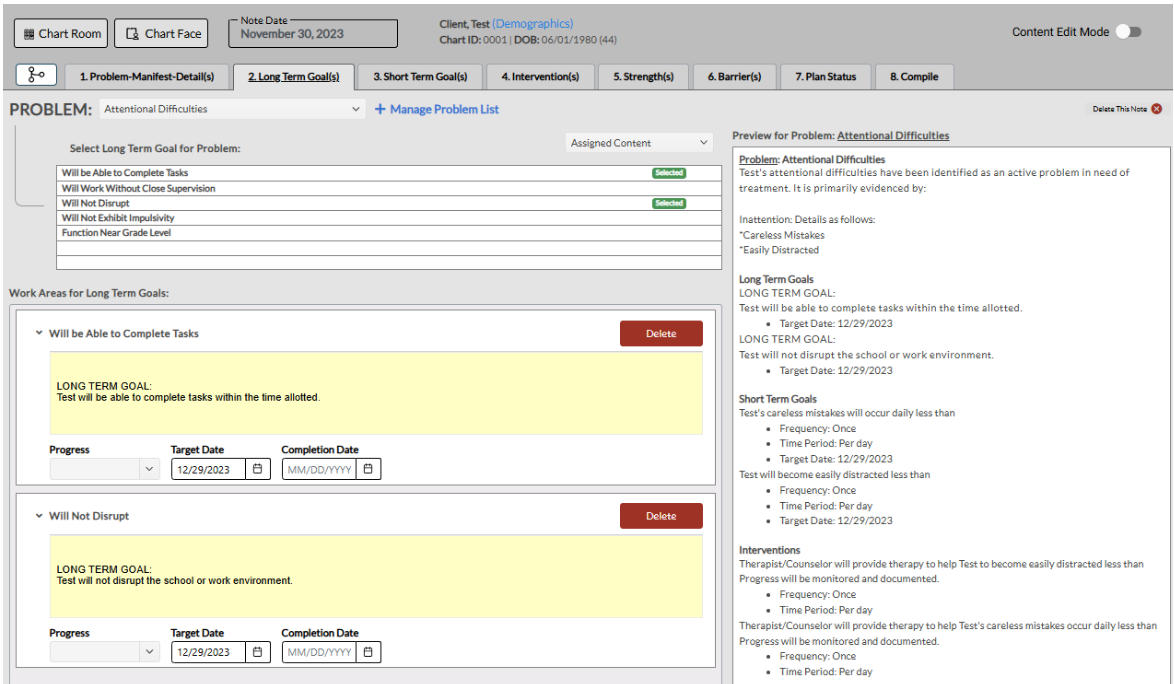
The Treatment Plan module in ICANotes contains robust clinical content for 90 common psychiatric problems and their manifestations. It also includes a wide range of long-term and short-term goals and intervention options.
Psychiatric Evaluation Example: Sample Initial Assessment
Seeing what a completed initial psychiatric evaluation looks like can help clinicians benchmark their own documentation. Below is an abbreviated sample psychiatric evaluation walkthrough illustrating how the template components come together in practice.
Sample Psychiatric Assessment
Patient: J.M., 34/F
Date of Evaluation: [Date]
Provider: [Provider Name], MD / PMHNP-BC
Chief Complaint: “I can’t stop worrying about everything and I’m not sleeping.”
Ms. M is a 34-year-old female presenting for initial psychiatric evaluation with a six-month history of excessive, uncontrollable worry (work, health, family), accompanied by muscle tension, restlessness, difficulty concentrating, irritability, and initial insomnia (sleep onset latency ~90 minutes). Symptoms began after a job transition and have progressively worsened. GAD-7: 16 (severe); PHQ-9: 12 (moderate). Denies SI/HI. Prior trial of sertraline 50mg x 3 months — discontinued d/t GI side effects without adequate anxiolytic response. No prior psychotherapy.
No prior hospitalizations. No history of self-harm or suicide attempts. Diagnosed with “anxiety” by PCP 2 years ago; sertraline was the only medication trial.
Hypothyroidism (levothyroxine 75mcg, stable). NKDA. Last TSH within normal limits 3 months ago.
Social alcohol use (1-2 drinks/week). Denies illicit drug use. Denies tobacco. AUDIT-C: 1 (low risk).
Mother — GAD (treated with buspirone). Maternal grandmother — “depression.” Father — alcohol use disorder (in remission). No family history of suicide.
Lives with partner. Employed as a project manager (recently transitioned from a different company). College-educated. No legal history. Denies trauma history. Reports strong social support through partner and close friends, though has been isolating recently.
Well-groomed, cooperative. Psychomotor: mildly restless (fidgeting with hands). Mood: “anxious and tired.” Affect: anxious, congruent, full range. Speech: normal rate and volume, slightly pressured when discussing work. Thought process: linear, goal-directed with ruminative quality. Thought content: preoccupations with work performance and health; no delusions. Perceptions: no hallucinations. Cognition: alert, oriented x4, attention intact. Insight: good. Judgment: good.
Denies SI/HI. No history of suicide attempts. Protective factors include social support, future orientation, treatment engagement. Risk level: LOW.
- Generalized Anxiety Disorder (F41.1) — primary
- Major Depressive Disorder, Single Episode, Moderate (F32.1) — provisional; will clarify with symptom tracking
Presentation is consistent with GAD with comorbid depressive features in the context of occupational stress and family predisposition to anxiety. Adequate social supports and good insight support outpatient management. Prior SSRI trial was limited by tolerability rather than non-response.
- Start buspirone 5mg BID, titrate to 10mg BID over 2 weeks (rationale: family response to buspirone; avoidance of SSRI class given prior GI side effects)
- Referral to CBT-trained therapist for structured anxiety management
- Labs: TSH recheck, CBC, CMP (baseline for new medication)
- Sleep hygiene psychoeducation provided
- Follow-up in 3 weeks for medication response evaluation
- Safety plan not indicated at this time; patient instructed to contact office or crisis line if symptoms worsen
90792 (psychiatric diagnostic evaluation with medical services)
Want to see a full-length sample evaluation? Download our Initial Psychiatric Evaluation Example PDF created in ICANotes to see how structured templates produce professional, audit-ready documentation.
Psychiatric Evaluation Form vs. Template: What's the Difference?
Clinicians sometimes use the terms "psychiatric evaluation form" and "psychiatric evaluation template" interchangeably, but they serve different functions:
A psychiatric evaluation form is typically a structured intake document — often completed by the patient or front-desk staff — that collects demographic information, presenting concerns, and basic history before the clinical encounter. Forms are often paper-based or available as fillable PDFs and focus on data collection.
A psychiatric evaluation template, on the other hand, is a clinician-facing documentation framework used during or after the evaluation to structure the clinical narrative. Templates guide the provider through each required component (HPI, MSE, risk assessment, diagnostic formulation, treatment plan) and are designed to produce a comprehensive, billable note.
In an efficient practice workflow, the patient completes the intake form before the visit, and the clinician uses the evaluation template during the visit — ideally with intake data pre-populated into the template. ICANotes supports both sides of this workflow with its patient portal intake forms and its menu-driven initial evaluation template that auto-populates from patient-submitted data.
Why a Comprehensive Psychiatric Evaluation Template Matters
A comprehensive, consistent psychiatric assessment template ensures nothing critical is overlooked, while also:
- Supporting billing and documentation compliance — thorough documentation justifies level-of-service codes (90791, 90792, 99205) and reduces audit risk
- Improving interdisciplinary communication — a structured evaluation gives referring providers, therapists, and care coordinators a clear clinical picture
- Enhancing clinical decision-making — systematic data capture ensures diagnostic formulations are grounded in complete information
- Reducing risk of liability — including structured risk assessments and safety plans in every evaluation demonstrates standard-of-care documentation
- Meeting payer requirements — insurance companies increasingly require evidence of medical necessity, functional impairment, and treatment rationale — all of which are embedded in a well-designed template
How ICANotes Helps You Document Initial Psychiatric Evaluations More Efficiently
ICANotes was built specifically for behavioral health professionals — including psychiatrists and psychiatric nurse practitioners. Its menu-driven initial evaluation template is designed to streamline documentation while maintaining the highest clinical standards.
With ICANotes, you can:
- Use click-to-insert narrative content that aligns with clinical phrasing and DSM-5 criteria — no more writing from scratch
- Auto-populate relevant fields from patient-completed intake forms to reduce redundancy and documentation time
- Seamlessly generate PDF reports that are professional, shareable, and audit-ready
- Access built-in MSE tools, structured risk assessments, rating scales (PHQ-9, GAD-7, AUDIT, and more), and diagnostic libraries
- Customize templates for specific populations or specialties (e.g., geriatrics, addiction psychiatry, child and adolescent)
- Automatically determine the highest reimbursable CPT code based on the content of your note
- Order labs directly through integrated lab workflows or document lab needs in your treatment plan
- Justify level of care with structured clinical formulation fields that support medical necessity
- Ease the burden of PDMP checks with seamless integration into state databases during the e-prescribing workflow
The result? You spend less time writing and more time focused on patient care — without sacrificing the depth or quality of your documentation.
Complete Psychiatric Evaluations Faster — Without Missing Critical Details
ICANotes helps psychiatrists and PMHNPs document comprehensive psychiatric evaluations with structured, menu-driven templates for HPI, MSE, risk assessment, diagnostic formulation, and treatment planning.
Create thorough, audit-ready notes that support medical necessity and CPT 90791/90792 requirements — without writing everything from scratch.
Conclusion
A well-structured initial psychiatric evaluation template isn't just a documentation tool — it's a clinical asset. By standardizing the intake process, aligning with APA evaluation guidelines, and ensuring completeness across every domain, you improve outcomes, reduce risk, and support continuity of care.
With ICANotes, you don't have to choose between efficiency and thoroughness. Our intelligent templates help you deliver exceptional documentation — fast.
Related Resources
Looking to strengthen your clinical documentation across the full patient journey? Explore these related guides and examples:
Frequently Asked Questions: Initial Psychiatric Evaluations
Recent Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.






