Blog > Emerging Trends > Resilience Fatigue: Definition, Symptoms & Treatment Guide
Resilience Fatigue in Mental Health: Signs, Assessment, and Treatment Strategies for Clinicians
Resilience fatigue is an emerging clinical concern characterized by the gradual erosion of adaptive coping in individuals who have been “strong for too long.” This comprehensive guide explores the resilience fatigue definition, outlines key resilience fatigue symptoms across emotional, cognitive, behavioral, and physical domains, and provides real-world resilience fatigue examples to support accurate identification in clinical practice. Mental health clinicians will also learn how to assess resilience fatigue using existing tools and implement evidence-based treatment strategies that restore adaptive coping and promote sustainable functioning.

Last Updated: March 26, 2026


What You'll Learn
- A clear, clinically grounded resilience fatigue definition and how it differs from burnout, depression, and compassion fatigue
- The full spectrum of resilience fatigue symptoms, including subtle signs that are often masked in high-functioning clients
- How to identify resilience fatigue in practice using real-world resilience fatigue examples across caregiving, community, and chronic illness contexts
- Practical assessment strategies, including screening tools and targeted clinical interview questions
- Evidence-informed treatment approaches that restore energy, identity balance, and adaptive coping capacity
- How to help clients rebuild sustainable resilience without reinforcing harmful “always strong” narratives
- Key differential diagnosis considerations to improve clinical accuracy and documentation defensibility
Ethical and systemic factors that contribute to resilience fatigue, including cultural expectations and chronic adversity
Contents
- Introduction: When Resilience Becomes the Problem
- Resilience Fatigue Definition: Clarifying the Construct
- Resilience Fatigue Symptoms: A Multidimensional Profile
- Differential Diagnosis: Distinguishing Resilience Fatigue from Related Conditions
- Resilience Fatigue Examples: Clinical Vignettes
- Assessment Frameworks for Clinical Practice
- Treatment Strategies for Resilience Fatigue
- Systemic and Ethical Considerations for Clinicians
- Frequently Asked Questions About Resilience Fatigue
- Conclusion: Toward a More Honest Relationship with Resilience
Introduction: When Resilience Becomes the Problem
The language of resilience dominates modern mental health care. Clients are praised for “bouncing back,” encouraged to develop grit, and celebrated for weathering hardship without complaint. But what happens when the very act of enduring begins to break a person down? This is the clinical territory of resilience fatigue — a condition that is increasingly relevant in therapeutic settings yet remains under-recognized in formal diagnostic frameworks.
Resilience fatigue describes the progressive emotional, cognitive, and physiological depletion that occurs when an individual is required to demonstrate sustained resilience over an extended period without adequate recovery, support, or acknowledgment. Unlike acute stress reactions or single-event trauma responses, resilience fatigue is cumulative. It develops gradually, often beneath the awareness of the person experiencing it, and it mimics other clinical presentations — making accurate identification a challenge for even experienced practitioners.
This pillar post provides clinicians with a thorough, evidence-informed overview of resilience fatigue. It covers the construct’s definition and theoretical roots, outlines its symptom profile, offers assessment frameworks, distinguishes it from related conditions, presents real-world clinical examples, and details treatment strategies that can be integrated into existing therapeutic modalities.
Resilience Fatigue Definition: Clarifying the Construct
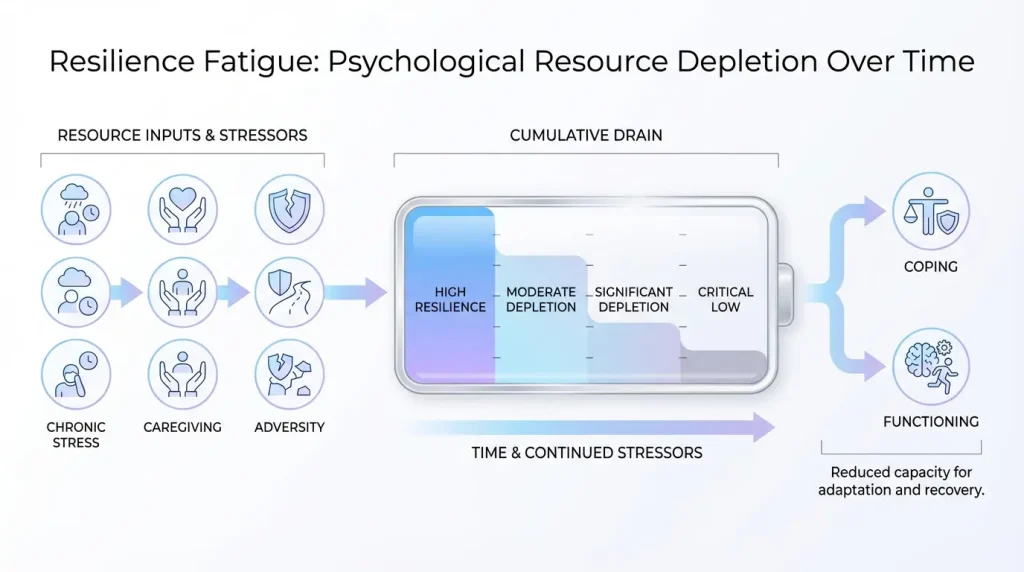
Before examining symptoms and treatment, clinicians need a clear resilience fatigue definition to anchor their conceptual understanding. Resilience fatigue can be defined as the state of diminished psychological, emotional, and physical functioning that results from the prolonged, unrelenting demand to adapt to adversity without sufficient restorative input. It is not a failure of character or an absence of strength. Rather, it is the predictable consequence of a system that has been operating beyond its sustainable capacity for too long.
Several key features distinguish resilience fatigue from general stress or burnout. First, it specifically involves the erosion of previously effective coping strategies. The individual once coped well — and may still appear to cope well externally — but the internal machinery of adaptation has been worn down. Second, there is often a paradoxical quality to the presentation: clients experiencing resilience fatigue may be among the highest-functioning people in their social systems, which is precisely why their distress goes unnoticed. Third, resilience fatigue carries a significant identity component. Many clients have built their self-concept around being “the strong one,” making acknowledgment of depletion feel existentially threatening.
A Note on Terminology
Resilience fatigue is not a formally codified diagnosis in the DSM-5-TR or ICD-11. It is a clinical formulation that synthesizes converging research on resource depletion, allostatic overload, and coping erosion into a practically useful framework. The construct draws on established theories and validated instruments cited throughout this post. Clinicians should understand it as an integrative lens for case conceptualization rather than a standalone diagnostic category.
Theoretical Foundations
The construct of resilience fatigue draws from several converging theoretical streams. Conservation of Resources theory, developed by Stevan Hobfoll, posits that stress arises when individuals face a net loss of valued resources — including energy, time, social support, and self-efficacy — without adequate replenishment. When an individual is continuously called upon to demonstrate resilience, they draw down their resource reserves at a rate that outpaces recovery, eventually reaching a deficit state.
Allostatic load theory offers a complementary physiological lens. Sustained activation of the body’s stress-response systems — originally adaptive — produces cumulative wear and tear on organ systems, immune function, and neurological architecture. The concept of “allostatic overload” maps closely onto resilience fatigue at the biological level: the body’s attempt to maintain stability through constant change eventually degrades the very systems tasked with maintaining equilibrium.
Additionally, the sociocultural dimension cannot be overlooked. Resilience fatigue disproportionately affects individuals in marginalized communities who are expected to endure systemic inequities while simultaneously being praised for their ability to do so. Clinicians must consider the role that cultural narratives of strength — particularly those imposed on communities of color, caregivers, first-generation immigrants, and women — play in perpetuating resilience fatigue.
Turn Insight Into Action With Practical Resilience Fatigue Tools
Understanding resilience fatigue is one thing—documenting and treating it effectively is another. This toolkit gives you structured, clinician-ready tools you can use immediately in session.
Inside the toolkit:
- Screening checklists to identify subtle symptoms
- Assessment worksheets across key domains
- Differential diagnosis support
- Treatment planning tools
- Client-ready psychoeducation handouts
Designed for behavioral health clinicians working with high-functioning clients who may be struggling beneath the surface.

Download Your Free Toolkit
Enter your details below to get instant access.
Resilience Fatigue Symptoms: A Multidimensional Profile
Recognizing resilience fatigue symptoms requires clinicians to look beyond the surface presentation. Because clients experiencing this condition have often developed sophisticated masking behaviors, the symptoms may not align with what clinicians typically expect from someone in distress. The symptom profile spans emotional, cognitive, behavioral, physical, and relational domains.
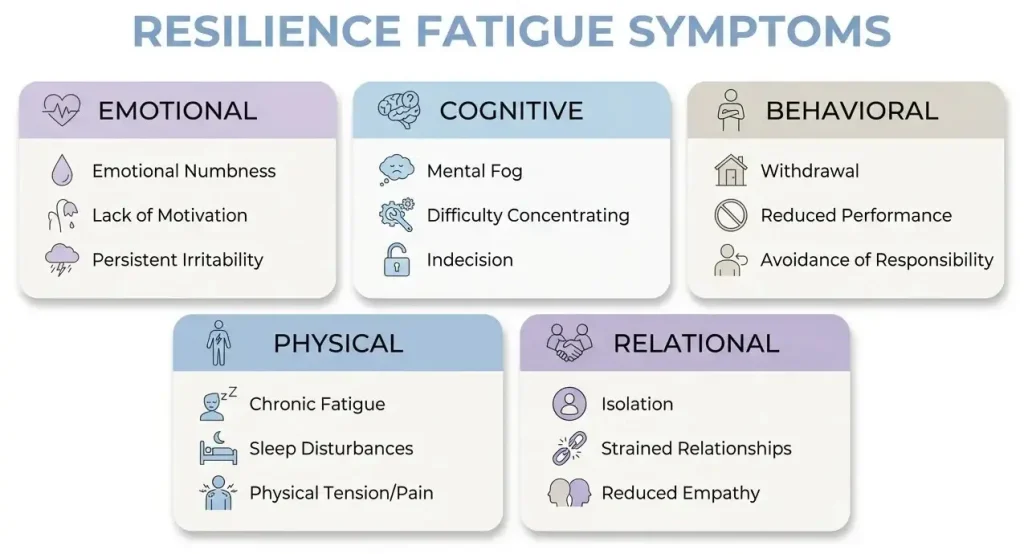
Emotional Symptoms
The emotional landscape of resilience fatigue is marked by a pervasive flatness that clients often describe as “feeling nothing” or “being on autopilot.” This is distinct from clinical depression in that the anhedonia is specifically tied to situations that formerly required, and received, an adaptive emotional response. Clients may report that they used to feel motivated by challenges and now feel only exhaustion at the prospect of another one. There is often a deep-seated resentment toward the circumstances or people that demand continued resilience, coupled with guilt about harboring that resentment. Irritability over minor inconveniences is common, as is a sense of grief for a version of themselves that once felt capable and engaged.
Cognitive Symptoms
Cognitively, resilience fatigue manifests as impaired decision-making, especially around self-care. Clients may demonstrate excellent judgment in professional or caregiving contexts while simultaneously neglecting their own needs in ways that are uncharacteristic. Mental fog, reduced creativity, difficulty concentrating on non-urgent tasks, and a narrowing of perspective — where thinking becomes rigid and binary — are all hallmarks. Clinicians may also notice a shift toward catastrophic thinking or a persistent internal narrative of “What’s the point?” that does not meet the criteria for suicidal ideation but signals motivational collapse.
Behavioral Symptoms
Behaviorally, the most telling symptom is the quiet abandonment of activities that once served restorative functions. Hobbies disappear. Social engagements are canceled or avoided. Self-care routines deteriorate. Meanwhile, obligations are still met — often with mechanical precision — creating the illusion of wellness. Some clients may increase substance use, not in dramatic fashion, but in small, incremental ways: an extra glass of wine, reliance on sleep aids, increased caffeine to compensate for diminished energy. Others may overcommit further, driven by a compulsive need to prove that they are still “fine.”
Physical Symptoms
The body often speaks before the mind gives itself permission. Physical resilience fatigue symptoms include chronic low-grade fatigue that is unresponsive to rest, disrupted sleep architecture (difficulty staying asleep rather than difficulty falling asleep is characteristic), somatic complaints such as tension headaches, gastrointestinal disturbance, and musculoskeletal pain without clear medical etiology. Immune suppression — manifesting as increased frequency of minor illnesses — is consistent with allostatic load theory.
Relational Symptoms
In the relational domain, resilience fatigue often produces a paradox: the individual remains outwardly supportive and attentive to others while becoming internally withdrawn. They may report feeling “invisible” in their own relationships, as if their role has been reduced to a function rather than a person. Intimacy decreases, not through conflict, but through gradual emotional unavailability. Close relationships may strain under the weight of unexpressed needs and unreciprocated care.
Resilience Fatigue Symptom Domains
Emotional
Emotional flatness, autopilot feelings, resentment with guilt, grief for a former sense of self
Cognitive
Impaired self-care decisions, mental fog, rigid thinking, reduced motivation, narrowed perspective
Behavioral
Abandonment of restorative activities, mechanical task completion, avoidance, incremental substance use
Physical
Chronic low-grade fatigue, sleep disruption, somatic complaints, headaches, gastrointestinal issues, immune suppression
Relational
Internal withdrawal behind outward supportiveness, decreased intimacy, feeling invisible, unexpressed needs
Differential Diagnosis: Distinguishing Resilience Fatigue from Related Conditions
One of the most significant clinical challenges is differentiating resilience fatigue from conditions with overlapping features. The following comparisons can assist clinicians in making more precise formulations.

Resilience Fatigue vs. Burnout
While burnout and resilience fatigue share features of exhaustion and diminished engagement, they differ in context and scope. Burnout is predominantly occupational, arising from chronic workplace stress characterized by emotional exhaustion, depersonalization, and reduced professional efficacy. Resilience fatigue is broader in its origin — it can stem from caregiving, systemic adversity, relational burden, community trauma, or any sustained demand for adaptive coping. A person can experience resilience fatigue without being employed, and they can be burned out at work without experiencing the broader identity erosion characteristic of resilience fatigue.
Resilience Fatigue vs. Compassion Fatigue
Compassion fatigue arises specifically from empathic engagement with others’ suffering, most commonly in helping professionals. Resilience fatigue is not limited to empathic strain; it can develop in contexts where the individual is the primary sufferer. A combat veteran navigating repeated deployments, a single parent managing chronic financial insecurity, or a patient managing a long-term illness may all develop resilience fatigue without meaningful exposure to others’ trauma.
Resilience Fatigue vs. Major Depressive Disorder
The symptom overlap between resilience fatigue and depression is substantial, particularly in the areas of anhedonia, fatigue, and cognitive impairment. However, resilience fatigue is context-dependent and functionally specific. The emotional numbness in resilience fatigue is most pronounced in the domains where resilience has been most heavily demanded. A clinician who is exhausted by years of crisis work may still experience genuine pleasure in gardening or music — something less characteristic of a pervasive depressive episode. Additionally, clients with resilience fatigue often retain their capacity for self-reflection and insight, recognizing that something has shifted, whereas depression frequently distorts self-perception more globally.
The table below highlights key differences between resilience fatigue, burnout, and depression to support more accurate clinical differentiation.
Resilience Fatigue Examples: Clinical Vignettes
The following resilience fatigue examples illustrate how the condition presents across different populations and contexts. Each vignette is a composite designed to protect confidentiality while reflecting common clinical patterns.
Case 1: The Long-Distance Caregiver
Mariana, 46, is a project manager and the only family member coordinating care for her mother, who has Alzheimer’s disease, from three states away. For four years, she has managed medical appointments, insurance claims, and rotating home aides while maintaining her own career and raising two adolescent children. Her partner describes her as “a machine”— a characterization Mariana used to take as a compliment but now finds suffocating. She presents to therapy after a panic episode at the grocery store, which she describes as “coming out of nowhere.” On assessment, she cannot identify a single restorative activity she has engaged in within the past year. She denies depression but admits she has stopped feeling “anything at all about anything” and has been drinking wine nightly “just to feel something different.”
Mariana’s case illustrates the hallmark trajectory: sustained demand, competent external performance, internal depletion masked by identity-level investment in being capable, and eventual somatic breakthrough when the system can no longer maintain equilibrium.
Case 2: The Community Leader
Darnell, 34, is a youth pastor in a neighborhood that has experienced three high-profile incidents of gun violence in two years. He has organized vigils, counseled grieving families, mentored at-risk adolescents, and advocated for community resources—all while processing his own grief for a childhood friend killed in one of the incidents. He is referred by his primary care physician after presenting with insomnia, weight loss, and chest tightness that cardiac workup cannot explain. In session, Darnell is articulate and composed. He describes feeling “empty behind the eyes” and notes that his sermons have become “mechanical.” He resists the framing of burnout because, as he explains, “This isn’t about my job. This is about being the person everyone needs me to be.”
Darnell’s example highlights the intersection of resilience fatigue with community trauma and culturally imposed strength narratives. His resistance to the burnout label is clinically significant — it signals that the source of his depletion is rooted in identity and social role, not occupational mechanics.
Case 3: The Chronic Illness Navigator
Priya, 29, was diagnosed with lupus at 21 and has spent the subsequent eight years managing flares, medication side effects, insurance battles, and the social consequences of an invisible illness. She has been described by every provider she has encountered as “remarkably positive” and “inspirational.” She seeks therapy after realizing she has been canceling plans with friends for months and spending weekends in bed not due to a flare but because she “can’t manufacture the energy to perform being okay.” She reports feeling fraudulent, as though her entire identity has become a performance of wellness for other people’s comfort.
Priya’s case demonstrates how external validation of resilience can paradoxically deepen the fatigue. The social reward for “being strong” creates a feedback loop in which the individual feels unable to express vulnerability without forfeiting the identity that others have constructed for them.
Assessment Frameworks for Clinical Practice
There is currently no standalone psychometric instrument validated specifically for resilience fatigue, but clinicians can construct a thorough assessment using a combination of existing tools and targeted clinical inquiry.
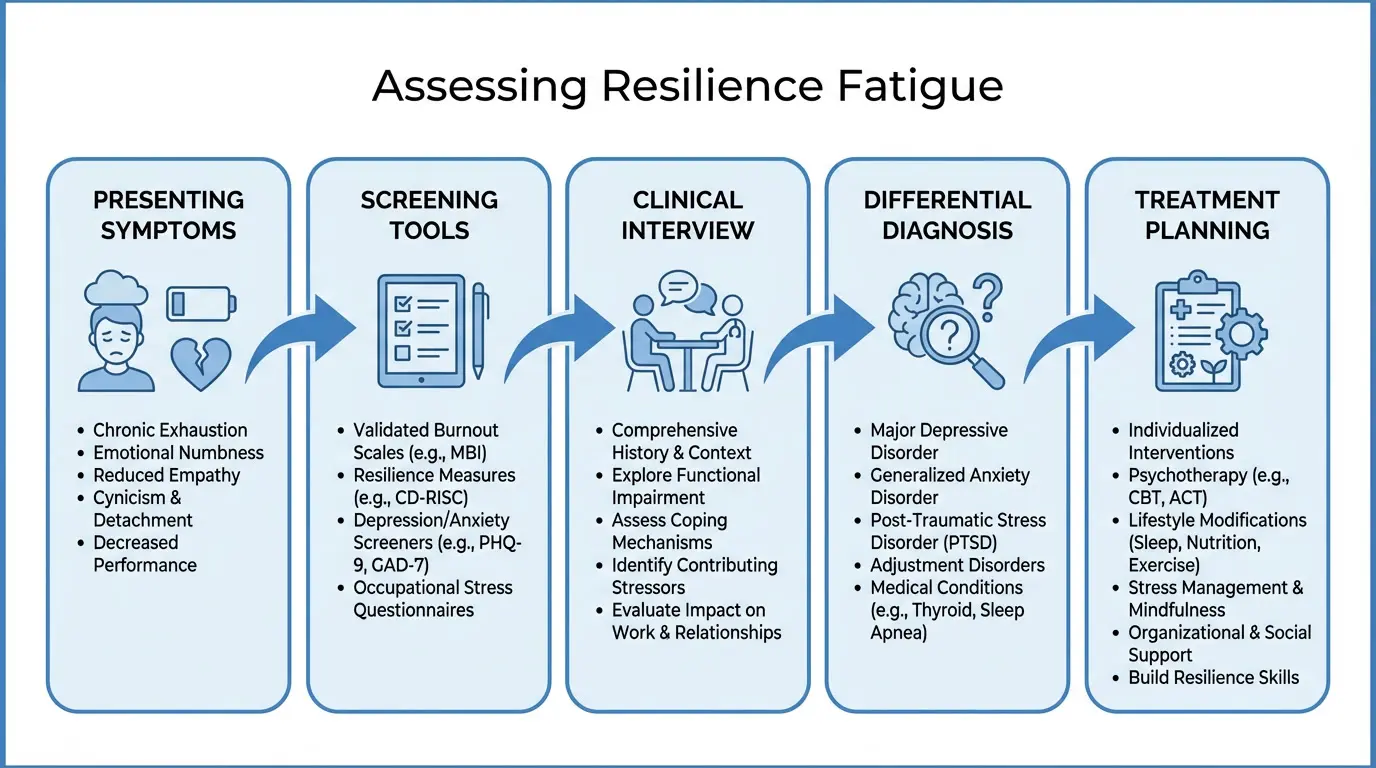
Recommended Screening Instruments
The Connor-Davidson Resilience Scale (CD-RISC) can be used as a baseline measure of resilience capacity, with serial administration revealing trajectory changes over time. A declining CD-RISC score in a previously high-scoring individual is a strong indicator of resilience fatigue. The Professional Quality of Life Scale (ProQOL) is useful for helping professionals, as it separates compassion satisfaction from compassion fatigue and burnout — allowing clinicians to distinguish among overlapping constructs. The Perceived Stress Scale (PSS) provides context for the overall stress burden, and the Maslach Burnout Inventory (MBI) can help rule in or rule out occupational burnout as the primary driver. Somatic symptom screeners such as the PHQ-15 are valuable for capturing the physical manifestations that clients may not spontaneously report.
Clinical Interview Probes
Beyond standardized instruments, the following clinical questions can help uncover resilience fatigue in session. These should be woven naturally into assessment conversations rather than administered as a checklist.
Suggested Assessment Questions for Resilience Fatigue
Use these targeted questions to uncover resilience fatigue in clients who may appear highly functional but are experiencing internal depletion. These prompts are designed to surface identity strain, coping erosion, and unmet needs.
“When people describe you, what word do they use most often? How does that word feel to you now compared to five years ago?”
“What is the last thing you did purely for your own enjoyment, with no obligation attached?”
“If you could put down one responsibility tomorrow with no consequences, what would it be? What prevents you from even imagining that?”
“Do you ever feel like the version of yourself that could handle everything has changed, but you’re still expected to show up as that person?”
“When was the last time someone took care of you—not because you asked, but because they noticed you needed it?”
“How do you feel when someone tells you how strong you are?”
The final question is particularly diagnostic. Clients experiencing resilience fatigue frequently report that praise for their strength now produces anger, sadness, or a sense of being trapped — a marked departure from how such praise was received earlier in their coping trajectory.
Treatment Strategies for Resilience Fatigue
Treatment for resilience fatigue requires a therapeutic stance that honors the client’s history of coping while creating space for a fundamentally different relationship with vulnerability. The following strategies can be integrated across theoretical orientations.
1. Psychoeducation and Naming the Experience
For many clients, simply learning that resilience fatigue is a recognized phenomenon produces profound relief. The act of naming the experience — distinguishing it from personal weakness, laziness, or failure — is itself therapeutic. Clinicians should introduce the concept directly, using language that validates the client’s history of strength while normalizing the cost of sustained adaptation. Framing such as “Your system has been running an extraordinary program for a long time, and what you’re experiencing is the natural result of that demand” can reframe the client’s self-narrative from one of failure to one of recognition.
2. Permission Architecture
Many clients with resilience fatigue lack internal permission to rest, to need, or to not be strong. Treatment should include the deliberate construction of what might be called a “permission architecture”— a set of cognitive, relational, and
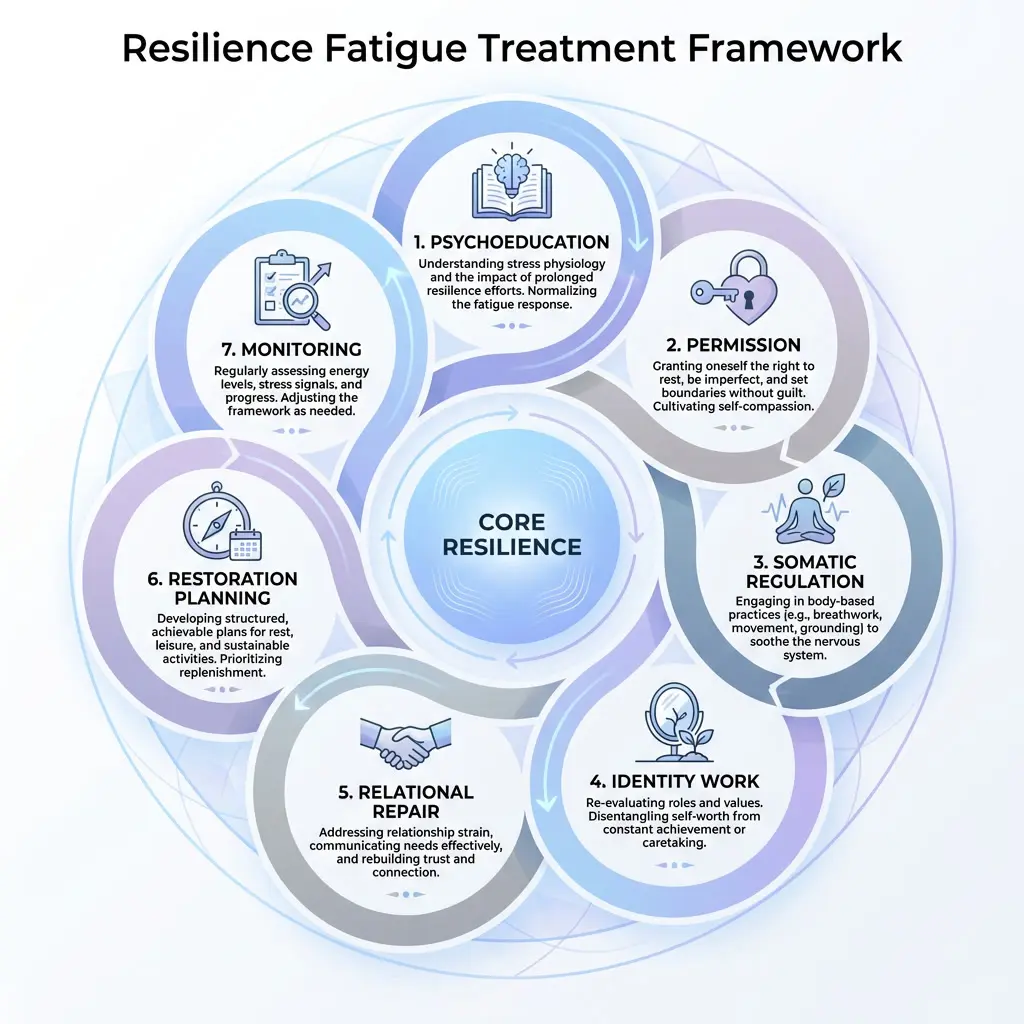
behavioral structures that make it safe for the client to step out of their resilience role. This may involve explicitly granting therapeutic permission (“In this room, you don’t have to be the strong one”), co-constructing a “moral permission” framework that challenges the belief that resting is selfish, and gradually building a practice of delegation and boundary-setting.
3. Somatic and Nervous System Regulation
Given the significant physiological component of resilience fatigue, treatment should incorporate body-based interventions. Polyvagal-informed approaches can help clients recognize the signs of dorsal vagal shutdown that often masquerade as “just being tired.” Breathwork, progressive muscle relaxation, gentle movement practices, and mindfulness-based stress reduction can help down-regulate the hyperactivated stress response. Clinicians should note that some clients will initially resist somatic work because their body has become a site of ignored distress. A gradual, consent-based approach to interoceptive awareness is essential.
4. Identity Work and Values Realignment
Because resilience fatigue is deeply intertwined with identity, treatment must address the client’s relationship to their own narrative of strength. Acceptance and Commitment Therapy (ACT) techniques, particularly values clarification exercises, can help clients distinguish between values they have freely chosen and roles that have been imposed upon them. Narrative therapy approaches can assist in “re-authoring” the client’s story to include chapters of rest and receiving, not only chapters of enduring and giving. The goal is not to dismantle the client’s identity as a resilient person but to expand it — making room for vulnerability, need, and interdependence alongside strength.
5. Relational Restructuring
Resilience fatigue rarely exists in a relational vacuum. Treatment should include exploration of the client’s interpersonal dynamics, with particular attention to patterns of over-functioning, unreciprocated care, and the suppression of needs. Where appropriate, couples or family sessions can address systemic patterns that perpetuate the client’s role as the identified “strong one.” Teaching the client to make direct requests for support — a skill that many high-functioning individuals have never developed because they have never needed to — is a critical component of relational restructuring.
6. Strategic Restoration Planning
Unlike general self-care advice, strategic restoration planning involves a clinician-guided analysis of the client’s specific resource deficits and the deliberate design of replenishment activities matched to those deficits. A client whose primary depletion is social isolation needs different restoration than a client whose depletion is sensory
overstimulation. The plan should include micro-restorations (brief, daily practices), meso-restorations (weekly or biweekly activities of moderate duration), and macro-restorations (periodic extended disengagement from the primary source of demand). Clinicians should help clients anticipate and manage the guilt that often accompanies early attempts at restoration.
7. Ongoing Monitoring and Relapse Prevention
Resilience fatigue has a recurrent quality, particularly for clients whose life circumstances involve ongoing adversity. Treatment should include the development of a personalized early-warning system — a set of behavioral and emotional indicators that signal the return of resource depletion. Regular check-ins using brief screening tools, collaborative review of the client’s restoration plan, and explicit identification of high-risk periods (seasonal stressors, anniversaries of loss, periods of increased caregiving demand) support sustained recovery.
Systemic and Ethical Considerations for Clinicians
Clinicians working with resilience fatigue must attend to several systemic and ethical dimensions that shape both the condition and its treatment.
Cultural Humility in Assessment
Resilience narratives are deeply culturally embedded. In some communities, the expectation of stoic endurance is so pervasive that even naming one’s depletion is taboo. Clinicians should approach assessment with cultural humility, recognizing that the construct of resilience fatigue may need to be presented in language that resonates with the client’s cultural framework. Asking “What does your community expect of someone who is struggling?” can reveal the social pressures that sustain the fatigue.
Clinician Self-Awareness
Mental health professionals are themselves highly susceptible to resilience fatigue, given the cumulative demands of clinical work. Clinicians should engage in regular self-assessment, recognizing that their own unacknowledged resilience fatigue can compromise therapeutic effectiveness — manifesting as emotional detachment, irritability with clients, or a subtle shift toward dismissiveness of client distress. Supervision, peer consultation, and personal therapy are not luxuries but necessities in this context.
Advocacy and Systems-Level Intervention
While individual treatment is essential, clinicians should also consider their role in addressing the systemic conditions that produce resilience fatigue. This includes advocating for institutional changes — such as realistic caseloads, trauma-informed organizational practices, and equitable distribution of labor in caregiving systems — that reduce the need for individuals to absorb systemic failures through personal endurance.
How ICANotes Helps Clinicians Identify and Document Resilience Fatigue
Resilience fatigue is often missed—not because clinicians lack skill, but because the symptoms are subtle, masked, and distributed across multiple domains. Clients may appear highly functional while experiencing significant internal depletion, making accurate documentation more challenging.
ICANotes is designed specifically for behavioral health clinicians, with structured prompts and narrative guidance that help surface clinically relevant patterns across emotional, cognitive, behavioral, and relational domains.
With ICANotes, you can:
- Capture subtle symptom patterns across multiple domains
- Document changes in adaptive coping over time
- Support medical necessity with clear functional impairment language
- Maintain consistency across sessions for better clinical insight
- Reduce documentation time while improving note quality
Because resilience fatigue develops gradually, structured documentation helps clinicians identify patterns over time—not just isolated symptoms—leading to more accurate diagnosis, stronger treatment planning, and more defensible clinical records.
|
START FREE TRIAL
Capture What Others Miss in Your Clinical DocumentationWhen resilience fatigue is subtle, your documentation matters more than ever. ICANotes helps you identify patterns, support medical necessity, and create audit-ready notes without slowing down your workflow.
No credit card required. Get 30 days of full access plus free training and support. |
|
Frequently Asked Questions About Resilience Fatigue
Conclusion: Toward a More Honest Relationship with Resilience
Resilience fatigue challenges the clinical community to hold a more nuanced view of human adaptation. Strength is not unlimited. Coping is not costless. And the individuals who appear most resilient are often the ones most at risk for a collapse that no one sees coming. By understanding the resilience fatigue definition in its full complexity, by learning to recognize resilience fatigue symptoms even when clients themselves do not report them, and by using real-world resilience fatigue examples to sharpen clinical intuition, practitioners can intervene earlier, more precisely, and with greater compassion.
The goal of treatment is not to make clients less resilient. It is to create the conditions under which resilience can coexist with rest, vulnerability can coexist with strength, and the human beings who have held up the weight of their worlds are finally permitted to set some of it down.
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.






