Blog > Documentation > EMDR Progress Notes: Template, Examples & Documentation Tips
EMDR Progress Notes: Templates, Examples & Documentation Tips for Every Phase
Writing effective EMDR progress notes requires more than capturing session details — it involves documenting targets, cognitions, and measurable change across each phase of treatment. This guide shows you how to write EMDR progress notes step by step, with a structured EMDR note template, real session examples, and practical guidance for documenting SUD and VOC scores, assessment questions, and treatment progress. Whether you're refining your documentation for clinical clarity or audit readiness, you'll learn exactly what to include in every EMDR session note.

Last Updated: March 30, 2026


What You'll Learn
- How EMDR therapy works and what sets it apart from traditional talk therapy
- The eight phases of EMDR treatment and what happens during each stage
- What to include in your EMDR progress notes for each phase
- How to use an EMDR note template to standardize your documentation
- Key EMDR assessment tools like the VOC and SUD scales and how to track them over time
Contents
- What EMDR Therapy Is and How It Works
- EMDR Note Template: What to Include in Every Session
- Phase 1: EMDR History Taking Questions & Treatment Planning
- Phase 2: How to Prepare Clients for EMDR
- Phase 3: EMDR Assessment Questions, VOC & SUD Scales
- Phases 4–7: EMDR Treatment Documentation
- Phase 8: EMDR Re-Evaluation
- EMDR Progress Note Examples
- Frequently Asked Questions About EMDR Documentation
- How ICANotes Can Help With EMDR Progress Notes
Accurate and consistent documentation is critical for effective EMDR therapy. Whether you're tracking client progress through each of the eight phases, preparing for audits, or ensuring continuity of care, a structured approach to your EMDR progress notes can streamline your workflow and strengthen your clinical record. A well-written EMDR progress note captures essential details from each session — including targets, cognitions, SUD and VOC ratings, and client response — helping ensure that your documentation reflects both the therapeutic interventions used and the client's movement across treatment.
This guide walks through what to document during every phase of EMDR, provides a ready-to-use EMDR note template, and includes EMDR progress note examples you can reference as you build your own documentation practice.
What EMDR Therapy Is and How It Works
Created by psychologist Francine Shapiro in the late 1980s, Eye Movement Desensitization and Reprocessing (EMDR) therapy was originally developed to treat post-traumatic stress disorder (PTSD). At the core of EMDR is the Adaptive Information Processing (AIP) model, also developed by Dr. Shapiro, which posits that PTSD symptoms and the symptoms of similar disorders stem from past experiences that the brain has not fully processed. The memories connected to those experiences remain loaded with the beliefs, emotions, and physical sensations that occurred at the time of the triggering event. Recalling the experience can unleash those unpleasant emotions, thoughts, and sensations, bringing on symptoms.
EMDR is notably different from other treatment modalities. Rather than asking a client to reflect on or discuss a traumatic experience in detail, an EMDR therapist guides the client through bilateral stimulation — most commonly guided eye movements — while the client focuses on the target memory. The goal is to change the brain's relationship with the memory so that recalling it no longer triggers a distress response.
EMDR is an example of short-term therapy. Sessions typically take place once or twice a week, and clients often complete treatment in six to 12 sessions, with some clients benefiting from fewer. Unlike CBT and other modalities that typically use 45-minute sessions, the average EMDR session runs about 90 minutes. The American Psychological Association (APA) conditionally recommends EMDR therapy as a PTSD treatment. For a deeper look at the research behind that recommendation, see our guide to EMDR effectiveness and how EMDR trauma therapy works.
EMDR therapy consists of eight phases: History Taking and Treatment Planning, Preparation, Assessment, Desensitization, Installation, Body Scan, Closure, and Re-Evaluation.
The 8 Phases of EMDR Therapy
EMDR treatment follows a structured eight-phase process that helps clinicians move from case conceptualization and preparation to reprocessing, closure, and ongoing re-evaluation.
What EMDR Therapy Is and How It Works
A consistent EMDR note template helps streamline documentation while ensuring that every clinically relevant detail is captured across sessions. Rather than rebuilding your note structure each time, a standardized framework allows you to quickly document key elements such as target memories, negative and positive cognitions, SUD and VOC ratings, interventions used, and the client’s response to processing.
Using a structured approach also makes it easier to track progress over time, demonstrate medical necessity, and maintain continuity of care—especially when clients move between phases of EMDR treatment. The template below outlines the core components you should include in every EMDR progress note, regardless of which phase you are documenting.
Session Information
| Field | Description |
|---|---|
| Date | Date of session |
| Client Name/ID | Client identifier |
| Session Number | Sequential EMDR session number (e.g., 1, 2, 3) |
| Current Phase | Which EMDR phase was addressed (e.g., Phase 4 – Desensitization) |
| Prong Addressed | Past memory, present trigger, or future template |
Target & Cognitions
| Field | Description |
|---|---|
| Target Memory/Issue | The specific memory, trigger, or future scenario addressed |
| Image | The image the client associates with the target |
| Negative Cognition (NC) | The client’s negative self-belief (e.g., “I am not safe”) |
| Positive Cognition (PC) | The client’s desired positive belief (e.g., “I can protect myself”) |
| VOC Rating | Validity of Cognition, rated 1 (completely false) to 7 (completely true) |
| SUD Rating | Subjective Units of Disturbance, rated 0 (no disturbance) to 10 (worst disturbance) |
| Emotions | Emotions the client reported during the session |
| Body Sensations | Physical sensations the client noticed |
Intervention & Clinical Notes
| Field | Description |
|---|---|
| Bilateral Stimulation Type | Eye movements, taps, auditory tones, etc. |
| Interventions Used | Safe/Calm Place exercise, cognitive interweave, containment, or other interventions used |
| Client Response | Shifts in imagery, affect, cognitions, or body sensations during processing |
| Clinical Impressions | Your assessment of client progress, affect tolerance, and engagement |
| SUD Post-Processing | SUD rating at end of session |
| VOC Post-Processing | VOC rating at end of session |
| Closure Method | How the session was closed (debriefing, containment exercise, Safe/Calm Place, etc.) |
Planning
| Field | Description |
|---|---|
| Client Status at End | Stable, mildly activated, or requires follow-up |
| Plan for Next Session | Target, phase, or additional interventions to address |
| Other Planned Treatments | Any concurrent therapies, such as CBT or medication management |
Using a structured template like this across all sessions makes it easier to track SUD and VOC trends over time, demonstrate medical necessity for audits, and maintain continuity if the client transitions to another provider.
Phase 1 - EMDR History Taking Questions and Treatment Planning
The first phase of EMDR — History Taking and Treatment Planning — typically spans one to two sessions. During this phase, you gather a comprehensive history from the client and identify the targets that will guide treatment.
EMDR history taking generally follows a three-pronged approach. You'll explore disturbing memories from the past, issues and triggers in the present, and the client's future goals and desired responses.
Questions to Ask During EMDR History Taking
Begin by asking the client what problem they want to address. From there, explore details such as when the issue happens, who's involved, when it first started, and what about it upsets the client most.
Next, ask the client to identify disturbing events in their past and provide a general age or timeframe for each. In your progress notes, lay these events out on a timeline so you can easily visualize the client's history and identify patterns.
Then examine how past events affect the client's present. Key questions include:
- When was the last time you experienced this issue?
- How did you feel when it happened? What did you experience in your body?
- What was the worst part of the situation — an image, smell, noise, emotion, or sensation?
- What negative beliefs do you have about yourself in relation to this situation?
Finally, address the client's future orientation with questions like:
- When do you see this situation happening again?
- How would you like to respond if it occurs in the future?
What to Document in Phase 1
In your progress notes for history taking sessions, record the client's identified targets and organize them on a timeline. Note the presenting problem, the client's negative and positive self-beliefs, the most distressing memory or memories identified, current triggers, and future goals. This documentation becomes the foundation for your EMDR treatment plan and guides which targets you'll address first.
It's important to remember that one feature setting EMDR apart from other modalities is that the client doesn't need to go into extensive detail about their most challenging memory. You can ask questions and take notes, but a complete narrative of the event isn't necessary for treatment to be effective.
Phase 2: How to Prepare Clients for EMDR
After gathering the client's history, the Preparation phase focuses on building trust, explaining the EMDR process, and equipping the client with self-regulation strategies they can use during processing.
Think of this phase as trust-building. If clients don't feel safe with you and confident in the process, therapy won't be as effective. One of the primary tools used in preparation is the Safe/Calm Place exercise, which helps clients establish an internal resource they can access when they feel activated during or between sessions.
The Safe/Calm Place Exercise
Walk your client through the following Safe/Calm Place Exercise steps:
- Identify the image. Ask the client to describe a place they find safe and calming. Document their description.
- Explore sensations. Ask what emotions and sensations they experience when thinking of that place. Record any images, sounds, smells, or physical feelings they describe.
- Deepen the experience. Ask the client to go deeper into the emotions and sensations.
- Introduce bilateral stimulation. Have the client think of their calm place and the sensations it creates, then ask them to follow your finger with their eyes. You may need to repeat this several times.
- Establish a cue word. Ask the client to summarize their safe/calm place with a single word. Write this word down — it's their cue word for future sessions.
- Test self-cueing. Ask the client to think of their cue word on their own and note how they feel.
What to Document in the Preparation Phase
In your EMDR progress notes for the Preparation phase, record the client's Safe/Calm Place description, their cue word, the bilateral stimulation method used, and the client's response to self-cueing. Also note any other stabilization or grounding techniques introduced and whether the client appears ready to move into the Assessment phase. If additional preparation sessions are needed, document why and your plan for the next session.
Phase 3: EMDR Assessment Questions, VOC & SUD Scales
Once the client has been prepared, you move into the Assessment phase. This is where you establish the baseline measurements that will guide and track treatment progress using two key scales: the Validity of Cognition (VOC) scale and the Subjective Units of Disturbance (SUD) scale.
Assessment Questions to Ask
Before applying either scale, the client needs to identify a specific, distressing image from the target experience. Ask the client to describe a mental picture or image from the event and note their response. Then guide them through the following:
- Identify the Negative Cognition (NC). Ask the client to state a negative self-belief connected to the experience. Examples include "I am bad," "I can't be loved," "I am weak," or "I am not safe."
- Identify the Positive Cognition (PC). Ask the client to choose a positive belief they'd like to hold instead. Ideally, this is the reverse of the negative belief — for example, "I am good," "I am loveable," "I am strong," or "I can protect myself." The goal is to give the client a sense of control.
- Rate on the VOC scale. Ask the client to rate how true the positive belief feels on a scale of 1 to 7, where 1 is completely false and 7 is completely true.
- Rate on the SUD scale. Ask the client to rate how disturbing the target memory feels on a scale of 0 to 10, where 0 is no disturbance and 10 is the worst disturbance they can imagine.

Tracking SUD and VOC Across Sessions
The VOC and SUD scales are your primary tools for measuring progress through treatment. Document the client's ratings at the beginning and end of each processing session. Over the course of treatment, the SUD should decrease (ideally reaching 0) and the VOC should increase (ideally reaching 7). Tracking these ratings session over session gives you a clear picture of whether processing is progressing or whether a different approach is needed.
Phases 4-7: EMDR Treatment Documentation
The treatment phases — Desensitization (Phase 4), Installation (Phase 5), Body Scan (Phase 6), and Closure (Phase 7) — may span multiple sessions. How you document each depends on how far the client progresses in a given session.
Phase 4: Desensitization
The goal of desensitization is to transform the target memory from something distressing into something that no longer activates the client. During this phase, you ask the client to focus on the target image and their negative cognition while performing bilateral stimulation, such as following your finger with their eyes. You'll guide them through multiple sets, checking in on their SUD rating after each one.
What to document: Record the target memory, the bilateral stimulation method, the number of sets completed, any shifts in the client's imagery or affect, the SUD rating at the start and end of the session, and the planned focus for the next session. The goal is to bring the SUD down to 0 — though for some clients, a 1 or 2 may be an acceptable endpoint.
Phase 5: Installation
While desensitization focuses on reducing SUD, the Installation phase aims to strengthen the client's positive cognition and increase their VOC rating.
Start by checking in with the client about their positive cognition. Is it still relevant, or has a more fitting belief emerged? Document any changes. Then ask the client to hold the positive cognition in mind while performing bilateral stimulation. After each set, ask them to rate the positive cognition on the VOC scale again. Continue until the client reaches a 7.
If the client consistently plateaus at the same rating, ask what's keeping them from fully believing the positive cognition. You may need to pause installation for the session and document the block for follow-up.
What to document: Record the positive cognition (and any changes), VOC ratings before and after each set, any identified blocks, and whether installation is complete.
Phase 6: Body Scan
Move to the Body Scan phase only when the client's SUD is 0 and their VOC is 7. Have the client think of the target image and their positive belief, then ask them to scan their body and note any remaining distress or tension. If distress is present, use bilateral stimulation to process it.
What to document: Record any body sensations the client reported, the bilateral stimulation used, and whether the body scan was completed successfully or requires further processing.
Phase 7: Closure
Closure happens at the end of every session, regardless of whether the client completed all treatment phases. If processing is incomplete, you may need to perform a containment exercise to stabilize the client before they leave.
If the session is complete (SUD of 0, VOC of 7, clean body scan), focus on debriefing. Let the client know they may continue to process the session material after they leave, and encourage them to record any thoughts, feelings, or dreams that come up. If additional sessions are planned, make a plan for the next one.
What to document: Record the closure method used (debriefing, containment, Safe/Calm Place), the client's status at the end of the session (stable, mildly activated, etc.), any instructions given to the client, and the plan for the next session.
Phase 8: EMDR Re-Evaluation
Re-Evaluation occurs at the beginning of each session after the first. During this phase, you touch base with the client to assess what has come up since the previous session — new memories, dreams, emotional shifts, or changes in how they experience the target issue.
What to document: Record the client's report of between-session experiences, any changes in SUD or VOC from the previous session's target, whether the previous target requires continued processing or is resolved, and your plan for the current session based on the client's presentation.
How EMDR Processing Typically Progresses in Session
During the middle phases of EMDR, clinicians often move through a repeatable workflow that helps reduce distress, strengthen adaptive beliefs, and confirm that the target has been fully processed.
In documentation, this sequence helps clinicians show not only what interventions were used, but also how the client responded and whether the target appears resolved.
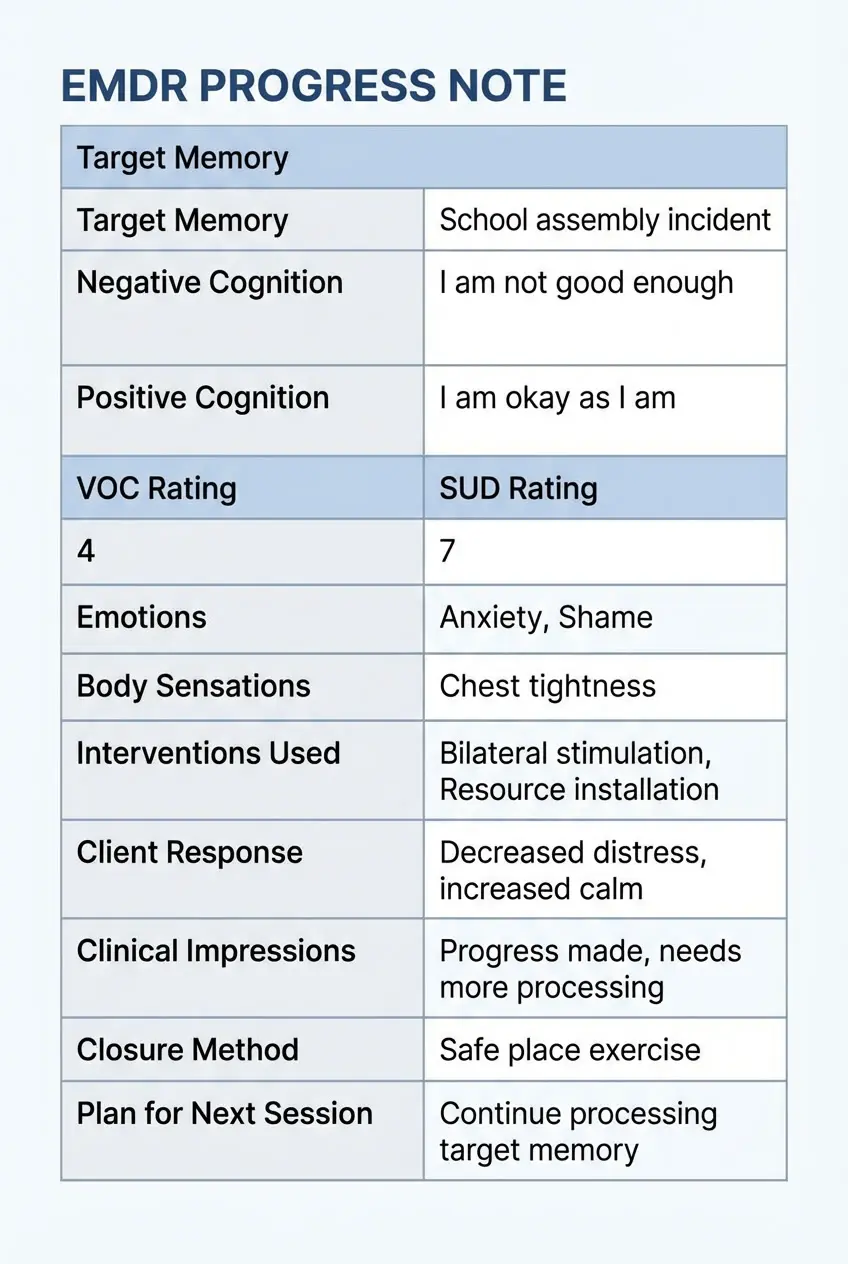
EMDR Progress Note Examples
Using structured EMDR note templates helps ensure consistency, supports medical necessity, and improves treatment planning. Below are two examples illustrating how to document different phases of treatment.
Frequently Asked Questions About EMDR Documentation
How ICANotes Can Help With EMDR Progress Notes
Accurate EMDR session notes are essential for tracking a client's progress through each phase of treatment, but detailed documentation shouldn't come at the cost of session flow. ICANotes simplifies the process with intuitive, structured EMDR note templates that guide you through documenting key clinical details — including targets, triggers, SUD and VOC ratings, cognitions, and client responses.
These templates help ensure your EMDR progress notes are both comprehensive and compliant, whether you're documenting a straightforward desensitization session or a complex multi-phase appointment. Schedule a demo to see how ICANotes can support your EMDR documentation needs.

Schedule a Live Demo
Experience the most intuitive, clinically robust EHR designed for behavioral health professionals—built to streamline documentation, improve compliance, and enhance patient care.
- Simplify clinical charting
- Stay organized with appointment scheduling
- Reduce no-shows with automated reminders
- Improve client engagement with a secure patient portal
- Provide flexible care with HIPAA-compliant telehealth
Simplify clinical charting
Stay organized with appointment scheduling
Reduce no-shows with automated reminders
Improve client engagement with a secure patient portal
Provide flexible care with HIPAA-compliant telehealth
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.








