Blog > Treatment Strategies > ACT for Depression: Practical ACT Interventions That Work
ACT for Depression: Practical Acceptance and Commitment Therapy Interventions for Chronic Depression
Acceptance and Commitment Therapy (ACT) offers a powerful, evidence-informed approach to treating depression by helping clients change their relationship to painful thoughts and emotions rather than trying to eliminate them. In this guide to acceptance and commitment therapy for depression, you’ll learn practical ACT interventions for depression, including cognitive defusion, values clarification, and committed action techniques that help clients move forward — even when symptoms persist. Whether you’re new to ACT therapy for depression or looking to deepen your clinical skill set, this article provides structured tools you can apply immediately.

Last Updated: March 12, 2026


What You'll Learn
- Why acceptance and commitment therapy for depression focuses on changing your relationship to thoughts — not debating them
- How cognitive fusion and experiential avoidance can quietly reinforce chronic depression
- Practical ACT interventions for depression: defusion scripts, mindfulness anchors, and values-to-action planning
- How to use the Choice Point and Struggle Switch to help clients stop organizing life around avoidance
- Case-based ACT techniques for depression you can apply with rumination, self-criticism, and low motivation
- How to structure ACT treatment for depression with micro-steps, self-monitoring, and values-aligned committed action
Contents
- The 6 Core ACT Processes
- 2 ACT Psychoeducation Tools Clients Actually Remember
- ACT Techniques for Depression You Can Use Right Away
- Case Vignettes: ACT Interventions for Depression in Context
- ACT Metaphors That Work Especially Well for Depression
- ACT and Suicidal Thoughts
- FAQ: ACT for Depression
- How ICANotes Supports ACT-Informed Depression Care
Depression doesn’t just change mood — it changes behavior, identity, and a person’s relationship to their own thoughts. Acceptance and Commitment Therapy (ACT) offers a powerful, strengths-based way to treat depression that doesn’t require clients to “think positive” or eliminate painful feelings before taking action. Instead, ACT helps clients build psychological flexibility: the capacity to experience difficult internal states while still moving toward what matters.
In this guide, you’ll learn how acceptance and commitment therapy for depression works, why it’s especially helpful for chronic depression, and which ACT interventions for depression you can apply immediately — using clear examples, metaphors, and brief case vignettes.
What Makes ACT Different for Depression?
Many approaches to depression focus on changing the content of thoughts (“Is this thought true?” “What’s a more balanced thought?”). ACT takes a different approach:
- In ACT, thoughts aren’t treated as literal truths or commands.
- ACT focuses less on symptom eradication and more on living a values-directed life even with symptoms present.
- ACT targets the processes that keep depression stuck: cognitive fusion, experiential avoidance, disconnection from values, and inaction.
Quick Clinical Snapshot: “Jordan” and the Depression Cycle
Jordan (32) presents with low mood, fatigue, and worthlessness. They’re fused to thoughts like “I’m a failure” and treat these thoughts as absolute truth. When those thoughts show up, Jordan withdraws, stays in bed, avoids jobs and friends, and becomes increasingly disconnected from values like connection, creativity, and contribution—fueling the depression cycle.
The 6 Core ACT Processes (and how they map to depression)
Think of ACT as a framework with six pillars. These are the core processes of ACT and the backbone of ACT treatment for depression:
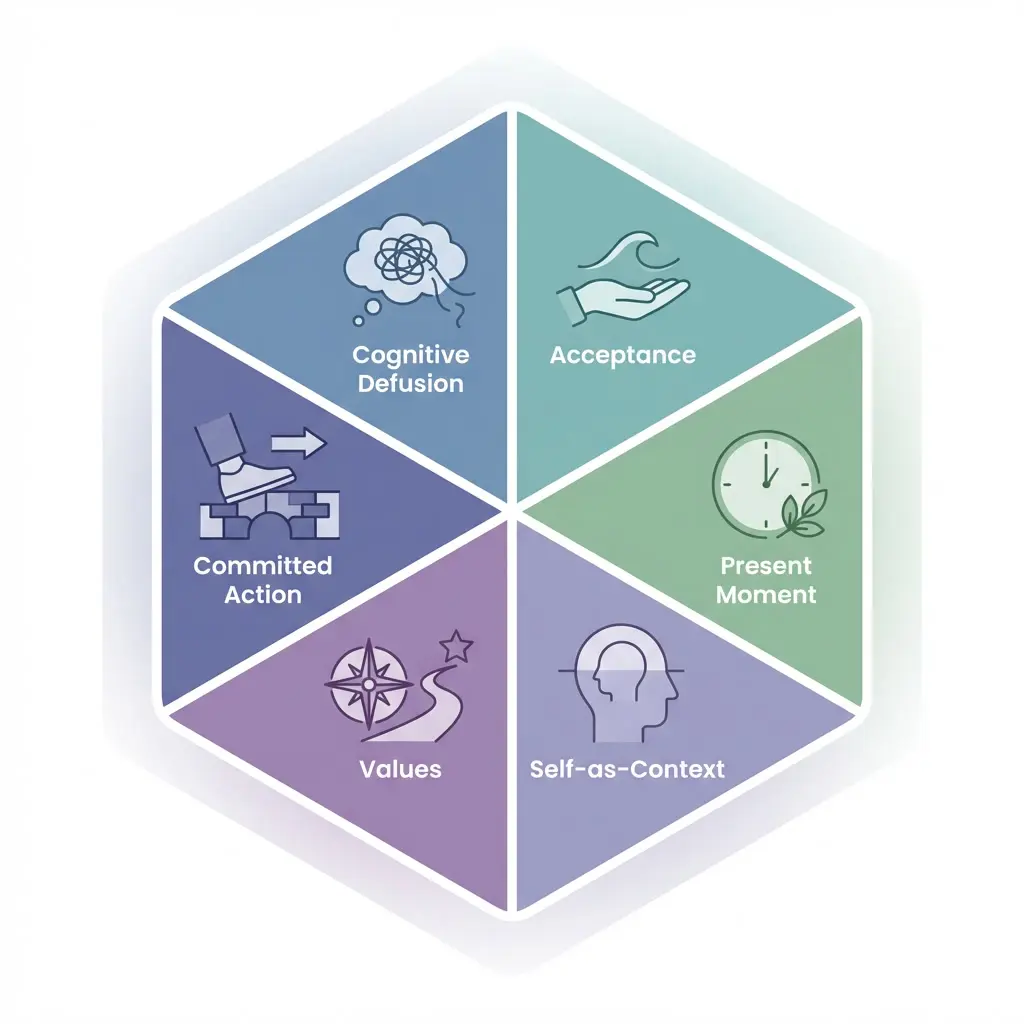
1) Cognitive Defusion
Goal: Help clients see thoughts as thoughts—not truths.
Depression Example:
Shift from “I am worthless” to “I’m having the thought that I’m worthless.”
That tiny language change often creates enough distance for a client to choose a different next step.
Simple Prompt:
“When your mind says ‘I’m a failure,’ can you practice saying: ‘I’m noticing my mind is offering the ‘failure’ story again’?”
2) Acceptance
Goal: Allow unpleasant thoughts and feelings without avoidance.
In depression, avoidance can look like staying in bed, canceling plans, not returning texts, “doom scrolling,” procrastinating, isolating—anything that temporarily reduces discomfort but expands the depression over time.
3) Present-Moment Awareness
Goal: Gently shift from rumination to noticing the here-and-now.
Depression often pulls clients into the past (“what I should have done”) or the future (“it won’t ever get better”). Present-moment skills create grounding and reduce the mental time travel that intensifies hopelessness.
4) Self-as-Context
Goal: Help clients experience a stable “noticer” perspective that isn’t defined by mood.
This is especially important in chronic depression, where identity can collapse into symptoms (“This is just who I am”).
5) Values Clarification
Goal: Identify what matters most—even when energy is low and symptoms persist.
Values aren’t goals; they’re directions. In depression, values help clients rebuild meaning and choose actions that support identity and purpose.
6) Committed Action
Goal: Take small, values-aligned steps—even with depression present.
Key ACT Stance: Action doesn’t require motivation first. In many cases, motivation follows action.
Once values are clarified and micro-actions are identified, link those activities to measurable treatment goals — see our guide on creating a depression treatment plan for templates and documentation tips.
Two ACT Psychoeducation Tools Clients Actually Remember
Before introducing ACT tools like the Choice Point or the Struggle Switch, it’s important to ground treatment in a clear understanding of symptom severity and functional impairment. Many clinicians begin with structured screening measures to establish a baseline and monitor progress over time. If you’re looking for validated instruments to support your clinical work, explore these depression assessment tools clinicians commonly use to measure mood, functioning, and risk.
Once symptoms are assessed and documented, psychoeducation becomes more effective. ACT-based tools like the Choice Point and the Struggle Switch help clients understand not just what they’re feeling — but how their relationship to those thoughts and emotions can either reinforce or interrupt the depression cycle.
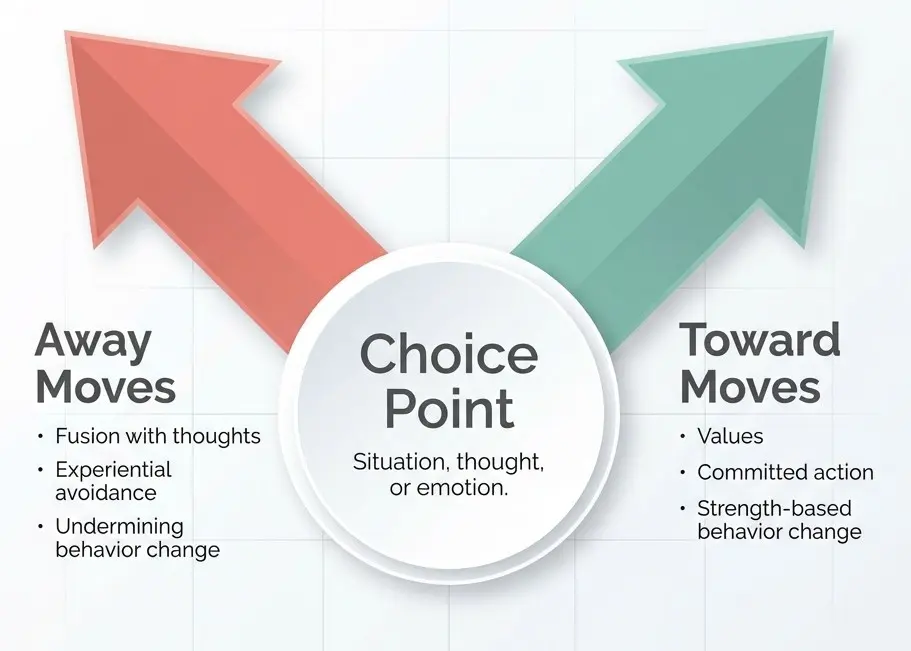
The Choice Point (hooks vs. helpers)
The “choice point” frames each moment as a fork in the road:
- Hooks pull clients into away moves (avoidance, isolation, rumination, shutting down).
- Helpers support toward moves (values-aligned action, connection, skill use, showing up).
This is a simple, empowering model for depressed clients: Even when depression is present, there’s still a choice point available.
The Struggle Switch (why fighting feelings can backfire)
The more clients struggle to eliminate depression (“I shouldn’t feel this way”), the more suffering can expand. Turning the struggle switch “off” doesn’t mean liking depression — it means reducing the energy spent fighting internal experiences so clients can spend that energy living.
A common metaphor: a beach ball held underwater. The harder you push it down, the more force it pushes back. When you stop struggling, you have more room to respond effectively.
ACT Techniques for Depression You Can Use Right Away
ACT Technique #1: “I’m having the thought that…”
This is one of the most accessible ACT techniques for depression, especially early in treatment.
Try it with common depressive thoughts:
- “I’m having the thought that nothing matters.”
- “I’m having the thought that I’m broken.”
- “I’m having the thought that I’ll always feel this way.”
Clinical aim: Reduce fusion so the client can choose behavior with more freedom.
ACT Technique #2: “Drop the Rope”
Tug-of-war defusion exercise: Use a short rope and set up a gentle tug-of-war where you represent the client’s depressive thought (e.g., “I’m worthless”). Then invite the client to drop the rope.
Key processing questions:
- “What changes when you stop wrestling with the thought?”
- “If the thought can be present without you fighting it, what could you do next?”
- “What would a ‘toward move’ look like—even with this thought riding along?”
Why it works: Clients directly experience how fighting thoughts consumes energy and narrows options.
ACT Technique #3: “Milk, Milk, Milk” Repetition
Have the client repeat a fused thought out loud multiple times (e.g., “I ruin all my relationships…”) until it starts to sound like a string of words rather than a fact.
Clinical aim: The thought loses some of its grip and emotional “charge,” supporting defusion.
ACT Technique #4: Values → Micro-Actions
Depressed clients often say, “I’m waiting to feel better first.” ACT responds: do before you feel—but do it small and values-aligned.
Example:
Clinical note: Normalize repetition. Depression-friendly behavior change is often a marathon, built from micro-steps.
Case Vignettes: ACT Interventions for Depression in Context
Case 1: Stuck in the past (rumination + guilt)
Client: Sarah, 34, teacher
Pattern: Persistent rumination and guilt about past relationship failures. Social withdrawal and poor sleep.
ACT focus: Cognitive fusion + present-moment awareness
ACT interventions:
- Defusion practice with her core thought (“I ruin all my relationships”), including repetition
- Mindful breathing + “noticer” language: observing thoughts without wrestling them
Case 2: “I’m not good enough” (identity fusion)
Client: Miguel, 27, graduate student
Pattern: Harsh self-criticism, procrastination, “I’m a failure.”
ACT focus: Self-as-context + defusion
ACT interventions:
- Leaves on a stream visualization (thoughts come, thoughts go)
- Chessboard metaphor: “You are the board; thoughts are pieces that move”
Case 3: Waiting to feel better first (low motivation trap)
Client: Jamila, 40, single parent
Pattern: Avoids activities she used to enjoy while waiting for depression to lift.
ACT focus: Values + committed action
ACT interventions:
- Values clarification (life domains worksheet; “preferred future” questions)
- Micro-commitments tied to values (e.g., 5 minutes of connection)
ACT Metaphors That Work Especially Well for Depression
Metaphors help depressed clients “get” ACT without over-intellectualizing it. A few favorites:
Passengers on the Bus
The client is the driver. Thoughts and feelings are passengers—some supportive, some loud and cruel. The goal isn’t to kick them off; it’s to keep driving toward values even while they shout.
Quicksand
The more you struggle to escape, the deeper you sink. ACT invites clients to make room and shift the relationship rather than intensifying the fight.
Weather in the Sky
A useful line (often attributed in ACT circles):
Depressive states are real—but they are not the whole self.
ACT and Suicidal Thoughts: A Careful Clinical Application
ACT defusion can be useful when clients experience suicidal thoughts, because it can reduce the “command” quality of the thought and help clients relate to it as a mental event rather than an instruction.
Examples of defusion language:
- “I’m having the thought that I want to die.”
- “I’m noticing my mind is offering suicide as a solution right now.”
ACT can also invite curiosity:
- “It’s interesting that this thought is showing up. What might it be signaling I need — support, rest, safety, connection, medical care?”
Important: Suicidal thoughts should always be handled within your scope of practice, with appropriate risk assessment, safety planning, and referral/emergency steps when indicated.
Frequently Asked Questions: ACT for Depression
How ICANotes Supports ACT-Informed Depression Care
ACT for depression works best when clinicians can document clearly, efficiently, and defensibly—especially when working with sensitive content like suicidal ideation, values work, or behavioral activation plans.
ICANotes supports this workflow in a few practical ways:
- Built-in screening tools and assessments (e.g., sending a PHQ-9 through the portal before session)
- Structured progress note options that help clinicians capture symptoms, functioning, and interventions efficiently
- Treatment plan linkage so progress notes align with goals/objectives (important for audits and medical necessity)
- Ambient Scribe with clinician control designed to generate a clinical note without retaining session transcript/audio—reducing legal and privacy risk compared to tools that store raw session records
- Custom buttons (“shortcuts”) so ACT interventions (defusion scripts, values prompts, metaphors used, committed action plans) can be inserted consistently without retyping
Ready to document ACT-informed depression care faster — without losing clinical depth?
Explore a demo or start a free trial.
Start Your 30-Day Free Trial
Experience the most intuitive, clinically robust EHR designed for behavioral health professionals, built to streamline documentation, improve compliance, and enhance patient care.
- Complete Notes in Minutes - Purpose-built for behavioral health charting
- Always Audit-Ready – Structured documentation that meets payer requirements
- Keep Your Schedule Full – Automated reminders reduce costly no-shows
- Engage Clients Seamlessly – Secure portal for forms, messages, and payments
- HIPAA-Compliant Telehealth built into your workflow

Closing: ACT gives depressed clients a way forward — even when depression is still present
Acceptance and Commitment Therapy for depression helps clients stop organizing life around avoidance and instead begin building a life around values. With core ACT processes like defusion, acceptance, present-moment awareness, self-as-context, values, and committed action, clients can learn an empowering truth:
They don’t have to feel better first to take the next meaningful step.
Related Posts
About the Author
Diane Bigler, LCSW, LSCSW, is a Licensed Clinical Social Worker in Missouri and Kansas with over 25 years of experience in the mental health field. She has held clinical positions as an outpatient and in-home therapist and clinical supervisor in diverse settings. Diane was an Adjunct Professor of Social Work for 10 years at The University of Kansas, School of Social Welfare and a Field Liaison and Field Instructor. She has also held administrative positions as a Program Director and Coordinator. Diane is a popular local and national trainer on a wide variety of mental health and workplace development topics for clinicians and corporations and has facilitated over 500 training courses in the last few years. Visit her website http://www.







