Blog > Documentation > Mental Status Exam Cheat Sheet + Examples
Mental Status Exam Cheat Sheet (Free PDF) — Descriptors, Examples & Templates
Accurate mental status exams (MSEs) are a core part of clinical documentation. This guide gives you a practical, comprehensive reference for assessing and recording MSEs across all key domains — mood, cognition, speech, thought process, thought content, perception, insight, judgment, and more. You'll find ready-to-use descriptors, sample documentation phrases, complete MSE write-up examples, and a free downloadable cheat sheet you can apply in your notes right away.

Last Updated: March 18, 2026


What You'll Learn
-
The purpose and clinical value of the Mental Status Exam—and how it differs from cognitive screening tools like the MMSE.
-
How to assess and document each MSE domain, including appearance, behavior, speech, mood/affect, thought process, thought content, perception, and cognition.
-
Clinically useful descriptors, prompts, and examples you can use immediately in your notes.
-
How to identify red flags—such as psychosis, suicidal ideation, or cognitive decline—that require urgent intervention.
-
How to adapt the MSE for clients with cultural differences, language barriers, or low literacy.
-
Sample MSE write-ups for common clinical presentations, including depression and anxiety.
-
Practical tips to strengthen documentation clarity, accuracy, and defensibility.
-
How ICANotes streamlines mental status exam documentation using structured templates and automated narrative generation.
Contents
Clear and consistent MSE documentation supports better treatment decisions, continuity of care, and compliance with medical and insurance standards. As workloads grow and expectations increase, having a reliable method for charting mental status helps clinicians work more efficiently without missing essential details.
What Is a Mental Status Exam?
A Mental Status Exam (MSE) is a structured clinical assessment used to observe and document a client's current psychological and behavioral functioning. It captures observations across domains including appearance, behavior, speech, mood, affect, thought process, thought content, perception, cognition, insight, and judgment.
Clinicians use the MSE to form diagnostic impressions, track changes over time, support treatment planning, and communicate findings across care teams. It is a core component of every psychiatric and behavioral health encounter.
MSE Full Form
MSE stands for Mental Status Examination — a structured clinician-administered assessment of a patient’s current mental functioning across behavioral, emotional, and cognitive domains.
What is an MSE in Psychiatry?
In psychiatry, the MSE is the primary observational tool used during every clinical encounter. It documents the patient's presenting mental state in real time and forms the foundation of the psychiatric formulation. Psychiatrists use it to monitor symptom progression, evaluate medication response, assess safety risk, and guide diagnostic and treatment decisions.
MSE vs. MMSE: What Is the Difference?
The MSE and the Mini-Mental State Exam (MMSE) are frequently confused but serve very different purposes:
MSE vs. MMSE: Key Differences
Although the terms are sometimes used interchangeably, the Mental Status Exam (MSE) and the Mini-Mental State Examination (MMSE) are different clinical tools used for different purposes.
Bottom line: The MSE gives a broad clinical picture of a patient’s mental and emotional presentation, while the MMSE is a brief scored screening tool focused specifically on cognition.
The MSE is a clinician's comprehensive observational record; the MMSE is a brief scored test. The two are often used together — the MSE for overall mental functioning, the MMSE when cognitive screening is indicated.
Download our
Mental Status Exam Cheat Sheet
Download our free mental health status exam cheat sheet to use as a handy reference when performing a mental status exam. This cheat sheet walks you through every domain of the mental status exam with prompts, descriptors, and example language.
What’s Inside:
- Complete MSE categories, from appearance to cognition and environment.
- Clinically relevant descriptors for quick point-and-click use.
- Prompts and examples to guide your assessments and improve chart clarity.
- A structured format that mirrors ICANotes' built-in documentation tools.
Why are Mental Status Exams Important?
The MSE provides a structured snapshot of a client's emotional and cognitive functioning at a specific moment. It supports clinical decision-making in several critical ways:
- Establishes a baseline for the client's current mental state
- Supports accurate diagnosis by identifying symptoms and patterns
- Tracks progress or deterioration over time
- Guides treatment planning by revealing areas that need intervention
- Improves care coordination through clear, shared documentation
- Provides defensible documentation in the event of adverse outcomes or legal review
The MSE is especially valuable at intake, during clinical changes, following hospitalizations, after medication adjustments, or when coordinating care with other providers.
MSE Mnemonics: ASEPTIC and Other Memory Aids
Several mnemonics help clinicians remember MSE domains. The most widely used is ASEPTIC, which covers all core assessment areas:
ASEPTIC Mnemonic for Mental Status Exam
The ASEPTIC mnemonic is a widely used tool to help clinicians remember the key domains of a comprehensive mental status exam (MSE).
ASEPTIC mnemonic summarizing the core domains of a mental status exam used by behavioral health clinicians.
Other mnemonics include JAMSTAMPED (Judgment, Appearance, Mood, Speech, Thought process, Affect, Memory, Perception, Estimated cognitive functioning, Data reliability) and COASTMAP (Consciousness, Orientation, Affect/mood, Speech/language, Thought, Memory, Appearance/behavior, Perception). ASEPTIC is generally preferred for its simplicity and comprehensive coverage.
Components of a Mental Status Exam
A complete mental status examination covers the following domains:
- Appearance
- General Behavior
- Speech and Language
- Mood (subjective) and Affect (objective)
- Thought Process
- Thought Content
- Perception
- Cognition
- Insight and Judgment
- Environment (when applicable)
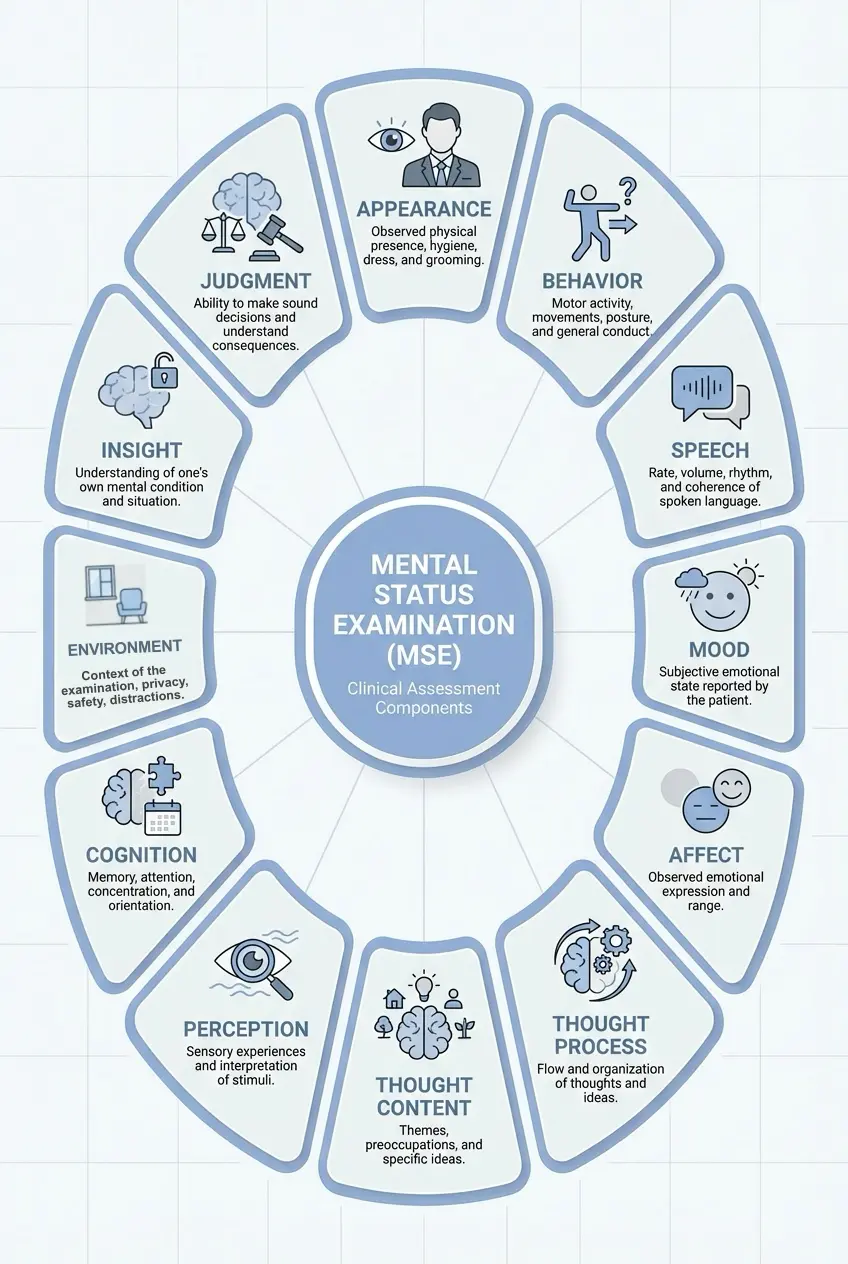
How to Perform a Mental Status Exam: MSE Checklist with Descriptors and Examples
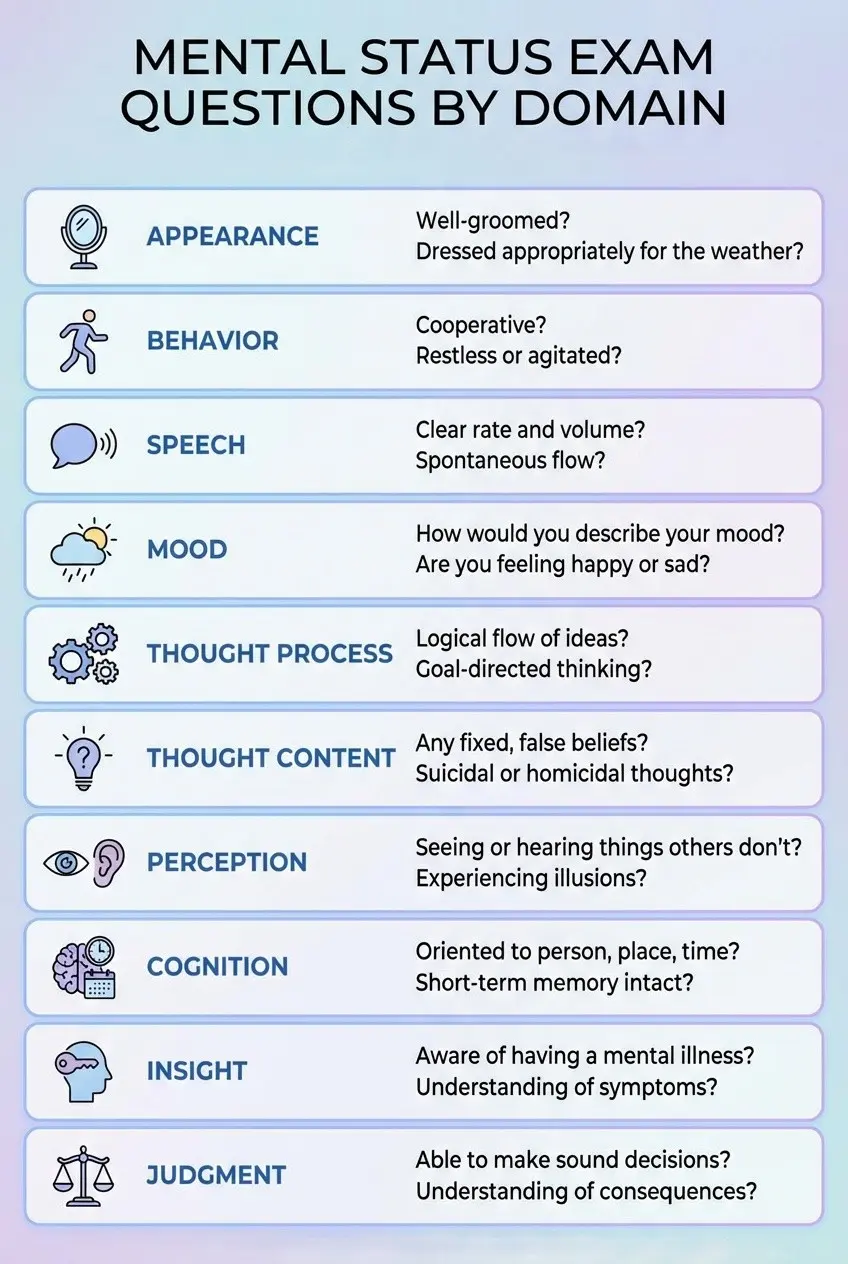
A mental status exam checklist helps clinicians observe and document key areas of a client’s mental functioning. While each session is different, the checklist below covers the core elements typically assessed and serves as a quick reference during documentation.
1. Appearance
Appearance refers to how the client presents physically during the session. This includes hygiene, grooming, clothing, posture, facial expression, and overall physical state. These observations offer insight into the client’s level of functioning, mood, and potential psychiatric symptoms. Look for signs of self-neglect, disorganization, or distress, and document objectively.
The client appears older than their stated age. Disheveled, with stained clothing and poor hygiene. Avoids eye contact and sits with a slouched posture.
Choosing precise appearance descriptors helps create clear, defensible documentation that supports diagnosis and treatment planning.
Appearance Descriptors & Sample Documentation Phrases
Use these common descriptors to document a client’s appearance clearly and objectively during a mental status exam.
Common appearance descriptors used in mental status exam documentation with example clinical phrasing.
- “How do you usually get ready for the day?”
- “Have you noticed any changes in your daily routines or energy levels?”
2. General Behavior
General behavior refers to how the client moves, responds, and engages during the session. This includes their motor activity, eye contact, cooperativeness, and any unusual movements. These observations can reflect a client’s emotional state, level of distress, neurological function, or possible side effects of medication. Note any signs of hostility, guardedness, or disinhibition.
The client sits rigidly, avoids eye contact, and displays frequent lip smacking. Motor activity is tense but controlled. Guarded attitude throughout the session.
Behavior Descriptors & Sample Documentation Phrases
Use these behavior descriptors to document how the client moves, responds, and engages during the session.
Common behavior descriptors used in mental status exam documentation with example clinical phrasing.
Use open-ended questions to assess engagement, motor activity, and behavioral patterns:
- “How are you feeling about today's session?”
- “Have you noticed any changes in your movement or body sensations lately?”
3. Speech & Language
Speech patterns offer insight into a client’s cognitive and emotional state. Evaluate how clearly the client speaks, the speed and rhythm of their speech, and the quality of their verbal expression. Disruptions may indicate mood disorders, anxiety, thought disorganization, or neurocognitive impairment. Pay attention to fluency, articulation, tone, and vocabulary use.
Speech is slow and soft, with a delayed onset. Responses are brief but coherent. Tone is flat; articulation clear.
Speech Examples for MSE Documentation
Use these speech and language descriptors to document rate, rhythm, volume, and verbal expression during the mental status exam.
Common speech and language descriptors used in MSE documentation with example clinical phrasing.
Use open-ended questions to assess speech patterns, language expression, and communication changes:
- “Has anyone mentioned changes in the way you speak lately?”
- “Do you feel like it’s harder to find words or express yourself?”
4. Mood and Affect
Mood is the client's subjective emotional experience (what they report). Affect is the clinician's objective observation of emotional expression (what you observe). Always document both, noting range, stability, intensity, and congruency between the two. These cues help identify mood disorders, anxiety, or trauma-related symptoms.
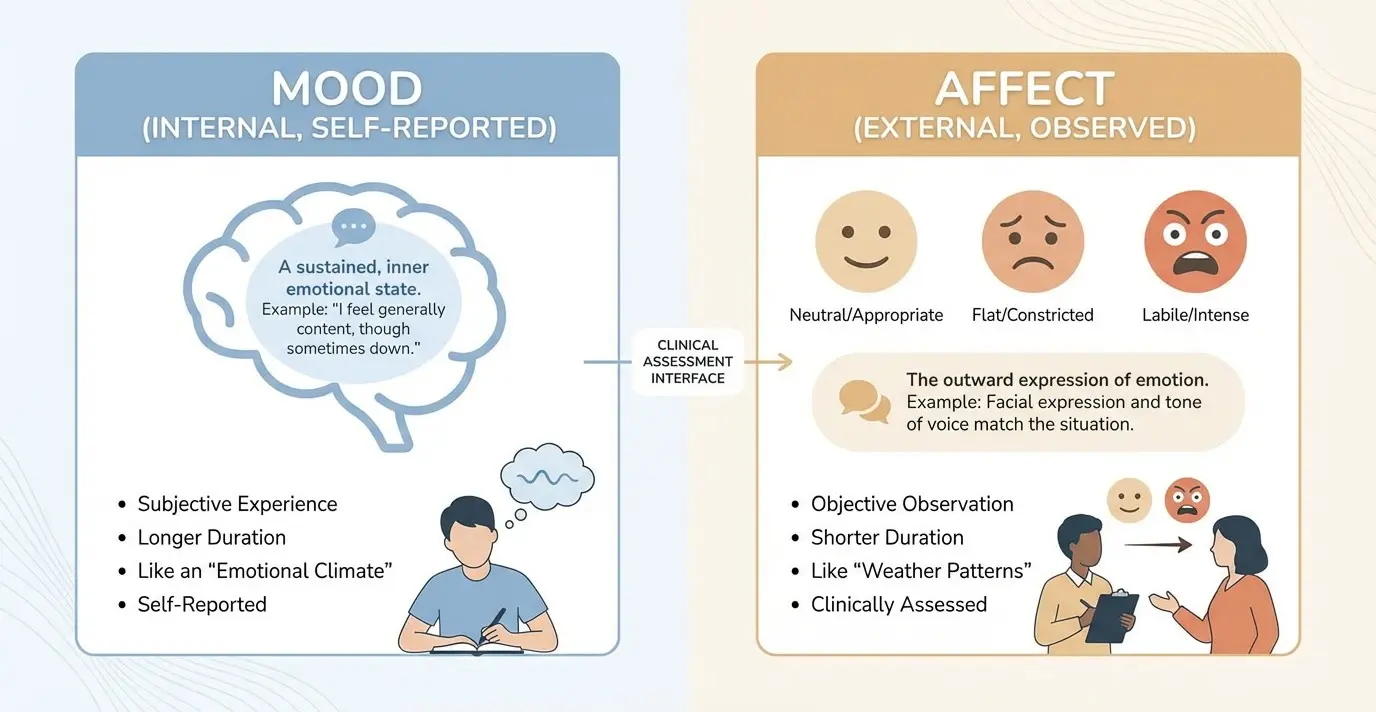
Client reports feeling "fine." Affect is flat with minimal expression and a monotone voice. Mood and affect appear incongruent.
Mood Descriptors & Sample Documentation Phrases
Use these common mood descriptors to document the client’s reported emotional experience during the mental status exam.
Common mood descriptors used in mental status exam documentation with example clinical phrasing.
Affect Descriptors & Sample Documentation Phrases
Use these descriptors to document observed emotional expression, including range, intensity, and congruency with mood.
Common affect descriptors used in mental status exam documentation with example clinical phrasing.
Use open-ended questions to assess the client’s subjective emotional experience and stability of mood:
- “How have you been feeling over the past few days?”
- “Would you say your emotions have been steady or up and down lately?”
5. Thought Process
Thought process describes how a client organizes and expresses ideas — the form or structure of thinking, not the content. It is evaluated through the flow, coherence, and organization of speech.
Thought process is tangential; client frequently veers off-topic and does not return to the original question without redirection.
Thought Process Examples & Descriptors
Use these descriptors to document how the client organizes, connects, and expresses ideas during the session.
Common thought process descriptors used in mental status exam documentation with example clinical phrasing.
Use open-ended questions to observe how the client organizes and connects their thoughts:
- “Can you tell me what brought you in today?”
- “What happened next?”
- “Can you walk me through that step by step?”
- “Can you help me understand how those ideas connect?”
Thought process is how the client thinks (the form), while thought content is what the client thinks about. Always document both separately to ensure a complete and clinically accurate mental status exam.
For a more in-depth look, read our related post: How do you assess thought process vs. thought content in a Mental Status Examination (MSE)?
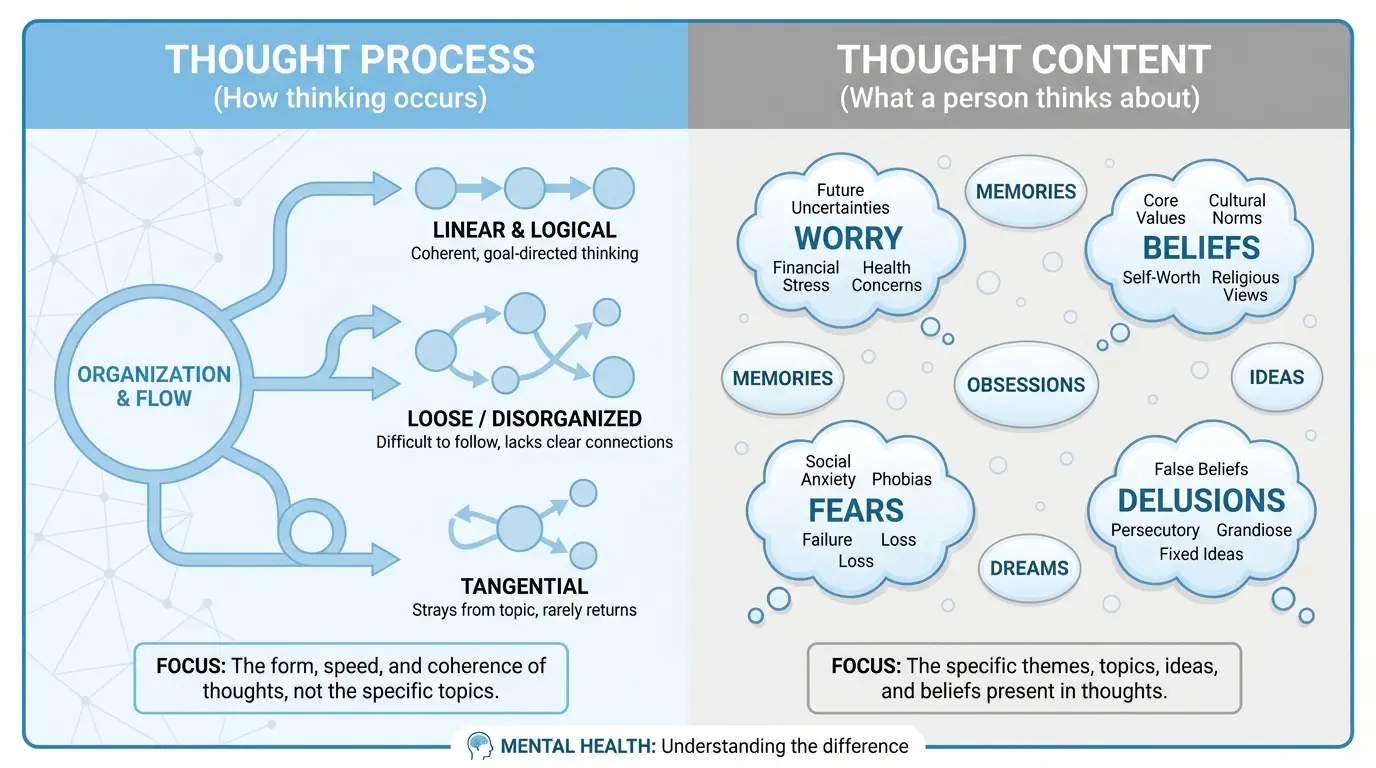
6. Thought Content
Thought content refers to what a client is thinking about — the dominant themes, beliefs, and preoccupations present in their thinking. This includes suicidal or homicidal ideation, delusions, obsessions, phobias, and other significant ideational content. Ask directly; do not assume absence of risk.
Client reports obsessive worry about contamination. Denies suicidal or homicidal ideation. No delusional ideation elicited.
Thought Content Examples & Descriptors
Use these descriptors to document what the client is thinking about, including dominant themes, preoccupations, risk, and distorted beliefs.
Common thought content descriptors used in mental status exam documentation with example clinical phrasing.
Use direct but non-assumptive questions to explore thought themes, beliefs, and safety:
- “What’s been on your mind most lately?”
- “Do you find yourself worrying about anything in particular?”
- “Have you had any thoughts about wanting to hurt yourself or someone else?”
- “Do you ever feel like people are watching you or talking about you?”
- “Do you have thoughts that feel intrusive or hard to control?”
When suicidal or homicidal ideation is present, always document: presence or absence of plan, intent, means, and any protective factors. Include disposition and safety planning.
7. Perception
Perception covers any alterations in sensory experience, including hallucinations (perception without external stimulus), illusions (misinterpretation of a real stimulus), depersonalization, and derealization. Ask about all sensory modalities, not just auditory.
Client reports hearing a male voice commenting on his actions approximately three times per day. No visual, tactile, or olfactory hallucinations reported.
Perception Descriptors & Sample Documentation Phrases
Use these descriptors to document perceptual disturbances, including hallucinations, illusions, and altered sensory experiences.
Common perception descriptors used in mental status exam documentation with example clinical phrasing.
Distinguish hallucinations (no external stimulus) from illusions (misinterpretation of a real stimulus). Always document modality, frequency, and the client’s response to the experience.
Normalize these questions to help assess perceptual disturbances without increasing stigma:
- “Have you noticed anything unusual with your senses, like hearing or seeing things others might not?”
- “Do you ever hear voices or sounds that others don’t seem to hear?”
- “Have you seen things that others don’t see?”
- “Have you had experiences where things didn’t feel real or felt distorted?”
8. Cognition
Cognitive assessment evaluates how well a client processes information, maintains awareness, recalls memories, and makes decisions. It can identify signs of dementia, delirium, traumatic brain injury, or other neurocognitive changes. Use formal screening tools such as the MMSE or MoCA when cognitive impairment is suspected.
Client is alert and oriented to person, place, and time. Attention is mildly impaired. Recalls 2 of 3 words after five minutes. Remote memory intact.
Cognition Descriptors & Sample Documentation Phrases
Use these descriptors to document orientation, attention, memory, and abstract reasoning during the mental status exam.
Common cognition descriptors used in mental status exam documentation with example clinical phrasing.
Use orientation, memory, and judgment questions to assess cognitive functioning during the mental status exam:
- “Can you tell me where we are and what today’s date is?”
- “I’ll say 3 words — can you repeat them back to me and remember them for later?”
9. Insight and Judgment
Insight refers to the client's awareness of their mental health condition and its impact. Judgment refers to their capacity to make sound decisions and anticipate consequences. Both are distinct domains and should always be documented together.
Insight impacts treatment engagement and adherence, making it a critical component of clinical assessment and documentation. Judgment is best assessed through both hypothetical safety questions and review of recent real-world decisions.
Insight Levels in MSE: A Five-Point Scale with Examples
Use this scale to rate and document insight consistently across clinical encounters.
A five-point framework for documenting insight in mental status examinations with clinical examples.
Judgment is fair; client demonstrates some awareness of consequences but reports recent difficulty making sound decisions under stress.
Judgment Descriptors & Sample Documentation Phrases
Judgment refers to the client’s ability to make sound decisions, anticipate consequences, and respond appropriately to everyday situations.
Common judgment descriptors used in mental status exam documentation with example clinical phrasing.
Impaired judgment increases risk for unsafe decisions, poor impulse control, and non-adherence to treatment. Always document how judgment impacts real-world functioning, especially when safety concerns are present.
Use hypothetical or real-world questions to assess how the client evaluates risk, consequences, and appropriate action:
- “What would you do if you smelled smoke in a building?”
- “What do you usually do when you have to make an important decision?”
- “Can you tell me about a recent decision you made and how you came to it?”
10. Environment (When Assessed)
When conducting a mental status exam in the client’s home or residential setting, their physical surroundings can offer important clues about cognitive functioning, reality testing, and self-care capacity. Environmental observations often supplement findings related to thought content, judgment, and overall functioning.
Key observations to document:
- Extreme clutter or hoarding behavior
- Unusual fortifications (furniture blocking doors or windows)
- Inappropriate use of household objects
- Evidence of unsafe living conditions
- Presence of dependents who may be at risk
Client's apartment is cluttered with stacks of newspapers and unused items. Furniture is positioned to block the front door. Client reports feeling safer with this arrangement.
Use these questions to assess safety, stability, and contextual factors in the client’s environment:
- “Where are you joining from today, and do you feel comfortable and safe there?”
- “Do you have privacy to talk freely right now?”
- “Have there been any recent changes in your living situation or environment?”
Always document environmental factors when they impact safety, privacy, or engagement — especially in telehealth sessions. Environmental context can influence risk assessment, disclosure, and clinical decision-making.
Complete Mental Status Exam Examples
The following complete MSE examples show how to document observations across all key domains. Use these as templates for your own clinical notes.
Mental Status Exam Example #1: Major Depressive Episode
Client: Maria R., 38-year-old Hispanic female.
Reason for visit: Worsening depressive symptoms over several weeks.
Appearance: Appears to be of stated age. Casually dressed, hair unkempt, minimal makeup. Mild body odor noted. Slouched posture.
Behavior: Psychomotor slowing observed. Avoids sustained eye contact but remains cooperative throughout. No abnormal movements.
Speech: Low volume, slow rate, monotone tone. Answers are brief but coherent.
Mood: Reports feeling "empty" and "exhausted."
Affect: Constricted and congruent with stated mood.
Thought Process: Logical and goal-directed, though slowed. No flight of ideas or tangentiality.
Thought Content: Endorses passive suicidal ideation ("I sometimes think people would be better off without me") without plan or intent. No delusions, obsessions, or phobias.
Perception: Denies hallucinations or perceptual disturbances.
Cognition: Alert and oriented x4. Attention mildly impaired; difficulty with serial 7s. Immediate and recent recall intact (3/3 words). Remote memory intact.
Insight: Fair. Acknowledges need for treatment.
Judgment: Intact for daily decisions.
Reliability: Considered reliable. Responses consistent and plausible.
Clinical Summary: Presentation consistent with a moderate depressive episode. No imminent safety risk identified, but suicidal ideation warrants monitoring. Safety plan reviewed and discussed.
Mental Status Exam Example #2: Anxiety with Panic Disorder
Client: Derrick W., 29-year-old White male.
Reason for visit: Episodes of intense anxiety and difficulty concentrating.
Appearance: Appears slightly younger than stated age. Clean and casually dressed. Frequent fidgeting noted.
Behavior: Restless; frequently shifts in seat. Good eye contact. No tics or involuntary movements observed.
Speech: Rapid rate with normal volume and clear articulation. Occasional pressured quality when describing panic symptoms.
Mood: Describes mood as "on edge" and "wired."
Affect: Anxious, with quick shifts in expression when discussing panic attacks. Congruent with stated mood.
Thought Process: Linear but occasionally distractible. No thought blocking or loose associations.
Thought Content: Excessive worry, rumination, and fear of future panic episodes. Denies suicidal or homicidal ideation. No delusional themes.
Perception: Denies hallucinations. Reports occasional derealization during panic episodes: "Everything feels unreal."
Cognition: Alert and oriented x4. Attention intact. Memory intact. Abstract thinking appropriate.
Insight: Good; recognizes symptoms as anxiety-related and is motivated for treatment.
Judgment: Intact.
Reliability: Reliable historian. Descriptions are detailed and consistent.
Clinical Summary: Findings support generalized anxiety with panic features. No acute safety concerns. Appropriate for outpatient treatment and monitoring.
Mental Status Exam Example #3: First-Episode Psychosis
Client: James T., 22-year-old White male.
Reason for visit: Family-initiated evaluation following two weeks of behavioral changes and social withdrawal.
Appearance: Appears consistent with stated age. Clothing is disheveled and inappropriate for weather; unkempt hair. Poor hygiene noted.
Behavior: Guarded and suspicious. Makes intermittent eye contact. Observed responding to internal stimuli — pausing, tilting head, and glancing toward the ceiling unprompted.
Speech: Slow rate with delayed onset. Articulation intact but speech is impoverished and difficult to initiate.
Mood: Reports feeling "watched" and "scared."
Affect: Blunted with flat expression. Incongruent with reported fear.
Thought Process: Loosely associated and tangential. Ideas do not connect logically. Occasional thought blocking noted.
Thought Content: Endorses persecutory delusions (neighbors are recording him through the walls). Ideas of reference present (television programs contain messages directed at him). Denies suicidal ideation. Denies homicidal ideation.
Perception: Reports auditory hallucinations — a male voice providing ongoing commentary on his actions. Frequency reported as "constant." Denies command hallucinations.
Cognition: Alert but disoriented to date. Attention severely impaired. Recalls 1 of 3 words after five minutes. Remote memory appears intact.
Insight: Absent. Does not believe he has a psychiatric illness; attributes experiences to external persecution.
Judgment: Severely impaired. Unable to identify appropriate responses to safety scenarios.
Reliability: Unreliable. Information is inconsistent with collateral report from family.
Clinical Summary: Presentation consistent with first-episode psychosis. Acute safety concern given impaired judgment, absent insight, and command hallucination screening negative. Psychiatric hospitalization discussed with family. Safety plan initiated.
Tips for Documenting a Mental Status Exam
Effective documentation of a mental status exam ensures that clinical observations are clear, useful, and defensible. These tips will help you document each session with greater accuracy and efficiency.
Observe Before Documenting
Begin by quietly observing the client’s behavior, appearance, and communication before asking structured questions or checking boxes.
First impressions are often the most revealing. Noting things like posture, clothing, grooming, and energy level during the first few minutes can give you an authentic baseline that scripted questions might not capture.
Use Objective and Descriptive Language
Your documentation should reflect what you can directly observe or what the client explicitly says. Avoid vague or subjective terms like "seems sad" or "looks anxious." Instead, describe the behavior: "Client avoided eye contact, sat hunched over, and spoke in a low, monotone voice." This type of language is clearer to other providers and strengthens the clinical value of your note.
Include Direct Quotes When Appropriate
Using the client’s exact words can provide valuable insight into their mental state, especially when describing mood, thought content, or delusions. Use quotes selectively for clinically significant expressions — for example, “I think I’m being followed” gives a clearer picture than a paraphrased summary.
Customize Your Documentation
Templates and checklists are helpful for structure, but overusing them can make notes feel generic or inaccurate. Always tailor the note to reflect the specific client’s presentation and behavior during the session. This ensures the documentation aligns with what actually occurred and avoids errors from autopopulated language.
Clearly Document Any Safety Concerns
Always document risk factors — suicidal ideation, homicidal ideation, psychotic symptoms — with specificity. Note what the client reported, how you assessed risk, and what actions you took. For example, “Client endorsed passive thoughts of suicide without plan or intent. Denied current suicidal or homicidal ideation. Safety plan reviewed and discussed.”
Consider Cultural Context
A client’s behavior and communication are shaped by cultural background, language, and life experience. What appears as restricted affect or guardedness may be culturally normative or trauma-informed. Ask clarifying questions and avoid diagnostic assumptions based solely on presentation.
Be Concise But Thorough
A well-organized MSE doesn't need to be lengthy, but it should touch on each major domain. Structured subheadings and consistent terminology help keep notes readable while ensuring all essential observations are captured.
Using ICANotes to Document Mental Status Exams
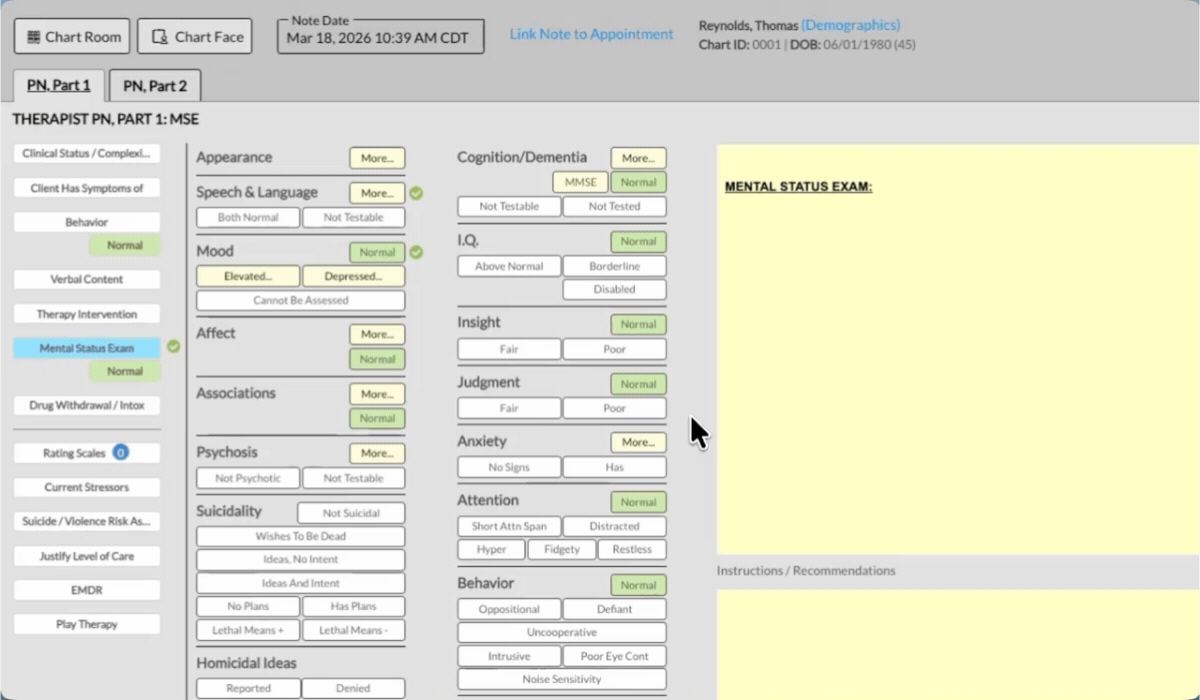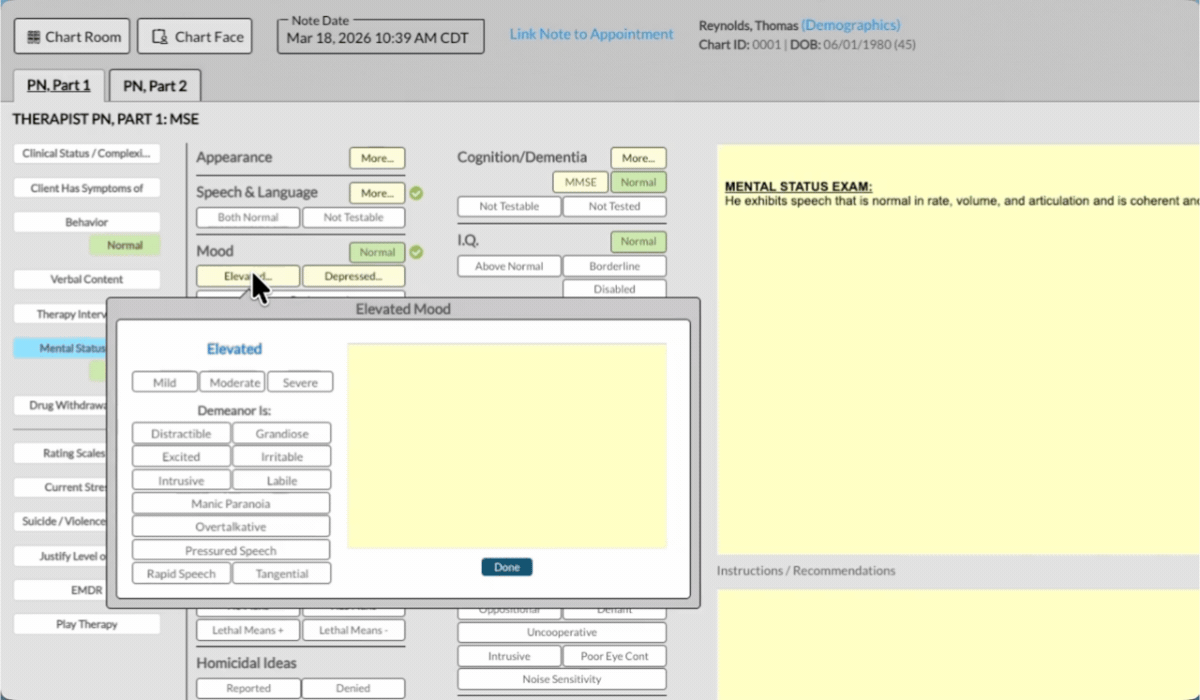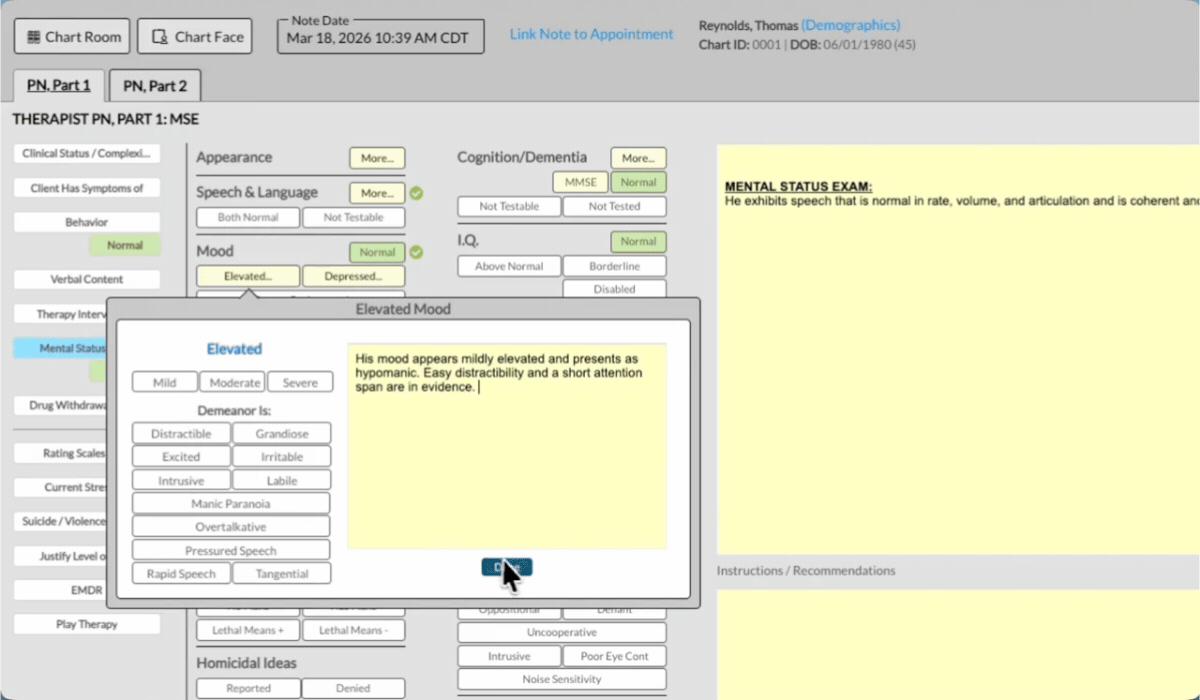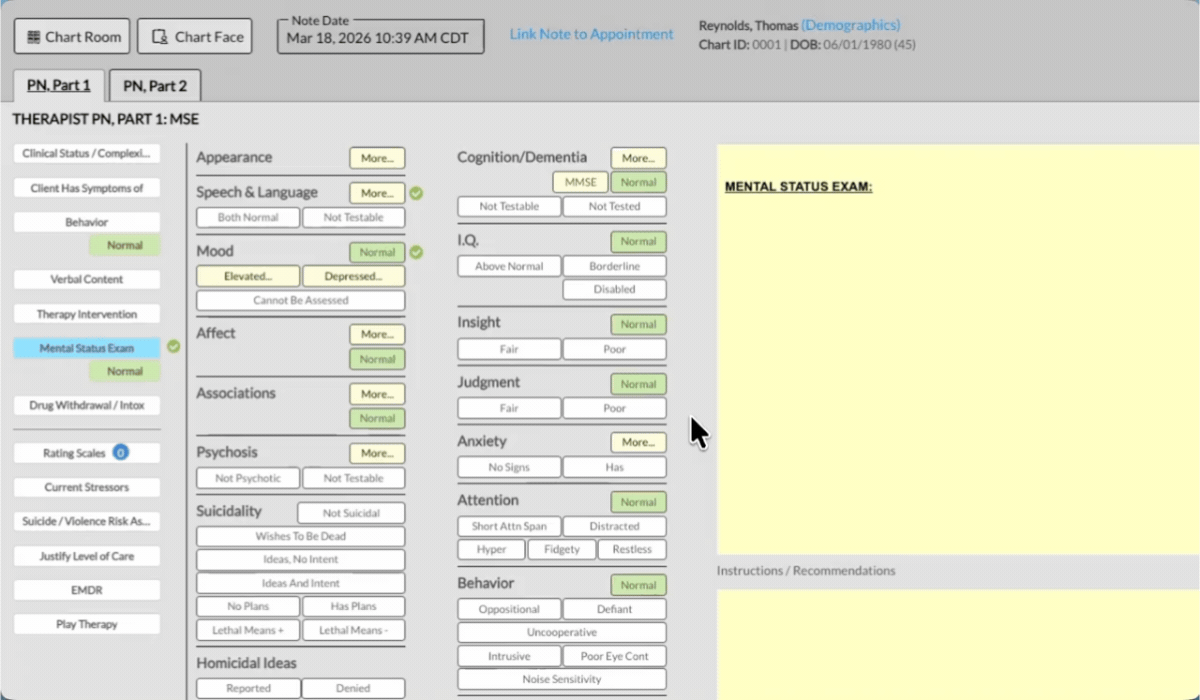
ICANotes makes mental status exam documentation fast and accurate with built-in tools designed specifically for behavioral health clinicians.
Pre-Built MSE Template: Choose from clinical descriptors for appearance, mood, cognition, and more — no typing required.
Instant Narrative Generation: Selections are automatically converted into a complete, professional MSE note.
Customizable Format: Add, remove, or adjust sections to fit your workflow and specialty.
Integrated and Secure: Document directly in your EHR with HIPAA-compliant data protection.
Start your free trial or book a demo today and simplify your MSE documentation with ICANotes.
Start Your Free Trial of ICANotes
Accurate and efficient documentation is essential for delivering quality behavioral health care. ICANotes simplifies the process with a clinically robust EHR software designed specifically for mental health professionals.
Our intuitive system comes preloaded with comprehensive templates for every setting and discipline, allowing you to create:
✅ Discharge summaries
✅ Group therapy notes
✅ Initial assessments
✅ Progress notes
✅ Treatment plans
Experience the EHR that thinks like a clinician. Try ICANotes free for 30 days, no credit card required!
Frequently Asked Questions About Mental Status Exams
What is a mini mental status exam?
The Mini-Mental State Examination (MMSE) is a brief, standardized 30-point screening tool used to assess cognitive functioning. It measures orientation, attention, memory, language, and basic visuospatial skills. Unlike the full MSE, which covers behavioral and emotional functioning, the MMSE focuses specifically on cognition and provides a scored result. It can be completed in about 5 to 10 minutes and is often used alongside the MSE for a complete clinical picture.
When are mental status exams performed?
Mental status exams are conducted at intake, during routine follow-up visits, following significant clinical events such as hospitalization or medication changes, and any time a change in behavior, mood, or cognition is observed. They provide a snapshot of current functioning and support continuity of care.
Who uses mental status exams?
MSEs are used by psychiatrists, psychologists, licensed therapists and counselors, psychiatric nurse practitioners, primary care physicians, neurologists, and emergency medicine providers. While originally developed for psychiatry, the MSE is now a standard documentation tool across behavioral health and many medical specialties.
What are the most common mistakes made during an MSE?
Common errors include confusing mood with affect, overlooking subtle safety signals, using vague or subjective language, relying too heavily on template autofill, and failing to consider cultural or developmental context. A structured, domain-by-domain approach helps ensure accuracy and completeness.
How do you assess thought process vs. thought content in an MSE?
Thought process is how a client thinks — the form, flow, and organization of thinking, evaluated through the structure of their speech. Thought content is what they think about — the actual ideas, beliefs, and preoccupations. Both must be assessed and documented separately. For example, a client may have an organized (goal-directed) thought process while expressing delusional thought content.
Read the full guide with examples for assessing thought process and content
What are some validated tools or scales for mental status assessment?
In addition to the standard Mental Status Examination (MSE), behavioral health professionals often use validated tools like the MMSE, MoCA, SLUMS, and Clock Drawing Test to assess cognitive functioning more objectively. These instruments help identify memory loss, executive dysfunction, and early signs of dementia, particularly in older adults or clients with neurocognitive concerns. Choosing the right tool depends on the clinical setting, client profile, and the purpose of the assessment.
View the full guide to validated mental status assessment tools
How do you adapt the MSE for patients with language barriers or low literacy?
To ensure accurate and culturally sensitive mental health assessment, clinicians must adapt the MSE for clients with language barriers or low literacy. This includes using trained medical interpreters, simplifying language-based tasks, relying more on behavioral observation, and selecting appropriate tools that minimize verbal or reading demands. Clear documentation of any adaptations is essential for clinical accuracy.
Read the full guide on adapting the MSE for language and literacy barriers
What are red flags in an MSE that require urgent intervention?
Red flags in the MSE—such as suicidal or homicidal ideation with intent, command hallucinations, severe psychosis, or grave impairment in judgment—indicate acute safety risks and require immediate clinical action. These findings may necessitate hospitalization, crisis intervention, or emergency services to protect the client and others. Prompt recognition, response, and clear documentation are essential for both clinical care and legal accountability.
Read the full guide to MSE red flags and emergency intervention protocols
What is MSE in psychology vs. psychiatry?
In both psychology and psychiatry, the MSE is a structured assessment of a client's current mental functioning. In psychiatry, it is used at nearly every encounter to monitor psychiatric symptoms, medication response, and safety risk. In psychology, it is more commonly used during intake evaluations and neuropsychological assessments. The domains assessed are the same across both disciplines.
Recent Posts
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







