Insurance Contract Negotiation for Mental Health Providers: When to Negotiate Better Reimbursement Rates—and When to Walk Away
Low-paying insurance contracts can quietly drain a mental health practice through inadequate reimbursement, excessive administrative burden, and rising denial rates. This guide helps therapists, psychologists, and behavioral health practice owners evaluate mental health reimbursement rates, assess payer mix objectively, and decide when insurance contract negotiation makes sense — and when walking away is the healthier business decision. You’ll learn how to calculate your true cost per session, identify red flags in low-value payer relationships, negotiate from a position of data and leverage, and transition away from unsustainable contracts ethically without compromising patient care or practice stability.

Last Updated: February 23, 2026


What You'll Learn
- How mental health reimbursement rates vary across payers and how to tell when a contract is paying below your true cost of care
- How to evaluate payer mix using revenue, reimbursement per visit, and administrative burden (not just patient volume)
- The hidden cost of denials, prior authorizations, and delayed payments — and how administrative friction erodes profitability
- Red flags that signal when a payer relationship should be renegotiated or reconsidered
- A practical, data-driven framework for insurance contract negotiation (including what to ask for and when to walk away)
- How to ethically transition away from low-paying payers while protecting patients, staff, and practice sustainability
Contents
- Understanding Mental Health Reimbursement Rates
- The Money Trail — How Payer Mix Shapes Your Reality
- Administrative Burden — The Cost You Don't See on the Fee Schedule
- Red Flags That It's Time to Reconsider a Payer
- How to Evaluate a Payer Objectively
- Ethical Tension: Access, Equity, and Boundaries
- Insurance Contract Negotiation: Your Step-by-Step Strategy Before Walking Away
- When Insurance Contract Negotation Fails — Moving to Termination
- How to Fire a Payer Without Burning Down Your Practice
- FAQs: Low Reimbursement, Firing a Payer, and Practice Survival
You can love your patients and still refuse to subsidize their insurance company. That tension is where a lot of good clinicians quietly burn out and a lot of good practices slowly bleed out. You do everything right clinically and operationally, but a few payer contracts keep dragging your revenue, your schedule, and your nervous system into the red.
This isn’t about being greedy. It’s about refusing to build a mission-driven practice on a foundation of bad math and worse behavior. The art is knowing when a payer is “annoying but workable,” and when it’s time to say: We’re done here.
This article will walk you through how to analyze mental health reimbursement rates, approach insurance contract negotiation strategically, and know when it’s time to end contracts that are quietly killing your practice.
Why Some Payers Are Quietly Killing Your Practice
Underpayment vs. Exhaustion — The Two Ways Payers Drain Practices
Not all low-paying contracts are created equal. A payer can hurt you in two ways:
- They underpay you (below what it costs to deliver care).
- They exhaust you (prior auth, denials, eligibility issues, payment delays, clawbacks).
In behavioral health, administrative burden often matters just as much as the reimbursement rate — especially for solo and small practices without dedicated billing teams. A low rate might be survivable if everything else is smooth. But low pay + high friction becomes a structural threat.
Why Behavioral Health Gets Hit Harder Than Other Specialties
On the hospital side, payer behavior scales into crisis: analyses of inpatient behavioral health services show reimbursement can sit materially below the cost of providing care while denials and utilization management requirements rise. If large systems with scale struggle under those dynamics, outpatient clinics with thinner margins feel the squeeze faster.
Understanding Mental Health Reimbursement Rates
Typical Reimbursement Ranges by Payer Type
Mental health reimbursement rates vary significantly by payer, region, and contract terms. While exact rates differ, national and state-level analyses show consistent patterns across payer categories for standard outpatient psychotherapy services (e.g., CPT 90834–90837).
Common reimbursement ranges include:
- Government payers (Medicaid and Medicare):
Medicaid reimbursement often falls at the low end of the spectrum, frequently ranging from approximately $60–$90 per session, depending on state and program. Medicare rates are typically higher and more predictable, often clustering around $90–$120 for 45–60 minute outpatient psychotherapy services. - Commercial insurance (mid-tier plans):
Many commercial plans reimburse in the range of $80–$100 per session, though these rates are often paired with higher administrative burden, including prior authorization requirements and higher denial rates. - Commercial insurance (premium or high-performing networks):
Higher-tier commercial plans and employer-sponsored networks may reimburse $110–$160 or more per session, particularly in higher cost-of-living markets or for practices serving in-demand specialties. - Self-pay / cash rates:
Self-pay rates in private practice commonly range from $150–$250+ per session, with variation driven by geography, clinician experience, specialization, and local market demand.
What matters most isn’t the exact dollar amount — it’s the spread. Practices often discover that two payers reimburse dramatically different amounts for the same CPT code, with gaps of $40–$60 per session not uncommon. Over hundreds or thousands of visits per year, those differences determine whether a practice has margin to reinvest — or quietly bleeds cash.
The Reimbursement Gap — Why Rates Lag
Mental health reimbursement rates lag behind both the cost of care and reimbursement in other medical specialties for structural reasons — not because the care is less valuable, but because the payment system has evolved to underprice it.
Three evidence-backed forces drive this gap:
1. Parity laws exist, but enforcement is inconsistent
Despite federal and state mental health parity laws, multiple analyses show that behavioral health services are still reimbursed well below their actual cost. A 2024 analysis of inpatient behavioral health services found that reimbursement averaged roughly one-third below the cost of delivering care, a gap that does not appear at the same scale in most medical specialties.
Parity violations often show up not only in fee schedules, but in utilization management: more frequent prior authorizations, narrower medical necessity definitions, and higher denial rates for the same diagnoses and services.
2. Administrative burden functions as a hidden reimbursement cut
Reimbursement rates alone understate the true financial impact of insurance contracts in behavioral health. Research consistently shows that behavioral health providers face disproportionately high administrative friction, which effectively reduces real reimbursement even further.
A 2024 CAQH analysis found that behavioral health providers spend significantly more time per transaction than general medical providers:
- Eligibility verification often takes 24 minutes per patient, roughly three times longer than for other specialties.
- Prior authorizations for behavioral health services average 25 minutes per request, compared to about 14 minutes for general medical care.
That time translates directly into labor cost. When clinicians or staff spend hours each week navigating one payer’s rules, the “headline” reimbursement rate no longer reflects what the practice actually earns per session.
3. Market power and mission-driven acceptance suppress rates
Mental health care is delivered largely by solo clinicians and small practices, many of whom accept low reimbursement out of ethical commitment or concern for access. Payers have learned that this dynamic allows them to hold rates down while increasing administrative controls.
Ironically, this occurs alongside widespread provider shortages. In a normal market, scarcity drives prices up. In behavioral health, it often does not — because fragmented providers lack negotiating leverage and because access gaps are absorbed by clinician burnout rather than payer accountability.
Why This Gap Matters Operationally
The reimbursement gap is not an abstract policy problem. It directly shapes:
- whether practices can hire and retain staff
- whether clinicians limit caseloads or panel size
- whether services are shortened, delayed, or discontinued
When reimbursement falls below the cost of care — after accounting for administrative burden — practices are forced to subsidize insurance contracts with unpaid labor. Over time, that model collapses.
This is why evaluating reimbursement rates without accounting for friction leads many practices to underestimate how damaging a contract truly is.
What Reimbursement Should Be: Your Floor Is Your Cost
Calculate Your Fully Loaded Cost per Session
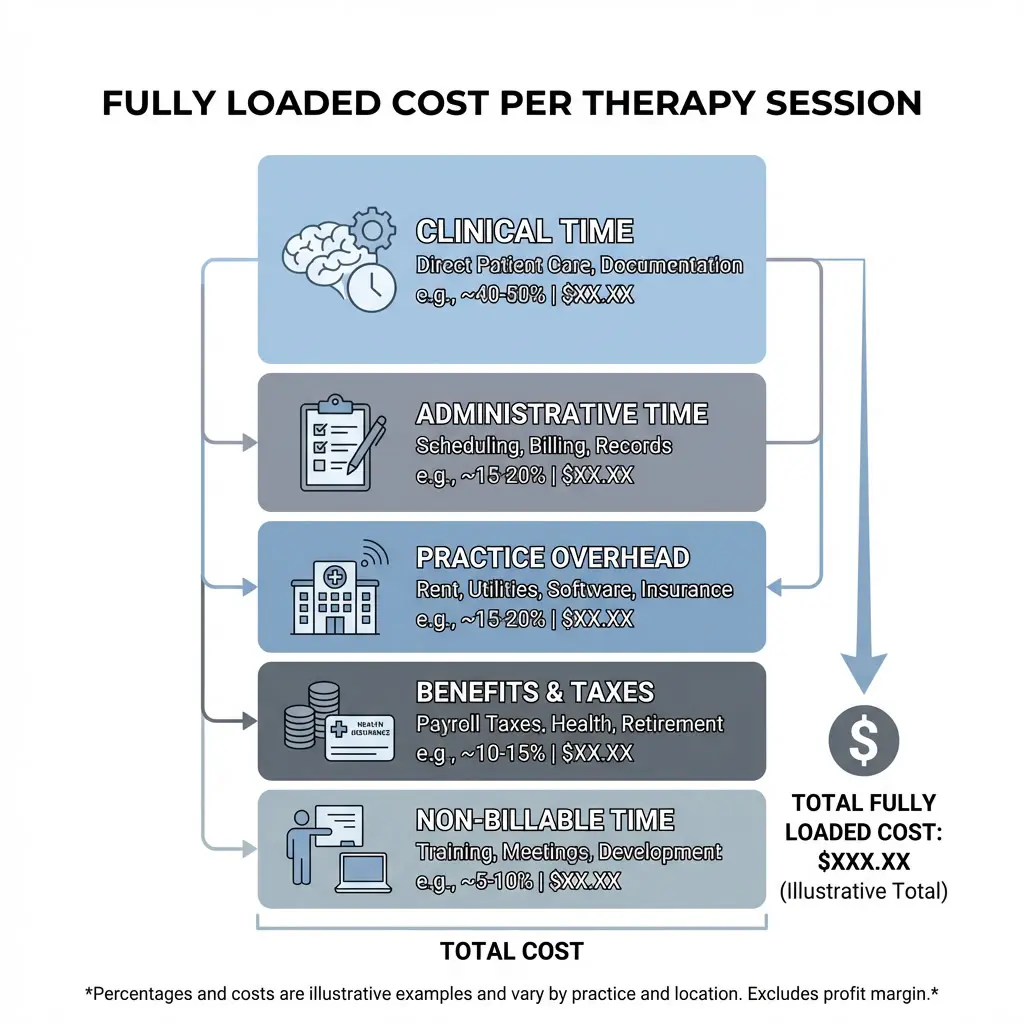
To determine if your mental health reimbursement rates are sustainable, calculate your fully loaded cost per session:
- Clinical time (session + documentation)
- Administrative time (scheduling, billing follow-up, prior auth)
- Overhead (rent, utilities, insurance, software, supervision, supplies)
- Payroll taxes/benefits (if applicable)
- Non-billable time (no-shows, consults, care coordination, training)
National data suggest that private‑pay psychotherapy sessions average around $140–$150 per hour, and practice overhead commonly consumes 30–50%+ of revenue. When you factor in rent, staffing, benefits, and non‑billable time, many outpatient mental health practices effectively spend on the order of $75–$110 per clinical hour to deliver care. If your reimbursement rate is at or below your cost, you're literally paying to see patients.
“If reimbursement does not cover clinician compensation, overhead, administrative labor, and a reasonable margin for reinvestment, that contract is operating at a loss.”
— Gabrielle Juliano-Villani, LCSW | GJV Consulting and Training LLC ( medicareconsultingfortherapists.com )
Use Medicare as a Baseline Benchmark
Medicare isn’t always generous, but it’s transparent and consistent. If a commercial payer is paying you less than Medicare for comparable services, that’s a clear signal the contract is undervaluing your work.
The Spillover Effect: Low Rates Anchor the Market Down
Economic research shows that reimbursement rates do not exist in isolation. Public payer payment decisions, especially Medicare, tend to set informal benchmarks that ripple across the private insurance market.
A landmark economic analysis found that for every $1.00 reduction in Medicare payment rates, private payer reimbursement decreased by approximately $1.12 to $1.16. Rather than compensating for public payer cuts, commercial insurers often follow them, amplifying the overall decline in reimbursement.
This dynamic has important implications for mental health providers. When clinicians accept contracts that pay below sustainable benchmarks — particularly below Medicare rates — they may unintentionally reinforce downward pricing pressure across the market. Over time, this spillover effect contributes to chronically suppressed reimbursement, even as demand for mental health services continues to rise.
The takeaway is not that Medicare rates are “too low” or “too high,” but that they are powerful anchors. When reimbursement falls below these anchors, the consequences extend beyond a single contract and shape the financial viability of mental health care delivery more broadly.
“If a contract requires you to sacrifice clinician wellbeing or client outcomes to survive, that isn’t an access solution — it’s a slow leak.”
— Matt Grammer, LPCC-S, Owner | Counseling Now
The Money Trail — How Payer Mix Shapes Your Reality
Why Patient Volume Is a Trap Metric
A payer can represent 15% of your caseload and only 5% of your revenue. Volume is emotionally loud; revenue is operational truth.
A Simple Payer Mix Review (Quarterly Minimum)
Payer mix analysis — looking at what percentage of your revenue comes from each payer and at what average rate — is basic, but most small practices only do it annually, if at all. At least quarterly, perform these steps:
- Calculate payer mix by revenue, not just by patient count.
- Compare average reimbursement per visit for your top CPT codes across payers.
- Look at denial and adjustment rates by payer, not just overall.
- Assess average days in A/R by payer
- Evaluate whether reimbursement aligns with your cost per visit, including clinical and admin time (admin “touches” per claim: calls, resubmissions, appeals—rough counts still help)
Your Payer Mix Can Make You Feel “Bad at Business” When You’re Not
If your practice feels like it’s working harder and earning less, payer mix is often the culprit. The issue isn’t effort. It’s the math of who you’re serving, at what rate, and with how much friction attached.
Administrative Burden — The Cost You Don’t See on the Fee Schedule
Denials, Prior Auth, and Payment Delays Are a Financial Leak
Every extra hour your team spends chasing one payer is an hour not spent on higher-yield work: patient care, scheduling fill, clean claims, or improving patient experience.
Administrative friction reduces your effective reimbursement rate. A “decent” fee schedule can still be a bad contract if it drives disproportionate time cost.
Why Admin Friction Drives Burnout and Panel Closures
In mental health, administrative burden isn’t just annoying — it influences whether clinicians accept insurance at all. When low pay and high friction combine, providers eventually respond by tightening panels, limiting services, or leaving networks entirely.
Denials and Payment Delays Are an Escalating Operational Risk
Administrative burden isn’t static, it has been intensifying. In 2023, claims denials by some commercial payers increased by more than 20%, while the time required to receive payment on claims rose by nearly 20% as well. These trends represent a direct hit to both cash flow and staff morale, compounding the strain created by already low reimbursement rates.
For mental health practices operating on thin margins, delayed payments can disrupt payroll timing, increase reliance on credit, and force staff to spend more time on follow-up and appeals. Over time, this escalation turns administrative friction from an inconvenience into a material financial risk — and one that disproportionately affects practices with limited billing infrastructure.
Red Flags That It's Time to Reconsider a Payer
“Firing” a payer is serious. But there are clear warning signs that you’re no longer in a healthy business relationship. Think of these as your clinical criteria for a toxic contract. Here are key red flags, grounded in what we know about payer mix and admin burden.
Financial Red Flags
- Rates consistently below your benchmarks (and/or below Medicare)
- Reimbursement below your fully loaded cost per session
- The payer is a small share of revenue but consumes big operational bandwidth
Operational Red Flags
- Denial rates materially higher than your baseline
- Chronic payment delays relative to other payers
- Frequent retroactive denials, recoupments, or shifting “medical necessity” rules
- Heavy prior auth requirements with little clinical logic
The Payer Performance Grid
Finance and strategy guides for mental health practices often summarize payer performance using a simple grid. The goal is not to label payers as “good” or “bad,” but to evaluate the relationship objectively based on both financial return and operational effort.
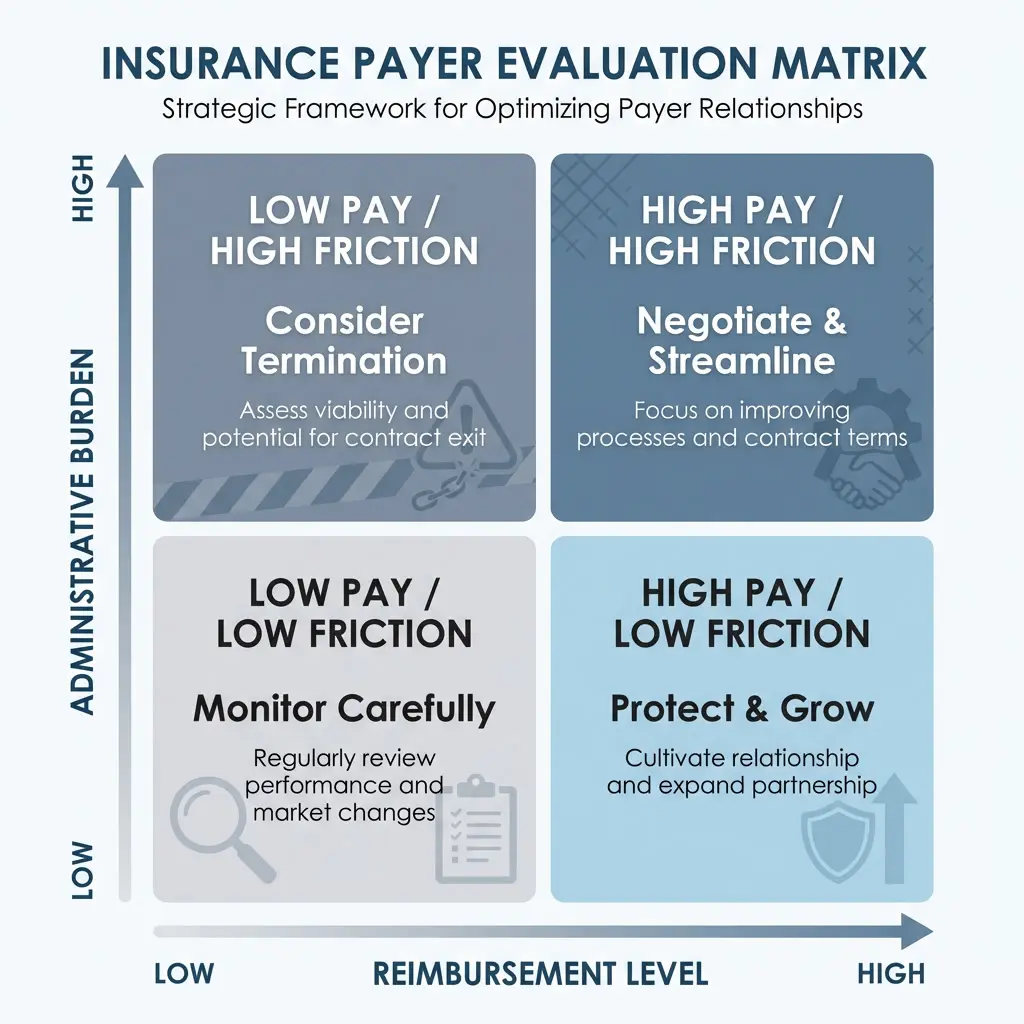
A payer performance grid typically looks like this:
- High pay / low friction: protect and grow
- High pay / high friction: negotiate + streamline
- Low pay / low friction: monitor (volume may still matter)
- Low pay / high friction: top candidate for termination
If a payer lives in that bottom‑right corner and has resisted prior attempts to improve the relationship, you’re not being dramatic by considering a breakup. You’re being a responsible steward of your practice. Sustainable care delivery requires sustainable contracts.
Run the Numbers Before You Make the Call
Download the Payer Performance Scorecard and the “Should I Fire This Payer?” Decision Checklist to evaluate reimbursement, denial trends, administrative burden, and revenue impact with clarity — not emotion.
These tools help you move from frustration to facts before renegotiating or terminating a contract.
How to Evaluate a Payer Objectively (Not Just Emotionally)
You may feel done with a payer long before the numbers prove it. Feelings are an early warning system — but don’t fire a payer on vibes alone. Start with a simple, repeatable analysis that mirrors what larger systems do.
How to Use a Repeatable Payer Scorecard (Step-by-Step)
The goal of a payer scorecard is not perfection. It’s consistency. You’re trying to answer one question:
Is this payer pulling its weight — or quietly draining my practice?
You can do this in a simple spreadsheet and update it quarterly.
Step 1: Rate vs. Benchmarks
What you’re measuring: How this payer’s rates compare to reasonable alternatives.
How to calculate it:
List your top 3–5 CPT codes (e.g., 90834, 90837, intakes).
For each CPT:
- Write the average amount actually paid by this payer (not the fee schedule).
- Compare it to:
■ Medicare (local rate)
■ Your highest-paying commercial plan
■ Your estimated break-even rate
Score It
- ● Above Medicare and near top commercial rates
- ● Near Medicare but below top commercial
- ● Below Medicare or below your cost per session
Why It Matters
If a payer is paying below Medicare, that’s rarely sustainable long-term — especially when paired with administrative friction, denial work, and delayed payments.
Step 2: Cost-to-Serve Estimate (Admin Time × Loaded Wage)
What you’re measuring: How much staff time this payer actually consumes.
How to calculate it:
Estimate average admin time per claim for this payer:
- Eligibility checks
- Prior authorizations
- Claim resubmissions
- Appeals and follow-up calls
Multiply:
- Estimated minutes per claim × staff hourly cost (wages + benefits)
Example:
If a biller earns ~$28/hour fully loaded and spends ~20 minutes per claim:
- Cost per claim ≈ $9–10
Multiply by volume and suddenly a “decent” rate isn’t so decent.
Score It
- ● Minimal follow-up, mostly clean claims
- ● Occasional rework
- ● Frequent manual work, calls, or appeals
Why It Matters
Administrative burden acts like a silent pay cut that never shows up on the fee schedule.
Step 3: Denials + Rework Rate
What you’re measuring: How often this payer creates avoidable extra work.
How to calculate it:
Look at a 90-day period:
- Total claims submitted to this payer
- Number denied, downcoded, or adjusted
Divide to get a rough percentage
- Compare it to:
■ Your practice average
■ Your best-performing payer
Score It
- ● At or below practice average
- ● Slightly above average
- ● Consistently higher than other payers
Why It Matters
High denial rates often reflect payer behavior, not documentation quality — especially when other payers are paying cleanly.
Step 4: Days in Accounts Receivable (A/R)
What you’re measuring: How long this payer holds your money.
How to calculate it:
- Pull average days from submission to payment for each payer.
- Compare across payers.
Score It
- ● Pays within 15–25 days
- ● 30–40 days
- ● 45+ days or unpredictable timing
Why It Matters
Slow payers create:
- • Cash-flow stress
- • Payroll timing issues
- • Increased follow-up work
Even “eventual” payment has a cost.
Step 5: Revenue Share
What you’re measuring: How much this payer actually contributes to your business.
How to calculate it:
- Total revenue from this payer ÷ total practice revenue
- Compare that percentage to:
Percentage of admin time
Percentage of billing headaches
Score It
- ● High revenue share, reasonable effort
- ● Moderate revenue, manageable effort
- ● Low revenue share, high operational drag
Why It Matters
A payer that brings in 5% of revenue but 25% of your billing pain is a prime candidate for renegotiation or exit.
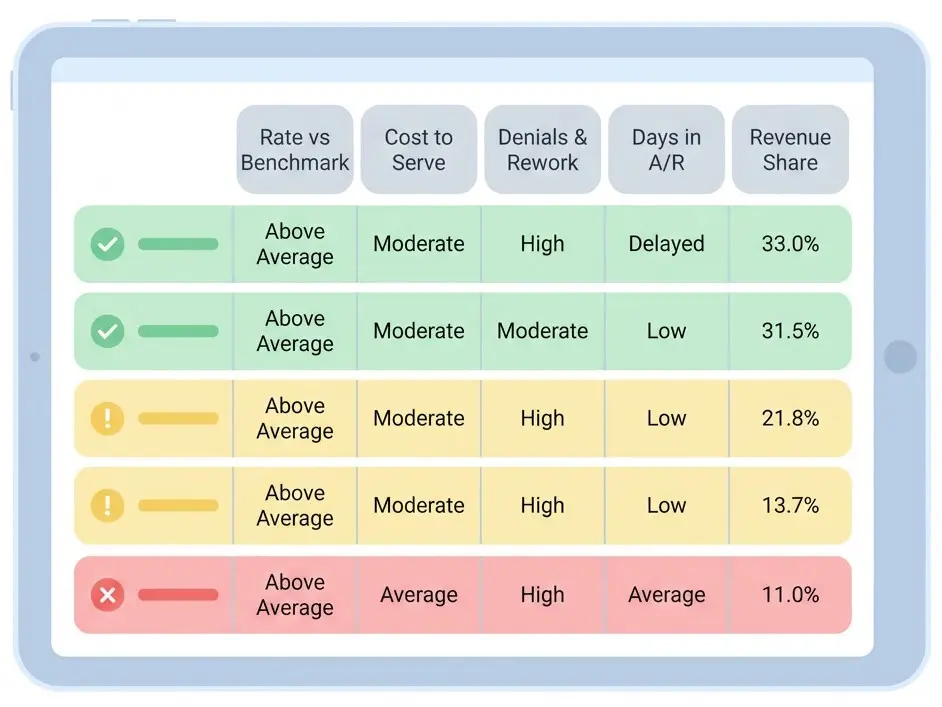
Putting It All Together: The Scorecard View
You don't need fancy math. Just line items and color-coding.
The Scorecard View
Patterns matter more than any single score.
A payer with multiple ● ratings is not a “gut feeling” problem — it’s a data problem.
How Clinicians Should Use This Scorecard
- Quarterly review: spot problems before burnout sets in
- Negotiation prep: bring this data to provider relations
- Ethical clarity: distinguish discomfort from unsustainability
- Decision-making: set objective thresholds for renegotiation or termination
If the same payer scores poorly quarter after quarter — and refuses to improve — walking away isn’t emotional. It’s responsible.
Ask the One Question That Clarifies Everything
If I stopped taking this payer tomorrow, what would happen to my bottom line — and what would happen to my workload?
Often the fear of change is bigger than the financial reality.
Ethical Tension: Access, Equity, and Boundaries
If you’re a conscience‑driven clinician, this is the part that keeps you up at night. Dropping a low‑paying payer can feel like abandoning your patients who rely on that coverage. And it’s true: insurance churn and instability are real. National data indicate that 15–20% of insured individuals experience coverage disruptions or plan changes each year, with many cycling back to previous insurers over a few years. Patients get stuck in systems they didn’t design.
But here’s the hard truth: you cannot rescue a broken insurance market by martyring your practice. Studies of hospital and physician behavior show that when reimbursement falls and financial pressure rises, access to low‑paying coverage often shrinks anyway, just in more chaotic ways—closed panels, longer waits, fewer services.
“When a payer consistently underpays and increases administrative demands, it forces practices to make unsustainable tradeoffs. Boundaries in business protect the longevity of care.”
— Vickery Rendall, LCSW, Owner | Paper Birch Therapy, PLLC

A more honest approach is:
- Be transparent with patients about changes.
- Offer alternatives where you can (sliding scale slots, group visits, time‑limited continuation).
- Use your data and your story to advocate for better reimbursement and simpler policies at the policy or association level.
Boundaries are not a lack of compassion. They are what make sustainable compassion possible.
Insurance Contract Negotiation: Your Step-by-Step Strategy Before Walking Away
Before you terminate a low-paying contract, insurance contract negotiation should always be your first strategic move. Many providers assume payer contracts are non-negotiable, but that's rarely true — especially if you approach insurance contract negotiation with data, leverage, and a clear plan.
Contract-optimization frameworks emphasize running scenarios and approaching payers with evidence before deciding to terminate. The goal isn't just to get a "yes" — it's to determine whether the payer is willing to operate in good faith. If they refuse to engage or offer only token adjustments, you'll know termination is justified. If they come to the table, you may salvage the relationship on better terms.
Step 1: Build Your Negotiation Case With Hard Data
Successful insurance contract negotiation starts with evidence, not emotion. Payers respond to data that shows you are undervalued relative to market benchmarks and that their behavior is creating unsustainable conditions.
Gather these core data points before you contact provider relations:
- Your current reimbursement rates vs. benchmarks: Pull your top 5-10 CPT codes and compare what this payer pays versus Medicare, your highest-paying commercial contract, and published fair market rates for your region and specialty. If you're a mental health provider getting $65 per session while Medicare pays $80 and other commercial plans pay $95-110, document that gap.
- Denial and adjustment rates: Calculate what percentage of claims this payer denies, adjusts, or delays compared to your practice average. If their denial rate is 15% and your practice average is 4%, that's a measurable problem.
- Administrative burden metrics: Estimate how much staff time goes into this payer's claims, prior authorizations, and appeals. If your biller spends 5 hours a week just on this one contract, quantify that cost. Research shows behavioral health providers spend about 24-25 minutes per eligibility check and prior authorization when done manually — at roughly $14 per transaction. Multiply that by volume.
- Your role in local access: If you're in a shortage area or serve a unique population (e.g., trauma, child/adolescent, bilingual services), document it. Payer networks are under regulatory and public pressure to maintain adequate networks, especially in mental health.
- Days in accounts receivable: Track how long this payer takes to pay clean claims compared to others. If they're consistently 20-30 days slower, that's a cash-flow cost you can quantify.
Present this in a simple one-page summary: "Current state" vs. "What we need" with specific numbers.
Step 2: Understand Your Leverage (and Theirs)
Insurance contract negotiation is about leverage. Both sides have it; the question is who has more.
Your Leverage
- Provider shortages: Mental health and primary care shortages are well-documented. If you're in a shortage area, the payer may struggle to replace you without violating network adequacy standards.
- Patient loyalty: Long-term patients who would leave the plan to follow you create pressure on payer retention metrics.
- Unique services or expertise: Specialized training, languages, or populations served that are difficult to replace increase your negotiating position.
- Market alternatives: If you can afford to walk away — financially and ethically — you hold the strongest leverage of all.
Their Leverage
- Patient volume: If this payer represents 30–40% of your patient base, they know termination would significantly impact your revenue.
- Market saturation: If many other providers are willing to accept lower rates, the payer has less incentive to negotiate.
- Contractual lock-in: Long notice periods or auto-renewal clauses can limit your flexibility and delay strategic decisions.
Before entering insurance contract negotiation, honestly assess where you stand. If you have minimal leverage, you may still negotiate, but your expectations should be realistic.
Step 3: Approach the Payer with a Clear, Professional Proposal
Payers get angry calls from frustrated providers daily. To stand out in insurance contract negotiation, be calm, data-driven, and solution-oriented.
Your opening message (email or formal letter to provider relations):
Request for Contract Review and Rate Adjustment
Subject: Request for Contract Review and Rate Adjustment – [Your Practice Name] Dear [Provider Relations Contact], I am writing to request a formal review of our current contract and reimbursement rates. Our practice has been an in-network provider with [Payer Name] since [year], and we are committed to continuing to serve your members. However, our recent financial analysis has identified significant concerns that are affecting our ability to maintain this relationship sustainably. Specifically: • Our current reimbursement rate for [CPT code] is $[X], which is [Y]% below Medicare and [Z]% below our regional commercial benchmarks. • We experience a denial rate of [X]% with your plan, compared to [Y]% across our other payers, resulting in substantial administrative costs. • Payment turnaround averages [X] days, compared to [Y] days for our other contracts, creating cash-flow challenges. • [If applicable: As one of only [X] providers in [specialty/region], our practice plays a critical role in your network adequacy for [population/service]. We are eager to continue serving your members, but we need contract terms that reflect the true cost and value of the care we provide.] I have attached a brief summary of our analysis and a proposal for adjusted rates. I would welcome the opportunity to discuss this with you at your earliest convenience. Thank you for your consideration.
Tip: Replace bracketed fields with your data, then attach a one-page scorecard summary (rates vs benchmarks, denials, days in A/R, and cost-to-serve).
What to ask for in insurance contract negotiation:
Be specific. Vague requests like "we need better rates" go nowhere. Instead:
- Rate increase: "We are requesting an adjustment to $[specific amount] for CPT codes [list], which represents [X]% increase and aligns with [Medicare/commercial benchmark]."
- Administrative relief: "We request elimination of prior authorization for [specific services], or implementation of auto-approval for patients with established diagnoses."
- Payment terms: "We request payment of clean claims within 15 business days, consistent with state prompt-pay laws."
Offer trade-offs where appropriate. For example: "We are willing to accept a [smaller rate increase] in exchange for [streamlined prior auth process]."
Step 4: Recognize Good Faith vs. Stonewalling
Real insurance contract negotiation involves back-and-forth. The payer may counteroffer, ask for data, or stall. Set a timeline and decision point for yourself.
Green Flags in Negotiation
- Timely engagement: Payer schedules a call or meeting within 2–3 weeks.
- Data curiosity: Asks clarifying questions about your analysis.
- Meaningful counteroffer: Proposes an adjustment, even if below your initial ask.
- Collaborative tone: Acknowledges the issue and shows willingness to problem-solve.
Red Flags in Negotiation
- Silence: No response after multiple follow-ups.
- Dismissive language: “These are our standard rates — take it or leave it.”
- Token acknowledgment: Recognizes the problem but offers no meaningful change.
- Symbolic increase: Counters with a 1–2% bump when you’ve documented a 30–40% gap.
If the payer engages in good faith and moves toward a sustainable middle ground, you've succeeded. If they stonewall or lowball you, you have your answer: this isn't a partnership, it's exploitation.
Step 5: Document Everything and Set a Decision Deadline
Keep records of all insurance contract negotiation communications — emails, calls, offers, counteroffers. If you do eventually terminate, this paper trail shows you acted professionally and in good faith.
Set an internal deadline: "If we don't have a signed agreement by [date], we will begin the termination process." Don't let negotiation drag on indefinitely while your practice continues to hemorrhage money.
When Insurance Contract Negotiation Fails — Moving to Termination
If negotiation doesn't yield sustainable terms, you've done your due diligence. Termination isn't failure — it's a strategic boundary decision backed by data.
The best insurance contract negotiation outcomes aren't always rate increases. Sometimes the best outcome is clarity: knowing that you tried, the payer refused, and you're now justified in moving on.
One final note: even after you terminate, some payers will suddenly "find" budget for a rate increase once they realize you're serious. If that happens, re-evaluate, but be wary of one-time appeasement that doesn't address systemic issues. Sustainable insurance contract negotiation requires structural change, not just a temporary bump.
How to Fire a Payer Without Burning Down Your Practice
Once the data and your gut agree it’s time to move on, the “art” is in the execution. This is where your inner Brian Tracy (clear plan, disciplined follow‑through) needs to lead.
Evidence‑based payer‑mix guidance and standard revenue‑cycle best practices suggest a structured approach:
-
Review the contract.
-
Confirm termination clauses, notice requirements (often 90–180 days), and any communication obligations.
-
Note effective dates and whether you’re obligated to complete episodes of care already authorized.
-
-
Model the impact.
-
Use at least 6–12 months of data to estimate lost revenue, freed staff time, and potential to backfill with higher‑paying payers or self‑pay.
-
Remember that some evidence shows payer shifts and coverage changes are common; patients may switch plans or follow you into different payment arrangements over time.
-
-
Negotiate before you walk.
-
Present your data to provider relations: low rates versus benchmarks, high denial or delay rates, and your role in access (e.g., local shortage of behavioral health clinicians).
-
Many payer‑optimization guides specifically recommend building scenarios for renegotiation before termination.
-
-
Plan your patient communication.
-
Draft clear, compassionate notices describing what’s changing, when, and what options patients have.
-
Offer help with superbills, out‑of‑network claims, or transitional visits when feasible.
-
-
Align your schedule and marketing.
-
Intentionally open more slots for higher‑paying payers or self‑pay services.
-
Consider adding group services, intensives, or consults that align better with sustainable reimbursement.
-
-
Monitor and adjust.
-
Re‑run your payer mix and revenue analysis 3–6 months after the change.
-
If you’re like many organizations that strategically adjust payer mix, you may see improved financial stability and more margin for mission.
-
Handled well, firing a payer is not a meltdown — it’s a strategic boundary decision.
Frequently Asked Questions: Low Reimbursement, Firing a Payer, and Practice Survival
The Infrastructure Behind Sustainable Negotiation
Insurance contract negotiation is strongest when it’s backed by clean, defensible data.
That means:
- Clear documentation that supports medical necessity
- Visibility into denial patterns by payer
- Reliable tracking of reimbursement by CPT code
- Insight into days in A/R and billing lag
- Confidence that your notes align with payer requirements
Without that visibility, negotiation becomes emotional. With it, negotiation becomes strategic.
ICANotes was built specifically for behavioral health practices that need documentation and billing alignment to support sustainable reimbursement. From menu-driven clinical content to integrated billing workflows, the platform helps practices:
- Strengthen documentation defensibility
- Reduce preventable denials
- Monitor reimbursement trends
- Track payer performance over time
When your documentation, billing, and reporting systems are aligned, payer conversations shift from opinion to evidence.
And evidence changes leverage.
Want clearer visibility into your reimbursement trends and denial patterns?
See how ICANotes supports documentation integrity and revenue stability for behavioral health practices.
Explore ICANotes by booking a demo today.
Schedule a Demo Today!
Experience the most intuitive, clinically robust EHR designed for behavioral health professionals, built to streamline documentation, improve compliance, and enhance patient care.
- Complete Notes in Minutes - Purpose-built for behavioral health charting
- Always Audit-Ready – Structured documentation that meets payer requirements
- Keep Your Schedule Full – Automated reminders reduce costly no-shows
- Engage Clients Seamlessly – Secure portal for forms, messages, and payments
- HIPAA-Compliant Telehealth built into your workflow
Complete Notes in Minutes – Purpose-built for behavioral health charting
Always Audit-Ready – Structured documentation that meets payer requirements
Keep Your Schedule Full – Automated reminders reduce costly no-shows
Engage Clients Seamlessly – Secure portal for forms, messages, and payments
HIPAA-Compliant Telehealth built into your workflow
Related Posts
About the Author
Dr. October Boyles is a behavioral health expert and clinical leader with extensive expertise in nursing, compliance, and healthcare operations. With a Doctor of Nursing Practice (DNP) and advanced degrees in nursing, she specializes in evidence-based practices, EHR optimization, and improving outcomes in behavioral health settings. Dr. Boyles is passionate about empowering clinicians with the tools and strategies needed to deliver high-quality, patient-centered care.







