Blog > Treatment Strategies > 20 CBT Techniques with Real Examples for Clinicians
Cognitive Behavioral Therapy Techniques: 20 CBT Techniques with Real Examples
Explore 20 evidence-based cognitive behavioral therapy techniques used by clinicians to treat anxiety, depression, trauma, and related mental health conditions. This comprehensive CBT guide includes real therapy examples, therapist scripts, practical applications, behavioral and cognitive interventions, and downloadable CBT worksheets to support session planning, treatment implementation, and clinical documentation.

Last Updated: May 14, 2026


What You'll Learn
- The core principles behind cognitive behavioral therapy (CBT) and how the CBT triangle guides treatment
- 20 evidence-based CBT techniques clinicians use for anxiety, depression, trauma, avoidance, and low self-worth
- Real CBT examples and therapist-client dialogue snippets that demonstrate how techniques work in session
- When to use cognitive, behavioral, emotion-focused, and problem-solving CBT interventions
- How to choose the right CBT technique based on presenting symptoms and maintaining mechanisms
- Common mistakes clinicians make when implementing CBT — and how to avoid them
- Practical tools including thought records, behavioral activation strategies, exposure hierarchies, and behavioral experiments
- How CBT techniques can be adapted for anxiety disorders, depressive disorders, and trauma-focused treatment
- Ways to improve clinical workflow and documentation using structured CBT treatment planning and progress notes
- Where to download a free CBT techniques PDF toolkit with worksheets, therapist scripts, and decision-support tools
Contents
- What Is Cognitive Behavioral Therapy (CBT)?
- How CBT Works: The CBT Triangle Explained
- 20 Evidence-Based CBT Techniques with Real Examples
- CBT Examples in Practice: 3 Real Therapy Scenarios
- Cognitive Behavioral Therapy Techniques for Anxiety
- Cognitive Behavioral Therapy Techniques for Depression
- Trauma-Focused Cognitive Behavioral Therapy Techniques
- How to Choose the Right CBT Technique
- Common Mistakes When Using CBT Techniques
- Download a Free CBT Techniques PDF Toolkit
- How ICANotes Supports CBT Documentation
- Frequently Asked Questions About Cognitive Behavioral Therapy Techniques
20 Evidence-Based CBT Techniques with Real Examples
The techniques below are organized into four categories: cognitive, behavioral, emotion-focused, and problem-solving. Most CBT protocols draw from across these categories rather than relying on a single technique. As you read, consider which fit your client population and which fill gaps in your current practice.
Cognitive CBT Techniques
Cognitive CBT techniques help clients identify, evaluate, and respond to the thought patterns that contribute to emotional distress and unhelpful behaviors. These interventions target automatic thoughts, cognitive distortions, and deeper core beliefs that shape how clients interpret situations, relationships, and themselves. The techniques below form the foundation of cognitive restructuring and are commonly used to treat anxiety, depression, low self-esteem, perfectionism, and related mental health concerns.
1. Thought Records
Thought records are one of the foundational tools in cognitive behavioral therapy because they help clients slow down automatic reactions and examine thoughts more objectively. By organizing the situation, emotional response, evidence, and alternative perspectives in writing, clients can begin separating facts from assumptions and develop more balanced thinking patterns over time.
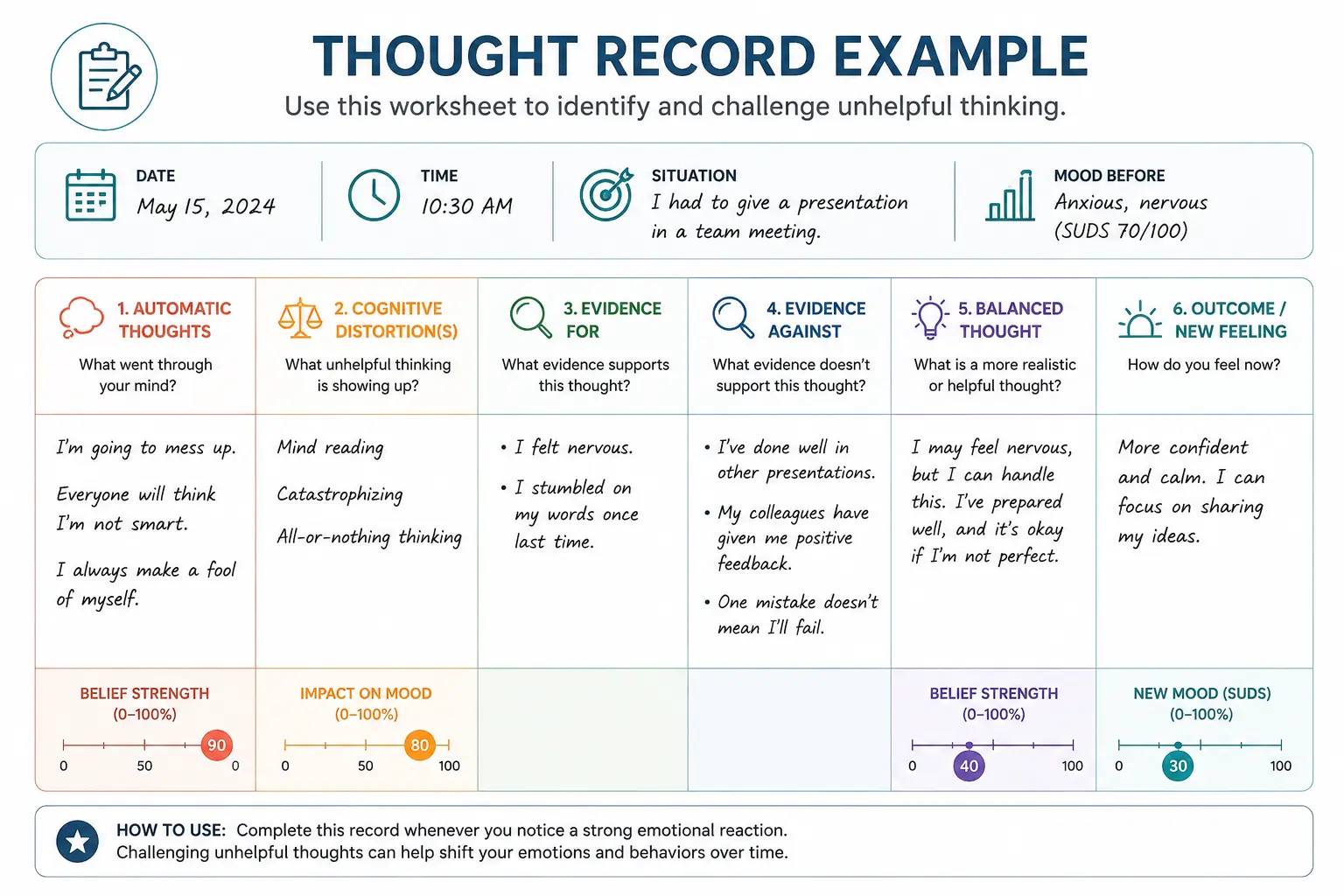
Over time, repeated thought-record practice helps clients build cognitive flexibility, reduce emotional reactivity, and recognize recurring thinking patterns that contribute to anxiety, depression, shame, and self-criticism.
2. Identifying Cognitive Distortions
- Catastrophizing — jumping to worst-case outcomes
- All-or-nothing thinking — viewing situations in extremes
- Mind reading — assuming you know what others are thinking
- Emotional reasoning — “I feel it, so it must be true”
- Personalization — taking responsibility for events outside your control
- “Should” statements — rigid rules about how you or others must behave
Learning to identify cognitive distortions helps clients recognize the predictable thinking patterns that intensify emotional distress and reinforce unhelpful behaviors. Naming these patterns creates psychological distance from automatic thoughts and opens the door to more balanced, flexible interpretations.

As clients become more skilled at spotting cognitive distortions in real time, they often develop greater self-awareness, improved emotional regulation, and a stronger ability to challenge thoughts before reacting automatically to them.
3. Socratic Questioning
- “What evidence supports this belief? What evidence contradicts it?”
- “What would you tell a friend in this situation?”
- “If this thought were 100% true, what would that mean? And what then?”
- “Is there another way to look at this that you’re not yet considering?”
4. Downward Arrow Technique
5. Core Belief Restructuring
- Continuum work — plotting the belief on a 0–100 scale rather than treating it as binary.
- Historical review — examining how the belief formed and updating it with current evidence.
- Acting “as if” — behaving in line with a more adaptive belief and observing the outcome.
6. Cost-Benefit Analysis
Behavioral Activation CBT Techniques
Behavioral CBT techniques focus on changing the actions, avoidance patterns, and routines that maintain emotional distress over time. Rather than relying on insight alone, these interventions help clients test predictions, re-engage with meaningful activities, and build new experiences that challenge anxiety, depression, avoidance, and low motivation. Behavioral techniques are especially effective because they create real-world evidence that supports lasting cognitive and emotional change.
7. Behavioral Activation
Behavioral activation planners help clients translate therapy goals into specific, measurable actions while tracking the relationship between activity and mood over time.
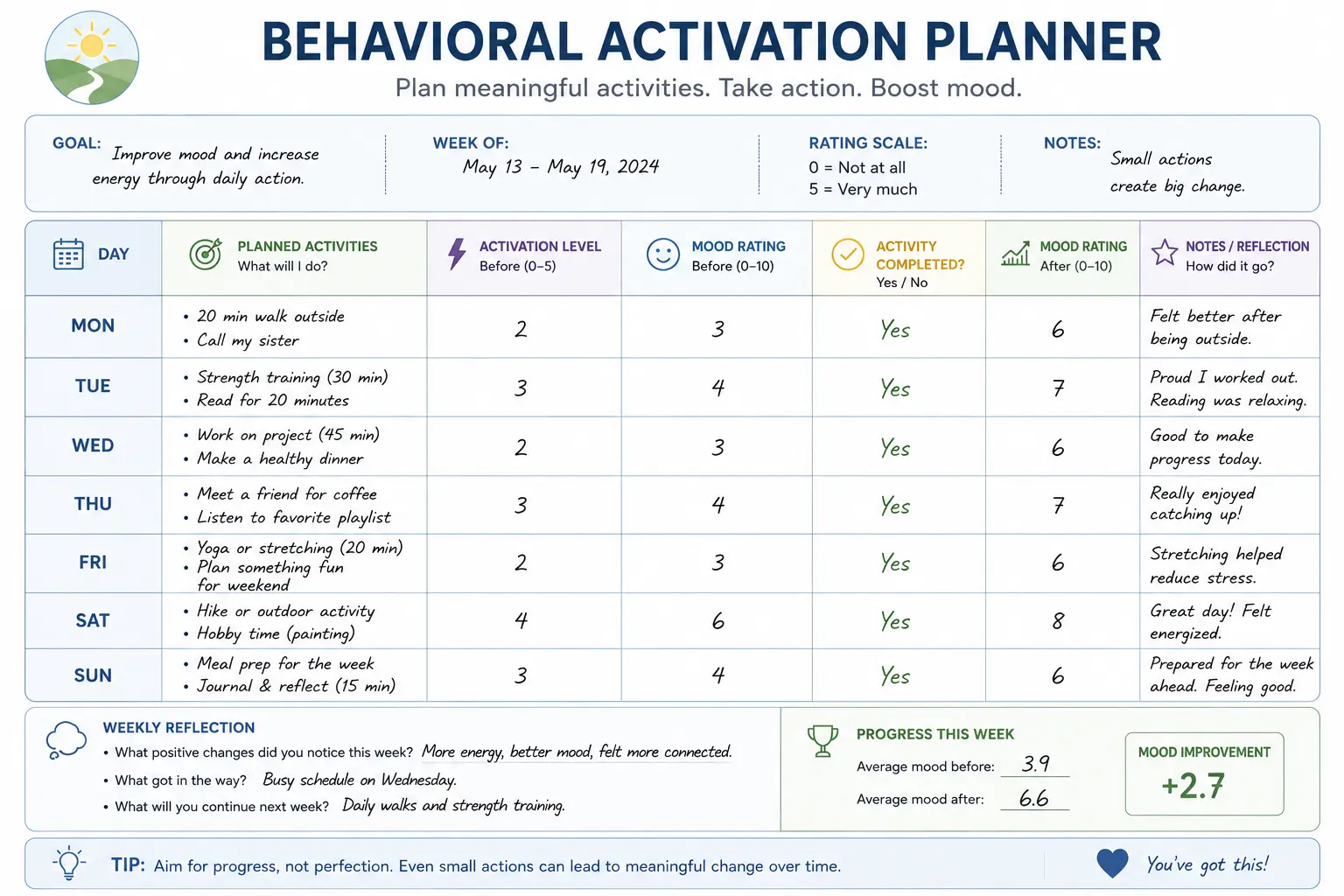
Even small increases in activity can begin disrupting the depressive cycle of withdrawal, low motivation, and reduced reinforcement that behavioral activation specifically targets.
8. Exposure Therapy
- Build a fear hierarchy from least to most distressing.
- Identify safety behaviors to drop.
- Begin with a step the client rates as moderately challenging.
- Stay in the situation long enough for new learning to occur — not necessarily for anxiety to drop.
- Reflect on what was learned and plan the next step.
Fear ladders help clients break overwhelming fears into smaller, manageable exposure steps that can be practiced gradually over time.
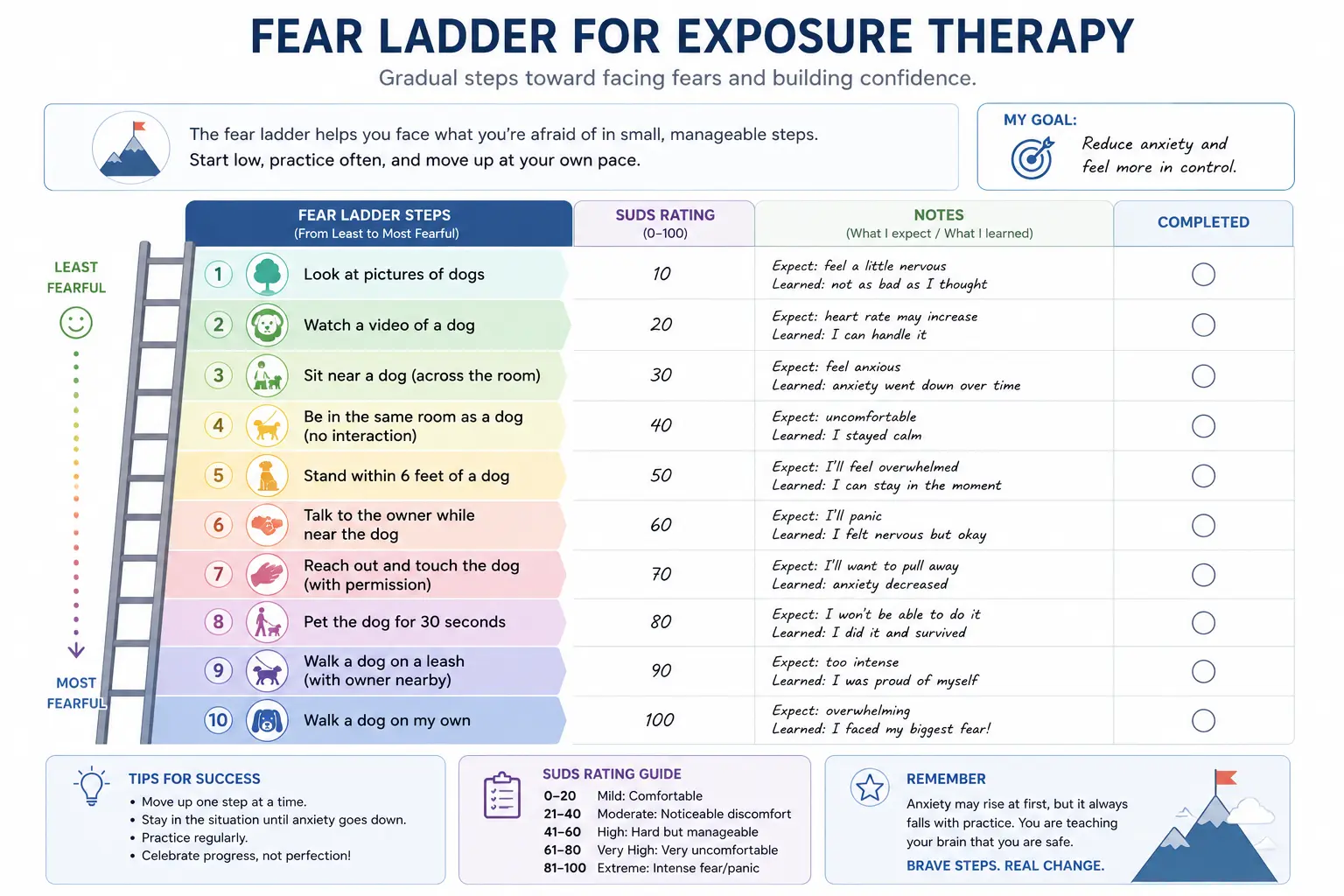
As clients repeatedly practice exposures and remain in the situation long enough for anxiety to decrease naturally, avoidance loses its reinforcing power and feared outcomes often become less believable and less overwhelming.
9. Behavioral Experiments
10. Graded Task Assignment
- Today: open a job board and bookmark three roles.
- Tomorrow: draft one paragraph of a cover letter.
11. Activity Scheduling
12. Self-Monitoring Logs
Emotion-Focused CBT Techniques
Emotion-focused CBT techniques help clients build awareness of emotional experiences, increase tolerance for distress, and respond to emotions more effectively rather than avoiding, suppressing, or becoming overwhelmed by them. These interventions are especially useful when strong emotional reactions interfere with cognitive work or contribute to impulsive behaviors, avoidance, shame, or relationship difficulties. By strengthening emotional regulation skills, clients become better able to engage in cognitive restructuring, behavioral change, and meaningful interpersonal interactions.
13. Emotion Identification and Labeling
- Emotion wheels
- Body-scan check-ins
- Emotion logs
14. Coping Skills Training
- Grounding: 5-4-3-2-1 sensory check
- Self-soothing: using the senses to support regulation
- Distress-tolerance skills: drawn from DBT and well-integrated with CBT
- Self-compassion practices: replacing self-criticism with more supportive responses
15. Relaxation Training
- Diaphragmatic, slow, paced breathing
- Progressive muscle relaxation
- Guided imagery
- Brief mindfulness practices
Cognitive behavioral therapy (CBT) is one of the most rigorously studied psychotherapies in modern behavioral health. Its appeal to clinicians is practical: CBT is structured, time-limited, and skills-based, which makes it easier to teach, supervise, and document than many other approaches. Whether you are an early-career therapist building a treatment toolkit or a seasoned clinician looking to refresh your repertoire, having a clear list of CBT techniques — along with real CBT examples and therapist language samples — makes session planning faster and more confident.
This guide walks through 20 core cognitive behavioral therapy techniques, organized by category. For each technique, you will find the clinical purpose, when to use it, a brief script you can adapt to your own voice, and a CBT example showing how it plays out in session. We also cover applications for anxiety, depression, and trauma, the most common mistakes clinicians make when implementing CBT, and an FAQ section addressing the questions trainees ask most often.
What is Cognitive Behavioral Therapy (CBT)?
Cognitive behavioral therapy (CBT) is a structured, evidence-based form of psychotherapy that helps people identify and change unhelpful thoughts, emotions, and behaviors. CBT is goal-oriented, skills-based, and commonly used to treat anxiety, depression, trauma, OCD, and related mental health conditions.
Cognitive behavioral therapy is a present-focused, goal-oriented psychotherapy developed by Aaron T. Beck in the 1960s. It rests on a simple but powerful premise: thoughts, emotions, and behaviors are interconnected, and changing one can change the others. Rather than excavating early childhood material, CBT focuses on the patterns maintaining a client’s distress right now and gives them concrete skills to interrupt those patterns.
Hallmarks of the CBT approach include:
- Present-focused and goal-oriented — sessions target specific, measurable problems.
- Collaborative and educational — the therapist and client work as a team, with the client learning skills they can use independently.
- Skills-based — between-session practice (often called “homework”) is part of the model, not an add-on.
- Evidence-driven — progress is tracked with measures, and treatment is adjusted accordingly.
How CBT Works: The CBT Triangle Explained
TThe CBT triangle shows how a situation can trigger automatic thoughts, emotional and physical responses, and behaviors that reinforce the cycle.
The CBT triangle (sometimes called the cognitive model) is the framework most clinicians use to introduce the model to clients. A triggering situation activates automatic thoughts, which generate emotional and physiological responses, which in turn drive behavior. Behavior then loops back to influence future thoughts and feelings. Most CBT techniques target one or more points on this loop.
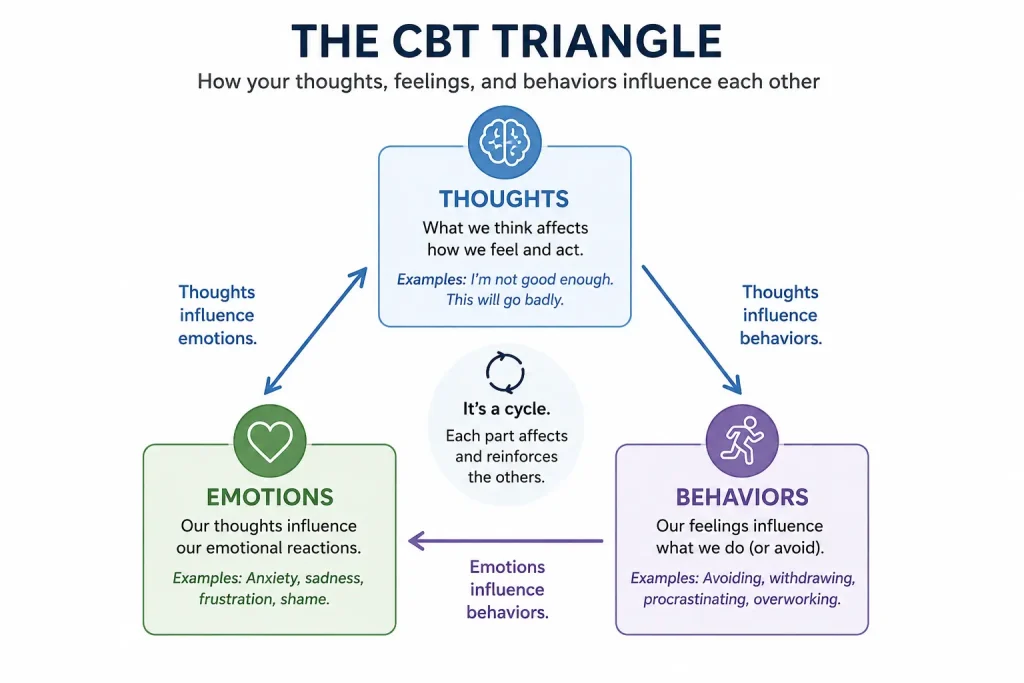
Drawing the triangle on a whiteboard during the first or second session gives clients a shared vocabulary for the work and helps them notice the loop in real time.
20 Evidence-Based CBT Techniques with Real Examples
The techniques below are organized into four categories: cognitive, behavioral, emotion-focused, and problem-solving. Most CBT protocols draw from across these categories rather than relying on a single technique. As you read, consider which fit your client population and which fill gaps in your current practice.
Cognitive CBT Techniques
Cognitive CBT techniques help clients identify, evaluate, and respond to the thought patterns that contribute to emotional distress and unhelpful behaviors. These interventions target automatic thoughts, cognitive distortions, and deeper core beliefs that shape how clients interpret situations, relationships, and themselves. The techniques below form the foundation of cognitive restructuring and are commonly used to treat anxiety, depression, low self-esteem, perfectionism, and related mental health concerns.
1. Thought Records
Thought records are one of the foundational tools in cognitive behavioral therapy because they help clients slow down automatic reactions and examine thoughts more objectively. By organizing the situation, emotional response, evidence, and alternative perspectives in writing, clients can begin separating facts from assumptions and develop more balanced thinking patterns over time.

Over time, repeated thought-record practice helps clients build cognitive flexibility, reduce emotional reactivity, and recognize recurring thinking patterns that contribute to anxiety, depression, shame, and self-criticism.
2. Identifying Cognitive Distortions
- Catastrophizing — jumping to worst-case outcomes
- All-or-nothing thinking — viewing situations in extremes
- Mind reading — assuming you know what others are thinking
- Emotional reasoning — “I feel it, so it must be true”
- Personalization — taking responsibility for events outside your control
- “Should” statements — rigid rules about how you or others must behave
Learning to identify cognitive distortions helps clients recognize the predictable thinking patterns that intensify emotional distress and reinforce unhelpful behaviors. Naming these patterns creates psychological distance from automatic thoughts and opens the door to more balanced, flexible interpretations.

As clients become more skilled at spotting cognitive distortions in real time, they often develop greater self-awareness, improved emotional regulation, and a stronger ability to challenge thoughts before reacting automatically to them.
3. Socratic Questioning
- “What evidence supports this belief? What evidence contradicts it?”
- “What would you tell a friend in this situation?”
- “If this thought were 100% true, what would that mean? And what then?”
- “Is there another way to look at this that you’re not yet considering?”
4. Downward Arrow Technique
5. Core Belief Restructuring
- Continuum work — plotting the belief on a 0–100 scale rather than treating it as binary.
- Historical review — examining how the belief formed and updating it with current evidence.
- Acting “as if” — behaving in line with a more adaptive belief and observing the outcome.
6. Cost-Benefit Analysis
CBT Examples in Practice: Three Vignettes
These short vignettes illustrate how techniques combine in real session work. Names and details are illustrative only.
Example 1: CBT for Anxiety — Thought Record + Exposure
Maya, 28, presents with generalized anxiety and avoidance of work meetings where she might be asked to speak.
After completing the thought record, the therapist proposes a behavioral experiment: contribute one prepared comment in the next meeting and observe what actually happens. Over four weeks, Maya moves up a hierarchy from prepared comments to spontaneous questions to leading a five-minute update. Anxiety doesn’t disappear, but its grip on her behavior loosens substantially.
Example 2: CBT for Depression — Behavioral Activation
David, 45, presents with major depressive disorder. He has stopped exercising, withdrawn from friends, and describes most days as “gray.”
Over the next month, walks expand, and David adds one social contact per week. Cognitive work follows once activation has built some traction.
Example 3: CBT for Social Anxiety — Behavioral Experiment
Aisha, 33, holds the belief that if she expresses a different opinion at her book club, the group will think less of her.
Aisha agrees to share one different opinion at the next meeting and notes responses afterward. The actual reaction — a thoughtful follow-up question from one member, no negative responses — directly contradicts her prediction. Over time, repeated experiments erode the original belief more effectively than verbal disputation alone.
Primary Headers
Subheader
This is the main blog copy
How to Choose the Right CBT Technique
With twenty techniques on the table, technique selection becomes the clinical question. A simple decision framework:
- Anxiety → exposure plus cognitive restructuring; behavioral experiments to test predictions.
- Depression → behavioral activation first; cognitive work after activation gains traction; core belief work for chronic presentations.
- Low self-esteem or chronic shame → core belief restructuring, positive data logs, continuum work.
- Avoidance and safety behaviors → behavioral experiments and graded exposure.
- Trauma → a manualized trauma-focused protocol (TF-CBT, CPT, PE) rather than improvised CBT.
- Worry and rumination → structured problem-solving, worry postponement, and metacognitive work.
- Crisis or high distress → stabilization, coping skills, and safety planning before any exposure or restructuring.
Always anchor technique selection in the case formulation. The question is not “Which technique is best?” but “Which mechanism is maintaining this client’s problem, and which technique targets that mechanism?”
Use the client’s presenting concern and case formulation to identify the CBT techniques most likely to target the maintaining pattern.
