Blog > Treatment Strategies > Transference & Countertransference in Therapy: Examples & Tips
Transference and Countertransference in Therapy: Definition, Examples, and How to Manage It
Transference and countertransference in therapy refer to the relational dynamics between client and therapist — where clients project past relationships onto the clinician, and therapists experience emotional reactions in response. Understanding these patterns is essential for maintaining boundaries, strengthening the therapeutic alliance, and improving clinical outcomes. This guide explains the key differences, provides real therapy examples, highlights warning signs, and offers practical strategies for managing both effectively in session.

Lindsay Rutter, MA, NCC, LPC
Last Updated: April 7, 2026


What You'll Learn
- The difference between transference and countertransference, including how each shows up in therapy and how to identify them in real time.
- Common types of transference — including positive, negative, parental, and romantic — and what they reveal about a client’s relational patterns.
- Real examples of transference and countertransference across therapy, counseling, and social work settings to sharpen clinical awareness.
- Warning signs of countertransference and how unrecognized reactions can impact boundaries, objectivity, and treatment decisions.
- How to manage transference and countertransference using supervision, mindfulness, and structured clinical reflection.
- Practical strategies to maintain therapeutic boundaries, prevent burnout, and use relational dynamics to improve outcomes.
Contents
What Is Transference in Therapy?
What Is Countertransference in Therapy?
Transference vs. Countertransference: What’s the Difference?
Examples of Transference and Countertransference in Therapy
Warning Signs of Transference and Countertransference
How to Deal With Transference as a Therapist
How to Manage Countertransference in Therapy
Self-Care Strategies for Therapists
Enhancing Patient Care Through Therapeutic Boundaries
Transference and Countertransference in Counseling and Social Work
What Is the Difference Between Transference and Countertransference?
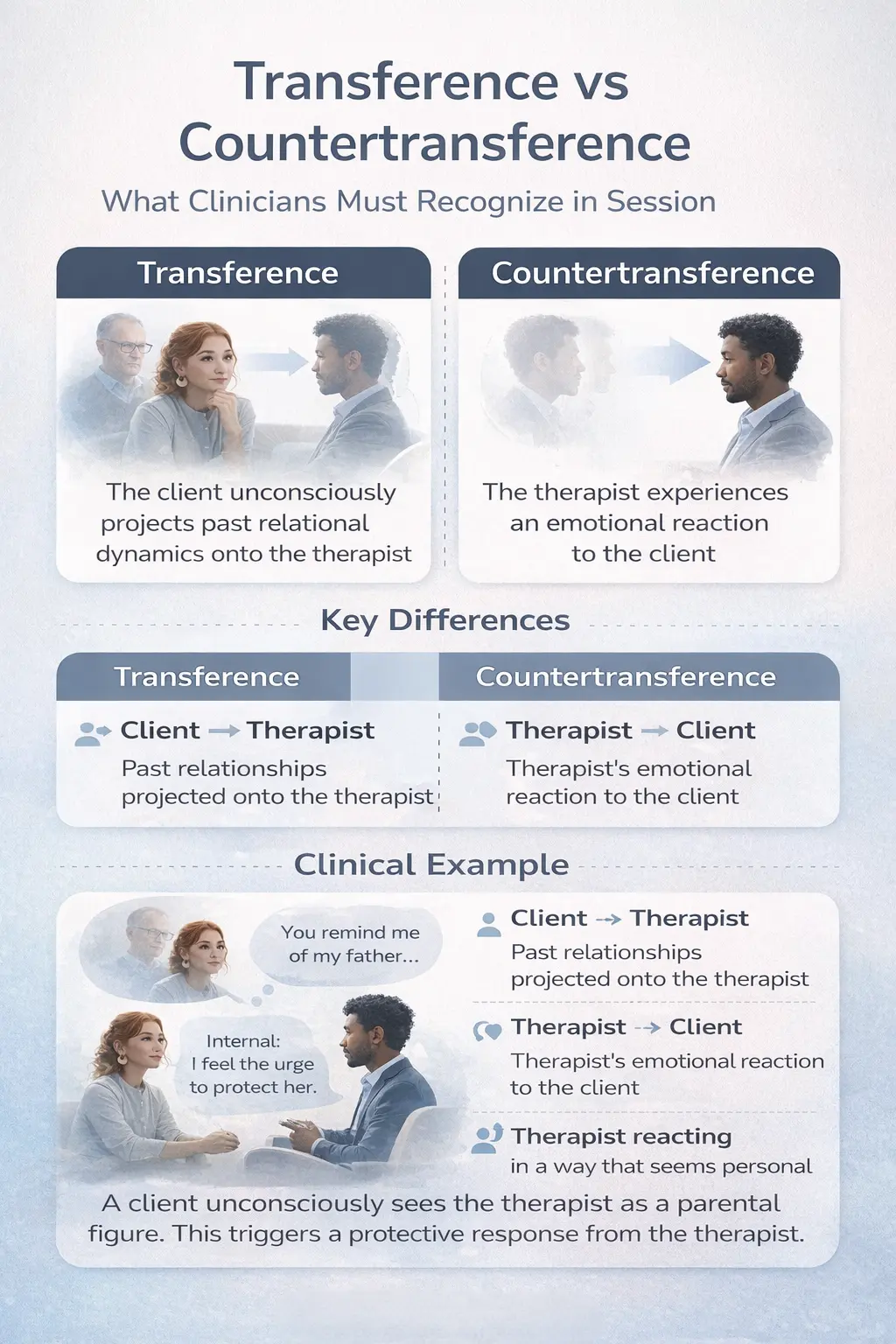
Transference occurs when a client unconsciously redirects feelings, expectations, or relational patterns from past relationships onto the therapist. Countertransference refers to the therapist’s emotional reaction to the client, which may be shaped by the therapist’s own experiences, biases, or unresolved issues.
Transference
The client projects emotions, assumptions, or patterns from earlier relationships onto the therapist.
Countertransference
The therapist experiences an emotional response to the client that can affect the therapeutic relationship if left unexamined.
In simple terms: transference comes from the client toward the therapist, while countertransference comes from the therapist in response to the client.
Understanding transference and countertransference in therapy is central to ethical, effective clinical work. These interpersonal phenomena shape the therapeutic relationship, influence the therapeutic alliance, and — when handled skillfully — become powerful clinical data you can use to advance treatment.
This guide defines transference and countertransference, explains the key differences between them, provides real clinical examples, and offers practical management strategies so therapists, counselors, and social workers can translate awareness into better outcomes. You’ll also find a downloadable checklist and FAQ to support your ongoing professional development.
What is Transference in Therapy?
Transference in therapy refers to when a client projects their feelings about someone else — typically a parent, caregiver, or former partner — onto their therapist. This redirection of feelings can be both positive and negative and often stems from unresolved issues or past experiences.
The concept of transference, first described by Freud in psychoanalytic theory, plays a fundamental role in understanding the patient relationship dynamic. From a cognitive perspective, transference represents how past experiences shape current interactions, while attachment theory helps explain why certain patterns emerge in the therapist-patient relationship.
For example, a patient who lost a parent as a child may look to the therapist for acceptance and unconditional love, demonstrating parental transference. While the therapist cares for their patient, it might not feel like enough to the patient, which can lead to misunderstandings, hurt, disappointment, and even anger.
Recognizing transference is not a sign of therapeutic failure. In fact, transference often provides a window into the client’s core relational patterns and can become some of the most transformative material in treatment when addressed skillfully.
Types of Transference
Understanding different types of transference helps clinicians navigate the therapeutic relationship more effectively:
- Positive transference: The client experiences warm, affectionate feelings about someone from their past and projects these onto the therapist. While this can strengthen the therapeutic alliance, unchecked positive transference may create dependency or inhibit honest feedback.
- Negative transference: The client manifests hostile or angry feelings transferred from past relationships, often appearing as resistance, missed sessions, or confrontational behavior in therapy.
- Parental transference: The client treats the therapist as a parent figure, seeking approval, nurturing, or rebelling against perceived authority—mirroring dynamics from their family of origin.
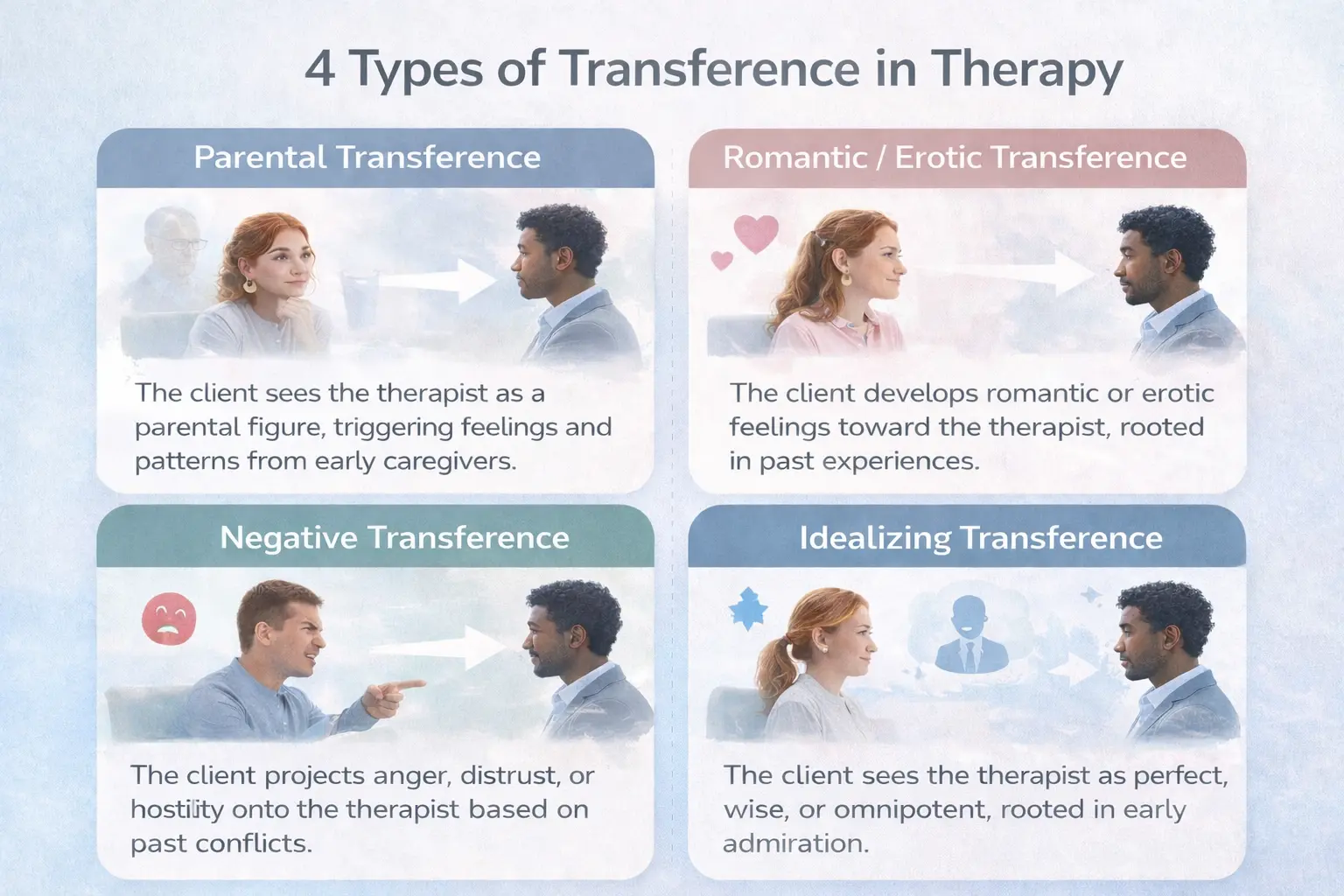
- Romantic transference (erotic transference): The client develops romantic or sexual feelings directed toward the therapist. This is one of the most clinically complex forms to navigate and requires clear boundaries, direct discussion, and often supervision.
- Familial transference: The client reflects broader family dynamics in the therapy session — such as sibling rivalry, caretaking roles, or enmeshment patterns.
- Emotional transference: A broader category encompassing any intense emotional response — fear, sadness, guilt — that the client displaces from a past relationship onto the therapist.
Transference plays a significant role in therapy by providing insights into a patient’s inner world. When a patient transfers feelings from their past onto the therapist, it can reveal deeper issues and unresolved conflicts. Being able to identify transference allows both the client and therapist to delve deeper into underlying problems and address them together, strengthening the therapeutic alliance and improving therapy outcomes.
What is Countertransference in Therapy?
Countertransference occurs when a therapist’s emotional reactions to a client are influenced by the therapist’s own unresolved issues, personal history, or unconscious processes. The definition of countertransference encompasses the full range of emotional reactions, thoughts, and feelings that a therapist experiences in response to a patient.
While the classical definition limited countertransference to the therapist’s unconscious response to a client’s transference, the modern understanding is broader: it encompasses any emotional reaction the clinician has that may affect clinical judgment. Like transference, countertransference can provide a critical source of information about the inner world of both the patient and therapist.
Countertransference is a normal and inevitable part of clinical work. The issue is not whether it occurs — it will — but whether the therapist recognizes and manages it. Unaddressed countertransference can lead to biased judgments and compromised treatment decisions, hindering the therapeutic process.
Types of Countertransference
- Concordant countertransference: The therapist empathically identifies with the client’s emotional experience — feeling sad when the client describes loss, anxious when the client describes threat. This is generally adaptive but can become problematic if it leads to over-identification.
- Complementary countertransference: The therapist takes on the role of a significant other in the client’s life. For example, a therapist may become overly directive with a client who unconsciously seeks a controlling authority figure, essentially reenacting the dynamic the client is trying to resolve.
- Reactive countertransference: The therapist’s personal triggers are activated by the client’s material. A therapist who recently experienced a divorce may find themselves emotionally flooded when working with a client processing a separation.
Learning to recognize, understand, label, and express your feelings about your sessions can help you use countertransference to provide effective care. Working with a supervisor and engaging in regular reflection can help you develop greater awareness of your countertransference reactions and unconscious feelings.
Transference vs. Countertransference: What's the Difference?
While transference and countertransference are closely related, they operate from different directions in the therapeutic relationship. Understanding the difference between transference and countertransference helps clinicians identify which dynamic is at play — and respond appropriately.
| Dimension | Transference | Countertransference |
|---|---|---|
| Direction | Client → Therapist | Therapist → Client |
| Source | Client’s past relationships and unresolved conflicts | Therapist’s personal history, unresolved issues, or reactions to client material |
| Awareness | Typically unconscious to the client | May be unconscious or conscious to the therapist |
| Clinical Value | Reveals core relational patterns and can be used therapeutically in treatment | Signals where objectivity may be compromised and can also deepen empathic understanding |
| Primary Risk | The client reenacts maladaptive patterns without insight | The therapist responds from personal emotion rather than clinical judgment |
| Management | Interpretation, exploration, psychoeducation, and consistent in-session boundaries | Supervision, personal therapy, reflective practice, and careful documentation |
Both dynamics can coexist in the same session. A client’s transference may trigger the therapist’s countertransference, creating a feedback loop that can intensify if neither party is aware of what’s happening. This is why ongoing self-reflection and clinical supervision are critical — and why structured documentation helps you track these patterns over time.
The Process of Transference and Countertransference in Therapy
In practice, transference and countertransference unfold as a relational sequence. A client brings emotional expectations into the session, the therapist reacts, and clinical awareness helps guide a therapeutic response.
Client Brings Emotion
The client enters therapy with unresolved feelings and relational patterns from past experiences.
Transference Emerges
The client begins to experience the therapist through the lens of earlier relationships.
Therapist Reacts
The therapist notices emotional responses such as protectiveness, frustration, or over-identification.
Clinical Awareness
Reflection and supervision help the therapist identify what belongs to the client, therapist, or dynamic.
Therapeutic Response
The therapist uses the dynamic to support insight, maintain boundaries, and guide treatment.
These steps often happen quickly and subtly, which is why recognizing transference and countertransference is such a critical clinical skill.
Examples of Transference and Countertransference in Therapy
Concrete clinical examples help clinicians recognize transference and countertransference in their own practice. Below are representative scenarios across common therapeutic settings.
Transference Examples in Therapy
Idealization and Dependency (Positive Transference)
A client in individual therapy begins telling friends that their therapist is “the only person who truly understands me.” They request extra sessions, text between appointments, and become visibly distressed at session endings.
What’s happening:
The client is projecting attachment needs—likely rooted in inconsistent caregiving during childhood—onto the therapist. The therapist has become a stand-in for the nurturing parental figure the client never had.
Clinical approach:
This positive transference can be therapeutically valuable if explored as material. The therapist might gently name the pattern: “I notice that our relationship has become very important to you. Can we talk about what that feels like and whether it reminds you of other relationships?”
Authority-Based Hostility (Negative Transference)
A male client in court-mandated anger management therapy becomes confrontational whenever his female therapist sets structure for the session. He dismisses her suggestions, arrives late, and frequently says, “You don’t know what it’s like.”
What’s happening:
The client is projecting feelings associated with a controlling or dismissive female authority figure—possibly a mother, teacher, or supervisor—onto the therapist. The mandated nature of treatment intensifies the power dynamic.
Clinical approach:
Rather than confronting the resistance directly, the therapist might explore the pattern: “It seems like being told what to do in here brings up strong feelings. Has that been true in other areas of your life?”
Romantic or Erotic Transference
A client begins dressing differently for sessions, making flirtatious comments, and asking personal questions about the therapist’s relationship status. They express that the therapist is “different from anyone else” in their life.
What’s happening:
Erotic transference often reflects the client’s conflation of emotional intimacy with romantic or sexual attachment—particularly in clients with histories of enmeshed family systems or relational trauma.
Clinical approach:
This must be addressed directly but without shaming. The therapist should name the dynamic, reinforce the therapeutic frame, and explore the underlying relational pattern. Supervision is strongly recommended.
Countertransference Examples in Therapy
The Rescuer (Over-Identification)
A therapist working with a young single mother who is struggling financially finds themselves spending extra time on the case, providing resources beyond the scope of therapy, and feeling personally responsible for the client’s wellbeing outside sessions.
What’s happening:
The therapist’s own background—perhaps growing up in a family with financial instability or having a personal identification with the client’s situation—is driving them beyond clinical boundaries into a caretaking role.
Clinical approach:
The therapist should examine in supervision: “What need of mine is this meeting?” The urge to rescue often reflects the clinician’s unresolved material, not the client’s actual treatment needs.
Avoidance Countertransference
A therapist consistently steers sessions away from a client’s trauma narrative, focusing instead on present-day coping skills. When the client attempts to discuss the traumatic event, the therapist redirects with, “Let’s focus on what you can control right now.”
What’s happening:
The therapist may be experiencing vicarious traumatization, or their own unresolved trauma is being activated by the client’s material. The avoidance is protective—for the therapist, not the client.
Clinical approach:
Avoidance countertransference is particularly insidious because it can look like good clinical practice (stabilization, present-focus). Supervision and honest self-reflection are necessary to distinguish evidence-based pacing from clinician-driven avoidance.
Frustration and Over-Directiveness
A therapist working with a client who repeatedly returns to an abusive partner feels growing frustration and impatience. They notice themselves making more directive statements: “You know what you need to do.”
What’s happening:
The therapist’s frustration may stem from their own beliefs about self-advocacy, personal experiences with similar dynamics, or burnout from witnessing cyclical patterns. The directiveness signals a loss of therapeutic neutrality.
Clinical approach:
The frustration itself is clinically informative—it may mirror the frustration the client’s support system feels, revealing the relational pattern at play. Processing this in supervision preserves the therapeutic alliance.
Is this reaction about the client—or about me?
When you notice a strong emotional reaction in session, pause and ask yourself:
“Is this reaction driven by the client’s needs—or my own?”
This simple question can help you quickly distinguish countertransference from empathic attunement and guide you toward a more intentional, clinically grounded response.
Warning Signs of Transference and Countertransference
Early identification of transference and countertransference protects the therapeutic relationship and prevents boundary erosion. Use the following checklists to stay attuned — and bring them to supervision when you notice patterns emerging.
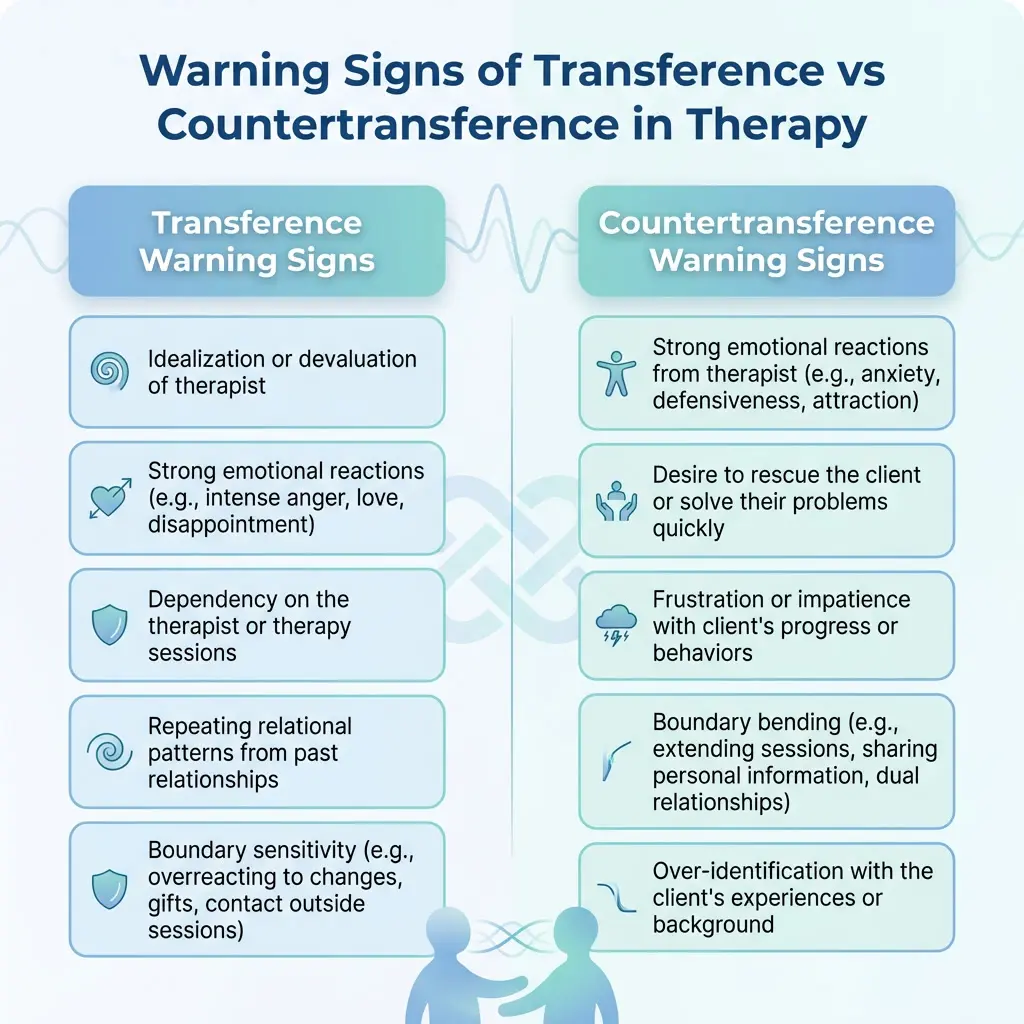
Warning Signs of Transference
- The client consistently reacts to you in ways disproportionate to the situation (e.g., intense anger over a minor scheduling change)
- The client idealizes or devalues you in patterns reminiscent of other key relationships in their history
- The client expresses feelings of love, dependency, or fear that seem disconnected from the actual therapeutic relationship
- The client’s relational patterns with you mirror the dynamics described in their personal history
- The client resists exploring the therapist-client dynamic when gently invited to do so
- The client begins treating you as a friend, parent, or romantic interest rather than a professional
- Ruptures in the therapeutic alliance repeat without resolution, following a recognizable cycle
- Strong reactions to routine boundaries (fees, time limits) that mirror earlier relationship injuries
- Projective identification: the client pressures you into enacting a role that confirms their expectation
Warning Signs of Countertransference
- You dread or eagerly anticipate specific clients more than clinical reasoning warrants
- You find yourself thinking about a client outside sessions in personal rather than clinical terms
- You notice yourself bending your usual boundaries—extra time, reduced fees, personal disclosures—for a particular client
- You feel unusually protective, frustrated, bored, or anxious with a specific client
- You avoid certain topics or challenge a client more harshly than their presentation warrants
- You catch yourself identifying with the client’s perspective to the point where you’ve lost objectivity (“We’re basically the same”)
- You have difficulty maintaining documentation standards for a particular client—over-documenting or under-documenting
- Colleagues or supervisors notice a shift in your clinical approach with a specific case
- Irritability, attraction, excessive advice-giving, or “working harder than the client”
- Inappropriately disclosing personal information or wanting to “save” a client from their problems
Download the Transference & Countertransference Checklist
Give clinicians a practical tool for recognizing relational dynamics in session. This downloadable checklist helps identify signs of transference and countertransference, support clinical self-awareness, and strengthen therapeutic boundaries.
Ideal for supervision, consultation, and day-to-day clinical reflection.

Get Your Free Checklist
Enter your info below to download instantly.
How to Deal With Transference as a Therapist
While transference can reveal insights about a client’s psyche, you must effectively manage it to avoid distorting the patient-therapist relationship. The key lies in recognizing and harnessing its potential benefits while minimizing any negative impacts on the therapeutic journey. The goal is not to eliminate transference — which is neither possible nor desirable — but to use it as clinical material while preventing it from derailing treatment.
1. Address Transference from the Start
To prevent misunderstandings and provide the best possible care, address any transference patterns openly with your client from the start. Bringing awareness to them can help avoid a distorted dynamic and facilitate a stronger therapeutic alliance. Psychoeducation about how past relationships can influence the therapy relationship sets the stage for productive exploration.
2. Spot and Follow Anxieties
You can manage transference by following any anxieties your client is displaying and using them to promote healing and growth. For example, if your client projects anxieties about a parental figure onto you, delve deeper into the wishes beneath those anxieties. Name the pattern compassionately, anchor it to treatment goals, and invite curiosity: “What does my limit remind you of?”
3. Avoid Judgment
While some clients may appreciate learning how their patterns might be playing out in therapy, others may feel exposed or judged. Since transference often stems from past trauma, it’s crucial to be gentle and non-judgmental when bringing it up. Approach transference work with empathy and compassion — your tone matters as much as your clinical accuracy.
4. Maintain the Therapeutic Frame
Consistent boundaries are the foundation of safe transference work. Session times, cancellation policies, communication norms, and role clarity all serve as containment for the emotions transference stirs up. When transference intensifies, resist the pull to modify the frame — this is precisely when consistency matters most.
5. Use Supervision Proactively
Don’t wait for transference to become problematic before bringing it to supervision. Regular case consultation helps you see patterns you may be too close to recognize. Your supervisor can offer a different perspective and help you process whether the transference is productive material or a clinical risk that needs direct intervention.
6. Document Transference Patterns
Track transference observations in your progress notes to identify patterns across sessions. When transference dynamics are documented and linked to treatment goals, it’s easier to assess whether the therapeutic relationship is advancing or obstructing progress. A behavioral health EHR like ICANotes provides structured templates that make this documentation efficient and clinically meaningful.
How to Manage Countertransference in Therapy
While transference management is primarily an in-session skill, managing countertransference is an ongoing professional practice that extends well beyond the therapy room. Your reactions to your patient can often provide valuable insight into the reactions the patient might elicit in people around them — but only if you can distinguish your countertransference from the patient’s clinical material.
Practice Mindfulness
As a therapist, you are subjected to your own feeling states during sessions, both emotional and physical. The more feelings you can tolerate from yourself, the more you can contain and hold your patients’ unacceptable feelings. Mindfulness techniques help you become more present and aware of your emotional responses. If you can allow yourself to experience and accept your feelings—anger, jealousy, love, sadness—you will become a more present therapist and gain tools to provide better care.
Engage in Regular Supervision
Supervision is the single most effective safeguard against harmful countertransference. Present cases where you notice strong emotional reactions, boundary pulls, or deviations from your typical clinical approach. Strategies like guided imagery and role-playing in supervision can help you assess how you feel and what you learned by replaying challenging scenarios from both the therapist and client perspectives.
Pursue Your Own Therapy
Clinicians who engage in their own personal therapy are better equipped to recognize when their unresolved material is entering the clinical space. Personal therapy is not a sign of weakness—it is a professional investment in your capacity to do this work sustainably.
Use Documentation as a Reflective Tool
Progress notes and treatment plans are not just compliance instruments—they are clinical thinking tools. When you notice yourself documenting with more emotional language than usual, or struggling to write notes for a particular client, those are countertransference signals worth examining. An EHR system designed for behavioral health can streamline this process with structured templates that prompt clinical reflection while reducing administrative burden.
Know Your Triggers
Every clinician has populations, presenting problems, or relational dynamics that are more likely to activate countertransference. A therapist with a personal history of addiction may have stronger reactions to substance use disorder cases. A clinician who recently became a parent may find themselves more emotionally activated by child welfare cases. Knowing your triggers isn’t about avoiding these cases—it’s about approaching them with intentional self-awareness.
Know When to Refer
If you are having trouble managing countertransference and have taken steps to mitigate it, always put the patient first. If you feel like they could benefit, refer your client to a provider who is better prepared to engage with them. This ethical consideration protects both the therapist and patient and maintains the integrity of the therapeutic process.
Self-Care Strategies for Therapists
Self-care is crucial in your role as a mental health professional. Several self-care strategies can put you in a better mindset to work with clients, help you avoid burnout and manage countertransference more effectively. Working in psychology, psychiatry, and psychotherapy can be emotionally demanding, making self-care not just beneficial but essential.
Importance of Self-Care in Preventing Professional Burnout
There is a strong link between therapist well-being and effective patient care. Countertransference can easily occur when you are stressed or have a lot going on in your personal life, as can burnout — which can impact treatment outcomes and compromise the therapist and client relationship. Signs of burnout can include mental or emotional exhaustion, cynicism about work and reduced feelings of personal accomplishment.
Practical Self-Care Techniques for Therapists
- Boundaries: Set personal and professional boundaries. Learn to say no without guilt and recognize your limitations and capacity within professional relationships. Clear boundaries help prevent countertransference from interfering with therapy sessions.
- Regular breaks: Schedule breaks throughout the day to step away from work. Practice mindfulness, stretch, do yoga, or take a quick walk. This helps you recharge and maintain perspective on your work.
- Physical health: Prioritize your health by working out, eating well, and getting enough sleep. Regular exercise reduces stress and boosts well-being. Physical wellness supports your emotional capacity to process countertransference.
- Nurture your relationships: Spending time with loved ones provides emotional support in tough times and helps you maintain healthy relationships outside the therapy setting. These connections serve as an important resource for processing your experiences.
- Check in with yourself: Regularly assess what you’re feeling emotionally, mentally, and physically. When you become more mindful of your feelings, you can address issues before they escalate. Be kind to yourself when you notice countertransference — be proud of yourself for noticing and taking steps.
- Seek supervision and feedback: Regular supervision is essential for managing both transference and countertransference. Your supervisor can provide insight, offer a different perspective, and help you process your emotional reactions. Don’t hesitate to seek consultation when you encounter challenging situations.
Enhancing Patient Care Through Therapeutic Boundaries
Boundaries act as the guideline for all involved in the therapeutic relationship, helping you ensure a successful relationship between yourself and your clients. Professional boundaries protect both the therapist and patient and create a safe container for the therapeutic process to unfold.
How to Set Physical, Material, Time, Emotional, and Intellectual Boundaries
- Physical: Physical boundaries include how your patients reach you — in your office, virtually, or by phone. Consider whether you’re comfortable providing your personal cell phone number or prefer a separate work phone. Be upfront with patients about what you’re comfortable with. Physical boundaries help prevent boundary crossings that could complicate transference dynamics.
- Material: This relates to the financial side of your practice. Consider whether to offer alternative payment options and get comfortable discussing payment issues, such as missed payments. Clear material boundaries prevent resentment and maintain the professional nature of the therapeutic relationship.
- Time: Time boundaries include knowing when to wrap up sessions, creating dependable cancellation policies, and ending sessions on time. Consistent time boundaries communicate respect and reliability to patients — and serve as important containment when transference dynamics intensify.
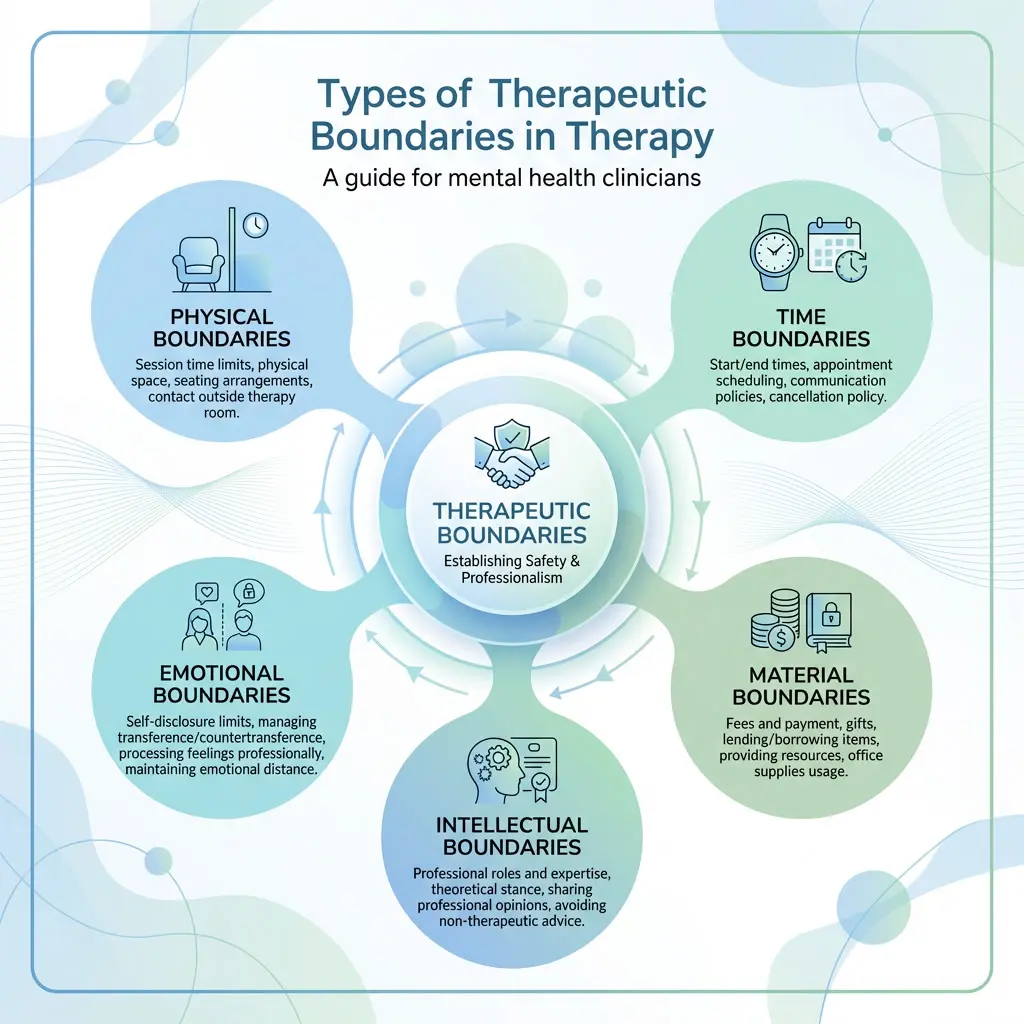
- Emotional: Maintain a network of support—local resources for patients and consistent coping mechanisms for yourself. Regularly care for your emotional well-being and connect patients with local resources when you are away. Emotional boundaries help you maintain empathy without becoming overwhelmed by countertransference.
- Intellectual or spiritual: Create space for compassion in situations where opinions differ. Know what ideas guide your practice and prepare patients for what to expect. Remember to set clear boundaries when beliefs and ideas differ. The goal is a safe space where patients can share their thoughts and explore their own perspective.
Clear professional boundaries create safety for both patients and physicians. As the therapist, you are responsible for preserving these boundaries. If a minor violation occurs, it's best to address it promptly before it becomes more problematic. By balancing empathy and professionalism, you can build a safe and effective therapeutic environment that supports healing and growth.
Related: Navigating Boundaries and Building Trust: Working with Clients with BPD
A Quick Example to Pull It Together
A client who often “forgets” copays arrives apologetic and eager to please (positive transference) but bristles when the fee is named (negative swing). You notice your own urge to waive it “just this once” (countertransference). Instead, you regulate, keep the boundary, and explore the meaning: money has always equaled love and power in their family. You co-design a transparent payment plan, and in sessions you track what happens in their body when fairness, limits, or dependence arise. Over weeks, the client practices tolerating limits without collapsing or fighting, and you practice holding limits without hardening or rescuing. The therapeutic relationship becomes the rehearsal space for healthier relationships outside the room.
Transference and countertransference are not limited to psychotherapy or psychoanalytic practice. These dynamics arise across all helping professions, including counseling, social work, school-based mental health, and case management.
In Counseling Settings
Counselors working in community mental health, school settings, or private practice encounter transference regularly — often in clients who may not have the language or framework to understand what they’re experiencing. Psychoeducation about the therapeutic relationship can be especially valuable in counseling contexts where the work may be shorter-term. Countertransference in counseling is particularly common when counselors carry large caseloads with limited supervision, making self-monitoring practices essential.
In Social Work
Social workers face unique countertransference challenges because their roles often extend beyond the therapy room into advocacy, case management, and systemic navigation. A social worker managing a child welfare case may experience intense countertransference when their client’s circumstances mirror their own family history — or when systemic barriers produce feelings of helplessness that get projected onto the client relationship. Transference in social work can also be complicated by the power dynamics inherent in mandated services, involuntary clients, and institutional settings.
Regardless of discipline, the management principles are the same: self-awareness, supervision, documentation, and a commitment to distinguishing your emotional reactions from your client’s clinical needs.
Frequently Asked Questions About Transference and Countertransference
Final Thoughts on Transference and Countertransference in Therapy
Understanding transference and countertransference in therapy is essential for providing effective mental health care. These phenomena — the concept of transference originally described by Freud and the parallel process of countertransference — offer valuable insight into the inner worlds of both patients and therapists when properly recognized and managed.
As we've explored in this article, both positive transference and negative transference provide important information about a client's past experiences and current relational patterns. Similarly, countertransference, when approached with awareness and supervision, becomes a therapeutic tool rather than an obstacle. The key is developing the ability to distinguish between your own emotional reactions and those projected onto you by patients.
For therapists, psychologists, social workers, and other mental health professionals, managing these dynamics requires ongoing commitment to self-care, professional development, supervision, and structured documentation. Each therapy session offers opportunities to refine your awareness and techniques, ultimately helping you provide better care to your clients and maintain your own well-being in this demanding but rewarding profession.
Related Resources
Boundaries in Counseling: Therapist-Client Limits
Learn how to set and maintain professional boundaries across emotional, time, and relational domains.
Read more →Navigating Boundaries and Building Trust with BPD Clients
Clinical strategies for maintaining structure while strengthening the therapeutic alliance with complex clients.
Read more →Vicarious Trauma, Compassion Fatigue, and Burnout
Understand how emotional strain impacts clinicians and how to recognize early warning signs.
Read more →Self-Care for Behavioral Health Professionals
Practical strategies to reduce burnout and sustain your clinical effectiveness over time.
Read more →Explore ICANotes to Help Maintain Ethical Standards and Enhance Patient Care
Understanding examples of transference and countertransference and how they manifest in sessions can help you harness their benefits and provide effective care to clients. Having the right tools and resources to support your practice makes managing these complex dynamics easier.
ICANotes is an electronic charting solution that helps you focus on the relationship rather than the record. Use templates to capture transference themes, note countertransference observations where appropriate, and document boundary discussions and alliance repairs — all linked to goals and interventions. The result is cleaner notes, smoother audits, and more emotional bandwidth for the moments that matter.
See how ICANotes keeps your clinical frame steady while you do the deep work. Book a demo or start a free trial.
Stay Present in the Session—Without Losing the Clinical Thread
When you’re managing transference, countertransference, and therapeutic boundaries, your documentation system should support your clinical thinking—not pull you out of the work. ICANotes helps behavioral health clinicians capture meaningful session content efficiently while maintaining a clear, defensible record.
Use structured note templates to document relational patterns, boundary discussions, treatment progress, and interventions with less typing and more consistency.
Why clinicians use ICANotes: Document complex therapy sessions more efficiently, reduce after-hours note writing, and keep your records aligned with the real work happening in treatment.
Start Your Free Trial
See how ICANotes helps you document therapy sessions clearly, efficiently, and with greater clinical confidence.
No credit card required.
Recent Posts
About the Reviewer
Lindsay Rutter, MA, NCC, LPC, is a Licensed Professional Counselor with a Master’s Degree in Clinical Counseling. She has nearly 15 years of clinical and supervisory experience with extensive knowledge of mental health diagnoses, their etiology, and evidence-based treatments. Lindsay is the Clinical Director of a non-profit community mental health center and the owner of a private practice in Chester County, PA.







Transference and Countertransference in Counseling and Social Work