Blog > Treatment Strategies > Grief Treatment Plan: Goals, Objectives & Sample Templates for Clinicians
Grief Treatment Plan: Goals, Objectives, and Examples for Clinicians
A grief treatment plan outlines structured goals, measurable objectives, and interventions to help clients process loss and improve functioning. This guide includes grief counseling goals, SMART objectives, a sample treatment plan, and specialized approaches for complicated grief and prolonged grief disorder.

Last Updated: March 31, 2026

What You'll Learn
- How to create a clinically sound grief treatment plan with clear goals, measurable objectives, and evidence-based interventions
- Examples of grief counseling goals and objectives organized by acute grief, complicated grief, and comorbid conditions
- How to apply the SMART goals framework in grief therapy to improve documentation, treatment planning, and outcomes
- Key differences in prolonged grief disorder (PGD) treatment planning and how to structure PGD-specific goals and objectives
- How interventions like CBT, ACT, and complicated grief therapy (CGT) map directly to treatment plan goals
- A complete sample treatment plan for grief and loss you can adapt for clinical use
Contents
- When is a Treatment Plan for Grief and Loss Clinically Appropriate?
- Types of Grief and Treatment Planning Considerations
- Grief Treatment Plan Goals and Objectives: Examples by Grief Type
- SMART Goals for Grief Therapy
- Therapeutic Interventions for Grief Treatment Plans
- Treatment Planning for Prolonged Grief Disorder
- Sample Treatment Plan for Grief and Loss
- Documenting Progress and Adjusting Grief Treatment Plans
- Write Better Grief Treatment Plans with ICANotes
- Frequently Asked Questions About Grief Treatment Plans
A grief treatment plan is a structured, clinician-led framework that supports clients as they process loss and work toward functional recovery. It defines personalized treatment goals, measurable objectives, and therapeutic interventions to help clients manage grief-related distress, maintain daily functioning, and adapt after a significant loss.
This guide provides mental health professionals and grief counselors with practical tools for grief treatment planning, including goal and objective examples organized by grief type, SMART goals for grief therapy, a full sample treatment plan, and an overview of evidence-based interventions. Whether you are developing a treatment plan for acute grief, complicated grief, or prolonged grief disorder, this resource offers a clinical framework you can adapt to each client's needs.
What is a Grief Treatment Plan?
A grief treatment plan is a structured, documented plan that outlines goals, objectives, and interventions to support a client coping with loss. It is used when grief significantly affects emotional well-being, daily functioning, or mental health and requires more than informal support.
The plan identifies key grief-related concerns, sets measurable goals, and guides care over time. Its purpose is not to eliminate grief, but to reduce distress, support adaptation, and help clients function while integrating their loss.
Grief treatment plans are individualized and flexible. They reflect the client's circumstances, cultural context, and the nature of the loss. Plans are reviewed and adjusted as grief evolves to support ethical, clinically appropriate care.
A grief treatment plan does not require a formal diagnosis. It can be used any time a clinician determines that structured, goal-directed support would benefit a client's grief process.
Grief Treatment Plan Process
The process below outlines how clinicians can structure a grief treatment plan—from initial assessment through goal setting, intervention selection, and ongoing adjustment.
Assess
Evaluate grief type, symptoms, and functional impairment
Define Goals
Identify treatment goals based on client needs
SMART Objectives
Create measurable, time-bound objectives
Interventions
Select CBT, ACT, CGT, or other evidence-based approaches
Track Progress
Monitor symptoms, functioning, and goal progress
Adjust Plan
Refine goals and interventions as grief evolves
Each step in thie process connects directly to the treatment goals, SMART objectives, and interventions outlined in this guide.
When is a Treatment Plan for Grief and Loss Clinically Appropriate?
Grief is a normal response to loss, and many clients adapt over time with natural support and routine. In these cases, formal treatment planning may not be necessary. A grief treatment plan becomes appropriate when grief does not ease over time or begins to significantly disrupt emotional well-being, daily functioning, or mental health.
Normal Grief vs Grief Requiring Intervention
Normal grief often includes sadness, longing, disrupted sleep, and emotional fluctuation. These reactions may be intense but usually lessen over time, allowing clients to maintain basic responsibilities and experience moments of relief or connection.
Grief may require clinical intervention when distress is persistent, worsening, or functionally limiting. Signs include emotional numbness, preoccupation with the loss, avoidance of reminders, or a sense of being unable to move forward. In these cases, a structured treatment plan supports adaptation and reduces impairment.
Related: Assessing Grief: Evidence-Based Screening & Treatment Guide

Functional Impairment Indicators
Functional impairment is one of the clearest indicators that treatment planning may be appropriate. Clinicians may consider formal planning when grief interferes with work, school, or caregiving responsibilities; relationships and social engagement; sleep, appetite, or basic self-care; or concentration, decision-making, and emotional regulation.
When these difficulties persist or worsen over time, documented treatment goals and interventions can help stabilize functioning and support recovery.
Risk Factors and Comorbidities
Certain factors increase the likelihood that grief will become complex or prolonged. These include sudden or violent loss, limited social support, prior trauma, or unresolved relationship dynamics with the deceased. A history of anxiety, depression, trauma-related disorders, or substance use can also complicate the grief process.
Grief that occurs alongside other mental health conditions often benefits from coordinated, goal-directed treatment. In these cases, a grief treatment plan helps clinicians address overlapping symptoms while respecting the individual grief experience.
Clinical Considerations and DSM-5-TR
The DSM-5-TR recognizes prolonged grief disorder (PGD) as a diagnosable condition when grief responses are persistent, severe, and impairing beyond culturally expected timeframes. However, most grief does not meet diagnostic criteria and does not require pathologization.
A grief treatment plan does not require a formal diagnosis. Its purpose is to support clinical judgment, guide care, and document progress when grief becomes disruptive or complex. Careful assessment, cultural awareness, and ongoing review help ensure treatment remains appropriate and client-centered.
Types of Grief and Treatment Planning Considerations
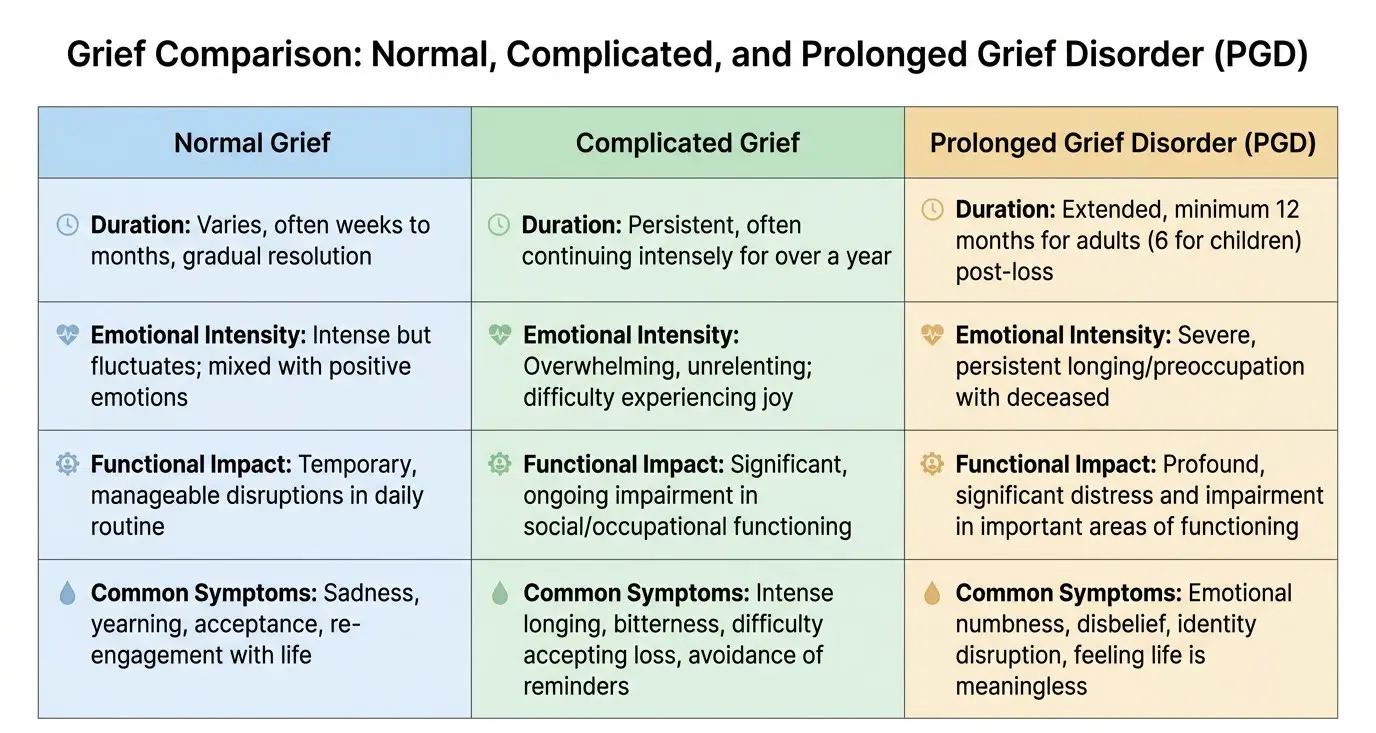
Grief presents in different patterns over time. Recognizing these patterns helps clinicians determine when supportive care is sufficient and when structured treatment planning is appropriate. These categories are clinical reference points, not fixed stages.
Acute Grief
Acute grief commonly occurs in the first months following a loss. Clients may experience intense sadness, yearning, guilt, disrupted sleep, poor concentration, emotional numbness, or physical distress. In many cases, acute grief does not require a formal treatment plan. Clients are often able to maintain basic functioning and gradually adapt with time, social support, and routine.
The clinical focus is typically on emotional support, validation, and stabilization. Psychoeducation, normalization of grief responses, and strengthening existing coping strategies are often sufficient. Structured treatment planning may be appropriate if acute grief intensifies over time, interferes with daily functioning, or is accompanied by significant avoidance, persistent distress, or comorbid mental health concerns.
Integrated Grief
Integrated grief reflects ongoing adjustment to loss. Clients may return to daily routines while continuing to experience sadness, longing, or emotional pain at times. The loss becomes part of their lived experience rather than the central focus of daily functioning.
Grief reactions may resurface around anniversaries, holidays, or reminders. This fluctuation is expected and does not indicate regression. Treatment planning during this phase may focus on maintaining functioning, reinforcing coping skills, and supporting meaning-making. Formal plans are often brief and flexible, with goals centered on resilience, role functioning, and emotional regulation.
Complicated Grief
Complicated grief involves persistent, intense distress that does not ease with time. Clients may experience ongoing preoccupation with the loss, intrusive memories, strong guilt, avoidance of reminders, or a sense that life cannot move forward.
This presentation is associated with increased risk of depression, anxiety, trauma-related symptoms, social withdrawal, and functional impairment. Formal, structured treatment planning is often necessary in cases of complicated grief. Clear goals, measurable objectives, and documented interventions help guide care, monitor progress, and support sustained clinical engagement.
Related: Exploring the Real Connections Between Trauma and Addiction and Loss
Grief Treatment Plan Goals and Objectives: Examples by Grief Type
Treatment goals for grief should be client-centered and outcome-focused. They describe what the client is working toward, rather than how quickly grief should resolve. Effective goals focus on improving functioning, reducing distress, and supporting healthy adaptation to loss — not eliminating sadness, longing, or emotional pain.
Objectives differ from goals in that they define how progress will be observed and evaluated. While goals describe the desired outcome, objectives break that outcome into specific, measurable steps that can be tracked over time.
The following examples are organized by grief presentation to help clinicians select and adapt goals and objectives for individual clients.
Download the Grief Goals & Objectives Quick-Reference Guide
Give clinicians a faster way to build grief treatment plans with a printable PDF of copy-ready goals, SMART-compatible objectives, and intervention guidance.
- Goals and measurable objectives organized by grief presentation
- Examples for acute grief, complicated grief, PGD, comorbid conditions, and special populations
- SMART goals framework and intervention quick reference for clinical documentation
Free download for behavioral health clinicians.
Goals and Objectives for Acute Grief
In acute grief, treatment goals often focus on stabilization, preserving basic functioning, and helping clients stay connected to supportive routines and relationships while the loss is still fresh.
Goal 1
Stabilize emotional functioning during acute grief.
- Client will identify and use at least two coping strategies during periods of grief-related distress within four weeks.
- Client will report a reduction in the frequency of overwhelming emotional episodes from daily to two or fewer times per week within six weeks.
- Client will demonstrate the ability to use grounding or self-regulation techniques during sessions within three weeks.
Goal 2
Maintain daily functioning and self-care routines.
- Client will resume a consistent sleep schedule (five or more nights per week of adequate sleep) within four weeks.
- Client will maintain at least three basic self-care activities (hygiene, meals, movement) daily over a two-week period.
- Client will return to at least one work, school, or caregiving responsibility within six weeks.
Goal 3
Reduce isolation and re-engage with support systems.
- Client will participate in at least one social interaction per week within one month.
- Client will identify and reach out to at least two sources of personal support within three weeks.
Goals and Objectives for Complicated Grief
When grief remains intense, persistent, and functionally impairing, treatment planning often shifts toward reducing avoidance, improving emotional regulation, restoring role functioning, and helping the client develop an adaptive ongoing connection to the deceased.
Goal 1
Reduce preoccupation with the loss and grief-related avoidance.
- Client will reduce avoidance of identified grief triggers through gradual exposure over a six-week period.
- Client will decrease the frequency of intrusive thoughts or rumination about the loss from persistent to intermittent, as reported in session, within eight weeks.
- Client will engage with at least one previously avoided activity, place, or memory related to the deceased within four weeks.
Goal 2
Improve emotional regulation and reduce persistent grief-related distress.
- Client will identify and practice at least three coping strategies for managing intense grief responses within six weeks.
- Client will report a decrease in the intensity of grief-related distress (using a self-rated scale) over a defined review period.
- Client will demonstrate the ability to tolerate grief-related emotions without engaging in avoidance or withdrawal during at least two sessions per month.
Goal 3
Support functional reintegration and role engagement.
- Client will resume participation in work, caregiving, or community roles with reduced grief-related disruption within three months.
- Client will engage in at least two meaningful activities per week that are unrelated to the loss within eight weeks.
- Client will establish at least one new routine or role-based activity within two months.
Goal 4
Develop a continuing bond with the deceased that supports adaptation.
- Client will articulate at least two positive memories or aspects of the relationship with the deceased without experiencing debilitating distress within eight weeks.
- Client will engage in a meaning-making activity (journaling, memorial, narrative exercise) at least once per month.
Goals and Objectives for Grief with Comorbid Conditions
When grief overlaps with depression, anxiety, trauma-related symptoms, or other mental health concerns, treatment goals should address both the grief process and the symptoms that may be intensifying impairment or slowing recovery.
Goal 1
Address grief-related depression symptoms alongside the grief process.
- Client will report a reduction in depressive symptoms (PHQ-9 score decrease of at least 5 points) within 12 weeks.
- Client will engage in behavioral activation by scheduling and completing at least three pleasurable or meaningful activities per week within six weeks.
Goal 2
Reduce grief-related anxiety and hypervigilance.
- Client will practice anxiety management techniques (deep breathing, progressive muscle relaxation) at least three times per week within four weeks.
- Client will report reduced frequency of catastrophic thinking related to further loss within eight weeks.
Goal 3
Address trauma responses that complicate the grief process.
- Client will report a reduction in trauma-related intrusive symptoms (nightmares, flashbacks) within 12 weeks.
- Client will demonstrate the ability to differentiate grief responses from trauma responses during sessions within six weeks.
Grief Counseling Goals for Special Populations
Grief counseling goals should be adapted to developmental stage, social context, and the nature of the loss. These examples reflect how treatment planning may differ for children and for clients whose grief is disenfranchised or anticipatory.
Goal
Support children in processing grief in developmentally appropriate ways.
- Child client will express grief-related emotions through play, art, or narrative activities in at least two sessions per month.
- Child client will demonstrate improved emotional vocabulary, identifying at least three grief-related feelings, within six weeks.
- Child client will resume participation in school and peer activities with reduced behavioral disruption within two months.
Goal
Support clients experiencing disenfranchised or anticipatory grief.
- Client will identify and articulate the nature of their grief experience, including any barriers to external recognition, within four weeks.
- Client will develop at least two personalized strategies for honoring and processing grief that may not be publicly acknowledged.
- Client will report increased self-validation and reduced internalized shame related to the grief experience within eight weeks.
SMART Goals for Grief Therapy
SMART goals provide structure in grief therapy without imposing unrealistic expectations. When goals are specific, measurable, achievable, relevant, and time-bound, they help clinicians and clients focus on functional progress while recognizing that grief does not follow a fixed timeline.
In grief treatment, SMART goals should prioritize coping, functioning, and emotional regulation rather than eliminating grief. Goals should remain flexible and be reviewed or adjusted as grief fluctuates.
The SMART Framework Applied to Grief
| SMART Element | What It Means in Grief Treatment | Example |
|---|---|---|
| Specific | Clearly defines the behavior, skill, or outcome being targeted | "Client will identify two coping strategies" rather than "Client will cope better" |
| Measurable | Includes a way to observe or quantify progress | "Reported sleep consistency of 5+ nights per week" rather than "Client will sleep better" |
| Achievable | Realistic given the client's current capacity and grief stage | Resuming one activity per week, not returning to full pre-loss functioning |
| Relevant | Directly connected to the client's grief experience and treatment goals | Coping with grief triggers, not unrelated life goals |
| Time-bound | Includes a review period or target timeframe | "Within four weeks" or "over a six-week period" |
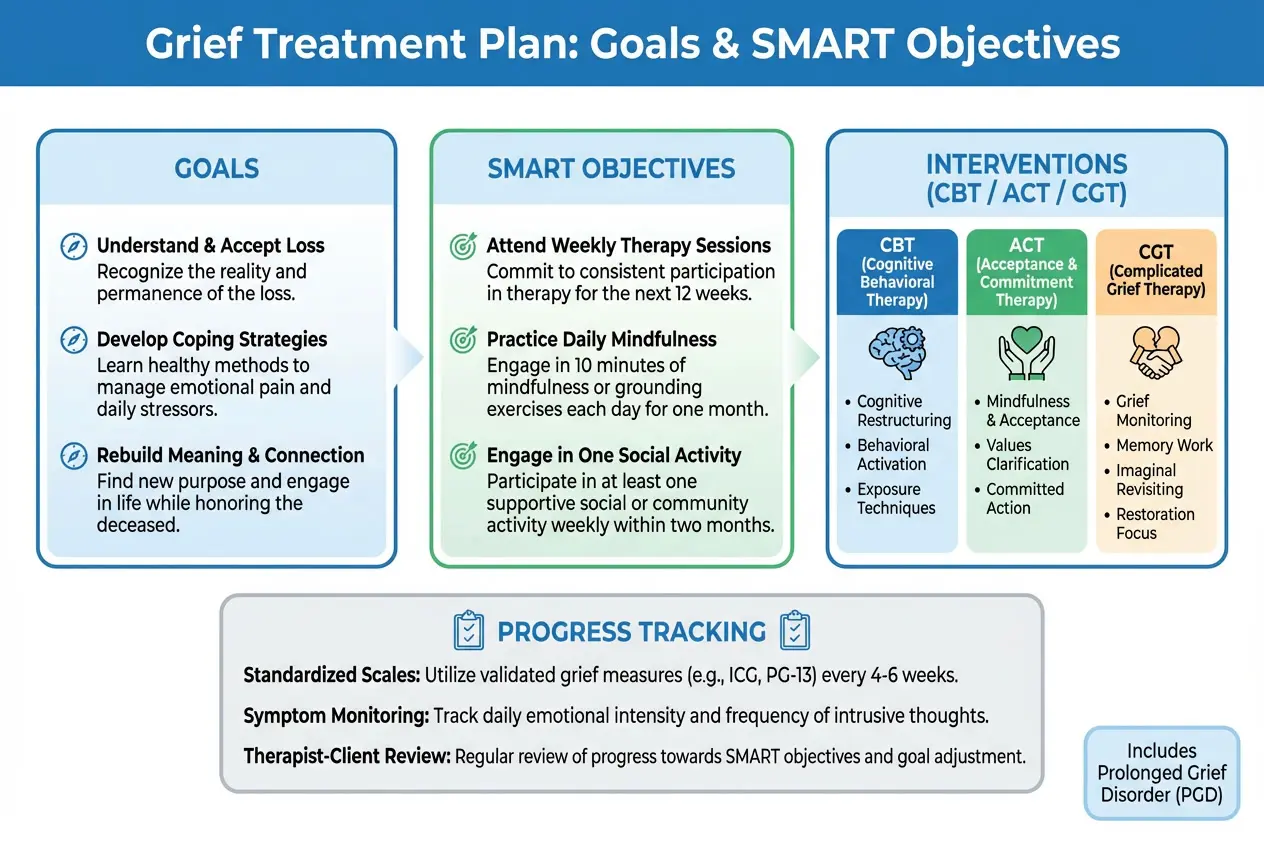
The visual below shows how the SMART framework can be applied to grief treatment goals using clear, measurable clinical examples.

The infographic below provides a visual breakdown of how SMART goals, treatment objectives, and evidence-based interventions align in a grief treatment plan.

The examples below show how SMART goals for grief can be translated into clear, measurable objectives across both short-term stabilization and long-term adaptation.
Short-Term SMART Goals for Grief
Short-term SMART goals often focus on stabilization and day-to-day functioning:
- Client will identify and use at least two coping strategies during periods of acute grief-related distress over the next four weeks.
- Client will resume one routine or social activity per week within one month.
- Client will establish a consistent sleep routine on at least five nights per week over a three-week period.
- Client will practice one grounding or self-regulation technique during grief-related distress at least three times per week within two weeks.
- Client will attend all scheduled therapy sessions (or reschedule within the same week) for a four-week period.
- Client will reduce avoidance of one identified grief trigger through gradual exposure within three weeks.
Long-Term SMART Goals for Grief
Long-term SMART goals support adaptation and reintegration:
- Client will engage in work, caregiving, or social roles with reduced grief-related disruption within six months.
- Client will report improved emotional regulation when experiencing grief triggers over a defined review period.
- Client will develop a personal narrative that integrates the loss while maintaining future-oriented goals within four months.
- Client will demonstrate the ability to experience grief-related emotions (sadness, longing) without significant functional impairment for a sustained period of eight weeks.
- Client will identify and maintain at least two ongoing sources of social support within three months.
- Client will articulate at least three coping strategies they can use independently after therapy concludes.
Measuring Progress Without Invalidating Grief
Progress in grief therapy should be measured through changes in functioning, coping, and emotional regulation rather than the absence of grief. Continued sadness or longing does not indicate treatment failure. Instead, clinicians should assess whether clients are better able to manage distress, engage in daily life, and respond flexibly to grief-related triggers.
Using SMART goals in this way allows clinicians to document meaningful progress while respecting the ongoing and individual nature of grief.
Therapeutic Interventions for Grief Treatment Plans
Clients process grief in different ways, and therapeutic interventions should be selected based on individual needs, the type of loss, symptom presentation, and treatment goals. The most effective approach depends on clinical context, and combining interventions may provide better support than using a single approach.
The following interventions are commonly used in grief treatment plans. Each section includes how the intervention connects to treatment goals so clinicians can align documentation across the plan.
Cognitive Behavioral Therapy (CBT) for Grief
Cognitive behavioral therapy helps clients identify unhelpful thought patterns and behaviors that contribute to grief-related distress. In grief treatment plans, CBT focuses on improving coping, reducing avoidance, and supporting healthier interpretations of the loss experience.
How CBT maps to grief treatment goals: CBT interventions support goals related to reducing avoidance, improving emotional regulation, and challenging maladaptive cognitions such as guilt, self-blame, or catastrophic thinking about the future. When a treatment plan goal targets "reducing grief-related avoidance," CBT provides structured techniques like behavioral experiments, graded exposure to grief triggers, and cognitive restructuring to address the avoidance cycle.
CBT strategies in grief treatment include identifying and addressing avoidance patterns, introducing adaptive coping strategies, using cognitive restructuring to challenge guilt or negative thought patterns, supporting behavioral activation to encourage re-engagement in meaningful activities, and developing a revised narrative around the loss.

Acceptance and Commitment Therapy (ACT) for Grief
Acceptance and Commitment Therapy helps clients relate differently to grief by increasing psychological flexibility rather than avoiding painful emotions. In grief treatment plans, ACT supports acceptance, present-moment awareness, and values-based action.
How ACT maps to grief treatment goals: ACT interventions align with goals related to reducing experiential avoidance, increasing engagement in meaningful activities, and building tolerance for difficult emotions. When a treatment plan goal targets "improving the client's ability to manage grief-related distress without avoidance," ACT provides the framework for approaching emotional pain with openness rather than suppression.
ACT strategies in grief treatment include helping clients identify personal values, supporting acceptance of difficult emotions related to loss, encouraging present-focused awareness through mindfulness, reducing experiential avoidance, and promoting engagement in valued activities despite emotional pain.
Complicated Grief Therapy (CGT)
CGT is a structured, evidence-based treatment for clients experiencing prolonged, intense grief that significantly interferes with daily functioning. It integrates elements of CBT, interpersonal therapy, and exposure-based approaches to address both the loss and its impact on the client's current life.
How CGT maps to grief treatment goals: CGT supports goals related to reducing preoccupation with the loss, decreasing avoidance of grief reminders, improving role functioning, and developing a continuing bond with the deceased that supports adaptation rather than fixation.
Traumatic Grief Therapy
Some cases of grief involve trauma, particularly when the death was sudden, violent, or witnessed by the client. Trauma can mask the grief response and make it difficult for clients to engage with the normal grieving process. Traumatic grief therapy addresses the trauma response alongside the grief, helping to disentangle the two experiences.
How traumatic grief therapy maps to treatment goals: This approach supports goals related to reducing trauma-related intrusions (flashbacks, nightmares), improving the client's ability to differentiate grief from trauma responses, and creating safety and stability as a foundation for grief processing.
Additional Interventions
Interpersonal Therapy (IPT): Addresses grief within the context of relationships and social roles. Treatment explores the client's relationship with the deceased and examines how the loss has affected current patterns of connection, communication, or withdrawal. Supports goals related to social reintegration and relationship functioning.
Group Therapy: Allows grieving clients to share experiences with others who have experienced similar losses. Reduces isolation, normalizes grief responses, and provides emotional support. Particularly useful for clients with limited personal support systems. Supports goals related to reducing social withdrawal and building ongoing support networks.
Behavioral Activation: Encourages gradual re-engagement in meaningful, pleasurable, or routine activities. Directly supports goals related to functional improvement, reducing avoidance, and increasing daily engagement.
Psychoeducation: Provides information about the grief process, mourning, and common grief reactions. Supports goals related to normalization, self-awareness, and informed coping. Psychoeducation can include discussion of grief models (such as Worden's Four Tasks of Mourning or the Dual Process Model), information about what to expect over time, and strategies for self-care during bereavement.
Companioning: Companioning focuses on presence, empathy, and validation rather than analysis or problem-solving. The clinician provides a supportive, non-judgmental space where clients can express grief openly.
Bibliotherapy: Bibliotherapy encourages clients to engage with written material related to grief and loss to support reflection and emotional processing.
Art Therapy: Offers a creative outlet for expressing grief when verbal communication is difficult. Supports goals related to emotional expression, distress regulation, and meaning-making.
Play Therapy: Commonly used with children who are grieving a significant loss. Through play, storytelling, or symbolic activities, children can express emotions and develop coping skills in a developmentally appropriate way.
Treatment Planning for Prolonged Grief Disorder
Prolonged grief disorder (PGD) is recognized in the DSM-5-TR as a diagnosable condition. It is characterized by intense, persistent grief that continues beyond culturally expected timeframes and significantly impairs functioning. Understanding PGD is increasingly important for clinicians, as its formal recognition provides a framework for more targeted, structured treatment planning.
Diagnostic Overview
PGD is distinguished from normal grief by the intensity and persistence of symptoms, as well as the degree of functional impairment. Core features include persistent yearning or longing for the deceased, preoccupation with the death or the deceased, and significant difficulty accepting the loss. Additional symptoms may include emotional numbness, avoidance of reminders, intense loneliness, difficulty engaging in activities, and a sense that life has lost meaning.
For a DSM-5-TR diagnosis, symptoms must persist for at least 12 months following the loss (or 6 months in ICD-11), cause clinically significant distress or impairment, and exceed culturally expected norms for the individual's community and context.
How PGD Treatment Planning Differs
Treatment plans for prolonged grief disorder tend to be more structured and longer-term than plans for acute or uncomplicated grief. Key differences include a greater emphasis on exposure-based strategies to address avoidance, explicit goals targeting preoccupation and yearning, focus on role functioning and reintegration over an extended timeline, and closer monitoring of comorbid symptoms (depression, anxiety, trauma-related presentations).
Clinical Interventions
Clinical interventions describe the therapeutic methods used to help clients meet their goals and objectives. Interventions should be selected based on the client’s needs, grief presentation, and clinical history, rather than applied uniformly.
Interventions must align clearly with stated goals and objectives. For example, interventions aimed at reducing avoidance should support functional re-engagement, while interventions addressing rumination or guilt should support emotional regulation and meaning-making.
Grief treatment plans should remain flexible. As grief evolves, goals, objectives, and interventions may need to be reassessed and adjusted. Regular review helps ensure care remains appropriate, responsive, and centered on the client’s experience.
PGD-Specific Goals and Objectives
Treatment planning for prolonged grief disorder (PGD) typically emphasizes reducing persistent symptoms, addressing avoidance, restoring functioning, and supporting adaptive integration of the loss over time.
Goal 1
Reduce the intensity and frequency of prolonged grief symptoms.
- Client will report a measurable reduction in yearning and preoccupation using a validated grief measure such as the PG-13 or ICG within 12 weeks.
- Client will demonstrate increased ability to redirect attention from grief-related preoccupation to present-focused activities during sessions within eight weeks.
Goal 2
Address avoidance of grief reminders and support acceptance.
- Client will engage in graduated exposure to at least three avoided grief-related situations, places, or memories over a 12-week period.
- Client will demonstrate improved tolerance of grief-related distress during exposure exercises, as observed in session.
Goal 3
Support functional reintegration and future-oriented planning.
- Client will resume participation in at least two major life roles such as work, caregiving, social, or community activities with reduced impairment within four months.
- Client will identify at least two future-oriented personal goals within three months.
Goal 4
Develop a sustainable continuing bond with the deceased.
- Client will articulate a personal narrative that integrates the loss and the ongoing relationship with the deceased within four months.
- Client will engage in at least one adaptive ritual or practice that honors the deceased without reinforcing avoidance within six weeks.
Recommended Interventions for PGD
Evidence-based approaches for prolonged grief disorder include Complicated Grief Therapy (CGT), which has the strongest evidence base for PGD and combines exposure-based techniques with interpersonal strategies; CBT for grief, particularly cognitive restructuring and behavioral activation components; and ACT-based approaches for increasing psychological flexibility and values-driven engagement.
Clinicians should also monitor for comorbid depression, anxiety, and trauma-related presentations, which are common alongside PGD and may require concurrent treatment.
Sample Treatment Plan for Grief and Loss
The following example reflects how a grief treatment plan may be documented in clinical practice. It is provided for educational purposes and should be adapted to the individual client's presentation, context, and clinical judgment.

Sample Treatment Plan for Grief and Loss
Client Presentation
Client is a 46-year-old adult presenting with grief following the death of a long-term partner nine months ago. Client reports persistent sadness, sleep disturbance, reduced concentration, and social withdrawal. Grief-related distress increases around reminders of the loss. Client continues to meet basic responsibilities but reports decreased motivation and difficulty experiencing pleasure. No current suicidal ideation or intent reported.
Primary Problem
Unresolved grief contributing to emotional distress, functional impairment, and avoidance of grief-related reminders.
Long-Term Treatment Goals
- Client will adapt to the loss in a way that allows for improved daily functioning and emotional regulation.
- Client will reduce grief-related distress while maintaining a healthy emotional connection to the deceased.
Short-Term Treatment Goals
- Increase the client’s ability to manage acute grief-related distress.
- Improve consistency in daily routines and social engagement.
Measurable Objectives
- Client will identify and practice at least two coping strategies to manage grief-related distress within four weeks.
- Client will resume participation in at least one social or routine activity per week within one month.
- Client will reduce avoidance of identified grief triggers through gradual exposure over a six-week period.
- Client will report improved sleep consistency, defined as five or more nights per week of adequate sleep, within six weeks.
Clinical Interventions
- Provide psychoeducation regarding grief, mourning, and the non-linear nature of the grief process.
- Utilize cognitive and behavioral strategies to address avoidance, rumination, and grief-related guilt.
- Support emotional regulation through grounding, mindfulness, and relaxation techniques.
- Implement behavioral activation to encourage gradual re-engagement in meaningful activities.
- Monitor mood, sleep, and functional impairment throughout treatment.
Review and Adjustment Plan
Treatment progress will be reviewed every four to six weeks. Goals and objectives will be adjusted based on changes in symptom severity, functional capacity, and client feedback. Increased grief intensity around anniversaries or reminders will be anticipated and addressed within the treatment plan. Continued treatment will be guided by clinical progress and client needs.
Expected Outcome
Client demonstrates improved coping with grief-related distress, increased engagement in daily activities, and greater emotional flexibility while continuing to process the loss.
Access Our Sample Treatment Plan Library
Get instant access to our full library of sample treatment plans.

Documenting Progress and Adjusting Grief Treatment Plans
Accurate documentation supports continuity of care, informs clinical decision-making, and helps ensure treatment remains appropriate as grief evolves.
Monitoring Symptom Change and Functional Improvement
Progress in grief treatment is best assessed through changes in functioning, coping, and emotional regulation. Clinicians should note shifts in sleep, concentration, social engagement, and daily routines, recognizing that progress may be gradual and non-linear. Documentation should capture both gains and setbacks. Increased grief does not necessarily indicate a lack of progress — notes should reflect how clients respond to distress and use coping strategies.
Revising Goals as Grief Evolves
Grief treatment plans should be reviewed regularly and updated as the client's needs change. Early goals may focus on stabilization and basic functioning, while later goals may shift toward meaning-making, reintegration, or long-term adjustment. Revising goals is a normal part of grief treatment. Adjustments should be documented clearly, with a rationale linked to observed changes in symptoms, functioning, or life circumstances.
Ethical Documentation Considerations
Ethical grief documentation requires careful language. Clinicians should avoid framing normal grief responses as pathology or measuring success by the absence of sadness. Notes should reflect respect for the client's individual grief process, cultural context, and personal values. Documentation should be objective, clinically relevant, and free from judgment.
Avoiding Over-Treatment of Healthy Grief
Not all grief requires ongoing clinical intervention. As clients demonstrate improved coping and functioning, clinicians should consider tapering or concluding treatment. Documentation should reflect the clinical reasoning behind reducing session frequency or closing treatment. Effective grief treatment planning recognizes when support is no longer needed and documents progress toward resolution or transition appropriately.
Write Better Grief Treatment Plans with ICANotes
No matter how grief presents for your clients, accurate and consistent documentation is essential for tracking progress and adjusting treatment plans over time. Clear records help ensure continuity of care while preventing over-treatment of healthy grief. However, time-consuming documentation can disrupt clinical flow and reduce the time you spend with clients.
With ICANotes, you can efficiently document grief treatment plans using intuitive templates and assessment tools designed for mental health professionals. ICANotes provides a robust, easy-to-use EHR that supports compliant documentation, collaboration, and clinical best practices — helping reduce your documentation burden so you can focus on client care.
Schedule a demo or start a free trial to see how ICANotes can streamline the process of creating and documenting grief treatment plans while improving consistency.
Build Better Grief Treatment Plans—Faster
ICANotes helps you create structured, compliant grief treatment plans with pre-built goals, SMART objectives, and clinician-friendly documentation tools.
- Pre-configured treatment plan templates for behavioral health
- SMART-compatible goals and measurable objectives built in
- Faster documentation with audit-ready clinical language
- Integrated billing and progress tracking tools
Frequently Asked Questions About Grief Treatment Plans
Related Posts
Kaylee, a certified grief counselor and social worker, has dedicated the past decade to reshaping our understanding and support of grief. With experience at a nonprofit hospice, she's empowered individuals to navigate their grief journeys, recognizing that loss extends beyond death. As an author, speaker, and event organizer, Kaylee fosters spaces for acknowledging and embracing life's most challenging moments. Her work has been featured across various media, amplifying voices and broadening awareness of the diverse sources of grief in our lives.






